- G
- B
- K
My name is Scarlett Smith and I am raising money for Whiston Hospital Critical Care Unit who saved my dad’s life.
My dad was admitted to the Critical Care Unit at Whiston Hospital from Thursday 27th November 2025 until Friday 2nd January 2026 with Guillain-Barré Syndrome. Words cannot express how grateful we are for the Critical Care Unit at Whiston Hospital. Without the Critical Care Team, my dad would not have survived and his story would be very different. His symptoms of Guillain-Barré Syndrome were not recognised or connected on the ward and only after examinations and tests done by the CRASH team was a potential diagnosis of the syndrome explored. From the moment the Critical Care team arrived, no time was wasted. They acted calmly, urgently and accordingly and he was able to receive the interventions and treatments which ultimately saved his life. As you can imagine, the entire experience has been extremely upsetting and overwhelmingly scary for my dad and our family but the competence, determination and relentless fight from the Critical Care team reassured us that he was in the best hands - and he was, without a doubt. From start to finish, throughout our journey with the Critical Care Unit, we were kept informed on what was happening and why and we were heavily involved in my dad’s care which brought us so much comfort. Not only did the Critical Care team save my dad’s life, they became part of our family - people that we could rely on for support. They got us all through the most horrific and traumatising time of our lives and filled us with hope when we were at a complete loss. We were treated with kindness, care, compassion, empathy, understanding and love from the moment we first met with the Critical Care team right up until his discharge from Whiston Hospital. The support did not end when we left the Critical Care Unit. They provided us with resources and information and are available to call or visit at any time which allows us process what has happened. Each and every single member of the Critical Care Unit were truly incredible. There are too many individual names to mention but we will never forget their huge impact and we are eternally thankful for them. The Critical Care Unit at Whiston Hospital will hold a special place in our hearts for the rest of our lives. Because of them, my dad got a second chance at life. They are angels on earth and we owe everything to them.
Myself, my dad and my family want to give back to the Critical Care Unit. Because of them, my dad is alive and because of them, our family is together. I am raising funds in the hope that they will help Whiston Hospital Critical Care Unit to access state-of-the-art equipment, enhance patient experience and comfort, provide support for relatives, support staff wellbeing and education and develop research. This will allow them to continue to save other people’s lives, like my dad and keep other families together, like mine.
My dad’s full story is below. Please read and consider donating to this amazing cause. All donations made will be sent directly to Whiston Hospital Critical Care Unit at a later date. Any donations, big or small, will be greatly appreciated. Thank you.
Mick’s fight against Guillain-Barré Syndrome
On the 23rd November 2025, our life came crashing down and changed forever when my Dad became unwell with Guillain-Barré Syndrome (GBS).
Guillain-Barré Syndrome is a rare autoimmune disorder where the immune system attacks peripheral nerves, causing rapid, assending muscle weakness, numbness and potential paralysis. Symptoms of Guillain-Barré Syndrome can progress rapidly over hours, days or weeks and can include; weakness and numbness (usually starting in the legs and feet then spreading to the arms, hands and face), tingling or prickling (a ‘pins and needles’ sensation in the hands and feet), pain (sharp, shooting or cramping pain in the legs or back, mobility issues (difficulty walking, climbing stairs or managing motor skills), face muscle issues (difficulty swallowing, speaking, chewing or drooping facial features) and respiratory distress. Guillain-Barré Syndrome is often described as a Post-Infectious Reaction as common illnesses such as a colds, flu, viruses, stomach bugs or food poisoning can trigger it. It is not typically contagious or inherited but rather a cross-reaction where the immune system accidentally attacks the nerves in the body whilst trying to fight an illness. Symptoms of Guillain-Barré Syndrome often appear within two to four weeks of an illness. Guillain-Barré Syndrome requires urgent hospitalisation, most often an Intensive/Critical Care Unit admission, where the main focus is immunotherapy to stop the immune attack on the nerves and supportive care to manage symptoms. The main treatments for this disease include intravenous immunoglobulin (IVIG) or plasma exchange (plasmapheresis). If symptoms of this disease are caught and treated early, it is unlikely to be life threatening but if treatment is delayed, it can and will be fatal. People who receive immediate treatment are likely to make a partial or full recovery with extensive rehabilitation which includes physical therapy, occupational therapy and speech and language therapy. However, if treatment is not received immediately Guillain-Barré Syndrome is serious. Guillain-Barré Syndrome can cause severe complications such as respiratory failure often requiring mechanical ventilation, autonomic dysfunction (unstable blood pressure, dangerous heart rythm abnormalities or cardiac arrest), blood clots, pneumonia, swallowing/feeding issues and serious infections such as sepsis), chronic fatigue, permanent paralysis and disability. Unfortunately for my dad, his symptoms were not recognised immediately which led to delays in his treatment meaning he suffered serious complications.
