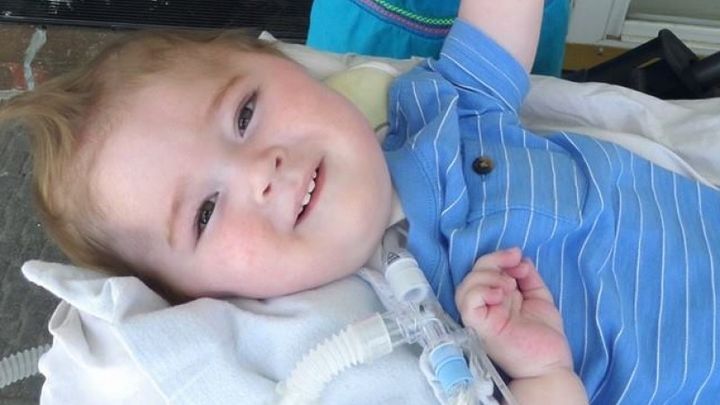
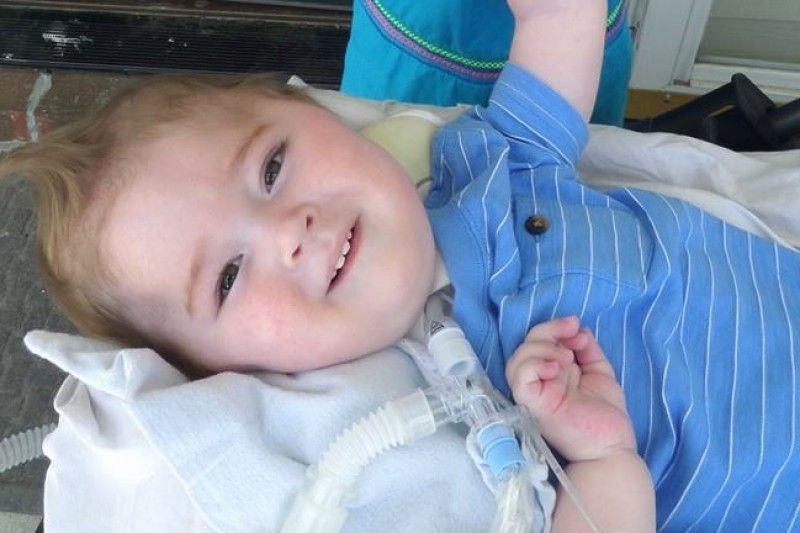
Here is our story:
Like most military families, we married young. We were 20 years old and my husband had just returned from his first deployment in Haiti. I transferred colleges and moved to Fort Bragg with him. We got an apartment and started our life together. Soon we found out we were pregnant with a little girl! My husband deployed to Iraq but was able to come home for R&R just in time for her birth. We welcomed our daughter Hanna into the world September 11, 2011. Two weeks later my husband returned to Iraq to finish his tour but was home to celebrate our first Christmas as a family of three.
Less than two years later we found out we were expecting again, this time a little boy! I had a normal pregnancy but ended up having an unexpected delivery. On October 19, 2013, with no medical intervention or assistance from the hospital staff my husband delivered my son in the font seat of our car in the hospital parking lot. He was perfect and cried right away. Once hospital staff arrived at our car a few minutes later we were helped in to the hospital to be checked out. There were no complications and my son Thomas and I were doing great. We were the talk of the hospital that day and while people were praising us in how everything was handled I didn’t feel like I did anything heroic. As I brought Thomas into the world, everything felt natural. He was finally in my arms where he belonged and since then I have never felt more complete.
We were a happy family four and everything was going great. But when Thomas was around 4-6 weeks old I noticed he was not holding up his head. After looking at pictures of my daughter Hanna around that age it was evident that he was as strong as she was. I was told boys develop later and that all babies develop differently so I was hopeful that he would catch up and he would be just fine. I pushed tummy time but he would either cry and scream with his face down or simply fall asleep.
He ended up having his two-month check up around 10 weeks old. I expressed my concerns about his neck strength being weaker that I expected and noted his head lag. The doctor said that he had weak tone as she placed him prone. He struggled helplessly to lift his face from examining table. It was then when we also discovered the weakness in his legs. He could not bare any supported weight on them. There was no resistance when they were pushed on and they appeared to be very loose. His legs would flop frog like and aside from flexing his feet at his ankles he could not kick or lifted then off the floor. He had no reflexes in his legs. The doctor stressed the need for tummy time and referred us to physical therapy through Early Intervention.
