- M
- M
- M
Tanya's Surgical History
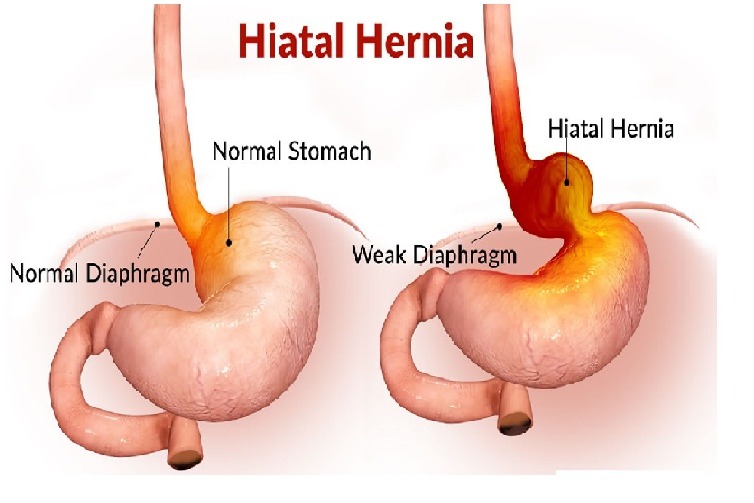
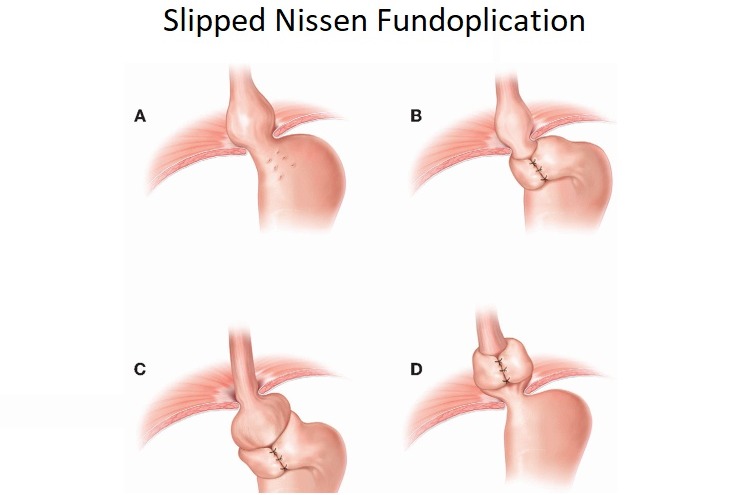
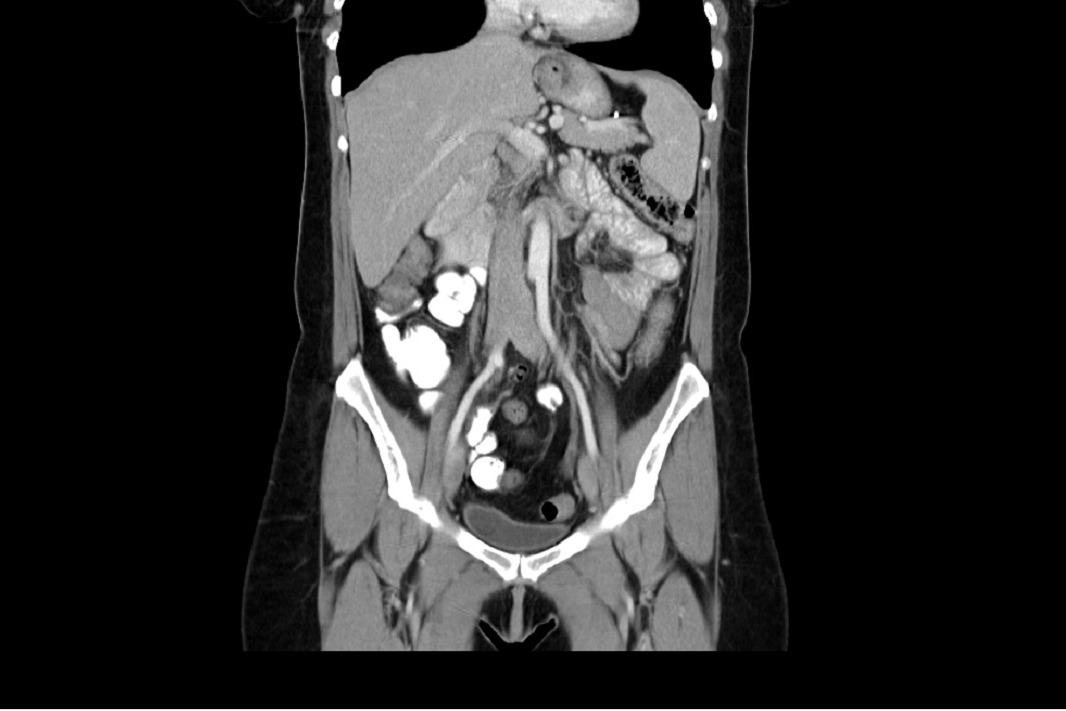
Back in January 2004 I was diagnosed with a large Hiatal Hernia with extreme GERD I then had a laparoscopic Nissen Fundoplication to try and repair this. After the surgery I still felt the sliding up and down motion and found it hard to breathe. I then went back to the surgeon that repaired it and he said it was fixed. I knew It wasn’t right, so I went and searched for other doctors. I found a doctor out of state and he also said I did not have a Hiatal Hernia. I told him I had “A knocking below my sternum” and so he removed half of it this left a Ventral and Incisional Hernia and I still felt an up and down motion leaving me extremely short of breath. I then found another G.I. doctor who found the problem. I had a large Sliding Hiatal Hernia at the 35cm at the E.G. Junction with the Nissen intact. He referred me to a surgeon who confirmed a Ventra Hernia with many adhesions. He never repaired the Hiatal Hernia, but the mesh and adhesion removal helped, and I’ve been functional for 14 years. However, I started working at a wholesale club where I had to twist and bend while lifting heavy things. At the same time, I contracted Bronchitis and I coughed a lot and gagged. I felt something pop and then all my symptoms began. I was able to get a surgeon right a way who did a CAT Scan. The CAT Scan showed a large Ventral and Abdominal Wall Hernia. My stomach, liver, and intestines were protruding outside my Ventral and abdominal wall. The next day they performed emergency surgery. I had my original paperwork from 2004 but they refused to see it. They opened me up and put mesh in the Ventral and Abdominal Wall. This seem to only make my breathing and sliding of my Hiatal Hernia worse. They said I did not have/ did not see a Hiatal Hernia. This seems impossible because they don’t just magically disappear. A week and