- C
- B
Sunday:
Kendall woke up not feeling well. He was nauseous, would fluctuate between sweating and freezing, had chills and a low grade fever. As the day progressed, his fever increased, and he began vomiting and had diarrhea. He ate and drank very little (dry Cheerios, a couple of apple slices, water, and Powerade) but anything he tried to consume, came right back out almost immediately. He couldn’t get comfortable. He went between sitting in the recliner to laying in the bed. He attempted to take medicine, but that had the same result as the small amount of food and drink he attempted to consume. He spent majority of the day asleep. Around 7, his stomach started cramping and the other symptoms continued. He stayed in the recliner while I put Ollie to bed and went to sleep myself. Around midnight, Kendall woke me up doubled over in pain and said he thought it was his appendix and needed to go to the hospital. I loaded Ollie and him into the car and we came to Baptist Desoto ER.
Monday:
We arrived at the ER between 12:15 and 12:30 Monday morning. Kendall could not stand up straight, nor could he get comfortable sitting in the emergency room. He would go from sitting up straight, to pulling his knees to his chest, to laying on his side in the fetal position from the pain. At 1:30 AM he was taken into a room, assessed, hooked up to ivs, and given fluids. Like Kendall, the nurse thought the pain in his abdomen was either his appendix or gallbladder. He was taken for a CT scan around 2 AM. While waiting for the results, Kendall could not get comfortable, even after being given morphine. He was tossing and turning in his bed, and continuing to fluctuate between sweating and freezing. I texted our parents and his sister basically saying that we were in the ER and that Kendall more than likely had appendicitis, and that I would keep them posted. After about an hour and a half, the results came back that he’d ruptured his esophagus, which was causing the intense pain Kendall was feeling. The nurse explained this is something EXTREMELY RARE and was more than likely caused by Kendall retching so hard while throwing up throughout the day.
After we learned of the diagnosis, another CT scan was performed to assess the damage. One of two things was going to happen...they’d admit him to the hospital, and monitor him while giving the tear time to heal itself, or they would operate (Kendall’s first surgery in his life). By now, it was 7:00 AM. Ollie had been such a trooper (just like her daddy) sleeping in her carrier in Kendall’s room all night. I had to get her fed, dressed, and to her babysitter to maintain some sense of normalcy for her. We were still waiting on the results/decision, so I left to tend to Ollie and my dad stayed with Kendall.
At 8:00, I was on my way to take Ollie to her babysitter and called dad. I was expecting that Kendall would be admitted and monitored...I couldn’t have been more wrong. My dad said “you need to get back up here...they’re prepping him for surgery now.” My heart sank to my stomach. When I returned to the hospital, I was given a brief synopsis of what would be done and why. The rupture was the size of a quarter and located right above his stomach. Not only that, but anything he’d eaten after the esophagus ruptured had leaked into his chest cavity and was referred to as “infectious matter.”
By 9:30, he was in pre-op. Kendall was awake, but strongly sedated. The anesthesiologist and surgeon came in and explained to my dad and me what exactly would happen in the OR. Kendall was going to have ivs in his hands, wrists, and neck to administer meds and keep constant check of his vitals. The incision would be under the scapula on his left side. They had to go between his ribs and down his esophagus to the tear. In doing so, they would deflate his left lung and intubate him. During his explanation, the doctor mentioned that he hadn’t seen an injury like this in about 10 years and that the esophagus doesn’t typically hold stitches very well...making this an extremely invasive and tedious surgery. However, they would call from the OR when starting the surgery and every hour after that for the duration.
Holding back my tears, I signed consent forms, kissed Kendall’s forehead, told him I loved him, and walked up to the waiting room. My dad and I waited for what seemed like forever to get the call that surgery had begun. The surgery took a little over 2 hours. The nurse said Kendall was doing great, his vitals were good, and that dr. Wolf was pleased with the result. Post-op, he was sent to recovery and then to cardiovascular ICU.
I finally saw him about 4:00 that afternoon. He was pale, still intubated, had chest tubes draining fluids, and was hooked up to more machines than I’d ever seen in one hospital room. The only thing I could do was hold his hand, tell him I was there and that I loved him. He never opened his eyes, but he squeezed my hand and i knew he knew I was there. He remained intubated and was closely monitored that first night in ICU.
