- S
- C
- M
Our daughter is in need of urgent evaluation and medical care from her team of specialists in southern California. Unfortunately, with a steady decline in her condition, this cannot wait. She will be flown to SoCal June 3rd and begin evaluation, so we come to you with an urgent request for support.
 

The story of pursuing proper diagnosis and the beginning complications-
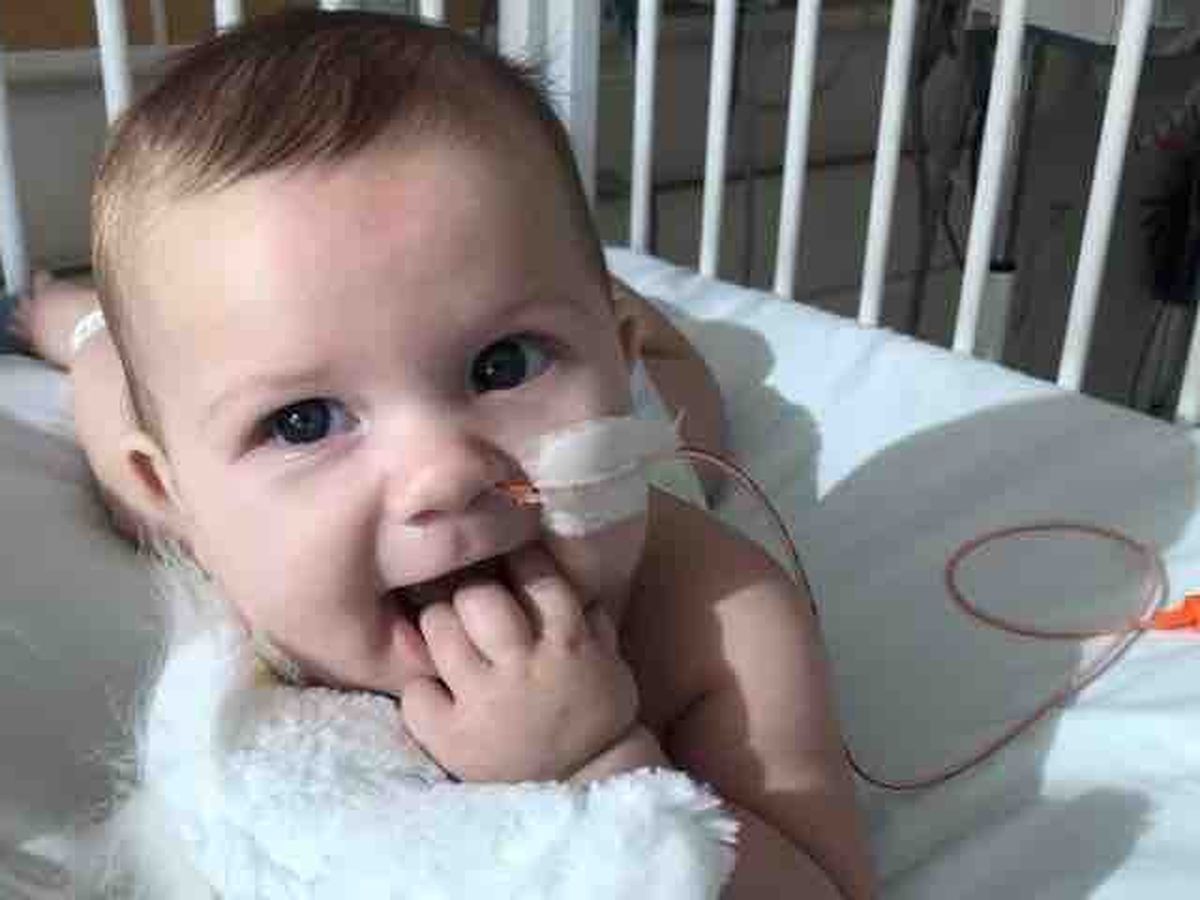
Teagan has struggled since birth with episodes of choking and feeding difficulties. For weeks we pressed doctors to look into the problems further, but we were consistently brushed off and told it was "normal". When she was about three months old, she had her first very serious illness, which was unfortunately, the same time her father left for sea for three months. She had retracted breathing, spiking fevers, and her choking escalated to the point she was turning deep red, almost purple during each episode. After the most severe choking episode, she had refused to eat entirely. She was no longer nursing and she had never accepted a bottle, so I knew it was even more serious. I contacted the doctor and they told me to bring her in. They examined her and determined she was severely dehydrated, but something else seemed to be wrong that they couldn't quite pinpoint so they told me to get her to the children's hospital as soon as possible. I raced Teagan there with her older brother.
When we arrived to the emergency room, they immediately took us back and began the process for an IV placement. After 7 tries with four different people, they got one placed. The doctor came in shortly after and told me that he was admitting her right away. He told me that it seemed like a serious upper respiratory infection, but since her oxygen levels were also so low he suspected something more serious.
 