a half post-surgery every time I breathe or talk it feels like my stomach is moving up and down and slamming into the mesh they placed in the Ventral area. I am unable to eat, sleep, or breath very well. I do not have any quality of life because I am too out of breath and this big bulge comes up when I breathe. I have told them of my symptoms, but the surgeon says he will not do anything until the surgery heals. I feel helpless and feel with every breathe I am going to die. I can’t eat so I am very weak. I need help fast and I don’t know what to do.
Post-Op 2019:
A life saving operation was performed recently and solved a Ventral Hernia and Abdominal Wall Hernia but Nissen Fundiplocation/Hiatal Hernia was untouched and unacknowledged which amounts to 100,000.00 just for initial charge not including hospital stay and any other various charges here soon. Unheased the liver, stomach, intestines, as they we intertwined. Which is why immediate Life-Threatening surgery was performed. We were discharged with 4 tubes still in the stomach area and staples from sternum through/ 1 inch past the belly button which makes maintenance a continuous 24/7 task to keep sanitary along with medications, contacting agencies such as Human Arc, following up with Medicare, find a doctor in the area willing to acknowledge and re-operate to solve the Nissen Fundoplication soon as we wait a second week to remove the 4 tubes. This has made every second of every day uncertain and continually asking what is right? Who do we see? What is next? Why must every waking second be difficulty and pain? Every minute has counted. Post-Op symptoms include but are not limited to: Further problem breathing, new mesh feels displaced and is rather large, and severe acid reflux preventing most solid foods, on and off numbness of the stomach area. Thus far she has been restrained to night shirts, mostly sitting and laying flat down, and inability to be seen/managed publicly and hindering day-to-day activities.