When he was around 12 weeks old we went to our first physical therapy appointment. He was assessed to be 1-2 months behind on his gross motor skills. We were assured that if we continually worked with him using the positions and exercises we learned at physical therapy he would catch up and progressively meet his milestones. I continued to work with him at home but I wanted to know why my baby was like this and what I could do to better understand him so I started to do some research.
Low muscle tone is called hypotonia. Hypotonia is usually a symptom rather than a diagnosis. Hypotonia can alone be the only issue a person can have and many times finding the reason why can remain unknown. As I networked through Facebook with other mom's of hypotonic children, I found a community that knew what I was going through. I told his story and was hopeful when I found that other children like him were meeting milestones. This gave me hope that eventually he would hold his head up.
However, one thing that troubled me with while on the hypotonia
Facebook group when the moms who said he sounded exactly like their children who have SMA. I was no stranger to SMA and was sure he didn't have it. My cousin had a very severe case of SMA type 1 and sadly passed away in 2012 at only 5 months of age. I had the pleasure of meeting and spending some time with her. I learned that SMA was a devastating disease. My son couldn’t possibly have what she had. We also learned that my husband's uncle had SMA and lived to be 3 years old. But that happened more than 40 years ago, before my husband was born so we didn’t have much personal knowledge of the circumstances.
As I continued to work with him doing physical therapy I became discouraged. He showed little signs of improvement. He had however been struggling with congestion for a few weeks. I know being sick makes you tired so I assumed that that was why he wasn't doing so well and once he's better he would start progressing.
When he was around 14 weeks old I noticed he was really breathing with his belly rather than his chest and that his chest presents with the left side sort of dented in. It was also relevant that he was much different than his peers at the playgroup we went to. I was able to compare him and his abilities to four other babies his age. The other mothers asked how I could possibly wake up at night when he cries because his cry was very faint and soft. As the other babies were on their bellies lifting their heads, baring weight on their legs when supported, rolling over and sitting supported, he was not.
On February 19th he went to his four-month check up. I spoke with the doctor about his hypotonia and asked if it could be anything to do with SMA. He asked if I meant MS - Muscular Sclerosis. I said No. SMA - Spinal. Muscular. Atrophy. It was evident he didn’t know what I was talking about as he did not carry on the conversation but continued to examine my child. I spoke about my concerns with his chest, belly breathing and congestion. He ordered a chest X-ray and suggested I come back next week to speak with the pediatrician since he was only a family practitioner.
On the 21st I took him to do the chest x-ray and on the 25th we are back at the doctor's office to see the pediatrician. This was the fifth doctor we had seen, as there was no consistency in the military treatment facilities. He told me the x-ray came back inconclusive because of a shadow. I asked him of he thought his hypotonia could be caused by SMA and once again he did not want to carry on the conversation. While being examined he cried and the doctor noticed his tongue vibrating. He asked me if it always vibrates or if it was just when he was crying. I said I never noticed and didn't think anything of it or why he might bring it up. The doctor said he would put in a referral for him to see a neurologist but it would take at least two weeks to find out who the neurologist is before we could schedule the appointment. I was so frustrated that we had no answers yet as to what was going on but was sure the neurologist could give me some insight.
On February 28th I noticed his tongue vibrating while he was smiling at me. I immediately recalled the doctor bringing that up and knew there had to be a reason why. That day I was checking facebook and in the hypotonia group another mother was telling me about how he sounds exactly like her daughter who has SMA. She asked me if his tongue vibrates and told me that is a major sign of SMA.
I then looked up the signs and symptoms of SMA.
• Absence of reflexes, particularly in the lower extremities
• Overall muscle weakness, poor muscle tone, limpness or a tendency to flop
• Difficulty achieving developmental milestones
• Adopting of a frog-leg position
• Loss of strength of the respiratory muscles: weak cough, weak cry, accumulation of secretions in the lungs or throat, respiratory distress
• Clenched fists with sweaty hands
• Head often tilted to one side, even when lying down
• Fasciclations or twitching of the tongue
• Difficulty sucking or swallowing, poor feeding
I knew then that my son had SMA. Without a doubt he had every single symptom listed for SMA.
