
The Picture Today
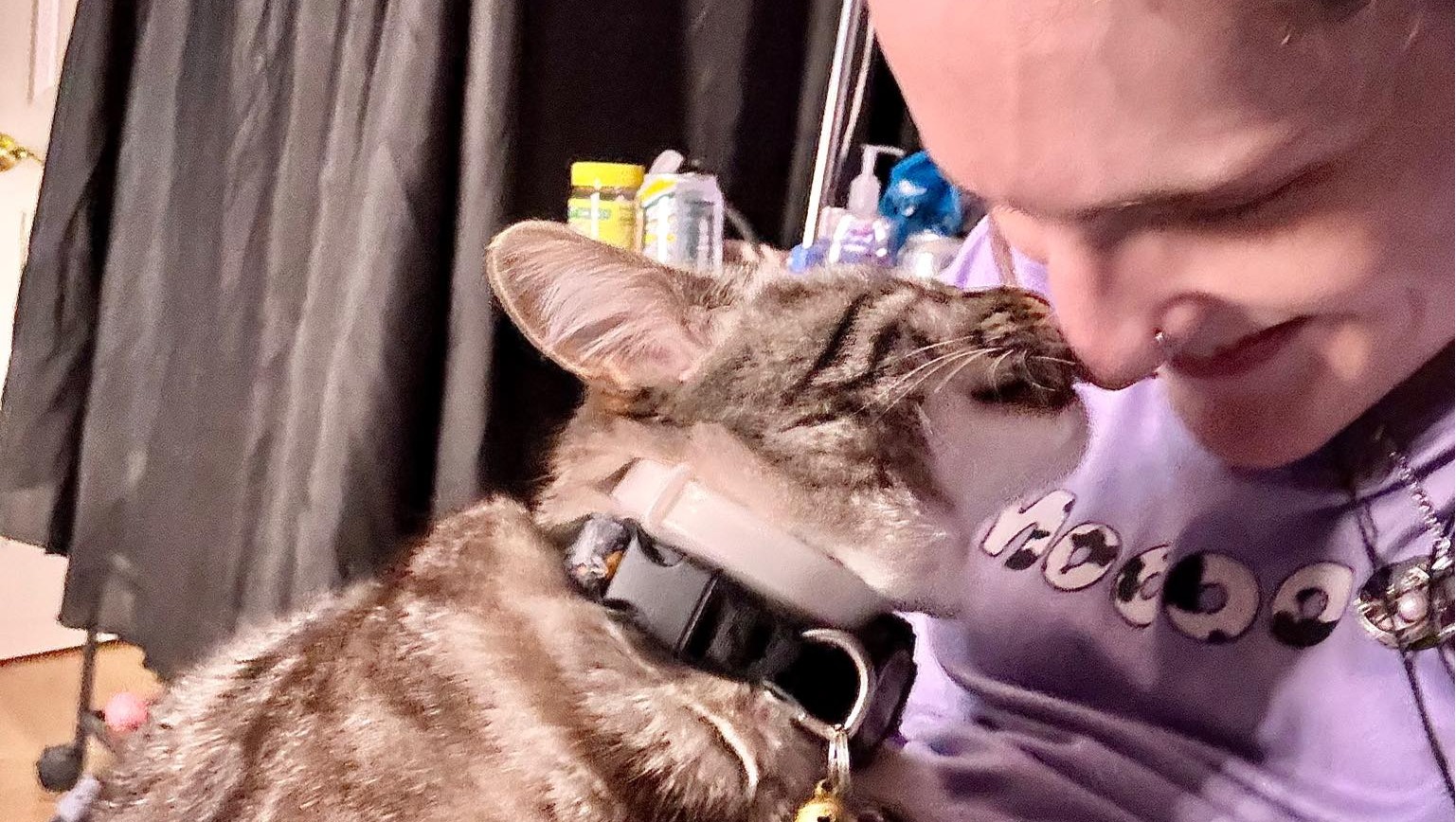
On 03 July 2025, almost exactly a year after being discharged from Yale-New Haven Hospital on palliative care, Ashlinn Erin Collins, with the aid of her medical team, decided that the best option that she had available to her was to transition to hospice care with Vitas Health. Faced with a looming autoimmune motor neuropathy diagnosis, a lack of viable options for curative treatment for her digestive disease, and UnitedHealthcare's decision to not cover outpatient palliative care services, Ashlinn made herself stand face-to-face with fears of death, of disappointing loved ones, of abandoning her feline and ferret kids, and of what people may say or how they may misconstrue her situation.

It was with bravery and strength that Ashlinn handled the sudden news that her options had diminished to going on hospice or returning to 'regular' medicine, where whether she was comfortable or miserable doesn't matter as long as she survives. When the intake nurse clarified that Vitas doesn't provide palliative care services, only hospice, she got more information from him, then made the decision to prioritize a higher quality of life over simply living longer.

Two months have passed since Ashlinn went on hospice. It's been a learning curve for both of us and just about everyone we interact with. Our society is so engrained with the fear of death and perhaps the stigma of dying, especially at a young age, that even when every other option boils down to "You will suffer and die at a point in time that may or may not be more predictable," it can be extremely difficult to choose hospice.
Ashlinn has additional conditioned hurdles because her prescribed identity from a young age was always focused on her being a "survivor" and completely ignorant to whether or not she suffered all along the way. From the day that she was born, there were very valid questions about whether or not Ashlinn would survive and what her future would look like if she did survive. Ashlinn was trained to fight for her life.
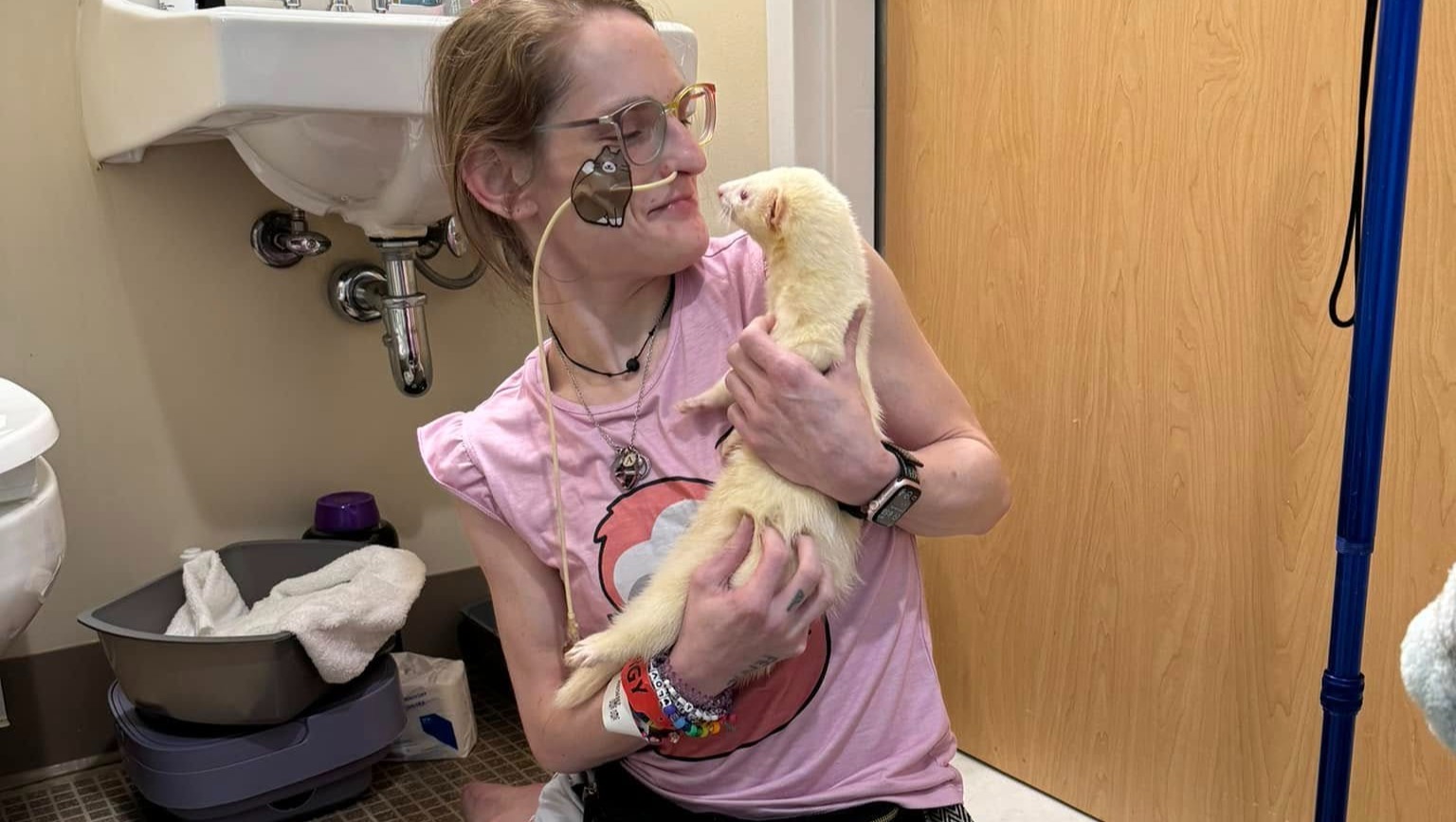
Ashlinn was emotionally led to the idea of hospice because she's tired of being mistreated in the medical field, getting painful procedures and painful symptoms, and needing to babysit the medical professionals that are supposed to be helping her, but when she came to make the decision to go onto hospice care, those painful emotions matched rationality and the facts of her situation perfectly. There are no viable curative options for her intestinal failure, and with the progression of her malnutrition and autoimmune motor neuropathy, she is very, very sick.

