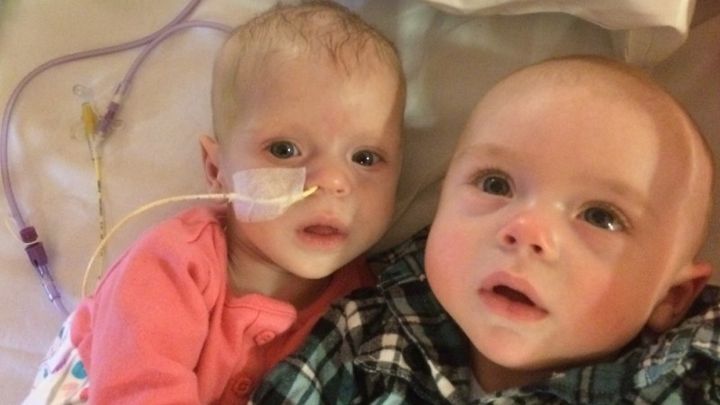
Help get Orin and Olivia home
Hello and thank you for taking the time to visit our page.
We are Stephen and Lyndsay Arthur, parents of Orin and Olivia. Twins with a life limiting illness called pompe disease (https://www.pompe.com/en/patients/about/progression.aspx).
Please take some time to read our story, that is all we ask.
We have setup this page with the hope of raising enough funds to help us get a house to bring our twins home, to a safe and secure environment and all be together at last after over a year in hospital. We also need to purchase an adapted car for when Olivia is discharged. Finally we need help with day to day finances whilst still at hospital and for home as we are unable to return work at present and for the foreseeable future.
Our Story (so far)

Orin and Olivia were born into this world on the 4th August 2014. This was the happiest day of our lives. Finally we had our two beautiful babies, both identical weight (6.95 lbs) and height. After 6 years of trying and being told we were unlikely to ever have children, it appeared all our prayers had been answered at once, not only do we have children we now have the perfect family all at once.

The magic was soon to fade, from the beginning Olivia started to lose weight very quickly, less than 12 hours after getting home for the first time we were back in hospital. After weeks of investigations the conclusion was that Olivia had a milk allergy, how we wish that had have been the problem. Our first month in hospital passed by and still no answers on what was actually wrong with Olivia. Orin was also had a visit in with the cold during this time.
Finally after weeks waiting and worrying, we had a stroke of luck. A visiting consultant took a particular interest in the dip in Olivia's chest. He decided to do a quick 5 minute scan. After 20 minutes and 8 other doctors entering the room it was beyond obvious that something was really wrong.

Olivia was initially diagnosed with left ventricular non-compaction, a heart condition which meant her heart had not formed properly, this condition was untreatable and incurable, this is the exact moment our world began to crumble. We now stood in a position where at 1 month old we were told Olivia was unlikely to survive the next few weeks.
Scans were ordered for the 3 of us the next day, my wife and I were clear, Orin however had the exact same heart condition as his sister. Here we stood within a 24hr period we were told we would lose both twins very quickly. At this point we were sent to Yorkhill to begin a cardiac drug which may delay their deterioration and help them survive long enough to get a heart transplant, this would mean taking both our twins to Newcastle and hoping there would be two hearts available for them before their own gave up. With the knowledge that only one suitable heart comes up in their size every year and they would be 3rd and 4th on the list, we were told to make our peace and say our goodbyes as at this point they were unlikely to make it through the week.
You don’t take that kind of news sitting down, we demanded every test, and we wanted to explore every avenue. This couldn’t be the end, we had just begun!
After a gruelling month of being told every day to say our goodbyes and be prepared for the worse we finally met with a metabolic consultant, who thought she had a different answer for us.
We waited day after day, hour after hour, for the results of all the tests she had ordered on the day we met. After a couple of weeks that felt like years Alison reappears, she had news for us, not good news just news…
When we heard the diagnosis and an explanation of the disease, it was apparent why it was only “news”. The twins had been diagnosed with infantile onset pompe disease. This is an incredibly rare life limiting and progressive disease. Alison explained to us that pompe was a metabolic disease which affected the body’s ability to process glycerine, this meant that the cells which made up the twins hearts, respiratory system, brain and muscle system would begin to overload and shut down. The immediate danger to the twins was heart failure. As the pompe was a progressive disease they were now also not eligible for transplants.
Although pompe has no cure, there was a treatment. An enzyme replacement therapy the twins could receive every week for the rest of their lives, however this had shown limited success and we were informed most babies with pompe die before they are one. Now we knew why she said “news”, so they won’t die today but maybe tomorrow, or the day after.
The next few weeks felt like we had been buried alive and were waiting to suffocate, we had meeting after meeting after meeting and in the end were left with the single most difficult decision I have ever encountered. The time had come, we had to make a decision.
Do we start the twins on the enzyme now or not? General consensus was that it wouldn’t work and the only way to know if it would work was to wait for a test result to identify the strain of pompe the twins had, the problem with this was the result would take three to four months to come back and if we didn’t start the enzyme now it was pointless.
To our minds there never was a question! Do we start a treatment that might prolong their lives or just pull the plug? We were living every parent’s worst nightmare! Whilst the twins were very ill, they were also smiling, gurgling babies. We agreed as long as the treatment wouldn’t hurt the twins we had to give them every chance we could.
We began the course of treatment as soon as possible. However it came with quite a few conditions, as the drug is currently not licensed in Scotland it would be subject to continuous review to justify it was worthwhile, or put more bluntly if it’s not making much of a difference let’s not waste the money. As if life wasn’t scary enough the funding of our children’s treatment was in the hands of the local councils, try to imagine our terror in knowing the only treatment to save and prolong their lives was the subject of a who should be paying row between councils.

Once the enzyme replacement therapy had begun it was a waiting game, the initial job of the enzyme is to repair the heart. This would take up to six months to see significant results and during this time we would have the constant reminder that the treatment could be pulled if their respiratory state degraded below an acceptable level.
The twins responded quite differently to the enzyme, Orin showed immediate signs of cardiac (heart) repair and his breathing improved significantly. This lead to him being discharged to us within a few months of arriving at Yorkhill, it was fantastic, they were measuring the repair of the heart using an ultrasound method called and Echo. Each Echo Orin got showed small amounts of repair, not enough to celebrate at this time, though every tiny step in the right direction is always welcomed.
