- A
- T
8/19/2025
Friends, family, acquaintances, thank you for taking the time to view my GoFundMe. This account is for any and all possible medical-related issues that arise during the treatment of breast cancer. That’s right, I have breast cancer.
In late May 2025, I noticed a lump. A small, marble-sized thing that didn’t cause any issue. In July, the dreaded mammogram and ultrasound revealed it was something more. Three more, to be exact. A biopsy (truly, one of the worst experiences) from each was taken; 8 samples from the first, 3 from the second, and 5 from the third.
On August 19th, 2025, the phone call came. The biggest mass came back with “poorly differentiated invasive carcinoma with associated necrosis,” the second mass was fibroadenoma (not cancerous), but the third “poorly differentiated invasive carcinoma with associated necrosis present in association with portions of the lymph node.”
So, what’s next? An appointment with a surgeon and an oncologist. That process is underway and will lead to these masses being removed and whatever may follow.
All in all, I am sad but I am hopeful. I have good health and young age on my side. If there is anything you can spare, I will greatly appreciate it. And if you can share this on social media, I would be so grateful (I deleted all of mine at the start of this year). More updates to follow.
8/21/2025
Today is my 37th birthday.
8/27/2025
I have an appointment schedule with MedStar Betty Lou Ourisman Breast Center on Friday where I will be meeting with a surgeon and potentially an oncologist. I will have much more information after this appointment (and potentially a surgery date). In the meantime, I wanted to keep everyone up to date as much as possible and have started an Instagram, @AmandaHatesCancer. As you can imagine, having to explain this situation can become overwhelming and as much as I want to share my story, sometimes I don’t have the mental capacity to do it. I appreciate everyone’s patience in this, it is certainly not easy.

8/29/2025
Today I met with my new doctor at the Betty Lou Ourisman Breast Health Center at MedStar Georgetown University Hospital. Dr Son explained in greater detail my current situation. This is what I learned:
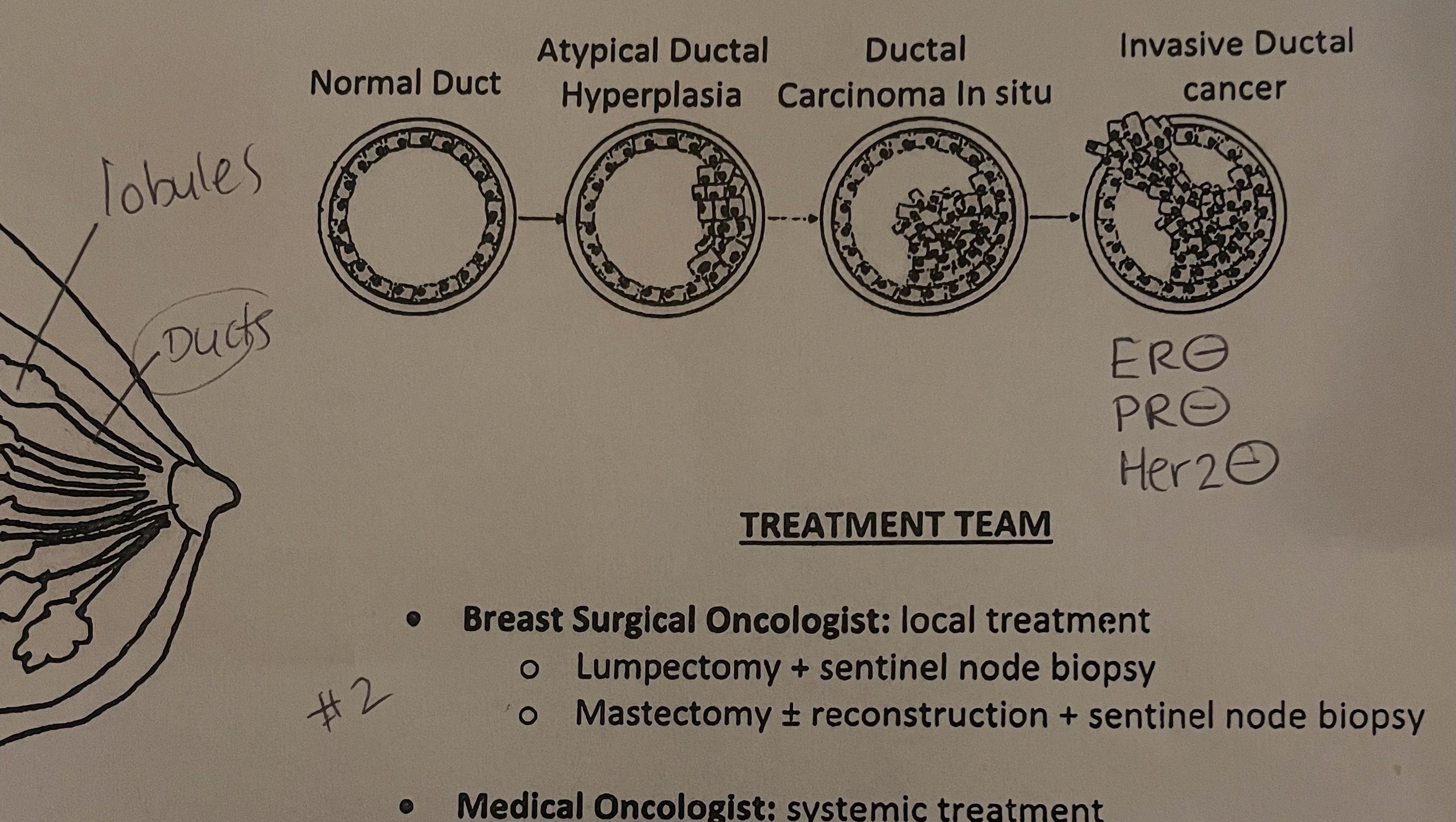
There are several types of growths and the most common occurs in the duct (which is what I have). From there, the classification goes from atypical ductal hyperplasia, to ductal carcinoma in situ, to what I have; Invasive Ductal Cancer (IDC). IDC can spread to other areas, which it has in that it has traveled to my lymph nodes.