Ashlinn eats what she usually doesn't throw up. She does her best, and tries new things as often as she can manage to try to get more nutrition in, but she usually eats an amount that would starve a toddler.
She's losing muscle, losing the ability to, with little to no pain, stand or walk for very long, to sit up for periods more than an hour or so, and to walk up and down a flight of stairs.

The Vitas workers, almost without exception, have been amazing. Whenever a new person comes to see her, they tend to ask questions to verify that she should actually being on hospice at thirty years old. It's never taken them long to figure out that the answer is yes. They seem to struggle more with sometimes giving mixed messages because they don't want to make her feel trapped or tell her that her situation means that she is going to die in the not-so-distant future, but as they get to know her, they learn how to be direct in a way that also comforts her.
It's obviously tragic that the circumstances in Ashlinn's life have led to her being on hospice at thirty years old, but given that they have, I hope that everyone can stand with her the way that I aspire to: With regard to and respect for her autonomy, dignity, and fulfillment.
Looking Forward
Although those who continue to be part of Ashlinn's every day life help as much as they can, the reality is that these are uncertain economic times. Unfortunately, being on hospice can be a very difficult, vulnerable place to be.
I felt compelled to share all of this and to ask for people's support because although she deserves it, Ashlinn is afraid to ask for help. I see every day pain and suffering that I just don't feel is necessary.
Currently, the plan for the money would be to use it as follows:
Companions & Homemakers Services - $11,830 over 6 months
To help with maintaining the household and a clean environment. Ashlinn becomes very stressed by the clutter and the cat hair on the floor and often times will overexert herself to rid herself of the stressor. She really needs someone who is more able to do these things than I am.
The estimate is based on the following projected costs (via Carescout) over a six month period, although there are a lot of difficult to predict factors that could alter this plan, from death to the discovery of more affordable, comparable options.
- Month 1: 4 hours per day, 2 days per week - $1,213/month
- Month 2: 4 hours per day, 2 days per week - $1,213/month
- Month 3: 6 hours per day, 2 days per week - $1,820/month
- Month 4: 6 hours per day, 2 days per week - $1,820/month
- Month 5: 8 hours per day, 2 days per week - $2,427/month
- Month 6: 6 hours per day, 3 days per week - $2,730/month
I wish that I could do more than I'm doing around the house, but with my own chronic illness, I'm very much limited in what I can do in a day, how long I can be on my feet, and how reliable I can be for any given task. I feel bad about it all the time, but no matter how sick Ashlinn gets, no matter how badly I want to take everything taxing off of her plate, no matter how much I try to convince myself that I'm just being lazy--I can't make the effects of my chronic illness go away. As embarrassing as it may feel, I really just need to be frank in that we need some help.
CallToU Pager System - $37.79 (One time purchase) - This pager system comes with two transmitters and two receivers. If Ashlinn needs something from me urgently and I'm on a different floor, she would be able to press a button and the receivers would ring so that I could help her as quickly as possible.
Reyhee Roamer Electric Wheelchair - $999.99 (One time purchase) - An electric wheelchair would allow Ashlinn to be engaged with people and the outside world because she wouldn't need to have the energy to propel herself to do something. That can very well be the difference between being able to participate in holidays and birthdays and staying home.
Ramps and related safety items:
- A ramp to get up the steps and into our home - $139.99
- A ramp to get the wheelchair into and out of the car - $155.99
- Cut resistant gloves - $13.99 - Per reviews on the ramps, they get hot and some have sharp edges.
- Bumper guard - $21.99 - To help stabilize the ramp when loading the wheelchair into the car and to protect the car from scratches.
Drafting chair - $59.11 - To use in the kitchen and bathroom, or where otherwise standing height is required.
Memorial items for select loved ones - $1,065.16
The total cost of these items is $14,586.93. In order to account for unforeseen taxes/fees the fundraiser has been set for a $15,000 goal.
Ashlinn is my best friend, my sister, my platonic life partner. I think I'm more comfortable with death than the average person, but I know that the day that I lose her will be one of the hardest days of my life. I imagine the kids' reactions sometimes--Especially Willow. Ashlinn is going to be so missed, and I only hope that she can experience the best parts of life before she goes.
We appreciate any and all help. I've felt for a long time that all Ashlinn needs is a break - Thank you for any part you play in that.
For another way to support Ashlinn, you can take a look at her Amazon wishlist [here] or get something for the kids on her pet registry [here].
Ashlinn's Story
(through my eyes)
Connecticuter at Large
March 2020 - September 2020
If there is one stroke of luck I've ever had, it was the happenstance of meeting Ashlinn Erin Collins. We became fast friends in Walden/Rockville General Hospital's EDU, and although we each have our share of problems, even the psychiatrist couldn't really recommend against our friendship.
While Ashlinn and I were co-patients, we spent a lot of time chatting, joking around--making our lives as close to tolerable as we could manage during our admissions. I learned that while I lived about forty-five minutes away from Rockville General Hospital, Ashlinn had taken an eighteen hour train ride from North Carolina in March 2020.

