(scroll down for updates :) )
Dear friends, family, and compassionate individuals,
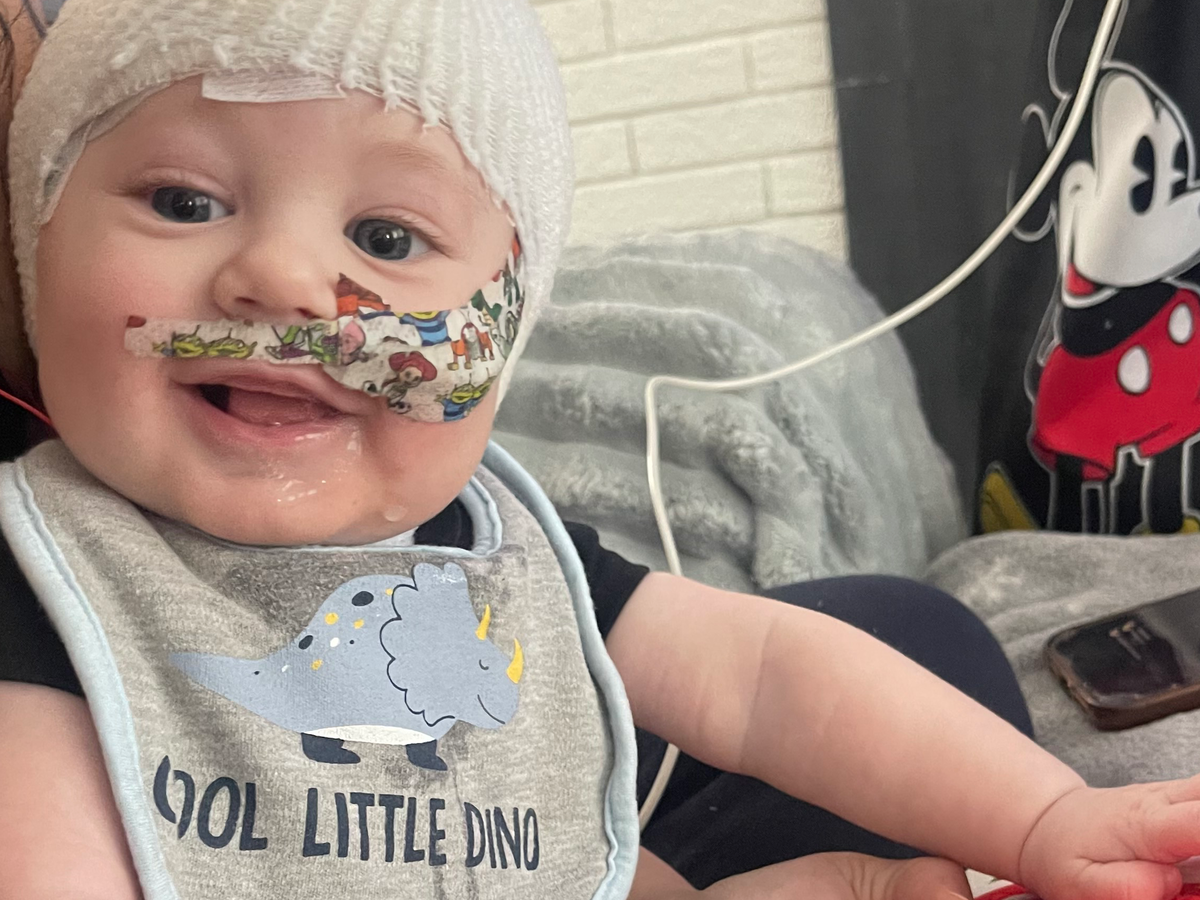
We are reaching out to you today to ask for your help and support for Grayson and his mother, Alexis, as they navigate an incredibly challenging and uncertain medical journey.