During this hospital stay Teagan would have 11 IV placement attempts, four blown veins, she lost an alarming amount of weight, and it just got worse from there. On the fourth morning of her stay, her doctor came into the room at 6:00am and asked me if I could contact my husband. I explained to him that contact was limited because he was at sea and the color flushed from the doctor's face. I was also terrified at this point. The doctor told me that he would start the necessary emergency paperwork to get her father home "just in case". I'll never forget those words. I quickly dialed the Red Cross Emergency contact line while staring at my pale, tiny little girl in her metal hospital crib. After an hour the doctor came back and told me that the emergency request letter had been sent and that he hoped my husband made it home. The following day and a half lead to Ben eventually flying home to see his little girl hooked up to an IV and a feeding machine. Despite several attempts with physical therapists, she was still refusing to nurse. The medical team requested an NG tube be placed so she could come off of the IV.
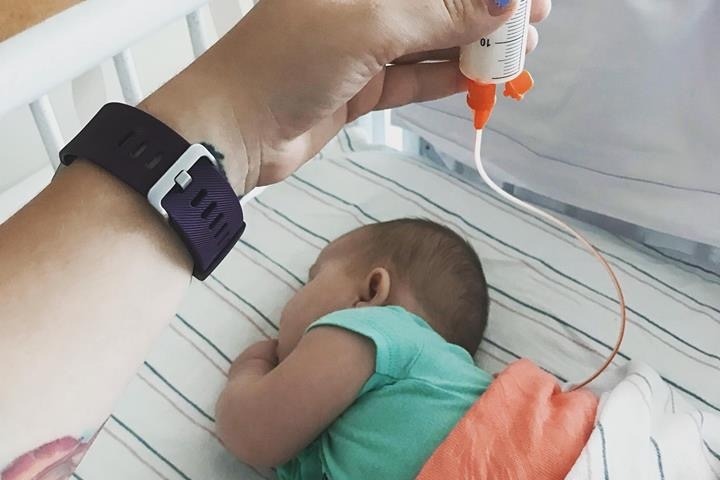 

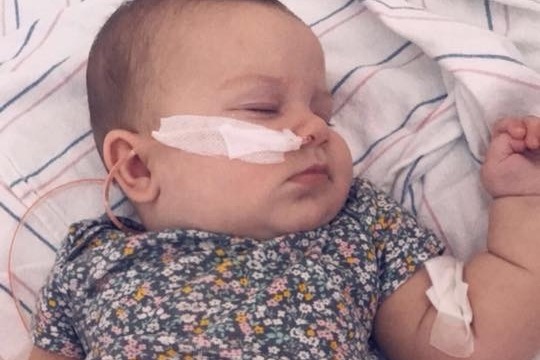 

Finally after almost 10 days in the hospital, Teagan was discharged with her feeding tube. She had only improved enough that the doctors felt I was capable of managing her feeds at home. But we left the hospital with no more answers than when we entered.
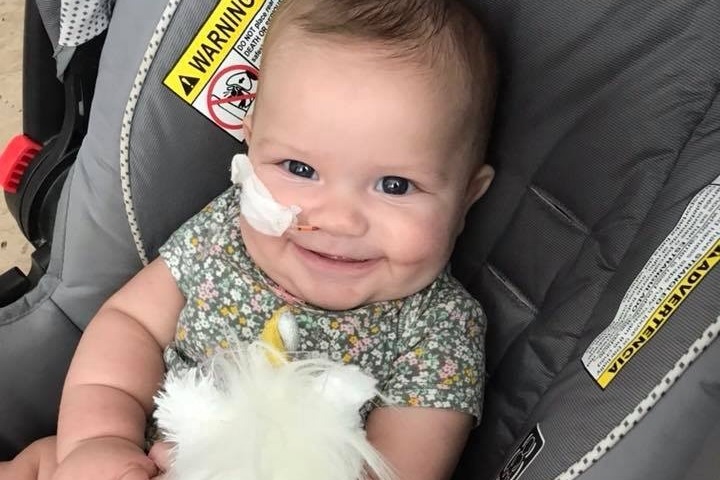 