I also learned that Ashlinn had lost her spleen'(and 80% of her pancreas) in an accident in 2015, so she doesn't have much of an immune system to speak of. She had managed to travel by train from North Carolina, through Washington, DC, through New York City, New Haven, and Hartford in March 2020 without contracting COVID-19 in March 2020, but I didn't have high hopes for her if she was going to do that again.
On her IV pole, Ashlinn had taped photos of her cat, Aspen. I've always been a cat person, perhaps even a crazy cat person. Ashlinn told me about how she needed to be a better mom for Aspen, and that that's why she knew she needed to go to treatment.
So obviously, I decided I was going to drive her home. We had some fun planning a road trip, but ultimately, Ashlinn always had one main goal in mind, and one thing that kept her grounded no matter how hard things got: She needed to get home for Aspen.

I was discharged in late May 2020 and started doing some preparation for our trip. Towards the end of her admission, she had to be transferred to a medical floor at Manchester Memorial Hospital due to a bowel obstruction and intussusception.* They discharged her on 03 July 2020, but that same night, it was clear that they had prematurely discharged her, and she ended up admitted to Waterbury Hospital to clear up the obstruction before we were able to start heading down south.
* Intussusception - When the bowels 'telescope' in and over themselves.
We took our time driving down to North Carolina. She had never been to New York, so we did a little sightseeing. Otherwise, we just drove a few hours per day, then hung out in air conditioned hotel rooms and talked. We covered a lot in hotel rooms during that trip, but what became immediately clear was that Ashlinn could not go back to the same home environment she'd come from and expect to live.

I wrote up a contract for Ashlinn that said that I would not expect the costs of the trip to be repaid as long as she made a significant effort to move out of the condo that she lived in with her mom. I went down to the hotel business center and printed it out and made her sign it. I didn't know exactly what to expect insofar as how seriously she would take it or what action she would put in while I wasn't there. I was obviously just still getting to know her, because once you understand who she is a little bit more, you understand that if she believes both that something is worth doing and that she has access to everything she needs to do it, she will do it.
When we arrived at her condo in North Carolina, Aspen was sitting at the window looking out into the parking area as if he knew that she would show up any second. He was thrilled to have her back. She raised him from just three weeks old, and they probably saved each other's lives.

I went back to Connecticut, but about a month later, I drove my grandparents to Florida. On the way back to Connecticut, I picked up Ashlinn, Aspen, and the belongings she could fit in my Nissan Altima. We stopped for a few nights in Virginia so that she could spend some time with her now-ex-fiancée, Rachel, then we headed back to Connecticut. We planned for her to move temporarily into an Extended Stay while we found an apartment for her.

October 2020 - July 2021
One of the first things that Ashlinn told me about herself was, "It's Murphy's law over here." We spent the last night of our trip in Pennsylvania, planning to drive the final leg to the Extended Stay in Meriden, CT the next day. She started feeling sick, so before we got on the highway in Pennsylvania, we stopped at CVS to buy a thermometer, and she was feverish.
The next day, Ashlinn had to call 911 from the Meriden Extended Stay because she couldn't breathe. She had COVID and shattered lung pneumonia. She forced herself to stay awake all night while hospitalized because the nurses kept suggesting that she go on a ventilator, and she knew that that, for her, would be a death sentence. She was born at twenty-four weeks gestation, weighing just a pound and a half. Her lungs were severely underdeveloped and she was on a ventilator for the first six months of her life. Even when she was able to leave the NICU, she had to be on a breathing monitor at home.
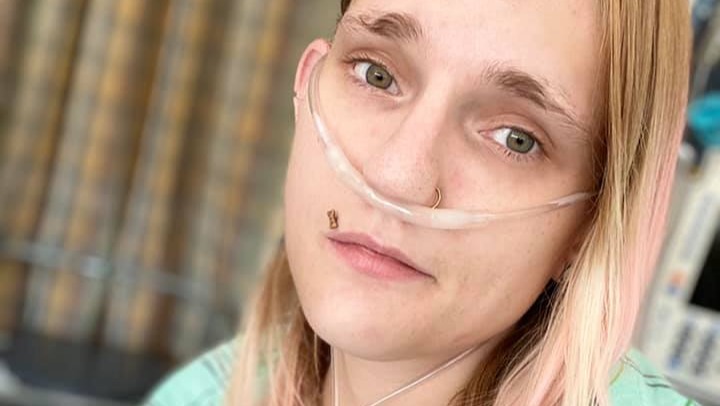
Through sheer tenacity, Ashlinn fought through COVID in October 2020. Before she was able to be discharged, though, her small intestine failed. She was no longer able to tolerate J-tube* feeds, so she had to have a PICC line** placed to receive TPN***. She was told to do bowel rest and to just eat for comfort until she ultimately had surgery to remove scar tissue and place a new feeding tube towards the end of November.
* J-tube - Jejuonstomy feeding tube that goes directly into the small intestine.
** PICC line - Peripherally inserted central catheter - An intravenous access line
that is placed into the upper arm with an internal catheter running
through a large vein near the heart.
*** TPN - Total parenteral nutrition - Complete nutrition run into a person's
bloodstream when digestive system must be bypassed.
While Ashlinn was hospitalized, I ran around trying to find her an apartment. With her income being only social security disability and survivor's benefits and the market at the time, very few landlords would even respond to me. I found one landlord that was at least willing to work with us: Mimi. There was a lot of back and forth between Mimi, me, and then, when she was discharged from the hospital, Ashlinn.

Initially, Mimi declined to rent an apartment to Ashlinn. We eventually were able to negotiate with her so that Ashlinn would have somewhere to live. The tradeoff, though, was using the majority of the money that Ashlinn received from the sale of the condo that she lived in with her mother to pay a full year's rent plus two month's security deposit and a pet deposit. For better or for worse, it was the only option.

After another several nights back in the Extended Stay, Ashlinn finally was able to get they keys to the apartment and start moving in. It was a studio apartment in a rundown building, about 300 square feet, but it was hers. She celebrated a Christmas, New Year, and the introduction of Ash and Willow into our little family, but unfortunately, we found out in the summer of 2021 that there was lead in the water.

Aspen was diagnosed with acute kidney failures with unreadable levels in lab testing. We had the water independently tested by a lab, as well as several other things. It found that the lead levels were just a little bit under the EPA limit. When we brought the results to Mimi, she had to be reassured that we weren't threatening to sue her, we just didn't want anyone else to die, but then she said, "Well, if this is true, we can't have babies in here."
Dr. Ali at Vet for Pet in East Hartford gave Ashlinn and Aspen time together in the condo that she and I now live in together. He kept Aspen inpatient for two weeks at a massively discounted rate because he could see how much genuine love and care Ashlinn had for him. We were already working on getting into a condo together, but we expedited the process so that in the week that Aspen was able to be out of the hospital, he could come to our home in Naugatuck. That was invaluable.

Our primary vet, Dr. Steinberg at Banfield in Manchester, has always been great at being really straightforward with recommendations and not beating around the bush. He told Ashlinn that it would be possible to keep Aspen alive, but he would have to be hospitalized frequently, and it wouldn't really be a high quality of life for him. We took him home for two more nights and drove him to New York because he liked to look at the lights, and then we brought him back to Dr. Steinberg and let him go.