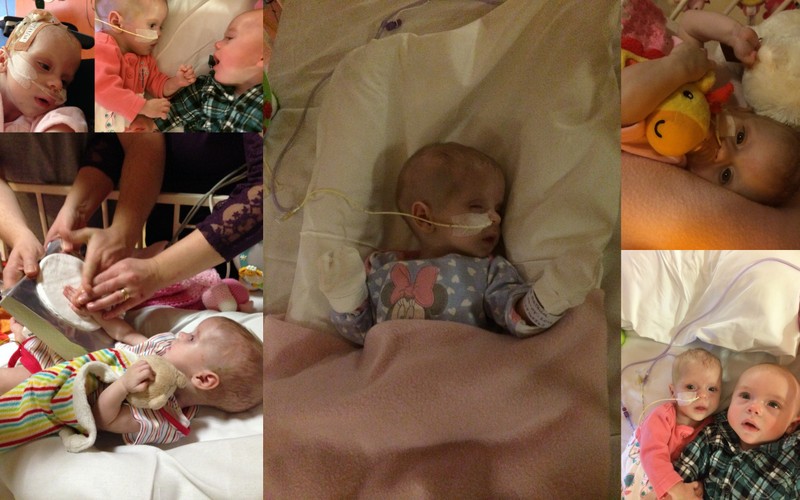
Olivia was showing signs of cardiac repair, it was much slower than her brother. This was fantastic news as we had been told if the heart did not show any signs of repair there was no hope. Poor Olivia had dropped to 4lb 8 and had now reached a point where she required additional breathing support. It didn’t matter, her heart was repairing we could fight everything else, there was hope.

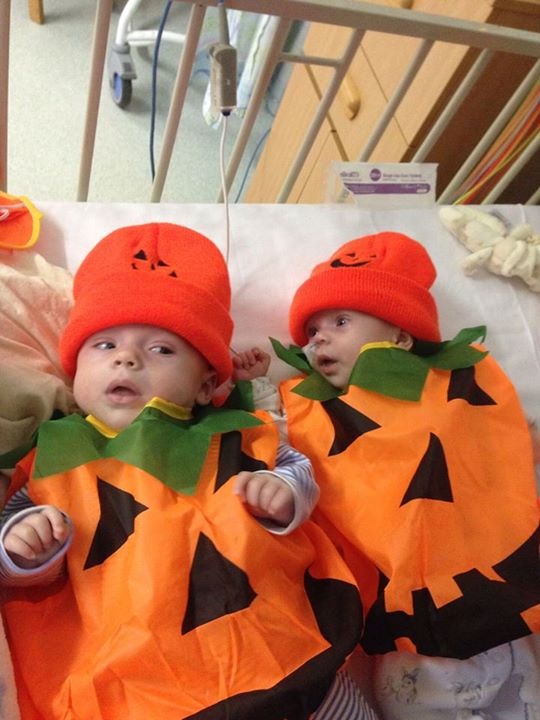
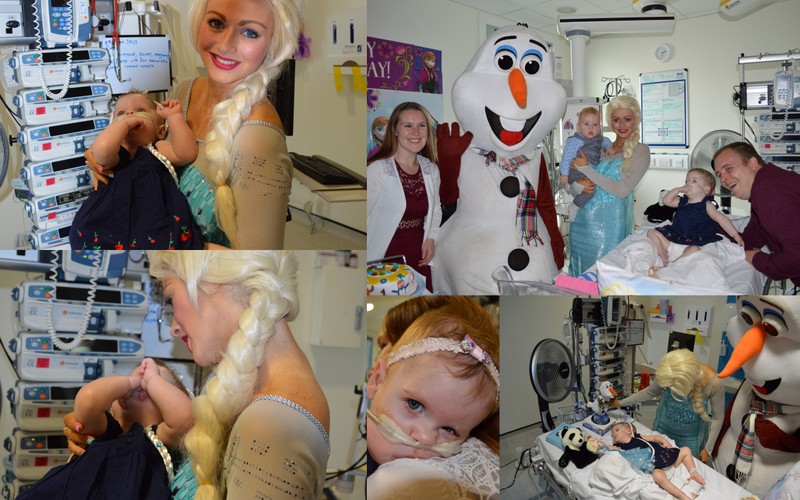
Enter the Christmas onslaught. Christmas in a children’s hospital is something you wish everyone could experience and at the same time wish no one ever had to experience. Christmas in Yorkhill is madness, there are celebrities everywhere and the hospital staff make such an amazing effort for the children, hats off to them they spread a little happiness at a time where a lot of the children and parents are really struggling to be here.
By Christmas we now have Orin out staying with us at Ronald Mc Donald house and we have been invited to join in with the Christmas prayer onstage with Jim (the hospital Chaplin, who required no introduction lol) and dance group Diversity. There is an immediate image that pops to mind of how miserable Christmas in hospital must be, could not be further from the truth, as a family we had a Christmas that will take some work to top. We were together and had just passed a major milestone by all still being here, what more could you possibly want? To us the world had very quickly become a different place, when you stand on the edge of the abyss and stare into the darkness that could await you, you suddenly see what is really important to you and to us our two babies being alive and ticking along was everything.

Nothing makes you think about the future like the dawn of a new year….
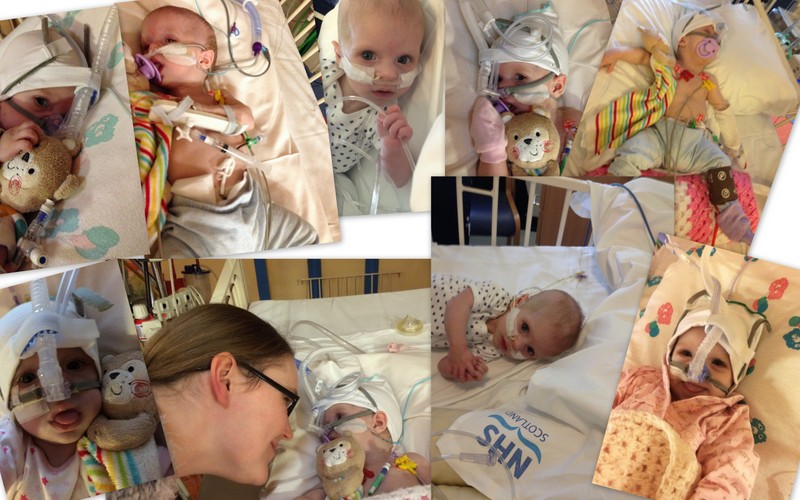
2015 arrived with a bang, this was to be the beginning of a very long year. January was the beginning of Olivia's long term stays in the ICU (Intensive Care Unit). Olivia was rushed to ICU as she was losing far too much weight. With a muscle wasting disease, the worst thing that could happen was for her to be dropping in size. Her breathing had now become a terrifying sight to watch. Our baby girl was fighting for every breath and there was nothing we could do, at this point the dreaded ventilator made its first appearance. This was to become the dark object in the corner of the room that inspired dread, fear and even terror.