Only three weeks later, Teagan ended up being admitted again with yet another serious illness that came on rapidly and hit her pretty hard. She had once again started choking, her fevers were spiking, she had retracted breathing, and she was refusing to nurse. During this stay, our concerns were FINALLY heard! Her new team of doctors pushed for further examination beyond the routine IV and oxygen monitoring. They scheduled her for a swallow study which revealed a few new answers. But that wasn't the end.
The months that followed had us in and out of physical therapy appointments, blood tests, swallow studies, GI appointments, and one very important clinic that gave us all the answers we needed, the Aerodigestive clinic. This clinic was a life saver for Teagan. An aerodigestive clinic is a day long event with a team of doctors and specialists that includes a dietitian, a pulmonologist, gastroenterologist, neurologist, a physical therapistand one of the nations leading pediatric otorhinolaryngologist.
 

Her final diagnosis was a malformed epiglottis that lead to additional epiglottis weakness and stage 2 Congenital Subglottic Stenosis (51-70% airway closure). Subglottic stenosis (SGS) is a narrowing of the airway below the vocal cords (subglottis) and above the trachea. Congenital subglottic stenosis occurs as a rare birth defect and may be associated with other genetic syndromes and conditions. The airway remains narrow because the airway cartilage did not form properly before birth. This condition makes contracting an illness especially dangerous because it does not leave much room for throat swelling or irritation. A healthy person typically has throat swelling with a cold or upper respiratory illness and their throat can accommodate for that swelling. Teagan’s airway has such high reactivity that even a simple common cold can cause serious problems for her.

Our plead for help-
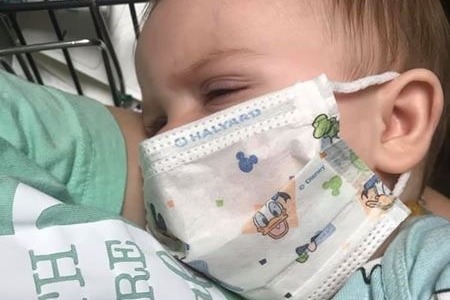
Since moving to Washington in January, Teagan has had four serious illnesses which have all landed her in the hospital for more thorough evaluation and care. We thought her condition would improve over time, but unfortunately, it has not. She still has days when she struggles to eat properly, she chokes every time she drinks water, every meal is a risk of choking, she is now anemic, and she is not properly gaining weight.
I contacted her team of specialists in SoCal last week and let them know about our rising concerns for Teagan’s condition and they told us that we need to get her to San Diego for care urgently. She is already scheduled for a three stage scope with a flexi scope and a rigid scope which is a fully sedated procedure in the OR with general anesthesia, she will have a full swallow study with radiology, she will go through the Aerodigestive clinic again to reevaluate any possible changes to her condition, and her team will decide if she needs to be admitted for further care or even potential airway surgery.
Our requested amount may seem high, but I encourage you to consider the necessary things our daughter will need for proper care and comfort during her stay. Ben and I NEVER ask for help. We will do anything possible to avoid needing to ask for help, but this is just not something we could have ever planned or budgeted for.
We will need:
• A flight there $200
• A flight home $400
• Rental car for ten days $1200
• Food for Teagan and myself $300
• Additional funds budgeted for emergencies
Teagan is such a sweet girl. She is outgoing and sassy. She is incredibly smart and playful. But when she is not well, she is not herself at all. And lately that has been the case more and more. We NEED her to see her team in Southern California. No matter what, Ben and I will make this happen for her. We are desperate at this point for help and hoping our friends can possibly help. Even if you just share our daughter’s story.
• Here is a great link for more information on part of her condition- https://www.chop.edu/conditions-diseases/subglottic-stenosis
 
The story of pursuing proper diagnosis and the beginning complications-
Teagan has struggled since birth with episodes of choking and feeding difficulties. For weeks we pressed doctors to look into the problems further, but we were consistently brushed off and told it was "normal". When she was about three months old, she had her first very serious illness, which was unfortunately, the same time her father left for sea for three months. She had retracted breathing, spiking fevers, and her choking escalated to the point she was turning deep red, almost purple during each episode. After the most severe choking episode, she had refused to eat entirely. She was no longer nursing and she had never accepted a bottle, so I knew it was even more serious. I contacted the doctor and they told me to bring her in. They examined her and determined she was severely dehydrated, but something else seemed to be wrong that they couldn't quite pinpoint so they told me to get her to the children's hospital as soon as possible. I raced Teagan there with her older brother.
When we arrived to the emergency room, they immediately took us back and began the process for an IV placement. After 7 tries with four different people, they got one placed. The doctor came in shortly after and told me that he was admitting her right away. He told me that it seemed like a serious upper respiratory infection, but since her oxygen levels were also so low he suspected something more serious.
 