I was scared when Aspen died. I didn't know how Ashlinn was going to take it. In the same way that she has persevered and pushed through when things have gotten hard every time since I've known her, though, she figured out how to cope. Some days were really hard, but she kept moving forward because that's who she is.
August 2021 - December 2023
Just weeks after Aspen's death, I was hospitalized with severe serotonin syndrome. I was hallucinating and several times thought I saw Aspen. I have very few memories from when I had serotonin syndrome, but Ashlinn has told me that I was stooping down, petting air, saying that it was Aspen. Although I can't remember, I know that must have been extremely difficult for her. Still, she persevered.
After my bout with serotonin syndrome, I relapsed into my eating disorder and struggled for the two years that followed. Through all of that, despite another person in her own home using eating disorder behaviors, Ashlinn continued to work to stay in recovery and get better every day.

Ashlinn was hospitalized a few times a year between 2021 and 2022, always either for an infection or a bowel obstruction (or an infection, then a bowel obstruction). She first was referred to a specialist at Hartford Hospital, but that doctor swiftly referred Ashlinn to Dr. Jill Deutsch, an intestinal disease specialist and surgeon at Yale-New Haven Hospital.

The Yale GI practice got Ashlinn in for occasional appointments with other providers in the office, but Dr. Deutsch had a long wait list, which Ashlinn was placed on in late 2021. In the years that followed, Ashlinn had testing done and talked to various gastroenterologists within Yale's outpatient practice and various inpatient gastroenterologists. They all said the same thing: Dr. Deutsch was her only hope.
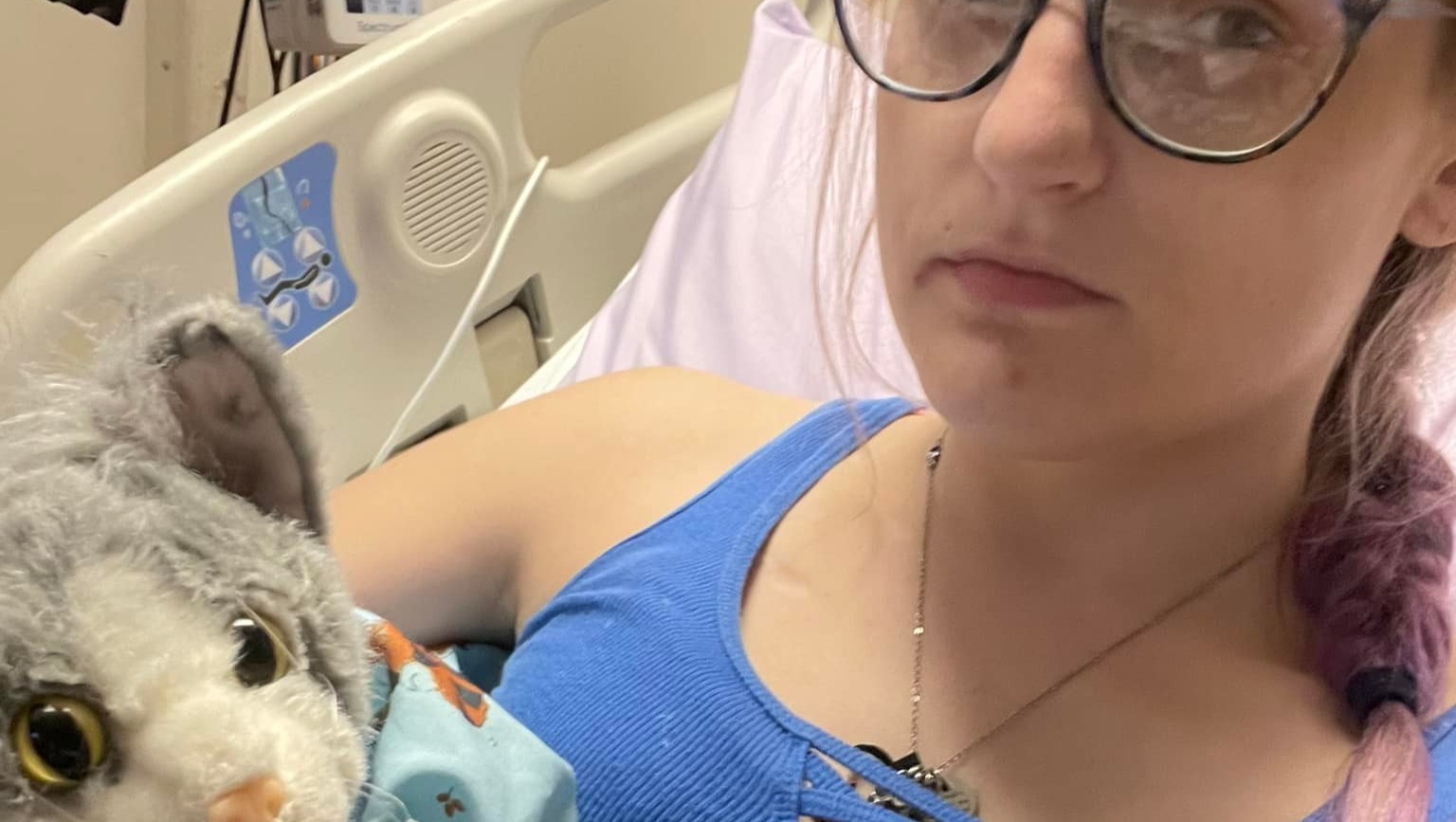
Since getting onto Yale's wait list, Ashlinn lost her feeding tube to an infection, developed colonized CRE (an antibiotic resistant superbug) in her small intestine, and, in December 2023, tested positive for COVID for a second time. Testing positive for COVID started her weight on its downward trend. It seemed to us that COVID was attacking the weakest link, which in both October 2020 and December 2023 was Ashlinn's small intestine. Her ability to digest food was cut to the extent that she is no longer able to digest enough food to keep her body going.
Ashlinn's CRE colony is its own issue that makes any path for her treacherous. The only things that could realistically give Ashlinn some amount of quality of life back would be either an ileostomy or an intestinal transplant. Unfortunately, we know that if an incision is made in Ashlinn's small intestine, the CRE will spread into her blood stream, and that would kill her.

What kept Ashlinn going through all that she's gone through is simple: She loves her kids. When we moved into the condo, we had Aspen, Ash, and Willow. Aspen died a few weeks afterwards. In November 2022, we added Chestnut to the mix, and in July 2023, we added our ferrets, Simba, Nala, and Mufasa.

January 2024 - June 2024
Ashlinn explained to me pretty early on in our friendship that she didn't think she could work at all because she had really struggled working a job at IHOP several years earlier. In February 2023, Ashlinn built up the confidence and decided to try working as an Event Coordinator for Advantage Solutions at the BJ's Wholesale Club in Waterbury, CT. She was everyone's favorite part of wholesale stores: Free samples! She took a lot of pride in her work and it was very difficult for her to go on medical leave to go to the hospital in May 2024. It was even harder when September 2024 rolled around and she had to resign her position because her health was still very unstable.

After losing over thirty pounds following her second COVID infection, Ashlinn, myself, and Ashlinn's primary care provider worked to make a plan for her to be admitted to Yale-New Haven Hospital. She was admitted on 29 May 2024, and we hoped that they could quickly find a solution for her and discharge her home so that she could restore some weight, start feeling a bit better, then go back to work. That isn't what happened.