Pompe disease is a cruel, sadistic master. Here we stand with two choices
1. Cling on to the cliff by our nails and pray we can hold on long enough
2. Let go and pray we land on something soft
By the middle of January Olivia’s condition had deteriorated to the point we had two options available
1. Do nothing and hope things improved
2. The ventilator.
The problem we faced with the ventilator was that it involved an anaesthetic and children with pompe under the age of one are not likely to survive the anaesthetic, the very thing Olivia required to save her life was almost certain to kill her!
We chose option 3! Off come the gloves pompe, we will fight you to the bitter end!
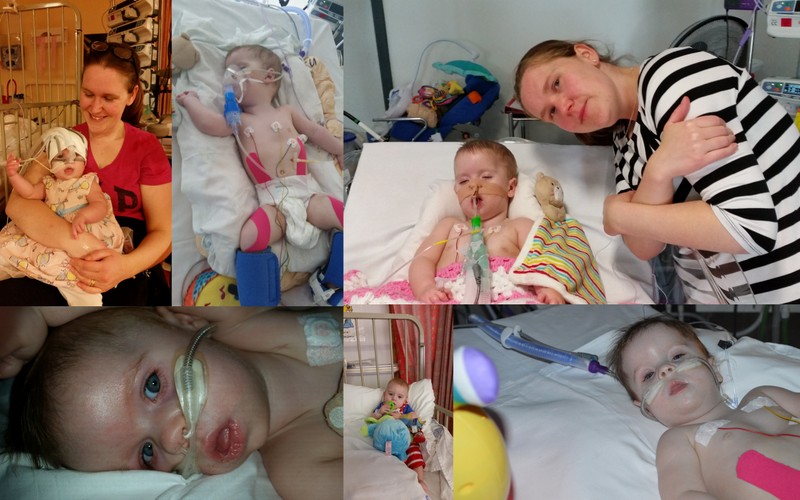
Over the next few months we circled the ring with the reaper on a daily basis, yet round after round Olivia showed a strength and spirit that left everyone in awe. We became medical experts, every day was a regiment of research, discussions with consultants and implement.
Olivia was switched to a high calorie milk and began to put weight back on. However she still required a great deal of breathing support as due to the weight loss she was breathing like she had just run a marathon all day every day. This fast breathing was burning through calories as quick as we could get them into her as a by-product to the rapid breathing was it made her vomit most of her feeds back up.
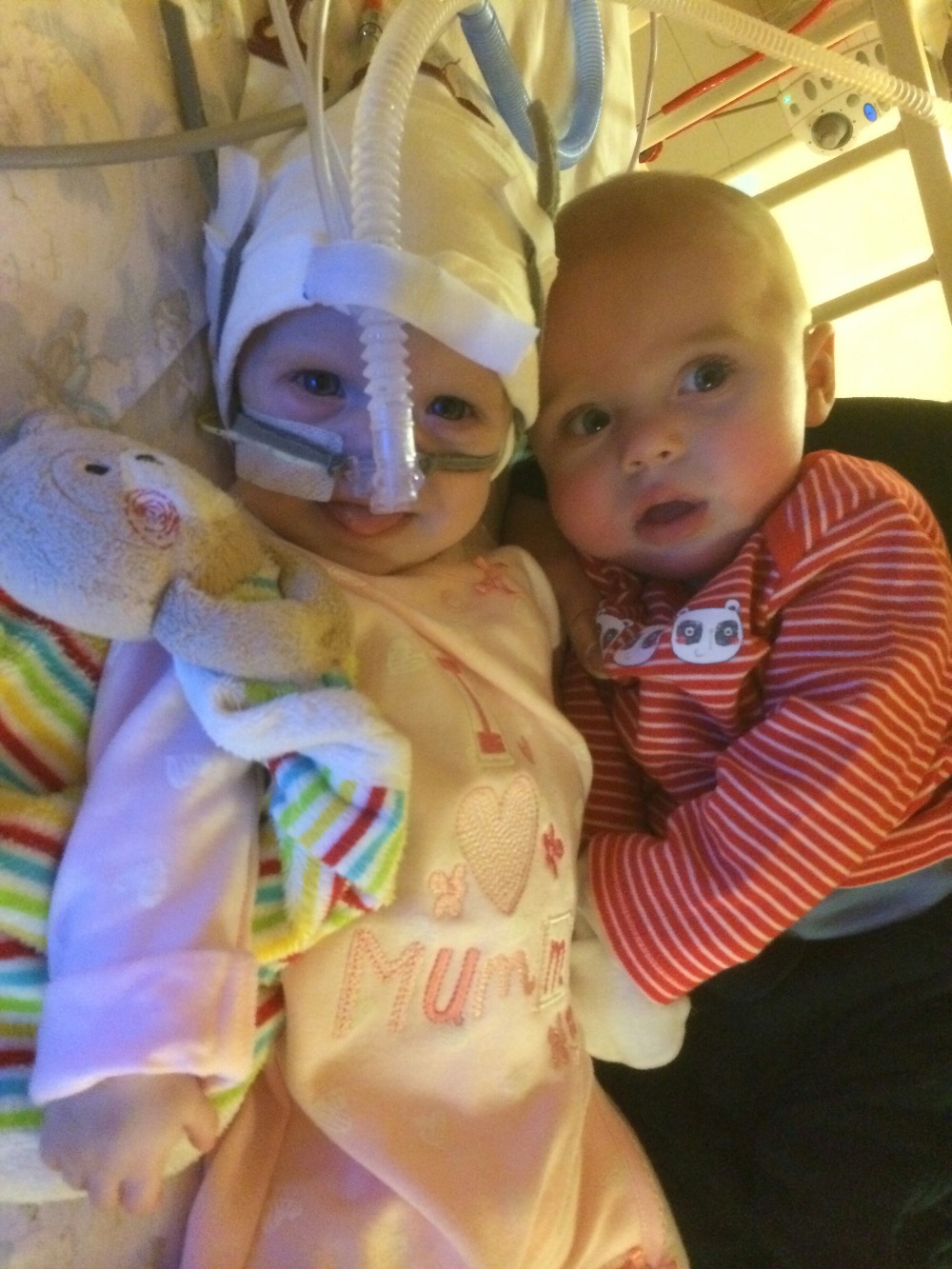
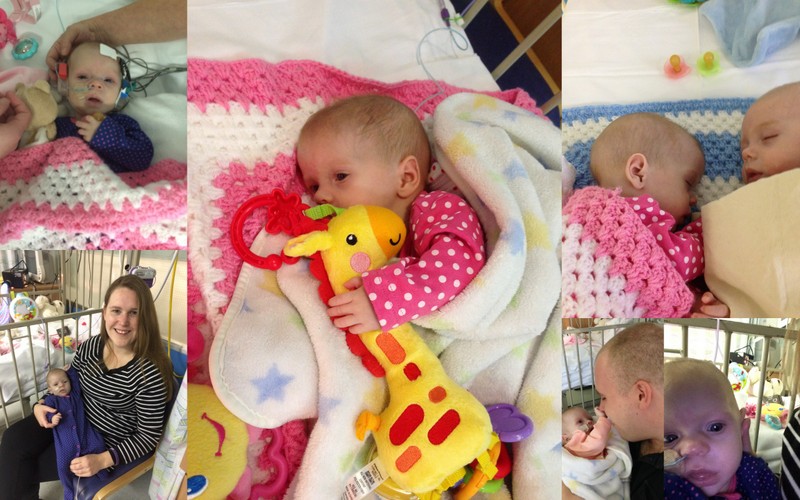