I told my husband and my mom. They told me to wait until a doctor said it before I freaked out too much. I think in their gut they knew I was right but didn’t want to believe it at the time. Little did I know how soon I would get that doctor confirmation we all desired but dreaded at the same time.
That night he didn’t nurse much before going to bed. I laid him down around 9:30pm and as expected he woke up around 1:30am, March 1st. He wasn’t interested in nursing and I couldn’t calm his faint distress cries. He worked so hard to breath as I watched his stomach go up and down, gasping for every breath. By 3am I took him to the emergency room. We got right in and were immediately surrounded by five or so nurses. He was given oxygen and breathing treatments. They struggled to find a vein that was large enough to insert an IV line in. After sticking him five times they decided to drill into the bone marrow. Once fluid and medicine were administered he was given an X-ray. Pneumonia.
How could pneumonia manifest from three days after last being seen by the doctors? Why didn’t he tell me this everlasting congestion should be treated immediately? These answers wouldn’t change fate but I needed to blame someone.
The ER doctor said that we would be better off going to Cape Fear, the local hospital, that has better pediatric care so we prepared to go in the ambulance. While being transported I start to think about the seriousness of the situation. Once we arrived at Cape Fear I rushed to keep up with the paramedics as they hurried the stretcher down each hallway until we reached our destination. Once in the room breathing treatments, oxygen, fluids and medicine worked to relieve the distress my baby was in. He was exhausted as the night turned into morning but as everything fell into place he was finally able to rest.
A social worker then came in to check on me. I told her everything that had happened up to this point. I told her about all the other doctors, his everlasting congestion, hypotonia, and my hutch that it all meant he had SMA. She listened, took notes and gave me a hug. From the window in our room I saw her talk to the doctor and the nursing staff. She must have relayed my story because then doctor came into the room.
He said, “So you think this is SMA?”
I nodded.
“Well, it is. Most likely type 1, given his age.”
Tears started to stream down my face as I pressed my fist against my mouth. It wasn’t a surprise because I already knew but the confirmation is what got me. I was holding on to that ounce of hope that I could be wrong, that it could be something else, something less dreadful. As my hope slipped away the doctor told me that he would be flown to Duke University Hospital for treatment.
My husband was on his way to bring me some food as I got this news. I called him and told him to hurry. When he arrived I was balling my eyes out in devastation, horror, sadness and every other emotion in the book. He saw me dropped to his knees pleading me to tell him what was going on. The words hardly escaped my mouth before we were both uncontrollably sobbing as we held each other tight. When our tear ducts were dry I was able to fill him in a little more.
The nurses placed my son into my arms as we awaited the helicopter to arrive. He had lines and wires coming from all angles. He looked into my eyes as if he was saying thank you, thank you for finally finding a way to help him. He was trying to tell me for so long.
The flight team arrived and got him ready to travel. I couldn’t go with him in the helicopter. I’ve never felt so scared to leave my baby. I felt nauseous. He would arrive within 30 minutes flying but it would take us two hours to drive. We knew that if we were going to Duke we would be staying there for at least a few days. We went home and grab a few things before making the longest drive up to the hospital.
Once he arrived at Duke he was placed in the Pediatric Intensive Care Unit (PICU). Thomas continued to receive treatments to open his airways and move secretions out of his lungs. He was on BiPAP when we arrived and later that day he was intubated. Because we didn't know if he had a virus or not Thomas had to be isolated. We had to wear a mask, gown and rubber gloves when we were close to him.
On March 2nd we were approved to stay at the Ronald McDonald house of Durham; a home away from home for families who have critically ill children. The next day Hanna was able to join us at the house.
On March 7th, after 6 days of helplessly watching my son be poked and hooked up to machines, I was able to hold him. It was an amazing feeling. I have since held him every day. Each day feels a little better than the day before but not as good as I knew the next day would feel.
The blood work came back on March10th confirming his diagnosis of SMA- type 1. It was like the knife that stabbed me in the back was twisted. The blood work made it final.