Ashlinn was hospitalized at Yale for seven weeks. Some days were pure torture, some felt like we were being punked, maybe a few were almost tolerable. Her gastroenterologist told her that he wasn't "sure [they] know how to place an NJ tube." When they figured it out and prepared to drop a tube, Ashlinn was sure to make it very clear that she has a severe deviated septum that means that the tube needs to be placed in the right nostril, not the left. Naturally, they put her under anesthesia to place it, and somehow managed to shove the tube through her left nostril. She was in horrible pain, but they made her try to run feeds through it for a couple of days before it got clogged and they had to pull it.
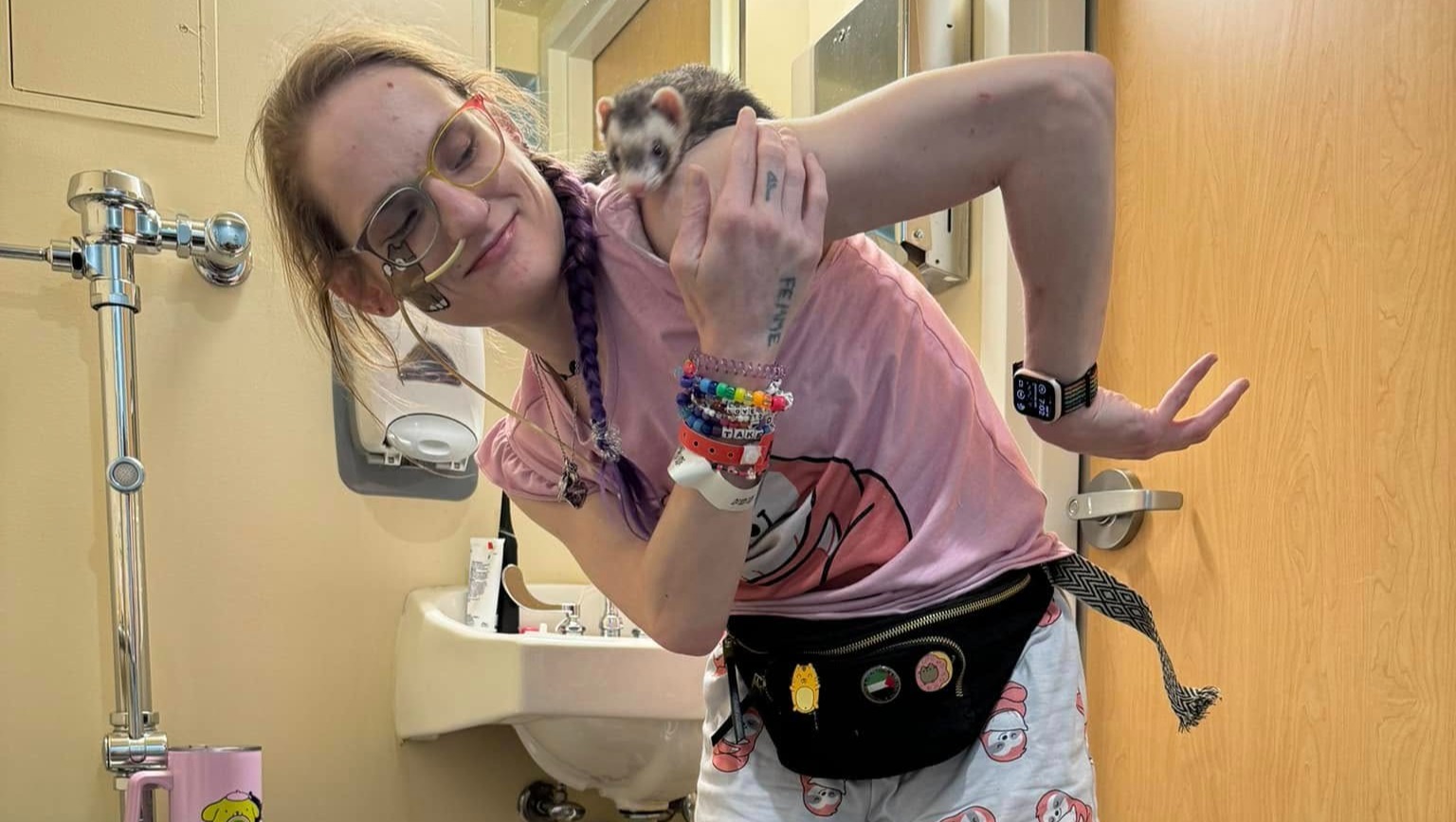
During all of this, one PA stands out to me as communicating the best and being as honest as Ashlinn needed him to be during that hospitalization. He's the one that decided to put in a formal consult with palliative care rather than the team just asking them for pain control recommendations. He admitted to her that they didn't know that they had any curative options for her, and that it was unlikely that any other hospital nationwide would be able to do anything that Yale couldn't do for her. Another provider also noted that she seemed to chronically have high cortisol levels, and he attributed that to her having had chronic pain her entire life without adequate pain control.
Yale tried a lot of different formulas for tube feeding with no luck. Every one seemed to make her sicker and sicker, but of course they wanted to turn over every stone. After five weeks of that, they decided they would place a PICC line and have her receive TPN at least until she could get back to her goal weight.
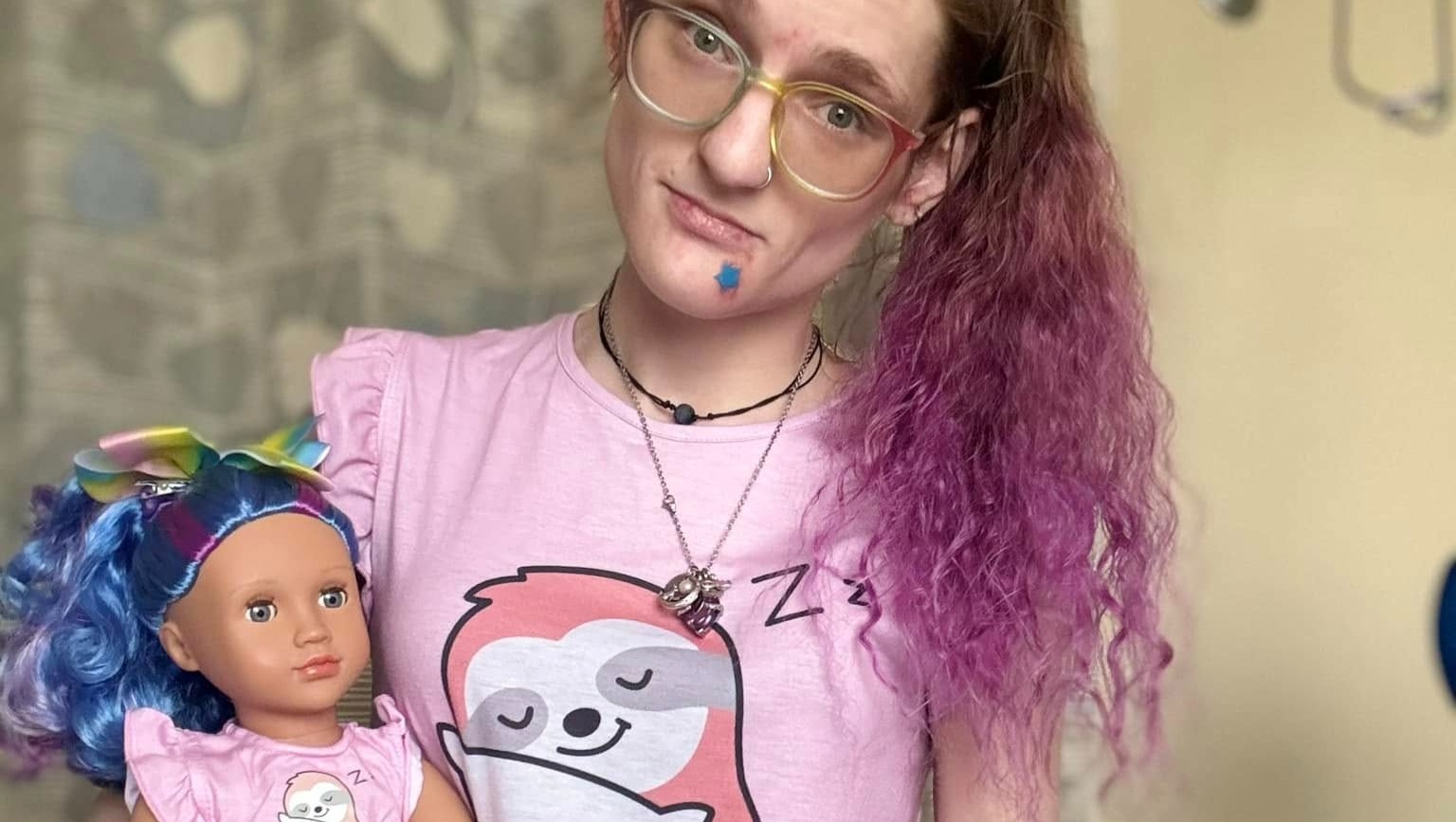
Her stay was prolonged by a week because so many providers were taking off of work for the Fourth of July. During that week, she developed a blood clot, and after a day or so, she began having cardiac symptoms. It took Ashlinn and I together arguing with them to put her on telemetry. They were extremely resistent to it, and only agreed when I asked what risks of telemetry they were worried about that would make it such an issue, and how the risks of her previous cardiac history weren't greater. Once they finally did that, they found that in her sleep, she was having heart blocks and episodes of both ventricular tachycardia and supraventricular tachycardia.
The entire time that we were there, we begged and pleaded for them to find a way to get Dr. Deutsch to come and see her. They told us that they were talking to her, and at one point, another doctor in her practice came to see her, but the doctor Ashlinn had been waiting for years to see did not come.
July 2024 - January 2025
She was finally discharged home on 15 July 2024. She got set up with Connecticut Hospice as an outpatient palliative care patient, and had nurses coming in weekly to change her PICC line dressing.
Just weeks after getting home, Ashlinn developed another blood clot near her PICC line site. Her veins became very pronounced and she occasionally had cardiac symptoms. We went to the emergency room and were basically laughed out. The day after that happened, I sat next to Ashlinn's bed while she rested and counted her respirations: Four breaths per minute. Eventually, we figured out a way to tie her arm to her bed tent to keep it elevated while she slept, and she lived through the night. She began seeing a hematologist and started taking subcutaneous blood thinners, and eventually, the blood clot went away.
Not long afterwards, though, a new threat emerged. First, Ashlinn noticed that her PICC line site was inflamed and discharging some goop. She brought it to the attention of the nurses and every time, they insisted that there was no infection. Ashlinn started running fevers, vomiting in unusual quantity and intensity, and having pain all over her body. She recognized them as being symptoms of sepsis.
We contacted Ashlinn's palliative care team and they advised that she go to the ER. Ashlinn didn't think that she could make the ride in my car followed by me pushing her in her wheelchair, so we called an ambulance. The EMTs were horrible to her, harping on semantics rather than recognizing how sick she was. When they gave report to the ER nurse, Ashlinn heard them laughing at her. They put her into the waiting room.
When I arrived to the St. Mary's Hospital ER a short while later, I told the triage nurse that having her in the waiting room was not just causing her pain and suffering and putting her at risk, it was also putting everyone else in the waiting room at risk. She was projectile vomiting the entire time she was there and has a colonized, antibiotic resistant superbug in her GI system, and that's not to mention whatever was making her sick that day. Magically, they could understand as long as it wasn't coming from the patient.
The providers in the ER were really just as bad. The doctor asked Ashlinn, "If it does turn out that you have an infection, do you even want antibiotics? You're on palliative care." Palliative care allows for continued curative treatment: It's not hospice. They told her that her labs were fine and sent her home. She got her labs on MyChart the next day and saw that her white count was elevated and that her liver values indicated that she had suffered an acute liver injury due to the infection that she had. This ER visit marked the final time that Ashlinn felt safe going to an ER to receive treatment for emergency conditions.