Grayson’s Journey So Far:
Grayson was born on July 26th at 39+3 weeks by a repeat c-section without any complications. However, Grayson soon faced feeding difficulties, including problems with sucking, swallowing, latching, gagging, and forming a seal, which were first observed shortly after birth. Despite these issues being flagged in the hospital, Grayson was discharged at 24 hours and continued to struggle with feeding at home.
In September, Grayson was referred to his GI specialist due to worsening feeding issues, reflux symptoms, and slow weight gain, and was diagnosed with severe GERD. However, his feeding difficulties persisted. By October, his condition had worsened to the point where he was able to take only a small amount of food before tiring out completely. Grayson’s GI specialist recommended further evaluations, including an assessment by speech-language pathologists and a swallow study.
Ongoing Struggles and Hospital Admissions:
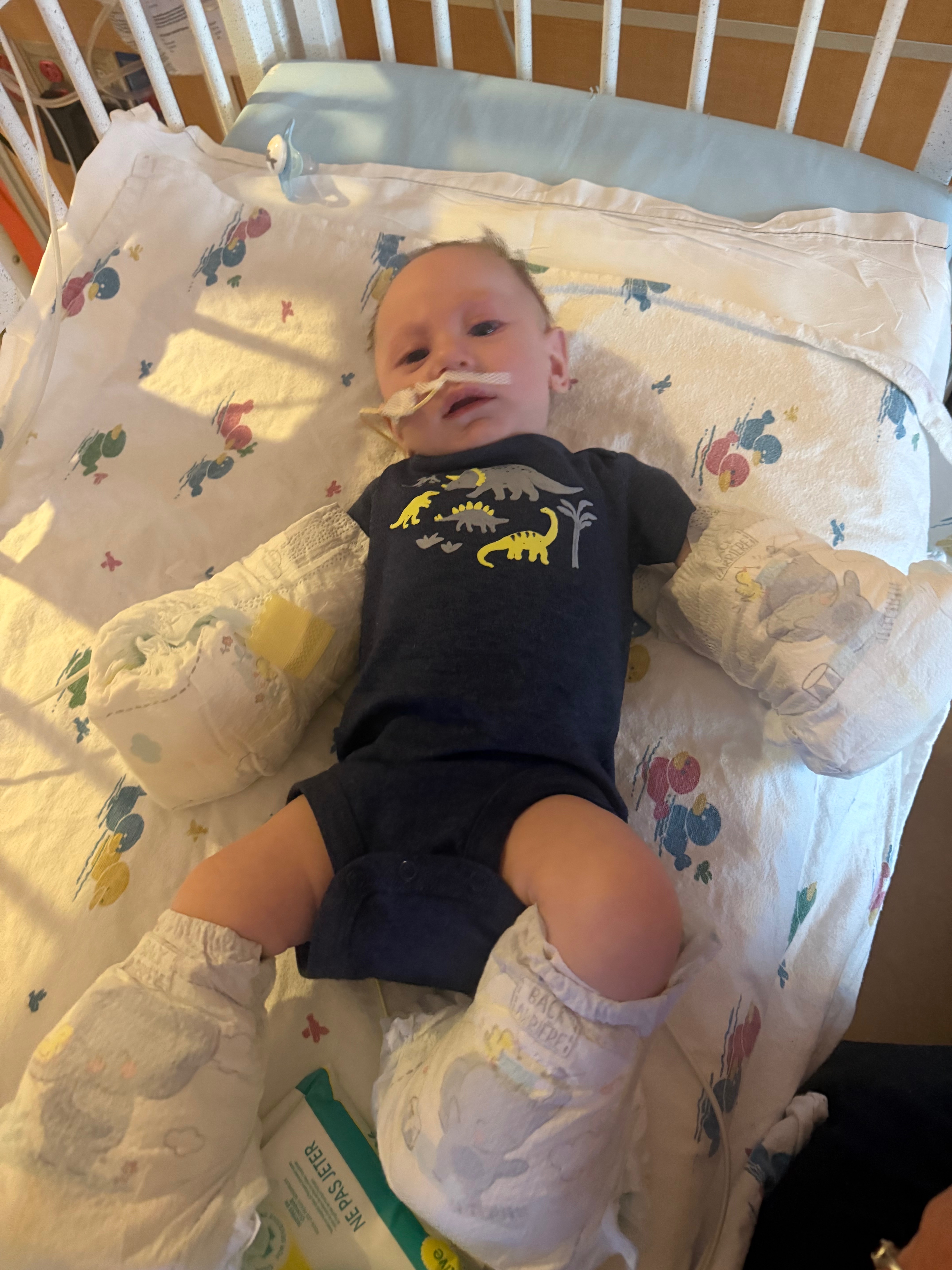
While waiting for the swallow study, Grayson was frequently seen in the ER for dehydration and malnourishment checks. Despite his struggles, Alexis has worked tirelessly, feeding him every hour to keep him just above the dehydration line. The first swallow study revealed significant delays in Grayson’s oral phase of swallowing, and additional symptoms such as low muscle tone, right-sided weakness, and facial asymmetry became more pronounced over time. Grayson was evaluated by multiple specialists, including his first speech-language pathologist, who diagnosed him with a high, sensitive palate, retrognathic mandible, and lip tie. She recommended feeding therapy, occupational therapy, physical therapy, and ultimately a