Over the next few months Olivia was up and down more than a yoyo. I have never really been inspired by anyone before and now I find myself stood here at 31 years of age and the first person to ever hold me in a state of awe is my 6 month old daughter. Olivia can lay there hooked up to a dozen machines, being injected, having bloods taken, dealing with teething, nappy rash, gasping for every breath and still look up at you and smile, a smile that doesn’t ask for pity just a great big cuddle….
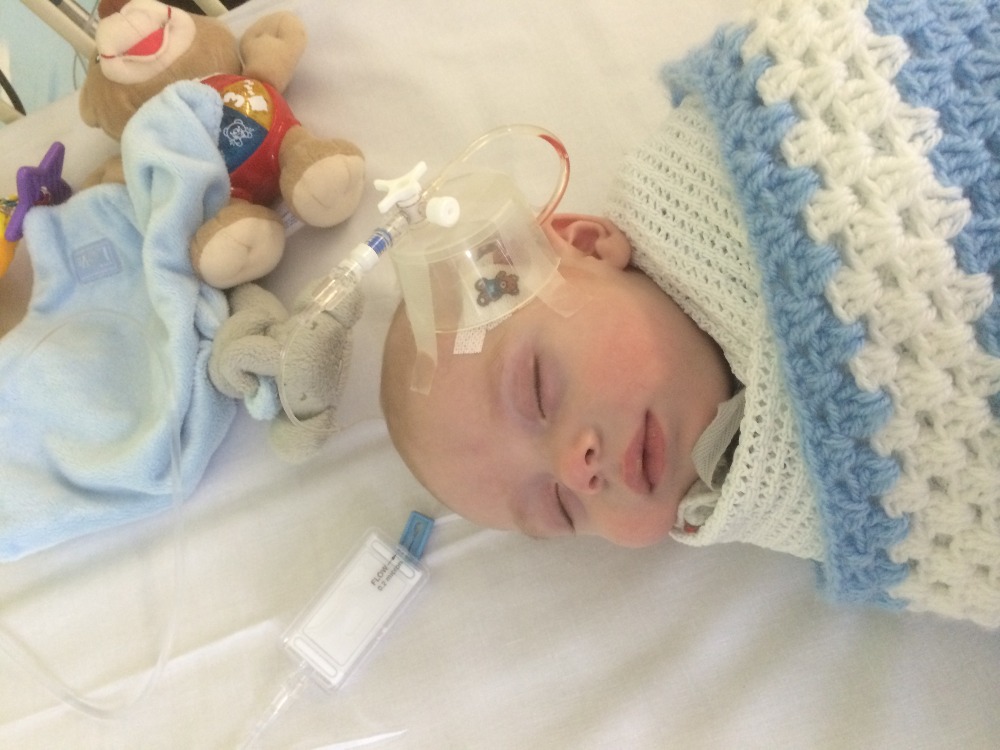
Orin is in hospital every Friday for his enzyme replacement therapy, as a result he had reached the point where it became near impossible to find a vein to put a cannula in and this meant only one thing… it was time for Orin to have surgery and risk the anaesthetic, although bigger and stronger than his sister, the risks were no different. The day of the surgery loomed like a dark cloud, various bugs and illnesses meant delay after delay, finally the day came. Not that I’m keeping score or anything but 1-0 pompe, Olivia's turn to get her port arrived, 2-0, next came the feeding peg she required to hook her feeding pump up to 3-0. Finally the day we all feared arrived, the arch nemesis raised his ugly head one more time.
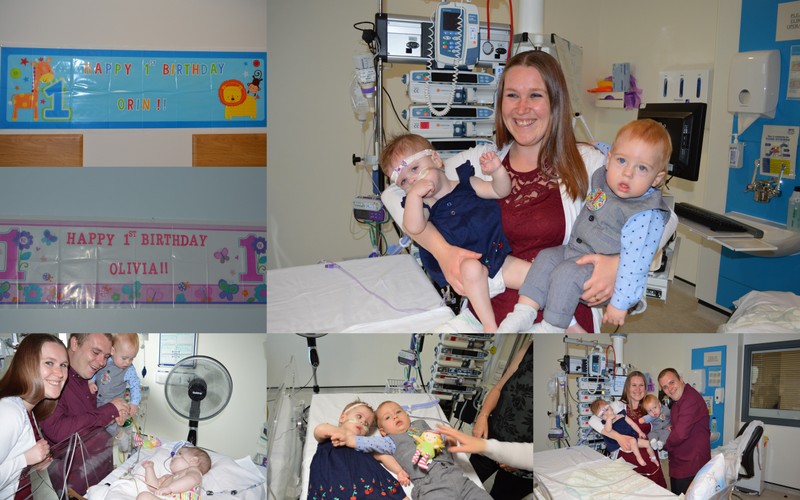
We had finally made it, 04/08/2015 happy birthday Orin AND Olivia. This was the most amazing day of our lives, we were never going to make it here! Wrong family! When you back a Doberman into the corner expect it to come out barking and snapping. On that day we became a pretty unique case, we are not following any book anymore, we are writing our own futures now.