About Tanya
Tanya is a divorced mother with a 17 year old son, and her condition has become debilitating to the point that she cannot work or provide for her family. Even buying basic necessities such as food and water have become a challenge for Tanya without work, and it is putting a lot stress on her and her family. Her son feels obligated to drop out of school to provide for his mother, and has been deeply distraught over the implications of the hernia. Tanya does not have insurance and even affording a visit to the specialist is a hurdle for her and her son.
Current Goal:
To give Tanya Anderson full and healthy life!!!
Any donations, thoughts, medical advice, and prayers would be greatly appreciated and help Tanya and her son pay for doctors visits, surgery, and any other expenses necessary for her treatment. We have an appointment with her old Dr in Staten Island, NY on the 20th for an EGD and a surgeon also Staten Island the 22nd. We need fund for transportation, visits, and own payment for surgery. Reach out to us at [email redacted]
Please help us with connecting to a good doctor or surgeon that will fix these things, we don't have many long connected doctors. The internet can only do so much. Anything can be said and taken for the truth. We are willing to go to any state if we can. Whatever it takes to save a life.
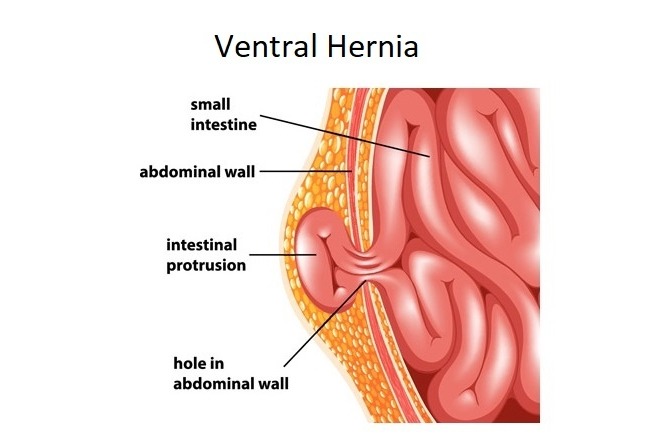
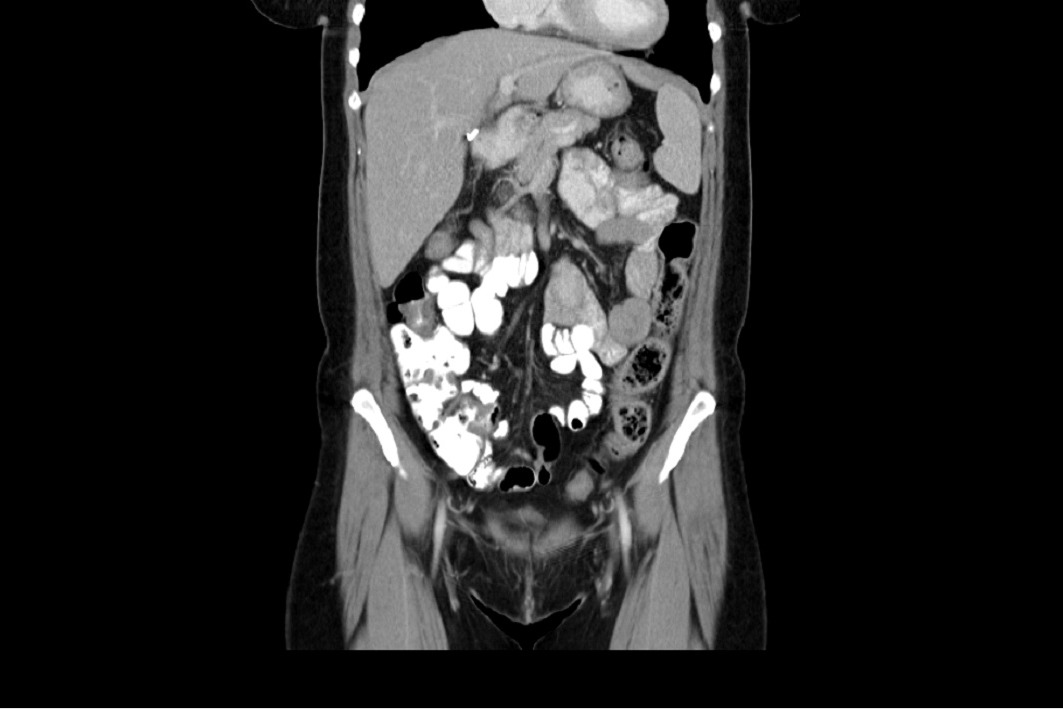
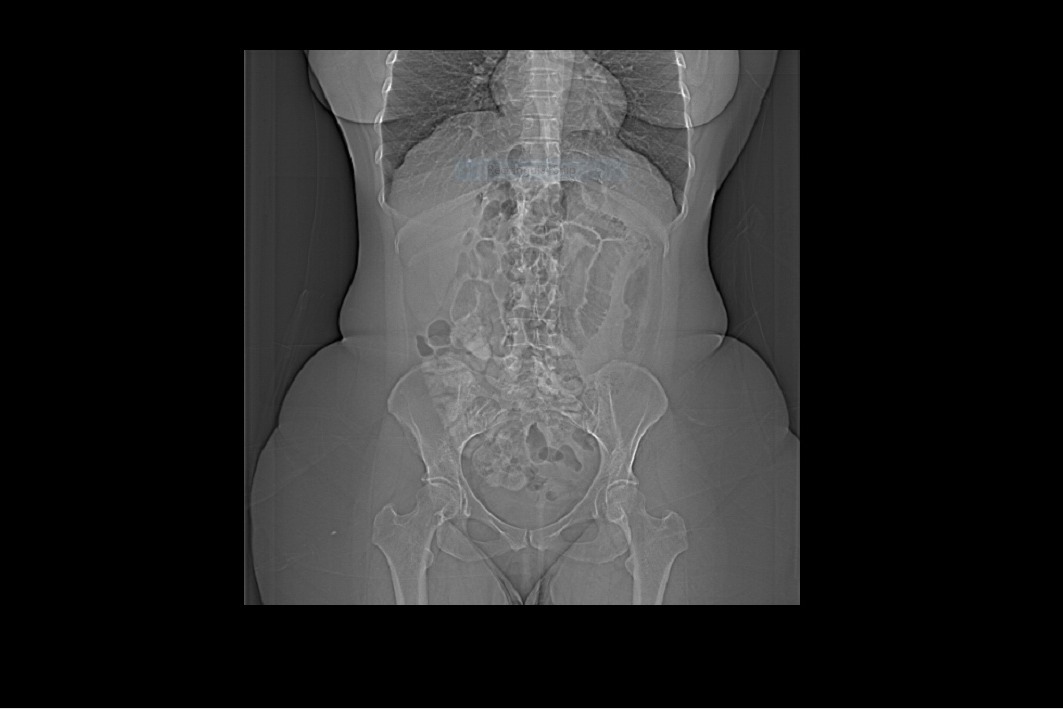
Ventral Hernia v
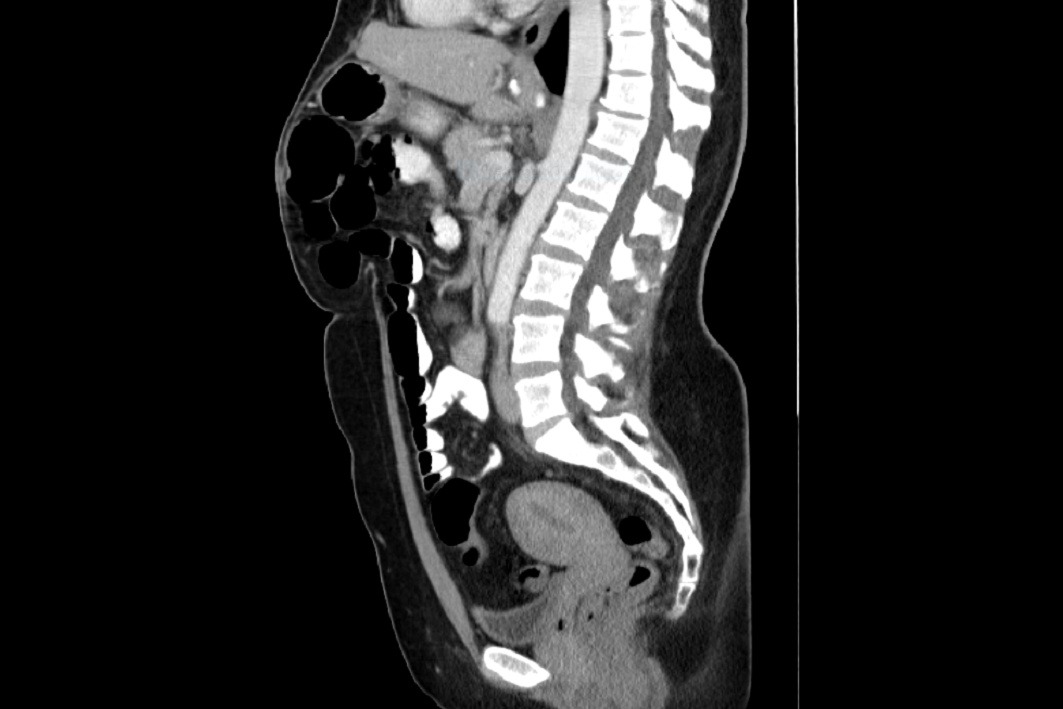
Ventral Hernia v
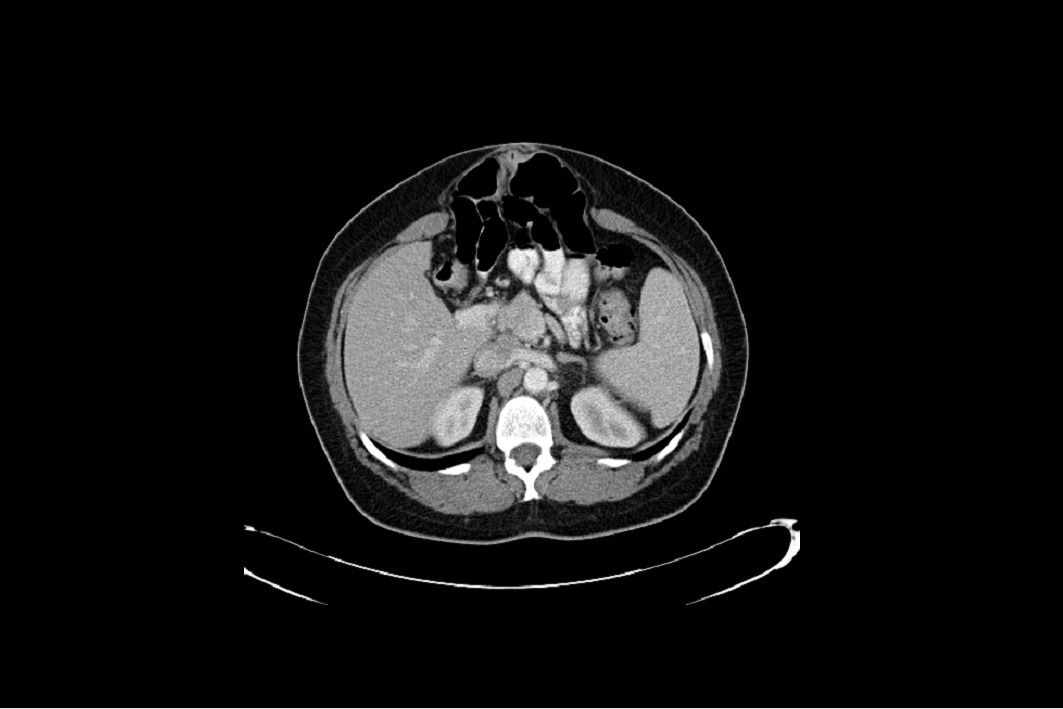