feeding tube to ensure adequate nutrition. During this evaluation, Grayson was found to be developmentally delayed, scoring in the 1–3 month range in most categories at 5 months old. As a result, his care team decided to move forward with the insertion of an NG tube for feeding.
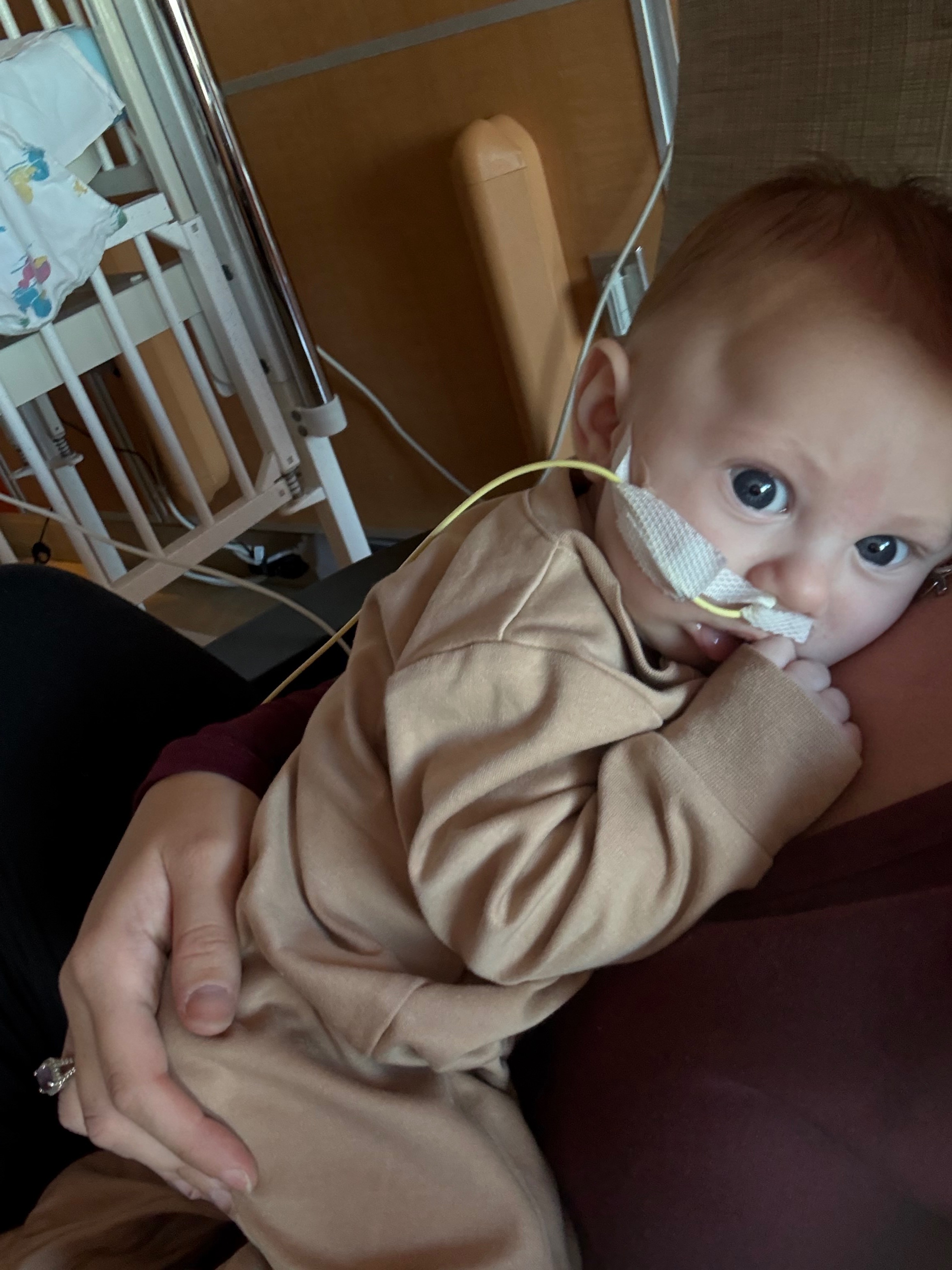
In his first hospitalization, Grayson’s NG tube was placed, and his medical team took the time to teach Alexis how to manage his feeding needs, as she has had to act as his primary caregiver due to his insurance not providing in-home nursing care. The hospitalization lasted longer than expected, as concerns over a potential genetic condition led to consultations with specialists across several fields, including neurology and genetics.
Genetic Diagnosis and Further Testing:
During his second hospitalization, Grayson underwent extensive tests, including a brain MRI to rule out tumors or masses. His swallow study showed that he continued to struggle with basic feeding mechanics despite trying various bottles and positions. His team of doctors became increasingly concerned about his neurological development, and genetic testing revealed a CACNA1S gene mutation, a condition that could affect his skeletal muscles, leading to muscle weakness and other complications.
Grayson also started having seizure-like episodes, which were captured on video and reviewed by his neurologist. He was admitted once again for EEG monitoring, which failed to provide definitive answers. Further testing revealed that Grayson has a congenital heart defect, and his eye exam showed no anatomical issues causing his head tilt. The speech-language pathologist confirmed that Grayson would not be able to drink from bottles due to the severity of his feeding challenges. The current goal is to maintain a positive oral sensory experience and hopefully transition him to solids in the future.