In the early hours of Sunday 23rd November 2025, my dad woke with numbness and tingling in his left arm and leg. The day before, he had been doing heavy lifting so he put it down to muscle strain and brushed it off. When he woke that morning, he was still experiencing numbness and tingling on his left side and he was unable to walk down the stairs. We phoned 111 who suspected a stroke and dispatched an emergency ambulance. Upon observations by paramedics, he was taken to Whiston Hospital A&E where he had scans and blood tests before being admitted to the stroke ward. Later that night he was able to walk to the toilet with the support of my mum and a ward nurse and was able to feed himself using his right side but felt that this side was also getting weaker. We left him in the hospital that night assuming that he would be treated and discharged within a few days. Little did we know the true horror that was going to unfold over the next 72 hours.
On Monday 24th November 2025, my dad woke unable to move both his arms and legs. Doctors couldn’t explain it and everyone was stumped. Throughout the day, my dad had more scans on his brain where no evidence of a new stroke was found but there were calcifications from previous strokes so doctors believed the damage could be hiding behind this. Once again, everyone was stumped. Later that night, my dad became unable to sit up unaided, he had lost all strength in his core. We left the hospital confused with no answers.
On Tuesday 25th November 2025, my dad had more scans on his brain and spine as doctors explored the possibility of a spinal stroke. There was still no evidence of a new stroke and there was no evidence of a spinal stroke which we thought was good news. The stroke consultant believed that the damage was hiding behind calcifications from previous strokes therefore it wasn’t showing up on scans. The consultant concluded that he had body mirroring, a phenomenon where the unaffected side of the body involuntarily mirros the symptoms of the affected side of the body due to the severe trauma that a stroke causes. This explained the paralysis on both sides of his body. The doctor explained that with time medications and mind training symptoms would relieve. This left us feeling reassured and hopeful. However, all hope would soon disappear and our lives would change forever over the next 24 hours.
On Wednesday 26th November 2025, my dad woke with the same symptoms accompanied by an extremely weak voice. His body became completely exhausted and his voice was getting progressively weaker. By early afternoon he began producing thick foam from his mouth which he was unable to cough up or spit out by himself. A sample of this was taken as doctors believed it was phlegm from a respiratory infection. Throughout the day, he continued to significantly decline. By the evening, the saturation of oxygen in his blood dropped to dangerously low levels. He lost the ability to swallow, was struggling to breathe, became pale/grey and disoriented. It was at this point when doctors realised that something sinister was causing him to have become so seriously unwell. The stroke ward called the CRASH team from the Critical Care Unit down to the ward. The CRASH team worked tirelessly for an hour and a half to stabilise my dad. He received medication and oxygen during this time but his oxygen saturation wasn’t improving. When checked, he had no reflexes in his body at all and upon arterial blood gas tests, dangerous levels of carbon dioxide was found in his blood. Over the course of the next few hours, he had multiple arterial blood gas tests done but the levels of carbon dioxide in his blood were not reducing, they were increasing. He also failed multiple spirometer tests to assess for respiratory muscle weakness. The Critical Care team found that he was in type two respiratory failure because his body was unable to expel enough carbon dioxide from his blood. The carbon dioxide was suffocating him. With all symptoms paired together, a potential diagnosis of Guillain-Barré Syndrome was mentioned for the first time. Unfortunately due to how long it took for my dad’s symptoms to be recognised and connected the disease had already taken over and began its path of destruction. Throughout the full day my dad’s body and organs had been shutting down and he was actively dying in front of our eyes. Without the Critical Care team, he wouldn’t have survived until the morning. There was little to no time to start interventions and treatment before it was too late. Due to the sheer scale of damage that the disease had already done, the Critical Care team were unsure if he would benefit from any interventions or treatment. We were sat down by the Critical Care team and told to prepare for the worst. This was when we were faced with the reality that the likelihood of my dad’s survival was extremely slim. We were at a complete loss. The physical pain and fear that took over my body that night is something that I had never experienced before and something I never want to experience again. It was completely earth shattering. After meetings and discussions it was decided that my dad would be taken to the Critical Care Unit for intervention and treatment to give him the best possible chance of survival.