Back in January 2004 I was diagnosed with a large Hiatal Hernia with extreme GERD I then had a laparoscopic Nissen Fundoplication to try and repair this. After the surgery I still felt the sliding up and down motion and found it hard to breathe. I then went back to the surgeon that repaired it and he said it was fixed. I knew It wasn’t right, so I went and searched for other doctors. I found a doctor out of state and he also said I did not have a Hiatal Hernia. I told him I had “A knocking below my sternum” and so he removed half of it this left a Ventral and Incisional Hernia and I still felt an up and down motion leaving me extremely short of breath. I then found another G.I. doctor who found the problem. I had a large Sliding Hiatal Hernia at the 35cm at the E.G. Junction with the Nissen intact. He referred me to a surgeon who confirmed a Ventra Hernia with many adhesions. He never repaired the Hiatal Hernia, but the mesh and adhesion removal helped, and I’ve been functional for 14 years. However, I started working at a wholesale club where I had to twist and bend while lifting heavy things. At the same time, I contracted Bronchitis and I coughed a lot and gagged. I felt something pop and then all my symptoms began. I was able to get a surgeon right a way who did a CAT Scan. The CAT Scan showed a large Ventral and Abdominal Wall Hernia. My stomach, liver, and intestines were protruding outside my Ventral and abdominal wall. The next day they performed emergency surgery. I had my original paperwork from 2004 but they refused to see it. They opened me up and put mesh in the Ventral and Abdominal Wall. This seem to only make my breathing and sliding of my Hiatal Hernia worse. They said I did not have/ did not see a Hiatal Hernia. This seems impossible because they don’t just magically