Tuesday
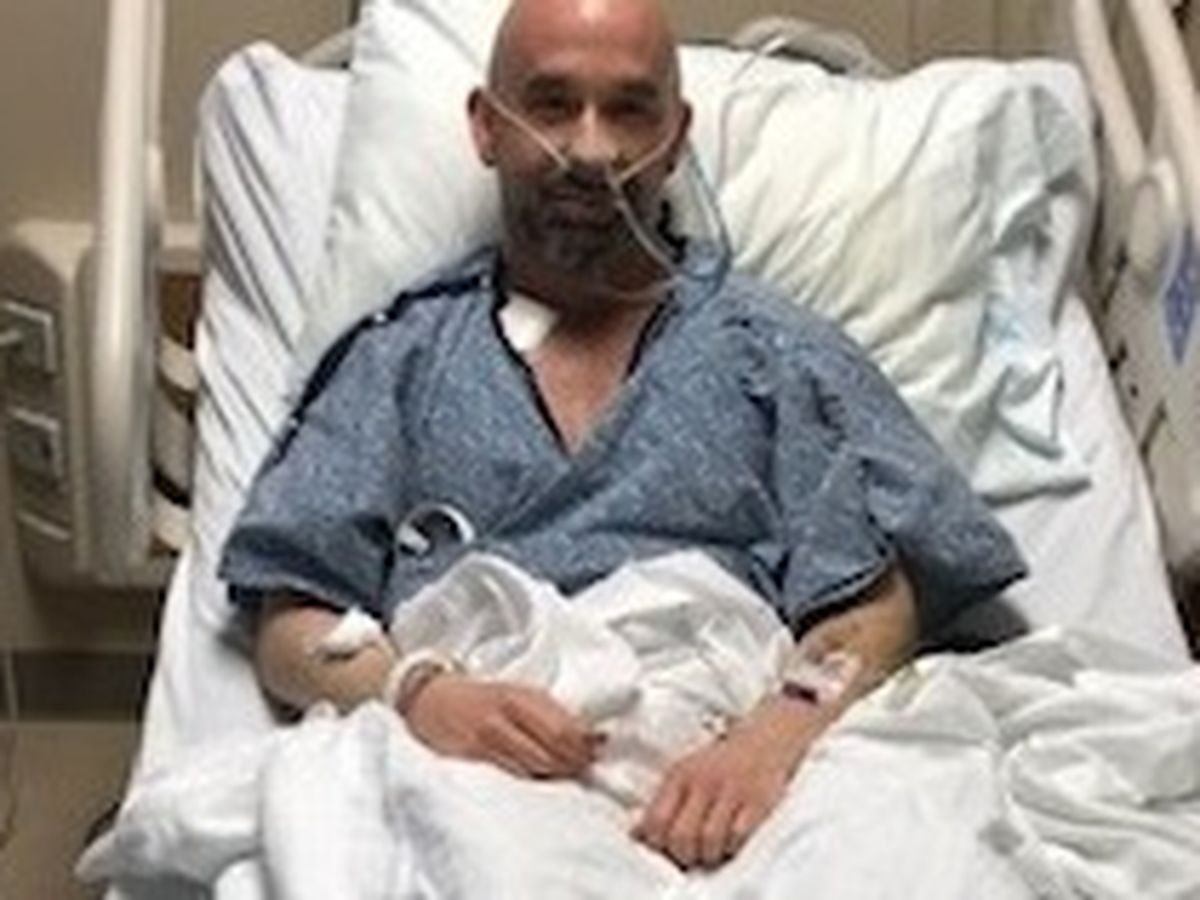
When I got to the hospital Tuesday morning, he was awake but still intubated. I could tell he wanted to talk so badly, he couldn’t stand it. I said good morning and he squeezed my hand. He immediately made an “o” with his hand. I wasn’t sure what he meant and I could tell he was getting frustrated. I figured out that he was asking about Ollie. My sweet husband was intubated in ICU from major surgery and asking about his baby girl. We anxiously waited for a respiratory specialist to give the ok for his breathing tube to be removed. At around 9, the tube was taken out. Kendall could talk, but not loudly or for an extended length of time. The color was slowly coming back to his face. He was still on oxygen, draining from his chest tubes, and hooked up to several machines. After getting the tube out, the remainder of the day was pretty quiet. He was monitored constantly and given pain medication about every hour. He slept off and on all day and night.