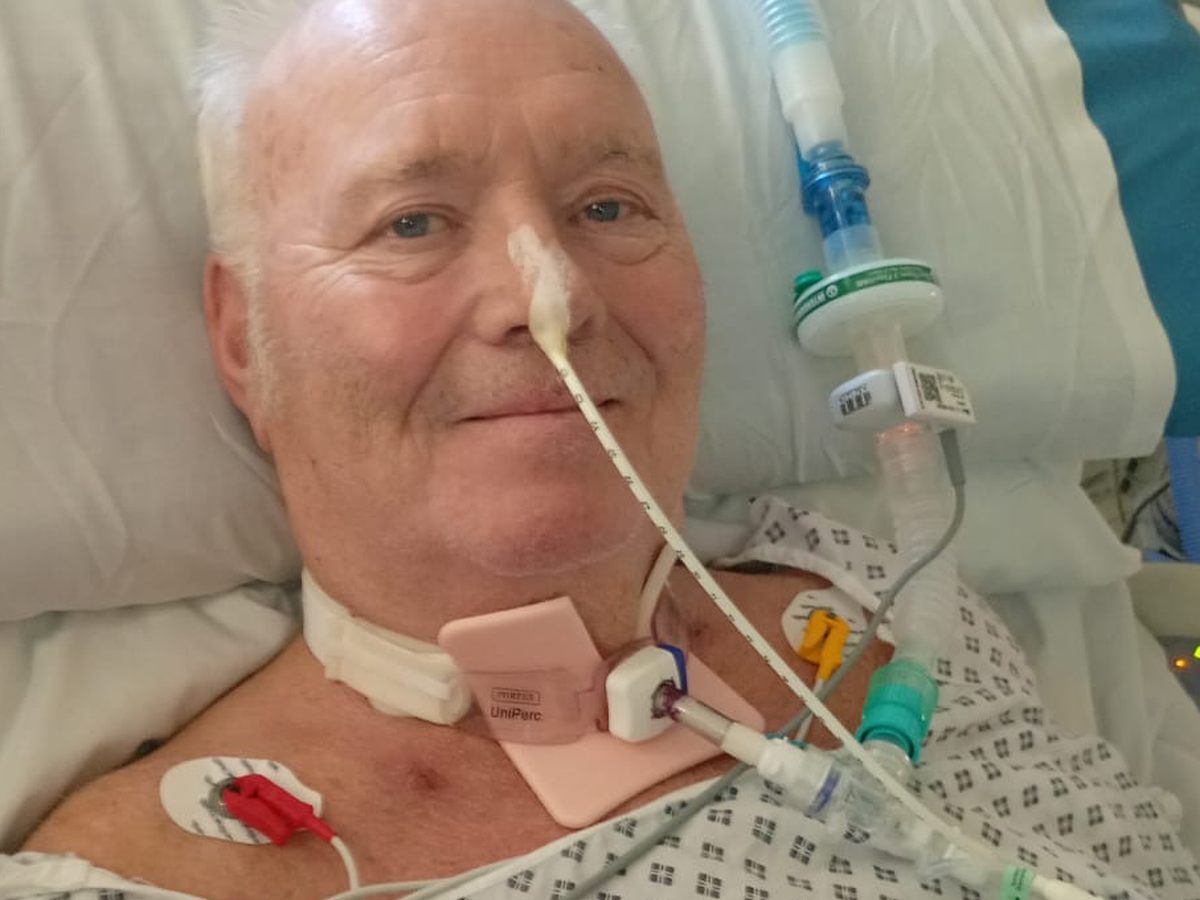
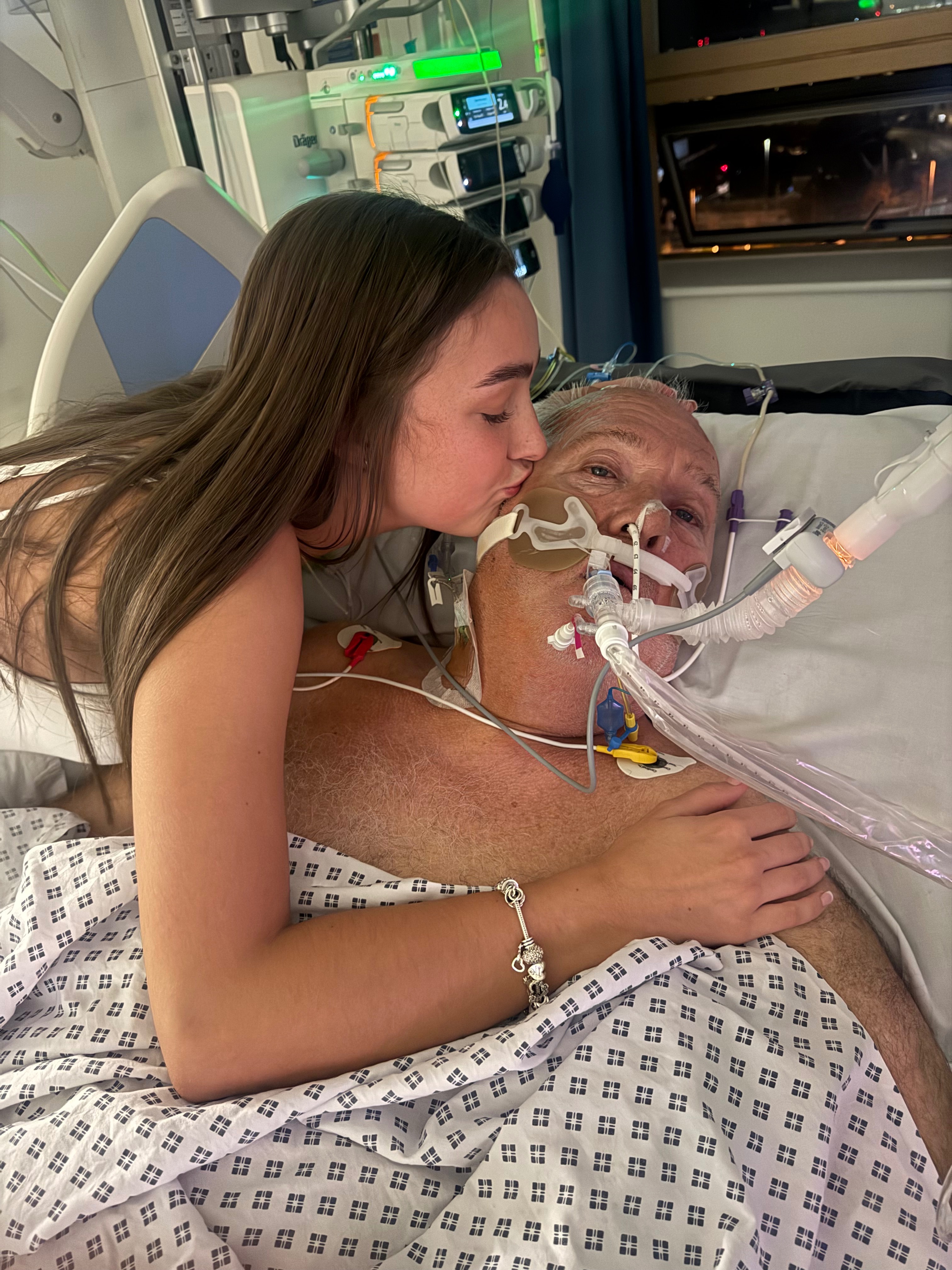
By this point, it was the early hours of Thursday 27th November 2025 and immediately after the decision had been made my dad was transferred to the Critical Care Unit. We were taken in to see him before he was placed into a medically induced coma and put on a ventilator. Saying goodbye to my dad that night was the the most traumatising but bravest thing I have ever done. The hours I spent watching him fight for his life and seeing the fear in his eyes as he realised what was happening to him will haunt me for as long as I live. Leaving him behind in that room, scared and alone broke me in a way I never could’ve imagined but knowing that the interventions and treatments would stop his suffering brought me an unspeakable amount of peace and comfort. Once he’d been put into a medically induced coma and ventilated, we were able to go back into the room to see him. He looked peaceful, a type of peace I had never seen before and have never seen since. The ventilation had brought back his colour and he looked like him again. He was finally getting the rest he so desperately needed after struggling and fighting for his life for so long. We were told that even though he was currently stable, his condition was critical and his chances of survival were low. For the first time in our lives, our eyes were opened to the true devastation and destruction of Guillain-Barré Syndrome. We had no choice but to go home. The silence was deafening. Empty corridors filled with hopelessness and dread. A type of pain and fear I’d never felt before.