The Need for Ongoing Care and Surgery:
Grayson’s care team recommended that he transition from the NG tube to a more permanent G-tube for feeding, and this surgery was scheduled for January 16th. In preparation for this, Grayson was referred to intensive outpatient feeding therapy once his G-tube was in place. Additionally, his neurologist has ordered a 72-hour at-home EEG test, and he was also referred to the Kennedy Krieger Institute for a second opinion regarding his genetic mutation and to evaluate whether additional conditions might be causing his issues. The appointment at Kennedy Krieger involved a thorough examination of Grayson’s medical history, leading to a diagnosis of a neurological disorder rather than a muscular issue. Grayson will also undergo further genetic testing for conditions not covered by his previous test, including Prader-Willi syndrome.
Current and Future Care:
Grayson is in weekly physical therapy, occupational therapy, and speech therapy, and is receiving services through AACPS Infants and Toddlers until he turns 3. He also requires 2–3 daily sessions of exercises for oral sensory and motor skills, as well as physical exercises to address his low muscle tone, motor skills, and developmental delays.
Grayson’s 72-hour EEG was scheduled for the second week of January, and he has follow-up appointments with his neurologist, geneticist, and other specialists. The results of the genetic testing may take up to 4 months, and Grayson’s care team will continue to adapt his treatment plan based on his evolving needs.