On March 13th he had surgery for g-tube and Nissen fundoplication or stomach wrap. SMA Type 1 children usually lose the ability to chew and swallow food and water safely. This can happen at different times for each child. Continuing to take in food and water by mouth can result in a high risk for aspirating and developing respiratory problems such as aspiration pneumonia. To prevent these complications, tube feeding is used to ensure he will get enough calories to grow and enough fluids to remain hydrated.
On April 7th he was extubated to BiPAP. He was able to be to maintain adequate support for about 6 hours before his blood gas was too high and he began to run out of energy. This resulted in taking a few steps backwards in having to be reintubated.
With few options left, we decided to schedule a tracheostomy surgery to provide stable airway for him. The surgery took place on April 10th.
On May 12th, after 73 days of being in the hospital, we were discharged to go home. Going home was exactly what we wanted but nothing like what we expected. We bring our baby home with two holes in his body and tubes coming from each, one to eat and one to breathe. The tubes are connected to machines that are always running. Accompanying us in our home are nurses that help care for our child while we sleep because of his extensive care requirements.
It has now been 1 year since our precious baby boy was diagnosed with Spinal Muscular Atrophy - type 1. He uses 6-7 machines as daily to keep him alive. We’ve learned to care for him just as nurses and respiratory therapists would. We’ve saved his life multiple times in our home when he crashed. My husband describes the horrid experiences as if he was done range being shot at. His like is in our hands and one wrong move it could be over. That hasn’t happened yet though. The good days certainly out weigh the bad.
Thomas, who we call “Bubby” is now 17 months old and thriving. He truly embodies strength, courage and perseverance. After a frustrating diagnosis process and spending almost 3 months in the hospital, we found support. The staff a Duke became our family and helped us advocate. The organization Cure SMA sent us an extraordinary care package and connected us with other families in the area. The Ronald McDonald House of Durham gave us an appropriate place to stay with Hanna and fed us daily. We found a community of experts online; the parents of SMA that had been through it all showed us they were there to guide us along the way. Family, friends and strangers opened their hearts to us and donations for our expenses poured in. We were eventually able to leave the hospital and go home. Tricare, EFMP and ECHO allowed us to hire nurses to help us care for our son, giving us a break from his constant needs. We traded in our vehicle and used donated funds for a handicap accessible van that could accommodate his amazing new medical stroller that held him and all his equipment. We got him set up with multiple therapies; PT, OT, play, and speech so he could adapt, learn and grow strong. We even learned about and applied a special diet that helps him thrive.
I never knew all this was possible or even existed a year ago. I didn't know I could ever see so much life in the eyes of a child fighting against a terminal timeline. By this point, I don't have to tell you how amazing, handsome, and smart he is or how much we have overcome. Today we choose not to be sad. Today we smile, just as he does everyday, because he is here and a year ago that wasn't a guarantee. We know our time with him may be short so we make the best of every day. Despite our obstacles we are a happy family that enjoys going out and doing normal things we just may do so a little differently. We will still face deployments in the future but husband is always working on creating opportunities that will help his career and our family in the long run. My goal is to keep my kids happy and healthy and educate everyone I can about SMA, the devastating disease we face daily.
Click here to follow our journey
SMA is caused by a mutation in the survival motor neuron gene 1 (SMN1). In a healthy person, this gene produces a protein that is critical to the function of the nerves that control our muscles. Without it, those nerve cells cannot properly function and eventually die, leading to debilitating and often fatal muscle weakness.
SMA affects approximately 1 in 10,000 babies, and about 1 in every 50 Americans is a genetic carriers. SMA can affect any race or gender.
There are four primary types of SMA - I, II, III, and IV - based on age of onset and highest physical milestone achieved. Type I—the most severe and the most common—is usually diagnosed during an infant’s first six months. Babies with SMA type I face many physical challenges, including muscle weakness and trouble breathing, coughing, and swallowing. They may need breathing assistance or a feeding tube. Type I is often fatal early on in life, most don’t reach age 2. 60% of all SMA cases are type I.
Individuals with SMA have difficulty performing the basic functions of life, like breathing and swallowing. However, SMA does not affect a person’s ability to think, learn, and build relationships with others.
Though there is currently no approved treatment for SMA, there’s great reason for hope. We know what causes SMA and what we need to do to develop effective therapies, and we’re on the verge of major breakthroughs that will strengthen our children’s bodies, extend life, and eventually lead to a cure.
More on SMA