Over the last month there was meeting, crisis meeting, discussions and heated discussions over the future. We had spent the previous months fighting tooth and nail to get Olivia off breathing support. All attempts ended either prematurely with a bug or an infection or ended in total failure.
5 litres of air doesn’t sound like very much, when you think of it in your mind you can’t even hold it, it feels like 1,000 tonnes of concrete when you can’t advance without removing it. After what felt like one million discussions over our options and the inevitable result, Olivia decided it was time to make some decisions of her own.
Until that day I had never thought of the difference between a respiratory arrest and a cardiac arrest, not that the difference mattered, Olivia had both in the space of a few days.
As Robert Burns once said “The best laid plans of mice and men often go awry”, Time for plan B version 10.6d!
The decision was now made. Olivia went to surgery to have a tracheostomy done the day after her birthday and began life on a long term ventilator. 4-0, not that we are keeping score of course!
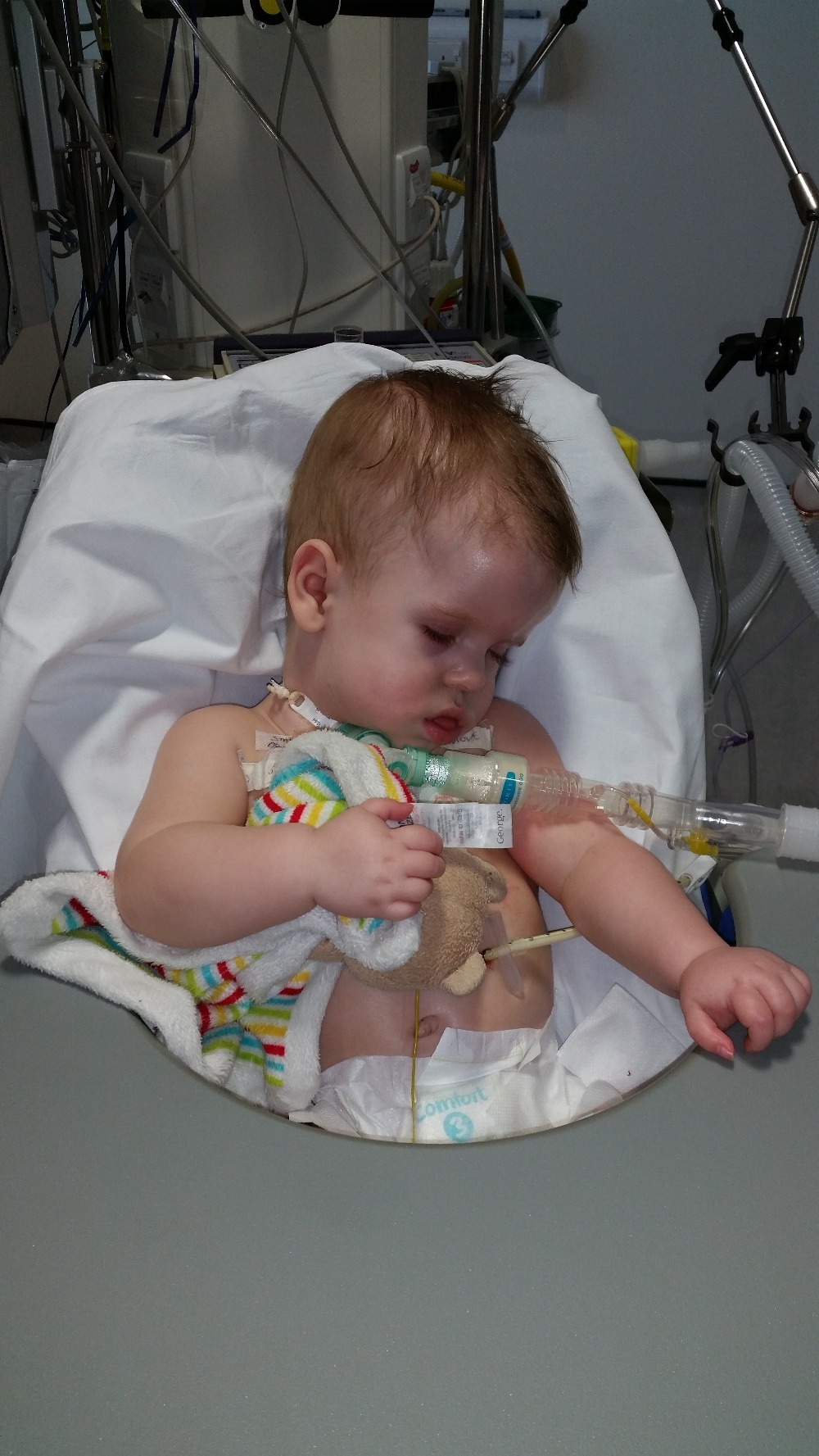
Olivia came back from surgery yet again.