Alexis’s Role:
Throughout this journey, Alexis has been an unwavering support for Grayson, providing 24/7 care and managing his medical needs. As a single mom of two children, Alexis has had to take time off of work to care for Grayson full-time, and she’s been doing so without in-home nurse care, as his insurance does not cover it. Despite the immense challenges she faces, Alexis is not one to ask for help, so I am stepping forward to ask on her behalf for support. How You Can Help:
Grayson’s journey has been filled with uncertainty, but with your support, we can provide him with the resources and care he needs to thrive.
The funds raised will go directly toward:
* Medical expenses (including surgeries, testing, and hospital stays)
* Feeding tube surgery and follow-up care
* Therapy and developmental services (including physical, occupational, and speech therapy)
* Daily medical needs (including feeding tube management and 24/7 care)
* Future treatments and interventions as Grayson continues his medical journey.
Grayson’s Current Diagnoses:
* Feeding Difficulties: Issues with sucking, swallowing, and latching.
* Risk of Dehydration: Due to poor fluid intake.
* Failure to Thrive: Struggles to gain weight and grow.
* Congenital Heart Defect: Heart issues present from birth.
* Abnormal Movements: Jerky, involuntary movements.
* Small Anterior Fontanelle: May signal developmental issues like microcephaly.
* Early Closure of Fontanelle: Early fusion of skull bones, affecting brain growth.
* Micrognathia: Small lower jaw, affecting feeding and speech.
* High Arched Palate: Narrow, elevated roof of the mouth.
* Oropharyngeal Dysphagia: Difficulty swallowing, leading to choking.
* Hyperactive Moro Reflex: Exaggerated response to sudden movements.
* Facial Asymmetry: Significant differences in facial features.
* Positional Plagiocephaly: Flattened spot on the skull due to positioning.
* Gastroesophageal Reflux Disease (GERD): Chronic acid reflux.
* Hyperkalemia: Elevated potassium levels in the blood.
* Congenital Myopathy: Genetic muscle disorder causing weakness.
* Congenital Malformation of Skull and Face Bones: Birth defects affecting head and face.
* Congenital Hypotonia: Low muscle tone affecting motor skills.
* Monallelic Mutation of CACNA1S Gene: Genetic mutation affecting muscle calcium channels.
We understand that these are trying times for many, but any contribution, no matter how small, will make a world of difference for Grayson and Alexis. If you’re unable to contribute financially, please consider sending your thoughts and prayers, as they are needed and deeply appreciated as well.
Please consider donating, sharing, and supporting this beautiful little boy and his family as they fight for his health and well-being.
Thank you for your kindness, support, and generosity. ❤️
———————————————
UPDATE: January 30, 2026
———————————————
Grayson has been sick with a virus, which then turned into an ear infection. Because of Grayson’s conditions, illnesses affect him much more than they affect most children. The progress he had been making has now been lost. For example, Grayson was previously able to sit with front-hand support for a few seconds. Now, he cannot sit at all and immediately flops over. He currently cannot self-support in any position, including holding his head up. He is presenting almost like a newborn again in terms of strength and control.
At his neurology appointment, his specialist explained that with his conditions, regression is normal. However, we won’t always know whether he will regain skills after an illness or if he will have to relearn them completely.
Right now, we know Grayson has a neurological condition—the question is what kind and from what. Today, Grayson had an appointment with the genetic counselor at Kennedy Krieger Institute. She emphasized that Grayson’s neurological condition is likely due to a genetic or chromosomal issue, not anything caused by birth or pregnancy.
The plan is to begin testing for Prader-Willi syndrome, followed by Optimal Genome Mapping (OGM) once he is fully processed into the Rare and Expensive Case Management (REM) program. Grayson’s neurologist is currently working on getting him registered for REM.