Wednesday
Like Tuesday, Wednesday was pretty quiet. He remained in icu, was given medication about every hour, monitored constantly, and the doctor said he was “looking good.” About 6 o’clock that night, he sat in a chair for the first time. He’d sat up and back in his bed, but his feet hadn’t touched the floor in a few days. It was an incredibly slow and tedious process! He sat upright for maybe 30 minutes and the was ready for more pain meds and to return to his bed. After he was comfortable, I went home to be with Ollie. I received a text from him that night that he was being moved to a step down room. He busted out of icu around 10:30 Wednesday night!
Thursday/Friday
On the step down floor, you still aren’t in a “regular” room, but you’re not watched as closely as in icu. He still has ivs, an ng tube in his nose, and chest tubes draining fluid. He isn’t allowed to have any type of nutrition (food or drink) because of the sensitivity of his surgery and the doctors want to insure the tear is completely closed so no more “infectious matter” could leak into his chest cavity. He spends most of his time in his hospital bed, but considering everything he’s been through, is in good spirits. He gets up from his bed once a day. We were hopeful that his chest tubes would be removed and a test called an esophagram would be done on Friday, but no such luck. Dr. Wolf (his surgeon) said that everything is staying put until Monday. He’s being given a strong antibiotic to fend off any possible infections in his chest and fluid that’s providing electrolytes, amino acids, and calories since he’s only cleared to have a couple ice chips every so often.
He’s improving, but still has a long way to go. The first steps are to have the chest tubes removed and have the esophagram performed to make sure there are no leaks. When those two things happen, the doctors will start thinking about the best way to feed him. We haven’t even thought about discharge or what will happen once he gets home. At this point, we’re taking it one day at a time. Both Kendall and myself are extremely appreciative of all the calls, texts, and messages we’ve received! From the bottom of our hearts, thank you!
Kendall woke up not feeling well. He was nauseous, would fluctuate between sweating and freezing, had chills and a low grade fever. As the day progressed, his fever increased, and he began vomiting and had diarrhea. He ate and drank very little (dry Cheerios, a couple of apple slices, water, and Powerade) but anything he tried to consume, came right back out almost immediately. He couldn’t get comfortable. He went between sitting in the recliner to laying in the bed. He attempted to take medicine, but that had the same result as the small amount of food and drink he attempted to consume. He spent majority of the day asleep. Around 7, his stomach started cramping and the other symptoms continued. He stayed in the recliner while I put Ollie to bed and went to sleep myself. Around midnight, Kendall woke me up doubled over in pain and said he thought it was his appendix and needed to go to the hospital. I loaded Ollie and him into the car and we came to Baptist Desoto ER.
Monday:
We arrived at the ER between 12:15 and 12:30 Monday morning. Kendall could not stand up straight, nor could he get comfortable sitting in the emergency room. He would go from sitting up straight, to pulling his knees to his chest, to laying on his side in the fetal position from the pain. At 1:30 AM he was taken into a room, assessed, hooked up to ivs, and given fluids. Like Kendall, the nurse thought the pain in his abdomen was either his appendix or gallbladder. He was taken for a CT scan around 2 AM. While waiting for the results, Kendall could not get comfortable, even after being given morphine. He was tossing and turning in his bed, and continuing to fluctuate between sweating and freezing. I texted our parents and his sister basically saying that we were in the ER and that Kendall more than likely had appendicitis, and that I would keep them posted. After about an hour and a half, the results came back that he’d ruptured his esophagus, which was causing the intense pain Kendall was feeling. The nurse explained this is something EXTREMELY RARE and was more than likely caused by Kendall retching so hard while throwing up throughout the day.
After we learned of the diagnosis, another CT scan was performed to assess the damage. One of two things was going to happen...they’d admit him to the hospital, and monitor him while giving the tear time to heal itself, or they would operate (Kendall’s first surgery in his life). By now, it was 7:00 AM. Ollie had been such a trooper (just like her daddy) sleeping in her carrier in Kendall’s room all night. I had to get her fed, dressed, and to her babysitter to maintain some sense of normalcy for her. We were still waiting on the results/decision, so I left to tend to Ollie and my dad stayed with Kendall.