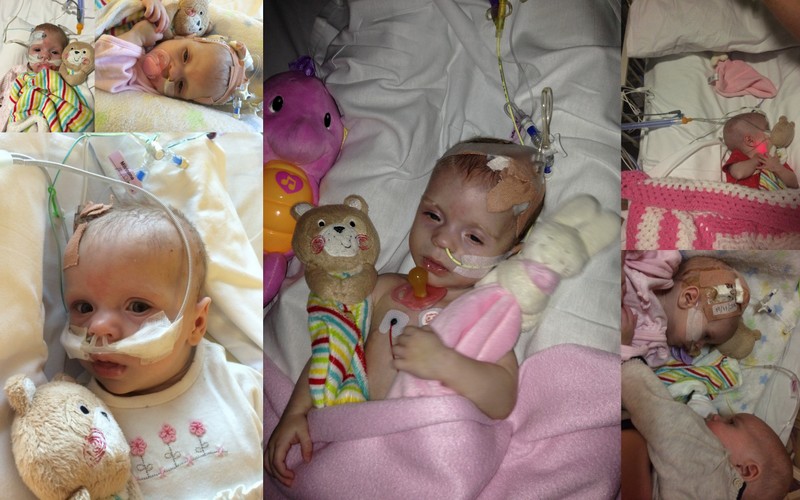
Now Olivia is known as the most chilled child in ICU, no matter what you have to do Olivia just runs with it. You want to take bloods? Fine just don’t get in the way of her watching frozen! It really is an insane sight to behold, Olivia watching tv without a tear or noise as a doctor stabs her foot and spends 10 minutes squeezing blood from it and Olivia’s only response is a dirty look as he announces he is done because he has interrupted her by making noise.
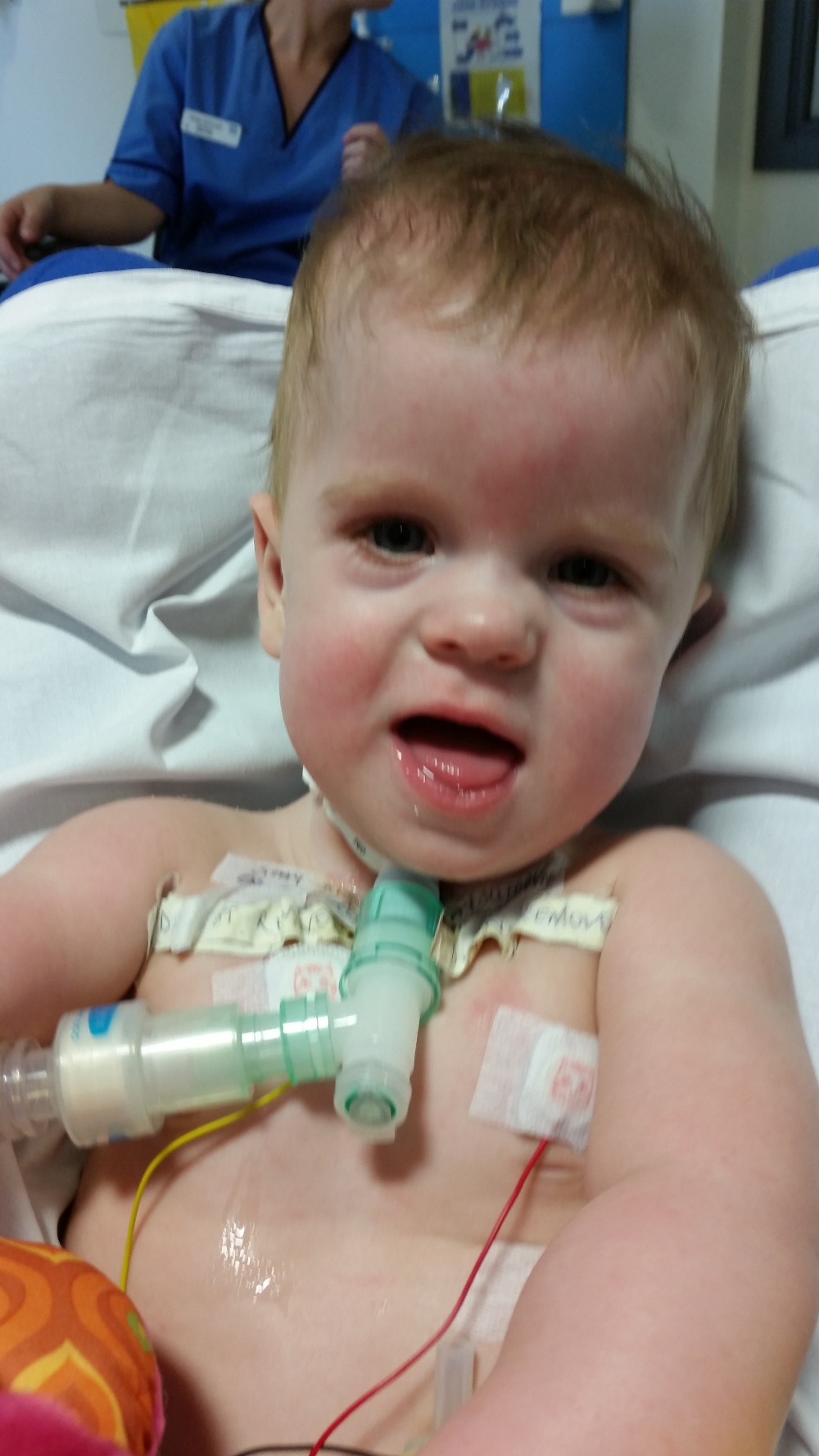
We get the call, Olivia’s back from surgery is sitting watching frozen, holding on to her precious “dolly”. As we walk in the consultant meets us to tell us that she’s just back and will probably sleep most of the day and be in a lot of pain, the news that she was awake and watching tv was met by the only response he could muster, he shook his head and walked off without a word lol.