My pathology revealed that my cancer is ER negative (estrogen does not contribute to its growth), PR negative (progesterone does not contribute to its growth), as well as Her2 negative (specific protein that does not contribute to its growth).
What does this mean? Basically since none of these factors were related to the growth of this mass, I will not be placed on any oral medical intervention to stop said hormones/proteins. Instead, I will be moving forward with chemo therapy (around 5 months of weekly infusions) to shrink the masses then surgery to remove them (either a lumpectomy or mastectomy, Dr Son is leaning heavily towards mastectomy).
First things first; I have to get some additional tests done. Next week I will be scheduled for an MRI and a PET/CT scan to check my body for the spread of cancer. Then I will be assigned a medical oncologist to begin my chemotherapy. I was able to fulfill generic testing on my end, so I will find out in 10-14 days if this breast cancer is genetic.
This is not the worst news I could have received. I’m pretty have to start chemo and not undergo surgery just yet.
9/3/2025
The next step in my treatment is scans, lots of scans. Tomorrow, bright and early at 6am I have an MRI and next week on 9/12/25 I have my PET/CT scans. All the results from that will go to my oncologist who I am meeting on 9/13. Sounds like a lot and feels like a lot .
9/11/2025
Today is my PET scan at the Nuclear Medicine Department of Georgetown University Hospital. They injected some radioactive fluid in me to help visualize and assess metabolic activity in my organs and tissue.
This procedure is used to detect and determine the stage of cancer I have. The fluid will light up areas with high metabolic activity (thus having to fast). Areas with high metabolic activity most likely are cancerous areas (cancer metabolizes sugar). After letting the radioactive material circulate in my system for an hour, I will go to into the scanner (which I hear is similar to an MRI, how exciting ). The scanner will detect gamma rays emitted by the tracer and generate a 3D image. From there, a radiologist will intercept the images and provide a report to my doctor. I’m meeting with my oncologist tomorrow so I should know more then.
9/12/2025
Just met with my oncologist and my cancer is a stage III which means it is in a mass in my breast and in a lymph node under my arm. This is good news because my PET and MRI did not show any signs of spread outside of those two places. I'll be out on a chemotherapy schedule of Taxol and Carboplatin along with Adriamycin and Cyclosphamide. I'll also receive an immunotherapy called Pembrolizumab. This will be the next 12 weeks for me; weekly infusions. After that, I will be assessed for surgery. This could be a mastectomy or, in a very rare instance, maybe even a lumpectomy. After surgery, because my type of cancer (triple negative with no genetic markers) I will start radiation therapy. This is to ensure that no remaining cellular cancer survives and everything is eradicated ("salt the earth" sort to say).
So yea, for the next 6 months I will be doing cancer stuff. I will be taking a leave of absence from work to avoid contact with possible complications. Getting sick with regular germs (anything from a cold to a GI issue) is very easy when the immune system is compromised.
9/15/2025
i just finished an echocardiogram where the doctors captured images of my heart to use as a baseline before chemotherapy. These images will help evaluate how/why/if chemotherapy is damaging my heart. The whole process took just under an hour and will be repeated throughout the next 12 weeks of chemotherapy to compare to today’s original. That being said, all the pre screening tests are out of the way. Next step is getting a port placed under the skin on my chest for intravenous drugs so that the smaller veins on my arms will be spared. I’m not sure when this will happen, I’m hoping within the next week. Regardless, I will be starting chemotherapy on Thursday so it is a possibility the doctors will use my arm veins for the first infusion.
9/18/2025 My first chemotherapy and my anxiety is through the roof. In a matter of hours, 3 different drugs will be given to me intravenously. These include: Taxol (Paclitaxel), Carboplatin, and Pembrolizumab (Keytruda). These drugs, although are meant to help me, they will initially cause some damage to my body (and probably my mind). I’m feeling a lot of emotions today and bravery isn’t one of them; I am scared and I know this will hurt. I’m not going to put on a facade like everything is ok, everything is not ok and I still can’t believe this is happening to me. The universe works in mysterious ways and I’m only getting through this out of spite and curiosity. At the very least, I hope all this trauma makes me extra funny.