Grayson qualifies for the REM program due to his microcephaly, a neurological birth defect where a baby’s head is significantly smaller than expected, indicating improper brain development. This condition is lifelong and can be caused by genetics, infections, or environmental factors. Outcomes vary from mild delays to severe developmental issues, seizures, and shortened life expectancy.
OGM testing will help identify structural DNA variants by visualizing long single molecules, offering 20,000 times greater resolution than traditional karyotyping. It detects large insertions, deletions, inversions, and translocations.
Being in the REM program will give Grayson access to any hospital in Maryland, including Johns Hopkins Hospital and University of Maryland Medical Center—the two hospitals he previously could not access. REM also covers advanced testing like OGM and other difficult-to-approve diagnostics.
The genetic counselor explained that we may never know the exact cause or type of Grayson’s neurological condition, how it will affect him long-term, or what to expect as he grows. We may continue discovering new things about his condition over time. She emphasized that I am doing everything right—getting him into top specialists and all appropriate therapies at just six months old.
For now, we remain in the “question mark phase” while waiting for the Prader-Willi test results and for Grayson to be fully processed into the REM program so additional testing can be scheduled.
⸻
UPDATE: February 15, 2026
—————————————————————
Grayson’s test results for both Angelman syndrome and Prader-Willi syndrome came back negative. Once he completes REM processing, he will move on to OGM testing.
Grayson’s developmental progress continues to be like driving up and down hills—constant regression followed by small steps forward, then regression again. His head growth is still slowing down due to microcephaly, meaning his brain is not growing properly. His soft spots are almost completely closed because of the improper brain growth. This condition is lifelong and causes intellectual and developmental delays, as well as the possibility of a shortened life expectancy.
Grayson’s weight has continued dropping over the last few weeks. He is still only 15.5 pounds at almost seven months old. When his nutritionist increased his feeding volume, he could not tolerate it, so it had to be lowered again. Once his stomach adjusts, his nutritionist will create a new feeding plan by the end of the week. We’re hoping this helps Grayson begin gaining weight again.
His right-sided weakness and head tilt have worsened this past week. During physical therapy, it was also noted that Grayson cannot multitask, and he now cannot tolerate tummy time—even when adjustments are made to reduce pressure from the G-tube, confirming it’s not tube-related.
Grayson has had a cold this past week and is also cutting his first two teeth, which contributes to further regression. This explains why his right-side weakness and other issues have worsened again.
Grayson had his intensive feeding therapy evaluation this week. They expect him to need intensive feeding therapy for many years. His first goal is to eat one full medicine cup of purée in a single sitting within 16 weeks in order to qualify for another swallow study. So our four-month goal is simply to qualify for a new swallow study.
⸻
UPDATE: February 18, 2026
—————————————————————
Grayson’s current main diagnosis is a lifelong neurological disorder. We are still trying to determine the exact type. His specialists have stated that we may never know the specific disorder since many neurological disorders are still unidentified.
Here is what we do know so far:
• Grayson’s neurological condition is causing multiple symptoms and related conditions.
• Microcephaly prevents his head—and therefore his brain—from growing properly. This is lifelong and may shorten his life expectancy. It causes intellectual delays, severe developmental issues, and possible seizures.
• Grayson also has a congenital malformation of the skull and facial bones, a birth defect that affects his bone and skull structure. This causes breathing issues, feeding issues, vision problems, changes to his head shape, and further restricts brain growth.
• His neurological disorder is causing right-sided weakness, which affects the right side of his arm, hand, leg, face, head, and neck. This impacts his head control, motor control, and daily tasks.
• Grayson has congenital hypotonia, which causes extremely low muscle tone. His muscles are very floppy—more like a rubber band than a firm support structure. This affects his posture, strength, and overall mobility.
These are only some of the challenges caused by Grayson’s neurological disorder. He will require lifelong medical care and therapies. Grayson will also need his feeding tube (G-tube) for the foreseeable future to eat and drink.
Grayson may never crawl, walk, talk, eat by mouth, or have the same future other children do. Some of his conditions significantly shorten life expectancy.