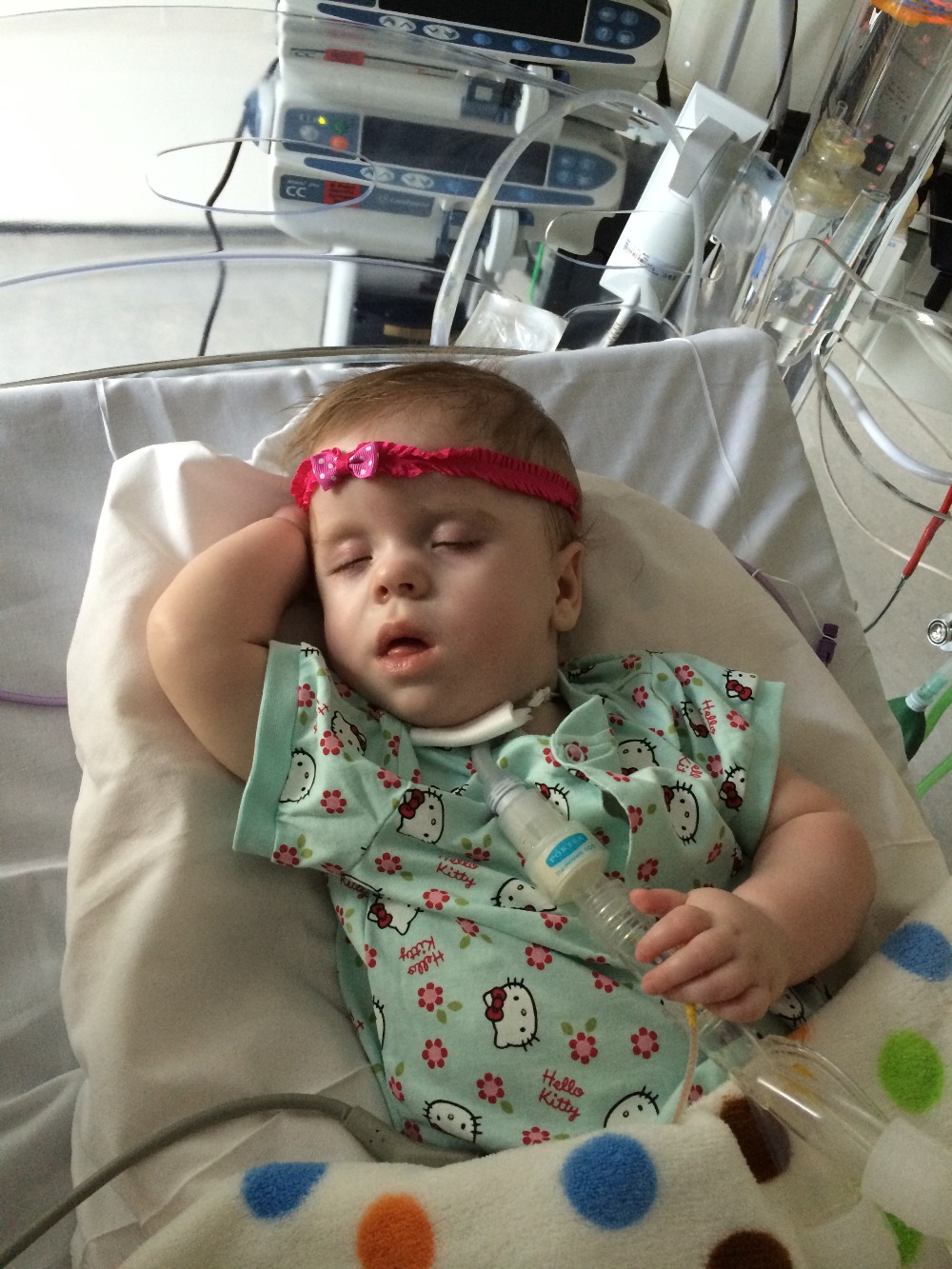
Olivia is now doing much better on the ventilator and has instantly adjusted to it, as we knew she would. This has opened the doors to a day we had long since stopped even thinking about. Olivia might be getting home in the next few months.
I say might because a child with a muscle wasting disease, a heart condition, feeding problems, a tracheostomy and long term ventilator does not just go home. There is a lot that needs to be in place for Olivia to be discharged from the hospital. we require a house the is specially adapted for her, she must have a large downstairs bedroom as she will have a lot of equipment and a dedicated nurse in the room at all times, the entire house will have to be tailored for Olivia as she will have a specialised chair which will require wheelchair access. We will have to have a vehicle adapted to take her new chair, as this new chair will carry her ventilator, feeding pump and equipment when she is on the move.
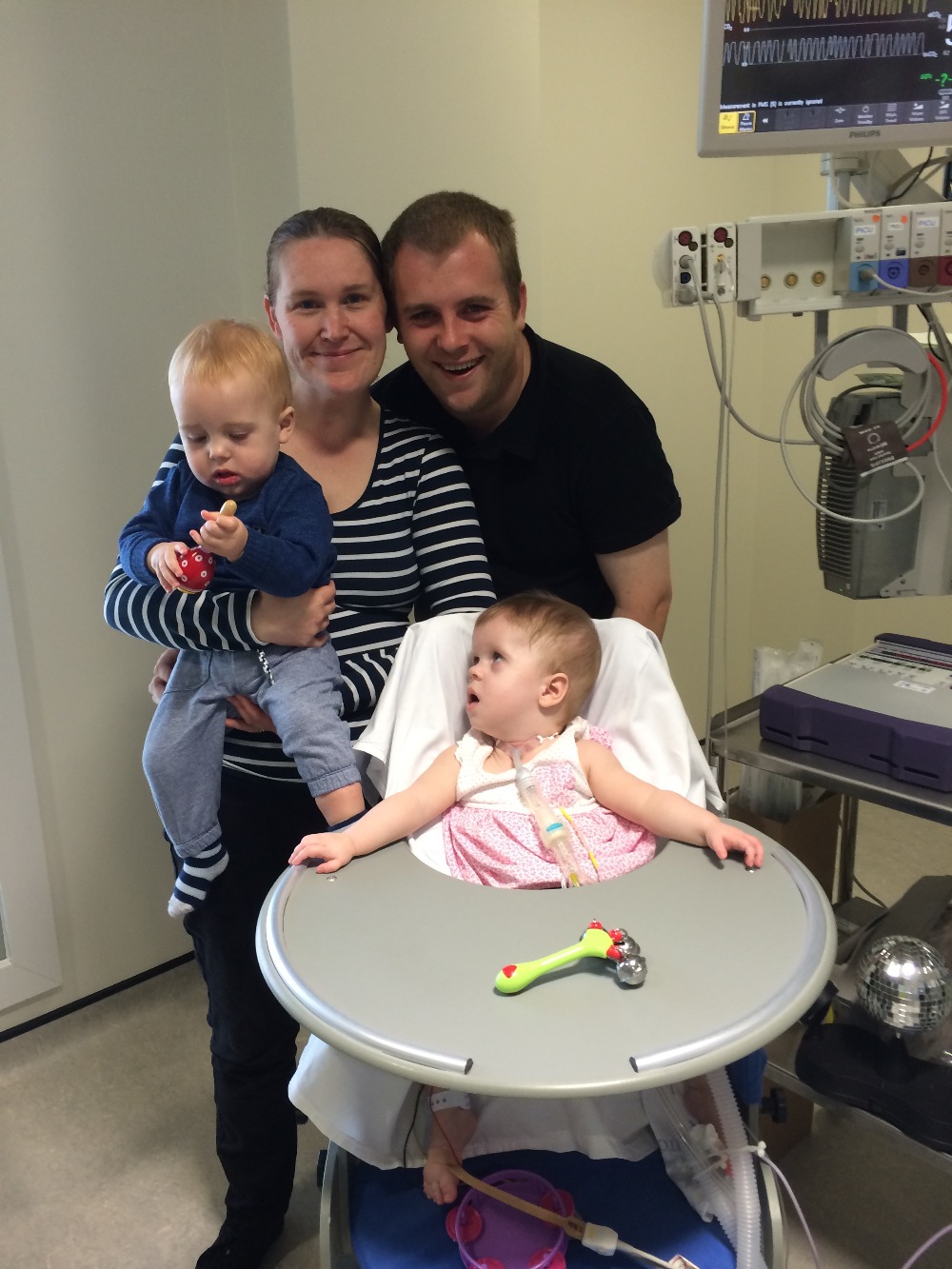
After 11 months living at the hospital with 2 children and not being able to work you can imagine our current financial situation. We have now found ourselves in a situation that is way beyond our control. Due to Olivia’s unpredictability and the speed at which she can crash we have found ourselves accepting we will be limited to an area close to the new Royal Hospital for Children in Govan. This in itself raises major problems. Glasgow is an area short of social housing and wait times are up to three years and even at that it may not be an area you would want to live in with two disabled children.