disappear. A week and a half post-surgery every time I breathe or talk it feels like my stomach is moving up and down and slamming into the mesh they placed in the Ventral area. I am unable to eat, sleep, or breath very well. I do not have any quality of life because I am too out of breath and this big bulge comes up when I breathe. I have told them of my symptoms, but the surgeon says he will not do anything until the surgery heals. I feel helpless and feel with every breathe I am going to die. I can’t eat so I am very weak. I need help fast and I don’t know what to do.
Post-Op 2019:
A life saving operation was performed recently and solved a Ventral Hernia and Abdominal Wall Hernia but Nissen Fundiplocation/Hiatal Hernia was untouched and unacknowledged which amounts to 100,000.00 just for initial charge not including hospital stay and any other various charges here soon. Unheased the liver, stomach, intestines, as they we intertwined. Which is why immediate Life-Threatening surgery was performed. We were discharged with 4 tubes still in the stomach area and staples from sternum through/ 1 inch past the belly button which makes maintenance a continuous 24/7 task to keep sanitary along with medications, contacting agencies such as Human Arc, following up with Medicare, find a doctor in the area willing to acknowledge and re-operate to solve the Nissen Fundoplication soon as we wait a second week to remove the 4 tubes. This has made every second of every day uncertain and continually asking what is right? Who do we see? What is next? Why must every waking second be difficulty and pain? Every minute has counted. Post-Op symptoms include but are not limited to: Further problem