——————————————
February 22nd, 2026 Update
———————————————
Grayson’s sister, Abrianna, is now also undergoing genetic testing. She was recently diagnosed with ADHD and is currently being evaluated for autism after both her behavioral therapist and pediatrician expressed concerns that she may be on the spectrum. Abrianna has also been referred to occupational therapy for her sensory and OCD-related needs. Her genetic testing will also support Grayson’s testing, as her results may help provide more clarity for his case.
Between both Grayson’s and Abrianna’s therapies and appointments, we currently have something scheduled five out of five weekdays every week. Abrianna has behavioral therapy on Mondays. Grayson has physical therapy on Tuesdays. Both children have occupational therapy on Wednesdays. Grayson has intensive feeding therapy on Thursdays and additional physical therapy sessions on Fridays. Outside of these therapy appointments, we also attend numerous doctor and specialist visits for Grayson, as well as appointments for Abrianna, who has her own set of specialists.
This demanding medical and therapy schedule is another reason Alexis cannot work. In addition to providing around-the-clock care for Grayson, she must attend all therapy sessions and appointments for both children. She also manages Grayson’s case entirely on her own—making phone calls, sending emails, placing supply orders, updating all of Grayson’s specialists, and keeping everyone informed. Insurance does not provide a case manager or nurse until Grayson is fully processed into the REM program, and we are still waiting for an update on that.
Grayson has an upcoming appointment at the Kennedy Krieger Institute within the next few weeks with his team of specialists to determine the next phase of his testing. He also has an appointment with his neurosurgeon to discuss concerns about his slowed head growth due to his brain’s progressively slowed development. In addition, Grayson will have his first G-tube change this coming week. Alexis will be performing the procedure in the doctor’s office under supervision and will handle all future G-tube button changes at home. Despite everything already on her plate, Alexis has completed all required medical training and received the necessary certifications to ensure she can safely and properly care for all of Grayson’s medical needs.
——————————
Funds will go toward essential medical and adaptive supplies, including but not limited to:
• Adaptive feeding items for feeding therapy
• Adaptive chairs, wheelchair, adaptive stroller, adaptive stander, gait trainer, Nobile stander
• Syringes, G-tube covers, Mepilex Transfer, gauze
• Feeding tube extensions, syringe caps, medical Q-tips, gloves, Grip-Lock, antibacterial spray
• Physical therapy equipment for home use
• Adaptive clothing and sewing materials to create adaptive clothing
• Sensory items
• Barrier creams for the G-tube site, stoma powder, Huggy G-tube site covers
• Feeding tube extension cleaning brushes, medical tape
• Specialty bath seat, specialty sit-up seat, Firefly seat, adaptive feeding seat
• Adaptive communication devices
• Leg and foot braces
• Floor sitter, feeding backpacks, transition adapters for feeding tube, pump caddy
• Extra feeding pump bags and extension locks
• Assistance with hospital trip costs and household bills, as Alexis is unable to work due to caring for Grayson, who requires occupational therapy, physical therapy, intensive feeding therapy, and daily medical care five days a week.
————————————-
UPDATE MARCH 27
————————————-
The past few weeks have mostly been a waiting game for calls and messages from Grayson’s team of specialists. Grayson has received two additional diagnoses to add to his already lengthy list. He has been diagnosed with an unspecified mitochondrial metabolism disorder and language regression.
Over the past few weeks, Grayson has unfortunately continued to regress. The weakness on his right side and his head tilt have become much more pronounced. Grayson just turned 8 months old yesterday, and these milestones have been especially hard for me.
Grayson still cannot sit up independently for more than a few seconds to about one minute at most. It’s very rare that I hear a “ma” anymore. He has his own little language that we call his “dolphin language” — he squeals like a little dolphin, and it’s the cutest thing. However, he isn’t able to make many distinct sounds other than “ma,” and even that is only about once a month now.
We are currently waiting to hear from Grayson’s team of specialists about the next steps in his care. I am hopeful that we will hear from them sometime next week.