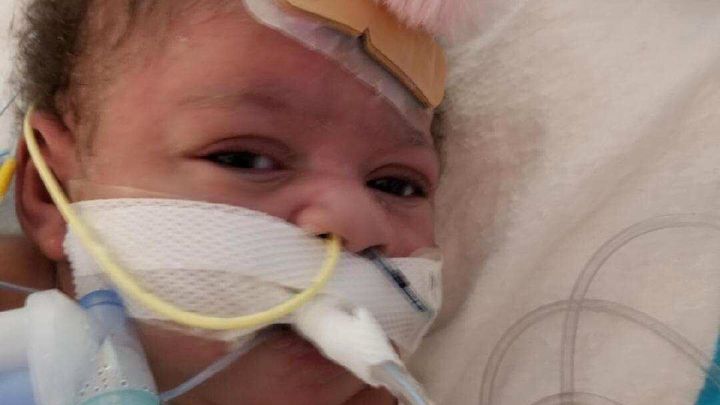
My four month old daughter, Phoenix Da'Vine (now 11 months), was a patient in the Pediatric Intensive Care Unit (PICU). I gave birth via C-Section on August 25, 2018 at 8:45 p.m. After Phoenix spent a few hours with me in my room after recovery, our nurse took her to the nursery for her routine checkup. She said that she would return in 5-10 minutes, but that turned into 20-30 minutes. When she finally returned, she informed me that Phoenix's oxygen saturations were low and a heart murmur was detected. Immediately after, Phoenix was admitted into the Neonatal Intensive Care Unit (NICU) where she spent a few days. At that time, an Echocardiogram (Echo) was performed on her heart and it was discovered that she has a major heart defect called Double Outlet Right Ventricle (DORV) that will require several surgeries in order for her to survive. From there, she was admitted into the PICU where a team of cardiologists started working on her cardiac plan. Phoenix's first palliative surgery took place on September 4, 2018 where she had a pulmonary arterial (PA) band surgically placed to limit the amount of blood that was flowing to her lungs in order to prevent congestive heart failure. Unfortunately, Phoenix was unable to tolerate the PA band, so she required a second surgery. On October 30, 2018, the PA band was removed, her atrial septal defect was enlarged, her pulmonary valve was removed and a Gortex shunt was placed. This is also a palliative operation. If Phoenix's heart cannot be fully repaired during her next operation, she will need to have a single ventricle palliation which includes the Glenn procedure at 6-12 months of age and a Fontan procedure at 18-24 months of age. Her four month hospital stay has definitely created a financial strain. Now we are faced with the likelihood of her having two more operations before we can consider her completely repaired.
Please view the attached link to read about Phoenix's current status. A devastating incident occurred on March 29, 2019 that has now made the above mentioned surgeries even more difficult to obtain since her campaign first started. All donations are appreciated and they will be used to pay off her past, current and future medical bills. We thank you in advance! https://www.gofundme.com/f/phoenixs-rising-to-recoveryhttps://wjla.com/news/local/miracle-baby-life-support-survived-celebrate-first-birthday
Please view the attached link to read about Phoenix's current status. A devastating incident occurred on March 29, 2019 that has now made the above mentioned surgeries even more difficult to obtain since her campaign first started. All donations are appreciated and they will be used to pay off her past, current and future medical bills. We thank you in advance! https://www.gofundme.com/f/phoenixs-rising-to-recoveryhttps://wjla.com/news/local/miracle-baby-life-support-survived-celebrate-first-birthday
Organizer and beneficiary
Susie Goldring
Organizer
Ft. Washington, MD
Monique Goldring
Beneficiary