The following day, Ashlinn vomited too frequently to keep track. She kept asking me to kill her because her suffering was so immense. She was sweating so profusely that the IV3000 dressing on her PICC line site came off. She tried to redress it, but she was sweating too much for it to adhere to her skin. When she was trying to apply the last dressing that she had available to her (without much luck), the PICC line started to emerge from the site and it became clear that if she were to try anything more to fix it, she would only expose herself to more deadly pathogens. The only choice that she had was to accept that it was falling out.
When the PICC line was fully out, I saw some white material fall from the site. Her primary care provider has since figured that she had a fungal infection, a common side effect of TPN. After it came out, Ashlinn was able to take children's ibuprofen and sleep for a few hours. When she woke up, her fever had finally broken. She lost access to her only source of complete nutrition, but the only other option at that time was death in the short run.
Around the same time that Ashlinn had the fungal infection, she had an appointment with one of the providers in Yale's GI office. That provider brought the office manager in to discuss Ashlinn's case so that they could push Dr. Deutsch to accept her case. Apparently, Dr. Deutsch only accepts one new patient per month, so although an earlier appointment would likely have meant that today, Ashlinn would not be on hospice, that isn't how they do things.
February 2025 - August 2025
In February 2025, Ashlinn finally had her first appointment with Dr. Deutsch. Once you finally get an appointment with her, Dr. Deutsch is amazing. She scheduled some more testing, ran labs to try to find an autoimmune condition (Long suspected, never found) so that she would qualify for insurance coverage for IVIg, which could potentially bolster her immune system to the extent that she could survive a surgery, and prescribed a nasal spray version of one of her most essential medications.
The labs found that Ashlinn's rheumatoid factor and ganglioside antibodies were elevated. That seemed to indicate some type of autoimmune motor neuropathy, which could be anything from multifocal motor neuropathy to amyotrophic lateral sclerosis. She saw a rheumatologist, who didn't appear to understand what cerebral palsy was and dismissed Ashlinn's case without looking into it particularly seriously. Then, she saw a neurologist who told her that she needed a nerve conduction study and that they would call her to schedule it. They never called.
At the same time, UnitedHealthcare did its thing and stopped covering Connecticut Hospice. She was forced to find a different provider, but there were no providers that her insurance would cover. In speaking with UnitedHealthcare, they gave me a few places. Two of them were the same and owned by UnitedHealthcare, but stated that UnitedHealthcare said that Ashlinn was ineligible. The other option was Vitas Hospice & Palliative Care and I was able to set up an appointment for their intake nurse to come out and talk with Ashlinn. We didn't know at the time, but in fact, they only offer hospice.
Although it seems that many people simply can't imagine a thirty year old on hospice, Ashlinn came to the decision to do hospice with a good understanding of what she really wants from the rest of her life. She knows that any "options" that are offered to her by medical providers are either temporary, but with risk and/or pain, or more likely than unlikely that it would simply kill her painfully.
So, she's making the best of it. There's been a bit of a learning curve going from a lifetime of being in the medical system with curative aims, then moving to hospice, with the goal being comfort and the quality of life over the quantity, but as always, she's persevering and trying to get the most meaning out of the time she has left.
"Nothing from the first day I saw her and no-one that has happened to me since has ever been as frightening and as confusing, for no person I've ever known has ever done more to make me feel more sure, more insecure, more important, and less significant."
Carolinian to Connecticuter
Birth - Age 4
Ashlinn was born to Leo and Lisa Collins four months premature, a micro-preemie, on 14 November 1994. She was airlifted from the small hospital she was born in to Wake Forest University Medical Center to be admitted to their NICU.
Her father was petrified, and as an Irish Catholic, he feared that if she did not live and wasn't christened, she would go to purgatory. The family's pastor from the UCC that Ashlinn was raised in came and spoke with them and told him that he had faith that she would make it, and that he'd christen her in the church.
Sure enough, she lived. As they spent time with her at home, though, they noticed that she wasn't using her right arm to reach for things and that she wasn't meeting all of her developmental milestones. At eighteen months, Ashlinn was diagnosed with right hemiplegic cerebral palsy. Immediately, she began receiving treatment.