The following week was the hardest week of our lives. It was a week of uncertainty, hopelessness and torture. We spent all day, every day sat by a bed in the Critical Care Unit watching someone who was completely healthy and so full of life just days before fight for every breath, hoping for nothing short of a miracle. A diagnosis of Guillain-Barré Syndrome couldn’t be confirmed without a lumbar puncture test but this couldn’t be performed for a week because my dad had previously been treated with blood thinners when a stroke was suspected which made the risk of bleeding to large. My dad began a five day course of intravenous immunoglobulin infusions in an attempt to stop the progression of the disease but the mass damage that had already been done was irreversible. Guillain-Barré Syndrome had left my dad completely paralysed from the neck down both internally and externally. Over the first week of his journey, the Critical Care team weaned down the sedation and brought my dad out of his medically induced coma however, Guillain-Barré Syndrome had paralysed his respiratory system and he was unable to breathe independently therefore, he still required mechanical ventilation to keep him alive. On Wednesday 3rd December 2025, my dad was put under general anaesthetic and underwent a lumbar puncture test and a tracheostomy procedure. A lumbar puncture test is a procedure where a needle is inserted into the spine to collect a sample of spinal fluid which is tested to diagnose conditions. A high level of protein in the collected spinal fluid confirms a diagnosis of Guillain-Barré Syndrome. A tracheostomy is a procedure where a surgeon makes an opening in the front of the neck area to provide an alternative airway for breathing. A tube is inserted into this opening to allow for long term mechanical ventilation. We received my dad’s lumbar puncture test results back which did show high levels of protein in his spinal fluid, confirming his devastating diagnosis. Following the confirmation of his diagnosis we were told that there were no more treatment options available and all we could do was wait to see if his nerves were able to regenerate themselves. Recovery from Guillain-Barré Syndrome is an extremely long, slow process and it is not guaranteed. Hearing this news was a massive shock to the system for my dad and for all of us. Within a week and without warning, our lives had been destroyed. We were left grieving what once was and were forced to accept a new reality.