During this hospital stay Teagan would have 11 IV placement attempts, four blown veins, she lost an alarming amount of weight, and it just got worse from there. On the fourth morning of her stay, her doctor came into the room at 6:00am and asked me if I could contact my husband. I explained to him that contact was limited because he was at sea and the color flushed from the doctor's face. I was also terrified at this point. The doctor told me that he would start the necessary emergency paperwork to get her father home "just in case". I'll never forget those words. I quickly dialed the Red Cross Emergency contact line while staring at my pale, tiny little girl in her metal hospital crib. After an hour the doctor came back and told me that the emergency request letter had been sent and that he hoped my husband made it home. The following day and a half lead to Ben eventually flying home to see his little girl hooked up to an IV and a feeding machine. Despite several attempts with physical therapists, she was still refusing to nurse. The medical team requested an NG tube be placed so she could come off of the IV.
 
 
Finally after almost 10 days in the hospital, Teagan was discharged with her feeding tube. She had only improved enough that the doctors felt I was capable of managing her feeds at home. But we left the hospital with no more answers than when we entered.
 
Only three weeks later, Teagan ended up being admitted again with yet another serious illness that came on rapidly and hit her pretty hard. She had once again started choking, her fevers were spiking, she had retracted breathing, and she was refusing to nurse. During this stay, our concerns were FINALLY heard! Her new team of doctors pushed for further examination beyond the routine IV and oxygen monitoring. They scheduled her for a swallow study which revealed a few new answers. But that wasn't the end.
The months that followed had us in and out of physical therapy appointments, blood tests, swallow studies, GI appointments, and one very important clinic that gave us all the answers we needed, the Aerodigestive clinic. This clinic was a life saver for Teagan. An aerodigestive clinic is a day long event with a team of doctors and specialists that includes a dietitian, a pulmonologist, gastroenterologist, neurologist, a physical therapistand one of the nations leading pediatric otorhinolaryngologist.
 
Her final diagnosis was a malformed epiglottis that lead to additional epiglottis weakness and stage 2 Congenital Subglottic Stenosis (51-70% airway closure). Subglottic stenosis (SGS) is a narrowing of the airway below the vocal cords (subglottis) and above the trachea. Congenital subglottic stenosis occurs as a rare birth defect and may be associated with other genetic syndromes and conditions. The airway remains narrow because the airway cartilage did not form properly before birth. This condition makes contracting an illness especially dangerous because it does not leave much room for throat swelling or irritation. A healthy person typically has throat swelling with a cold or upper respiratory illness and their throat can accommodate for that swelling. Teagan’s airway has such high reactivity that even a simple common cold can cause serious problems for her.
 
Our plead for help-
Since moving to Washington in January, Teagan has had four serious illnesses which have all landed her in the hospital for more thorough evaluation and care. We thought her condition would improve over time, but unfortunately, it has not. She still has days when she struggles to eat properly, she chokes every time she drinks water, every meal is a risk of choking, she is now anemic, and she is not properly gaining weight.
I contacted her team of specialists in SoCal last week and let them know about our rising concerns for Teagan’s condition and they told us that we need to get her to San Diego for care urgently. She is already scheduled for a three stage scope with a flexi scope and a rigid scope which is a fully sedated procedure in the OR with general anesthesia, she will have a full swallow study with radiology, she will go through the Aerodigestive clinic again to reevaluate any possible changes to her condition, and her team will decide if she needs to be admitted for further care or even potential airway surgery.
Our requested amount may seem high, but I encourage you to consider the necessary things our daughter will need for proper care and comfort during her stay. Ben and I NEVER ask for help. We will do anything possible to avoid needing to ask for help, but this is just not something we could have ever planned or budgeted for.
We will need:
• A flight there $200
• A flight home $400
• Rental car for ten days $1200
• Food for Teagan and myself $300
• Additional funds budgeted for emergencies
Teagan is such a sweet girl. She is outgoing and sassy. She is incredibly smart and playful. But when she is not well, she is not herself at all. And lately that has been the case more and more. We NEED her to see her team in Southern California. No matter what, Ben and I will make this happen for her. We are desperate at this point for help and hoping our friends can possibly help. Even if you just share our daughter’s story.
• Here is a great link for more information on part of her condition- https://www.chop.edu/conditions-diseases/subglottic-stenosis