Leo tied Ashlinn's feet to his, then walked around their house, to help her muscles get used to the motion of walking. She began receiving Botox injections in her right leg, along with serial casting, to try to ensure that her heel would be able to touch the floor. When she got a little older, she received two Achilles tendon lengthening surgeries. It's only been recently that I've seen her foot sickle as a result of atrophy from her autoimmune motor neuropathy, but she had pretty much only the option to have her foot at a right angle for most of the time that I knew her.

Age 6 - Age 10
In January 2000, Ashlinn was five years old. At the time, her mother, Lisa, worked as a phlebotomist/lab technician at a nearby hospital during the day. Her father, Leo, worked at a factory overnight. On this particular night, North Carolina was hit by an ice storm that the North Carolina Department of Transportation couldn't have had the resources to prepare for.
Leo, having been raised in Philadelphia, was certain that he would be able to drive to work and back home safely. He and Lisa argued about it, but ultimately, he left for work in a huff. Lisa told Ashlinn and her older brother, Tommy, to sleep in her bed, so they did.
Not long into his shift, the factory sent non-essential personnel home. Surely in a hurry to get home, Leo drove a little too fast and didn't see a patch of black ice in the shadow of the nearby trees. He lost control of his car and hit a telephone pole, which then broke and fell onto the driver's side of the car.
As in any fatal crash, the authorities that be investigated to find the cause. They noted that he wasn't wearing his seat belt, that his cell phone was open, that he had evidently taken his jacket off and thrown it onto the passenger seat, and that black ice was the primary cause of the crash. After Leo's death, they cut those trees down. He had a closed casket funeral because he had to be entirely reconstructed and Lisa didn't want her children's last memory of Leo to be the reconstructed, best-they-could-do version of him that was inside the casket. The only real solace is that the first responders said that he was killed instantly, likely didn't even know what happened, and almost certainly didn't feel any pain.
Perhaps more damaging than, theoretically, five-year-old Ashlinn and six-year-old Tommy seeing their father as he was at his funeral, particularly if they were given proper emotional support and grief counseling through and after all of this, was that they were not allowed to grieve:
Tommy was promptly told by his mother that he was the man of the house. He wasn't given space to process his grief, instead becoming his mother's trophy child and confidant. According to extended family members, it was evident that Lisa preferred Tommy to an extreme degree from the day that Ashlinn came home from the NICU. Lisa created a competitive dynamic between her children then gave only one of them the resources necessary to at least appear to win. At the same time, though, the way that she groomed her son has seemed, in the long term, to isolate him and potentially cut him off from self-fulfillment outside of the role that he's been placed into for so many years:
- Thomas has a brilliant mind for computer science and was receiving job offers from Google and Apple before graduating. Taking a job with Google or any similar company would mean that he had to move to the west coast. Lisa didn't want him to be that far away from her, so he dropped out of college with just one semester remaining before he would have graduated. More recently, he went back to school to become a gym teacher, and after Ashlinn left North Carolina, Lisa moved into his condo.
- Thomas has had girlfriends that have ended the relationships with him because his mother sent them pictures of engagements rings far too early.
Meanwhile, Ashlinn was the black sheep of the family. At such a young age, she didn't understand death. She knew and understood that her dad went to work and didn't come home, and that when she looked to the adults in her life for guidance, they weren't behaving in a healthy way. She was told that her father was in heaven and asked when he was coming back.
Questions about what happened to Leo, whether or not he was in pain when he died, and about the realities of death were met with accusations of Ashlinn being "morbid," obsessed with death, and perhaps enjoying the whole spectacle of death. Besides, it upset Tommy.
It's okay to be upset sometimes when dealing with grief: Grief is really hard. In this one instance of their parent's attitude, Ashlinn and Tommy were both deprived of the opportunity to process the grief associated with their father's death before the unresolved stress develops into the attachment issues that they both show evidence of today. I know that for her to process and understand something, she has to ask those questions and talk it out with somebody.

Lisa and Tommy would gang up on Ashlinn and taunt her, and if she got upset, she was in the wrong for "not having a sense of humor." Her mother in particular had a habit of either making fun of her or criticizing her for things that were caused by the disabilities that she was born with. Lisa spent hours every week attending dance classes and events with Tommy, but any request from Ashlinn to delve into poetry or music was met with extreme disinterest.
It's common for children with neurodevelopmental disabilities including cerebral palsy, autism, and ADHD to get overloaded and have reactions that, from the outside, appear excessive. Ashlinn experienced emotional and/or sensory overload frequently when she was young, and at times became so overwhelmed that all she could do was hit herself and scream. Her mother knew enough to know that what Ashlinn was experiencing were overloads, and even got a job in Ashlinn and Tommy's school system as a reading specialist and as an assistant for situations when a child needed to be restrained because she first learned to do it for Ashlinn. Yet rather than managing Ashlinn's symptoms appropriately, figuring out adaptive ways of dealing with the overload, and moving forward in a way that improved her daughter's health, she:
- Yelled to people passing by when Ashlinn was overloaded in public that Ashlinn wanted a pity party, so everyone should look.
- Pulled out a video camera and told Ashlinn that she was going to drop Ashlinn and the recordings off at an orphanage.
For anyone able to access basic empathy and regard for the wellbeing of other people, it would typically be very obvious that saying these things to a neurodevelopmentally disabled child in the midst of emotional and/or sensory overload would make everything worse.