At 8:00, I was on my way to take Ollie to her babysitter and called dad. I was expecting that Kendall would be admitted and monitored...I couldn’t have been more wrong. My dad said “you need to get back up here...they’re prepping him for surgery now.” My heart sank to my stomach. When I returned to the hospital, I was given a brief synopsis of what would be done and why. The rupture was the size of a quarter and located right above his stomach. Not only that, but anything he’d eaten after the esophagus ruptured had leaked into his chest cavity and was referred to as “infectious matter.”
By 9:30, he was in pre-op. Kendall was awake, but strongly sedated. The anesthesiologist and surgeon came in and explained to my dad and me what exactly would happen in the OR. Kendall was going to have ivs in his hands, wrists, and neck to administer meds and keep constant check of his vitals. The incision would be under the scapula on his left side. They had to go between his ribs and down his esophagus to the tear. In doing so, they would deflate his left lung and intubate him. During his explanation, the doctor mentioned that he hadn’t seen an injury like this in about 10 years and that the esophagus doesn’t typically hold stitches very well...making this an extremely invasive and tedious surgery. However, they would call from the OR when starting the surgery and every hour after that for the duration.
Holding back my tears, I signed consent forms, kissed Kendall’s forehead, told him I loved him, and walked up to the waiting room. My dad and I waited for what seemed like forever to get the call that surgery had begun. The surgery took a little over 2 hours. The nurse said Kendall was doing great, his vitals were good, and that dr. Wolf was pleased with the result. Post-op, he was sent to recovery and then to cardiovascular ICU.
I finally saw him about 4:00 that afternoon. He was pale, still intubated, had chest tubes draining fluids, and was hooked up to more machines than I’d ever seen in one hospital room. The only thing I could do was hold his hand, tell him I was there and that I loved him. He never opened his eyes, but he squeezed my hand and i knew he knew I was there. He remained intubated and was closely monitored that first night in ICU.
Tuesday
When I got to the hospital Tuesday morning, he was awake but still intubated. I could tell he wanted to talk so badly, he couldn’t stand it. I said good morning and he squeezed my hand. He immediately made an “o” with his hand. I wasn’t sure what he meant and I could tell he was getting frustrated. I figured out that he was asking about Ollie. My sweet husband was intubated in ICU from major surgery and asking about his baby girl. We anxiously waited for a respiratory specialist to give the ok for his breathing tube to be removed. At around 9, the tube was taken out. Kendall could talk, but not loudly or for an extended length of time. The color was slowly coming back to his face. He was still on oxygen, draining from his chest tubes, and hooked up to several machines. After getting the tube out, the remainder of the day was pretty quiet. He was monitored constantly and given pain medication about every hour. He slept off and on all day and night.
Wednesday
Like Tuesday, Wednesday was pretty quiet. He remained in icu, was given medication about every hour, monitored constantly, and the doctor said he was “looking good.” About 6 o’clock that night, he sat in a chair for the first time. He’d sat up and back in his bed, but his feet hadn’t touched the floor in a few days. It was an incredibly slow and tedious process! He sat upright for maybe 30 minutes and the was ready for more pain meds and to return to his bed. After he was comfortable, I went home to be with Ollie. I received a text from him that night that he was being moved to a step down room. He busted out of icu around 10:30 Wednesday night!
Thursday/Friday
On the step down floor, you still aren’t in a “regular” room, but you’re not watched as closely as in icu. He still has ivs, an ng tube in his nose, and chest tubes draining fluid. He isn’t allowed to have any type of nutrition (food or drink) because of the sensitivity of his surgery and the doctors want to insure the tear is completely closed so no more “infectious matter” could leak into his chest cavity. He spends most of his time in his hospital bed, but considering everything he’s been through, is in good spirits. He gets up from his bed once a day. We were hopeful that his chest tubes would be removed and a test called an esophagram would be done on Friday, but no such luck. Dr. Wolf (his surgeon) said that everything is staying put until Monday. He’s being given a strong antibiotic to fend off any possible infections in his chest and fluid that’s providing electrolytes, amino acids, and calories since he’s only cleared to have a couple ice chips every so often.
He’s improving, but still has a long way to go. The first steps are to have the chest tubes removed and have the esophagram performed to make sure there are no leaks. When those two things happen, the doctors will start thinking about the best way to feed him. We haven’t even thought about discharge or what will happen once he gets home. At this point, we’re taking it one day at a time. Both Kendall and myself are extremely appreciative of all the calls, texts, and messages we’ve received! From the bottom of our hearts, thank you!
Organizer and beneficiary
Kendall Capps
Beneficiary