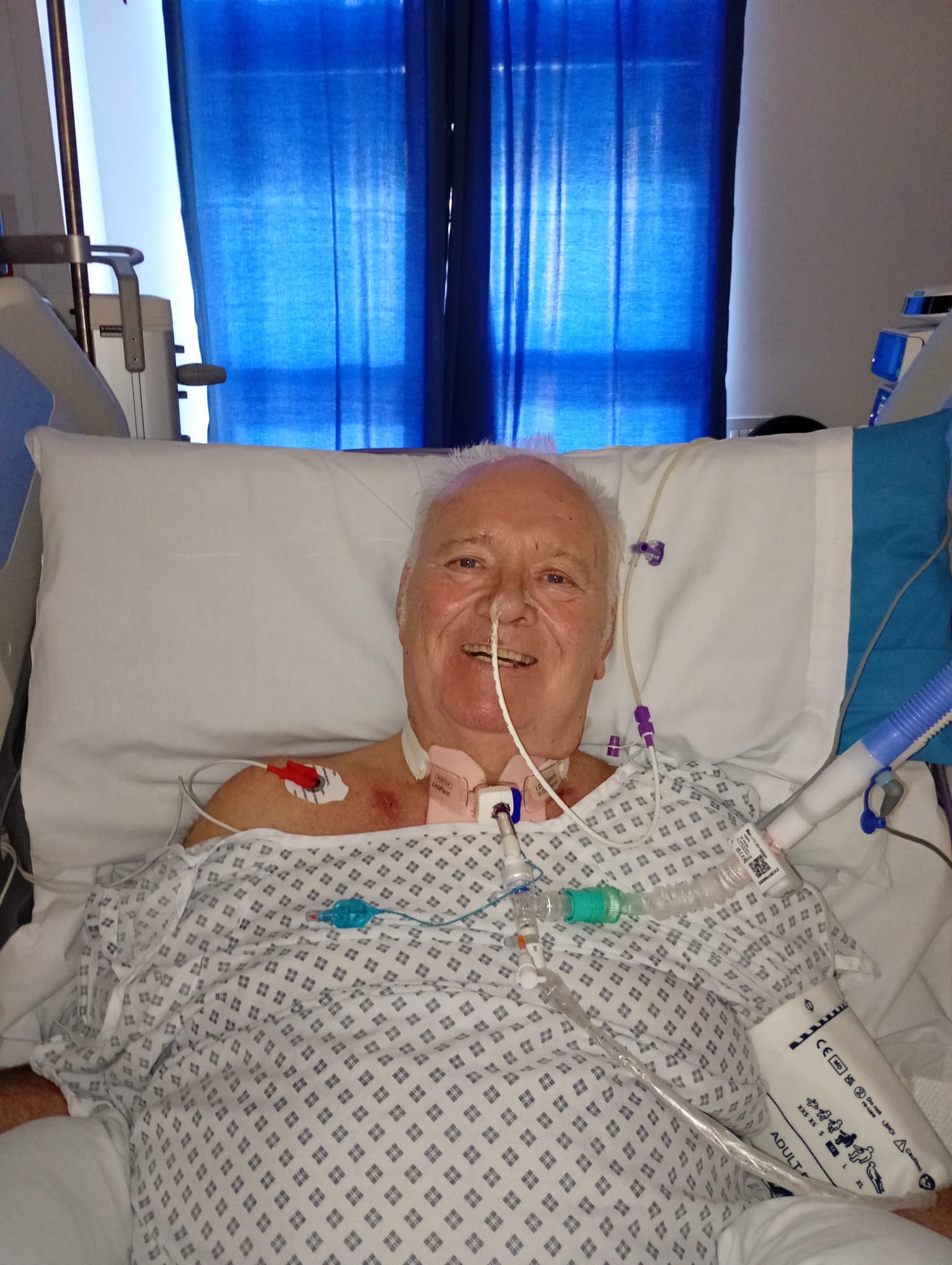
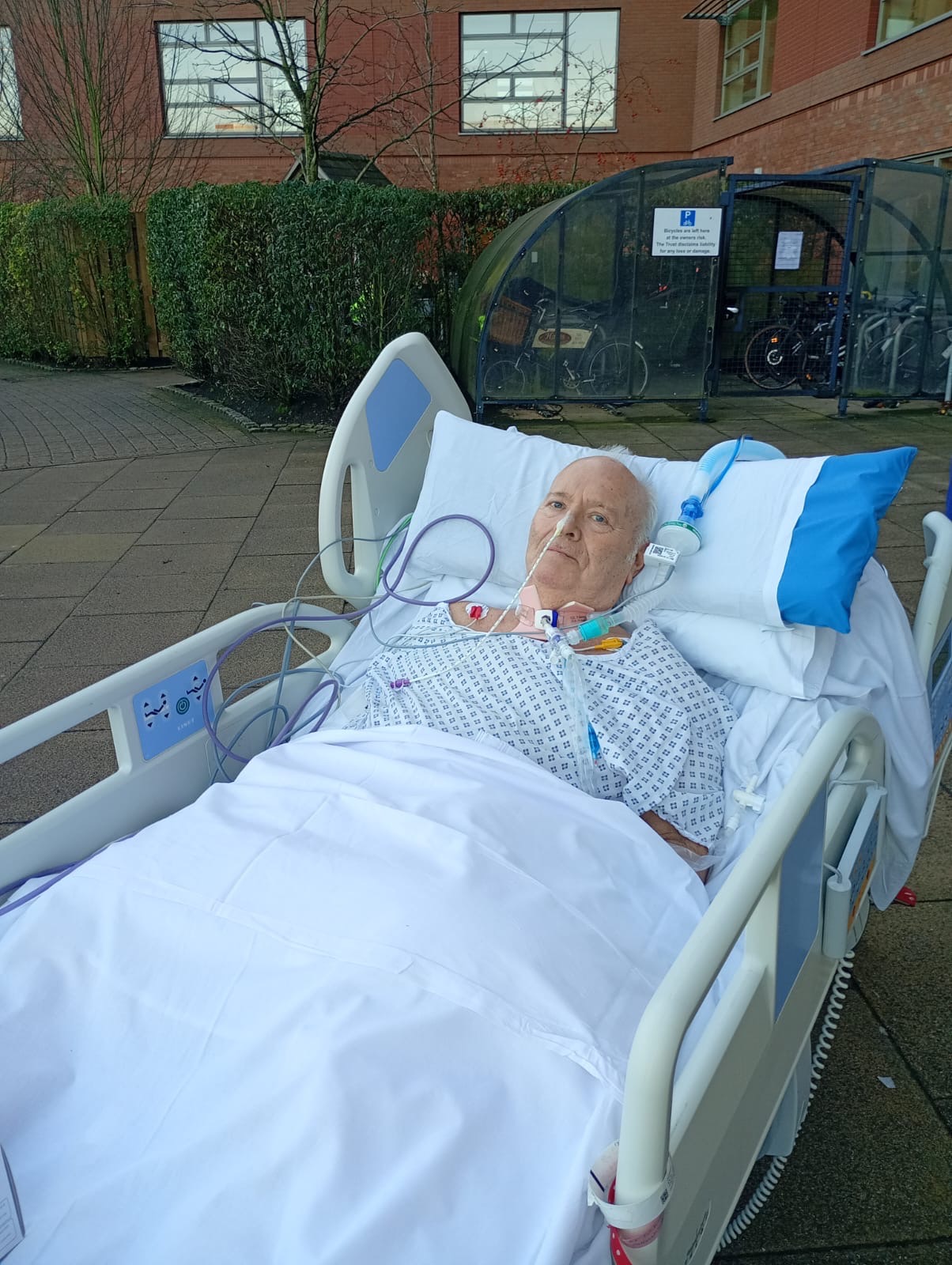
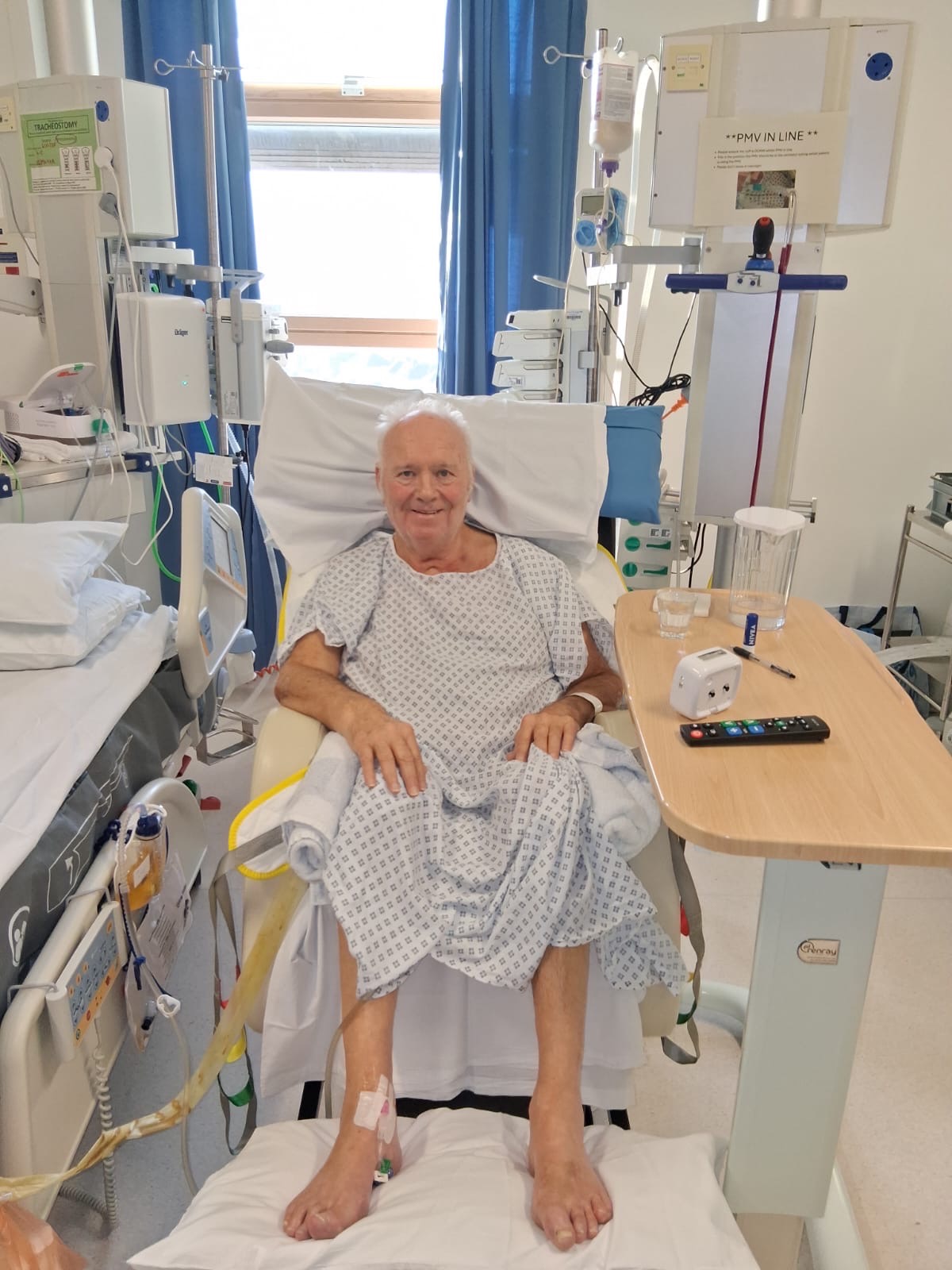
My dad remained in the Critical Care Unit for the next five and a half weeks. During this time, he underwent extensive rehabilitation everyday which included gruelling physiotherapy in a desperate attempt to regenerate his nerves. The nerve regeneration process created excruciating nerve pain all over his body which he has to endure all of the time. On Sunday 14th December 2025, with the incredible impact of the Critical Care team and modern medicine, we received the best news that we could’ve ever imagined. My dad was finally strong enough to breathe independently, the mechanical ventilation was turned off and on Wednesday 17th December 2025, his tracheostomy was removed. We thought we would never see my dad without tubes and machines keeping him alive again, it was bittersweet, a glimmer of light in such a dark time. He was monitored in the Critical Care Unit for a further two weeks and two days before being stepped down from here on Friday 2nd January 2026.