The dynamic that Lisa created for her children created a perfect opening for Lisa's mother to swing in and be the best adult figure that Ashlinn had. Although her grandmother regularly threated to kill herself, then pretended to leave the house, but actually just hid from Ashlinn, sexually abused her, was, per Lisa, a "loan shark," later enabled and encouraged her eating disorder behaviors, and had more recently been diagnosed as having "psychopathic traits," Ashlinn felt safer with her grandmother than her mother. To this day, she largely has fond memories of her grandmother. What keeps her awake at night is her memories of the environment that she grew up in with her mother.
Due to the way that she was treated at home, Ashlinn became progressively more depressed as time went on. When she was just ten years old, she attempted to overdose on ibuprofen. Ever a fan of anything that allowed her to escape from her home life, after she took the ibuprofen, she went to school, as usual. She passed out during class and was soon brought to the emergency room where her stomach was pumped. Luckily, as a ten year old, she didn't have the resources and knowledge to overdose on something that would cause more damage more quickly, and she didn't suffer lasting damage as a result of it.
Age 11 - Age 19
A ten-year-old child attempting to kill themselves should ignite an immediate call to action:
- That child needs to see a therapist;
- The environment that the child lives in needs to change so that the child gets the support that they need.
That isn't what happened. 10-year-old Ashlinn's desperate plea for support from her mother and brother did not yield the response that it should have.
Ashlinn likely suffered from a gastrointestinal condition and avoidant-restrictive food intake disorder from a younger age than when she first was diagnosed with any psychiatric conditions at age ten. Lisa told Ashlinn that she had her grandfather's nervous stomach from a young age. Ashlinn's maternal grandfather had Crohn's Disease and died from an infection contracted while he was having an operation to attempt to remedy a bowel obstruction.
It's likely that from a young age, pain, gastrointestinal symptoms, and discomfort became associated with food in general for Ashlinn. She experienced unusual aversion to certain foods, especially if she had become sick within a short timeframe after eating those foods, and generally felt apathetic towards food.
So, after attempting to overdose at ten years old, changes in Ashlinn's environment were not made. The emotional problems that were developing for her could only grow.
Ashlinn was hospitalized because of anorexia for the first time when she was eleven years old. Over the course of the nine years that followed, she was in and out of treatment. She had gone to every eating disorder treatment facility in the country that insurance would consider paying for. Many of the facilities seemed to see her as either a lost cause or too much of a liability and by the time Ashlinn turned twenty, many would not allow her back.
Age 20 - Age 25
With a dearth of treatment options, Ashlinn got desperate. She put in an application to attend Mercy Ministries in Nashville, Tennessee (now Mercy Multiplied). Mercy is a Christian program that promises to help young women with "life controlling issues." They provided services for free, often bragging that they rely solely on funding from private donors rather than the government. Ashlinn, and the other young women attending the program, had to write essays detailing their own connections with Christ and their faith.

Unfortunately for Ashlinn, Mercy is also a cult. It would take her years and speaking with her family's pastor to learn to reconcile the experience at Mercy with her experience growing up in the UCC. Mercy monitored resident phone calls, cutting them off if the resident began to talk about something that didn't align with what Mercy wanted them to talk about, not the least of which was the program itself.
Programming at Mercy included:
- Bible study
- Prayer groups
- Writing "Thank you" notes to donors
- Daily chores/Cleaning
- "Major cleaning days" weekly, rewarded with pizza
Mercy also rejected western medicine because they believed in the power of prayer and faith healing. When she arrived at Mercy, they refused to allow her access to any of her medication, from her antidepressants to her gastroparesis medication, metoclopramide.
Ashlinn arrived at Mercy shortly before her 21st birthday. She then spent Thanksgiving there, and on Thanksgiving Day, they prepared a decadent meal. On the Friday after, they had the same food again as leftovers. Saturday, as usual, was a major cleaning day.
When Ashlinn woke up on that Saturday, she didn't feel well. Her stomach was hurting badly. She told staff, and they didn't care, simply ensured that she was involved in cleaning. As part of her tasks for the day, they told her to climb a ladder and dust a fake plant. She told them no because with cerebral palsy, climbing a ladder is dangerous. They made her do it anyway.
Her next task was to vacuum the grand staircase that the facility was very proud of. Again, she protested because they were telling her to do something that was dangerous for someone with cerebral palsy. She had access only to a bulky vacuum with a cord too short to cover the whole staircase, so she would have to constantly stop, unplug it, and find somewhere different to plug it in. It all gives a lot of chances for Ashlinn, with cerebral palsy, to trip and fall on the stairs. Again, they told her that she had to do it.
Most of the residents and staff moved on to bible study. Ashlinn was instructed to vacuum, then join them at bible study. She never made it there.
Exactly what Ashlinn feared would happen happened. She tripped over the vacuum cord and fell down the stairs. The fall caused a concussion, a broken nose, a shattered elbow, and ruptured her pancreas and spleen. Through the pure adrenaline of needing to survive allowed her to drag herself to the door to the stairwell and to get it open.
At first, much of what Ashlinn got in response from Mercy staff was that she was being dramatic, that she needed to be quiet, and she needed to stop swearing. She did not do that and instead spent the next several hours screaming and begging for them to take her to the hospital. When they weren't admonishing her for her language and volume, they were praying over her.
It wasn't until one of the staff members meekly said, "God is telling me that she's not being dramatic, she really needs to go to the hospital," that they relented and drove her to the hospital that was affiliated with them. Despite that a level one trauma center was nearby, they chose a small hospital where they had enough pull to control the narrative.
At the ER, Ashlinn was initially dismissed, and they were going to send her back to Mercy. There was an ICU nurse working in the ER that day who, when walking by, noticed that the pain that Ashlinn was describing and pointing towards was her pancreas. She pushed for a CT scan and ensured that Ashlinn would be admitted to deal with it. If not for that nurse, Ashlinn would have been discharged and would have died at Mercy after significant suffering.
They did a series of CT scans over the course of the rest of Saturday and Sunday, watching while her abdominal cavity filled with fluid. When they were no longer able to see any of her organs, they decided that they would do surgery the next day.
Ashlinn's surgeon had never done a surgery like hers before. He was on the phone with Vanderbilt University Medical Center, a level one trauma center, the entire time. He told her that her surgery was the hardest he'd ever done.

She was hospitalized for the following twelve weeks, trying to figure out how she was going to get nutrition and slowly draining all of the lipase that had filled her abdominal cavity. She had to get all of her vaccines again because she lost her spleen, causing even more significant immunodeficiency than she already had.

The years that followed were filled with constant medical struggles, including but certainly not limited to:
- Lyme disease: Possibly from a tick bite from a decade earlier. She was hospitalized and began long-term doxycycline, which caused stomach bleeding. After being unable to complete that treatment, it developed into chronic Lyme disease.
- Supraventricular tachycardia (SVT): Caused by chronic Lyme disease. She had a loop recorder implanted while in North Carolina. When her heart went into SVT, her cardiologist's office would give her a call. When she moved to Connecticut and was in a relatively good place with her health, she didn't have SVT episodes for a while, so Dr. Gnanaraj, a cardiologist we each saw for some period of time, decided not to replace it.
- G/J and J-tubes: After her distal pancreatectomy and splenectomy, Ashlinn needed a feeding tube to get appropriate nutrition, supplementing what she was able to eat orally. Her feeding tubes caused infections and bowel obstructions.
- Ports, PICCs, and peripheral IV problems: When she wasn't tolerating even tube feeding and when her neurologist administered hydration therapy, because her veins roll and IVs blow quickly, she's had multiple different types of semi-permanent lines.
- Sepsis: Ashlinn has survived sepsis more than once--At least five or six bacterial and one fungal.
Her eating disorder remained a presence in her life throughout this time. In the Spring of 2019, though, Ashlinn's friend found a litter of kittens under his house, the mother never having returned. He offered her one and she jumped on it. When she visited the kittens, she thought she knew which one she wanted to adopt, but then the little grey and white cat started climbing up her pant leg. She named him Aspen.

Aspen was only three weeks old, so Ashlinn really had to be his mom. She kept up with everything he needed at the vet, weighed him on a kitchen scale at home, had alarms set to feed him every four hours, brought him everywhere with her, and most of the time, she carried him. Lisa even remarked that he wouldn't know how to walk.

She raised the best cat I've ever met and I've met some cats. He was very comfortable around people and could orient himself well enough to feel comfortable in any environment as long as Ashlinn was there. He had the biggest personality, rambunctious, defiant, and playful while also being affable, sweet, and extremely perceptive. He could clock a bad egg and the pieces would fall into place in human understanding six months later.

When Aspen was around a year old, Ashlinn went to Rockville General Hospital's EDU so that she could be the mom that Aspen deserved.

Organizer and beneficiary
Ashlinn Collins
Beneficiary