Here we are standing yet again with our backs to wall. Our situation has left us with no choice other than to put our careers on hold. We have also annihilated what savings we had over the last 11 months as living day to day in the hospital environment is extremely expensive.
Finally the end is in sight and we cannot go home because we cannot afford to!
After much discussion on how this situation could be solved it was suggested that we should start a gofundme page. Our aim is simple unfortunately it is also expensive.
We hope to raise enough money to purchase a home for the four of us to live in, as pompe is a progressive and life limiting disease we have to plan that the situation will escalate as time progresses, so we will require a single level house that may have two chair bound, ventilated children (I have to say, of all I have written here that is the single sentence the hurts the most). We will also need an adapted vehicle capable of taking Orin in his car seat, his buggy and Olivia in her chair. Finally as we currently renting a house we have day to day bills and day to day living expenses to cover.
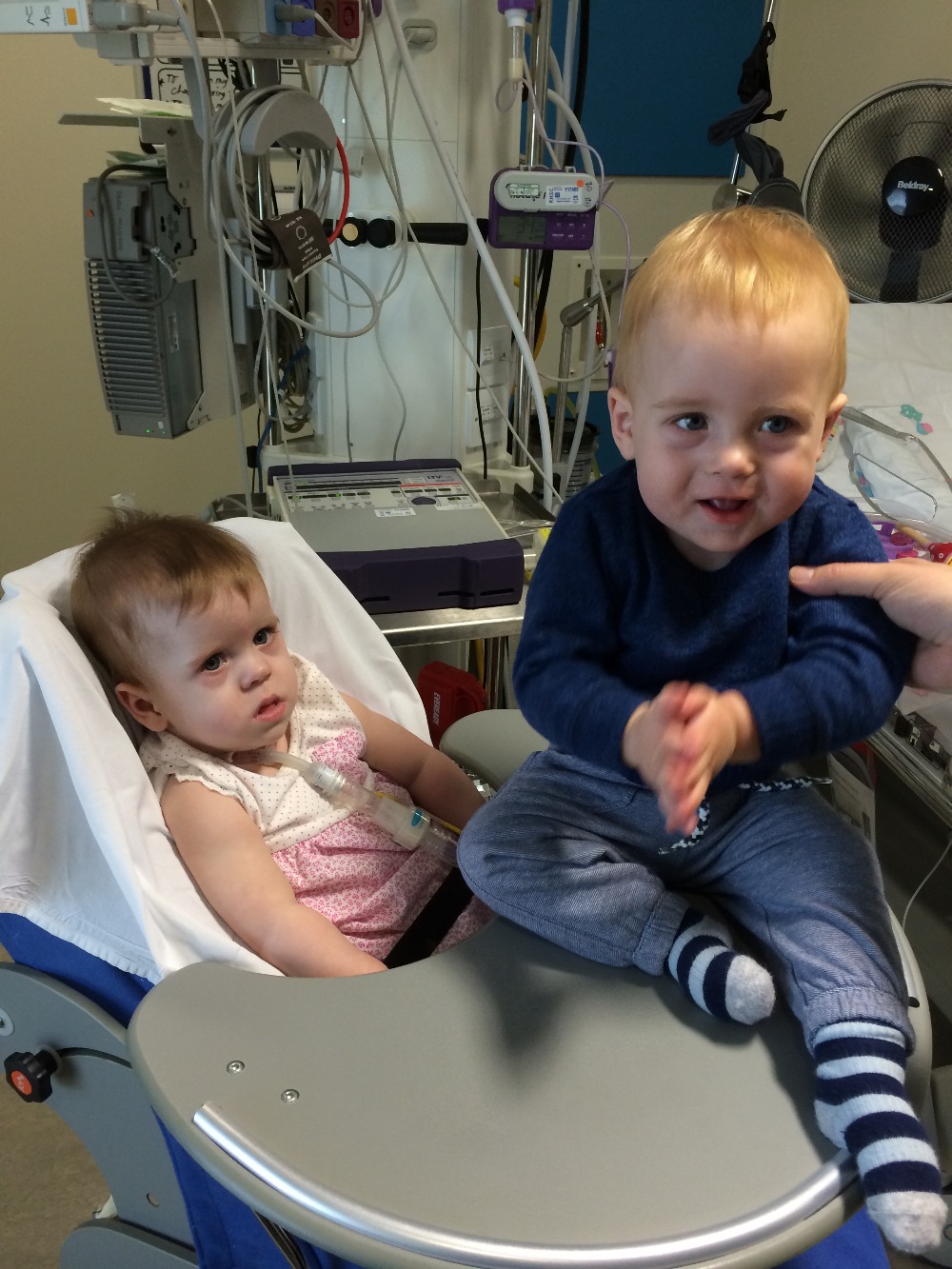
If you have made it this far I apologise for the length of our story, I have however made it as short as I could for you and I hope you can help in some way.
Thank you for taking the time you read our story so far, it is far from over and we will keep you all up to date on a regular basis