My dad remained on a ward at Whiston Hospital for thirteen days before being transferred by ambulance to the Walton Centre at Aintree Hospital on Tuesday 13th January 2026. He spent three and a half weeks here where he endured extensive rehabilitation in an attempt to regenerate and recover his nerves. On Saturday 7th February 2026, my dad was diagnosed with sepsis and pneumonia and was transferred to a medical unit at Aintree Hospital for treatment where he bravely overcame these illnesses. My dad currently remains at Aintree Hospital and is awaiting discharge to continue his recovery at home. However, Guillain-Barré syndrome does not end here and my dad still has a lifetime of physical and mental recovery ahead of him. Guillain-Barré Syndrome has left him completely paralysed from the neck down, he has no independence at all and has been stripped of his identity. He is faced with extensive rehabilitation and indescribable pain all over his body every day for the foreseeable future and will be have to live with the mental trauma it has caused forever. There is no guarantee that my dad will ever recover, only time will tell, but we remain hopeful and determined to get our lives back.
Words cannot express how grateful we are for the Critical Care Unit at Whiston Hospital. Without the Critical Care Team, my dad would not have survived and his story would be very different. His symptoms of Guillain-Barré Syndrome were not recognised or connected on the ward and only after examinations and tests done by the CRASH team was a potential diagnosis of the syndrome explored. From the moment the Critical Care team arrived, no time was wasted. They acted calmly, urgently and accordingly and he was able to receive the interventions and treatments which ultimately saved his life. As you can imagine, the entire experience has been extremely upsetting and overwhelmingly scary for my dad and our family but the competence, determination and relentless fight from the Critical Care team reassured us that he was in the best hands - and he was, without a doubt. From start to finish, throughout our journey with the Critical Care Unit, we were kept informed on what was happening and why and we were heavily involved in my dad’s care which brought us so much comfort. Not only did the Critical Care team save my dad’s life, they became part of our family - people that we could rely on for support. They got us all through the most horrific and traumatising time of our lives and filled us with hope when we were at a complete loss. We were treated with kindness, care, compassion, empathy, understanding and love from the moment we first met with the Critical Care team right up until his discharge from Whiston Hospital. The support did not end when we left the Critical Care Unit. They provided us with resources and information and are available to call or visit at any time which allows us process what has happened. Each and every single member of the Critical Care Unit were truly incredible. There are too many individual names to mention but we will never forget their huge impact and we are eternally thankful for them. The Critical Care Unit at Whiston Hospital will hold a special place in our hearts for the rest of our lives. Because of them, my dad got a second chance at life. They are angels on earth and we owe everything to them.
Words cannot express how incredibly proud we are of our hero. He has now been in hospital for ninety seven days which is 14 weeks which is three and a half months. Despite how hard this has been, he has had a smile upon his face and remained positive. He has fought for his life and has never once given up, even when all odds were stacked against him. He has shown and continues to show immense bravery, courage, strength and determination against a syndrome that has taken everything from him and came so close to taking his life. He is remarkable and a true inspiration.
Guillain-Barré Syndrome has taken everything from my dad and our family but together, we will take back control. Guillain-Barré Syndrome does not discriminate, it destroys everything in its path. It is essential to recognise the symptoms. If you experience any weakness or numbness in the legs/feet/arms/hands or face, sharp/shooting/cramping pains in the legs or back, tingling or pins and needles in the hands or feet, mobility issues, face muscle issues or respiratory distress (especially two to four weeks following a cold, flu, virus, stomach bug or food poisoning), I urge you to seek immediate medical care at your nearest Accident & Emergency Department. Early identification of symptoms, diagnosis and treatment is vital for a positive outcome. Ask yourself and medical professionals the question; Could it be Guillain-Barré Syndrome? Do not wait because Guillain-Barré Syndrome does not wait. It might just save your life.
Guillain-Barré Syndrome is extremely rare, affecting around one in one hundred thousand people a year but no one is invisible to it and the impact of it is devastating. Due to its rarity, it suffers from a general lack of public awareness. When you hear the words ‘Guillain-Barré Syndrome’, chances are you have never heard of it before and have no idea what it is. Maybe you have heard of it but don’t know that it a medical emergency that requires immediate and specialised care. We had never heard of it before and we had no idea what it was. This so desperately needs to change. Off the back of my dad’s strength, I now use my own strength to share his story to educate and raise awareness. In honour of him and every single life that has been affected by Guillain-Barré Syndrome, in any way, now and in the future.