breathing, new mesh feels displaced and is rather large, and severe acid reflux preventing most solid foods, on and off numbness of the stomach area. Thus far she has been restrained to night shirts, mostly sitting and laying flat down, and inability to be seen/managed publicly and hindering day-to-day activities.
About Tanya
Tanya is a divorced mother with a 17 year old son, and her condition has become debilitating to the point that she cannot work or provide for her family. Even buying basic necessities such as food and water have become a challenge for Tanya without work, and it is putting a lot stress on her and her family. Her son feels obligated to drop out of school to provide for his mother, and has been deeply distraught over the implications of the hernia. Tanya does not have insurance and even affording a visit to the specialist is a hurdle for her and her son.
Current Goal:
To give Tanya Anderson full and healthy life!!!
Any donations, thoughts, medical advice, and prayers would be greatly appreciated and help Tanya and her son pay for doctors visits, surgery, and any other expenses necessary for her treatment. We have an appointment with her old Dr in Staten Island, NY on the 20th for an EGD and a surgeon also Staten Island the 22nd. We need fund for transportation, visits, and own payment for surgery. Reach out to us at [email redacted]
Please help us with connecting to a good doctor or surgeon that will fix these things, we don't have many long connected doctors. The internet can only do so much. Anything can be said and taken for the truth. We are willing to go to any state if we can. Whatever it takes to save a life.






Ventral Hernia v

Ventral Hernia v


