Hi all, my name is Jordan, and I’m creating this fundraiser for my dear friend Emily. She has been living with Complex Regional Pain Syndrome (CRPS)—one of the most painful and debilitating neurological conditions—after a skiing accident that tore her ACL. Over the past three years, I’ve watched her life completely change.
Emily and her family have already spent over $100,000 searching for relief. Emily now has the opportunity to pursue specialized treatment in North Carolina. She will need to relocate for three months, and the $42,000 treatment is not covered by insurance. We are hoping to raise $50,000 to cover the treatment, travel, and living expenses so she can focus fully on healing. I asked Emily to share her story in her own words:
My Journey with CRPS:
I’ve been living with chronic nerve pain for almost 3 years. And it’s been four years since the accident and surgery that started it all. In February 2022, I had a ski accident and tore my ACL in my right knee. This is a very common injury and a pretty straightforward surgery to repair, but my recovery process has been far from normal.
After my ACL reconstruction surgery, I still had a lot of knee pain despite rigorous physical therapy. So in October 2023, I underwent a second revision surgery. I was so optimistic that the second surgery would finally do the trick, so you can imagine how crushed I was when my knee pain persisted. In retrospect, I probably didn’t need the second surgery, as the pain I was feeling was from CRPS. But my family and I had never even heard of CRPS then, and apparently neither had my surgeon.
For the vast majority of people with CRPS, onset is triggered by a traumatic injury or surgery. Any major injury or surgery is a shock to the neural system, but with CRPS, the body essentially stays in that state of shock. After an injury, the body’s nervous system becomes activated and launches an inflammatory response to promote healing. This is normal at first, but with CRPS, the response becomes dysregulated and the nerve inflammation stays turned on, leading to persistent pain long after the original injury has healed. Even though my ACL has been reconstructed and my knee is structurally healed, my nervous system has essentially gotten “stuck” with pain as the default.
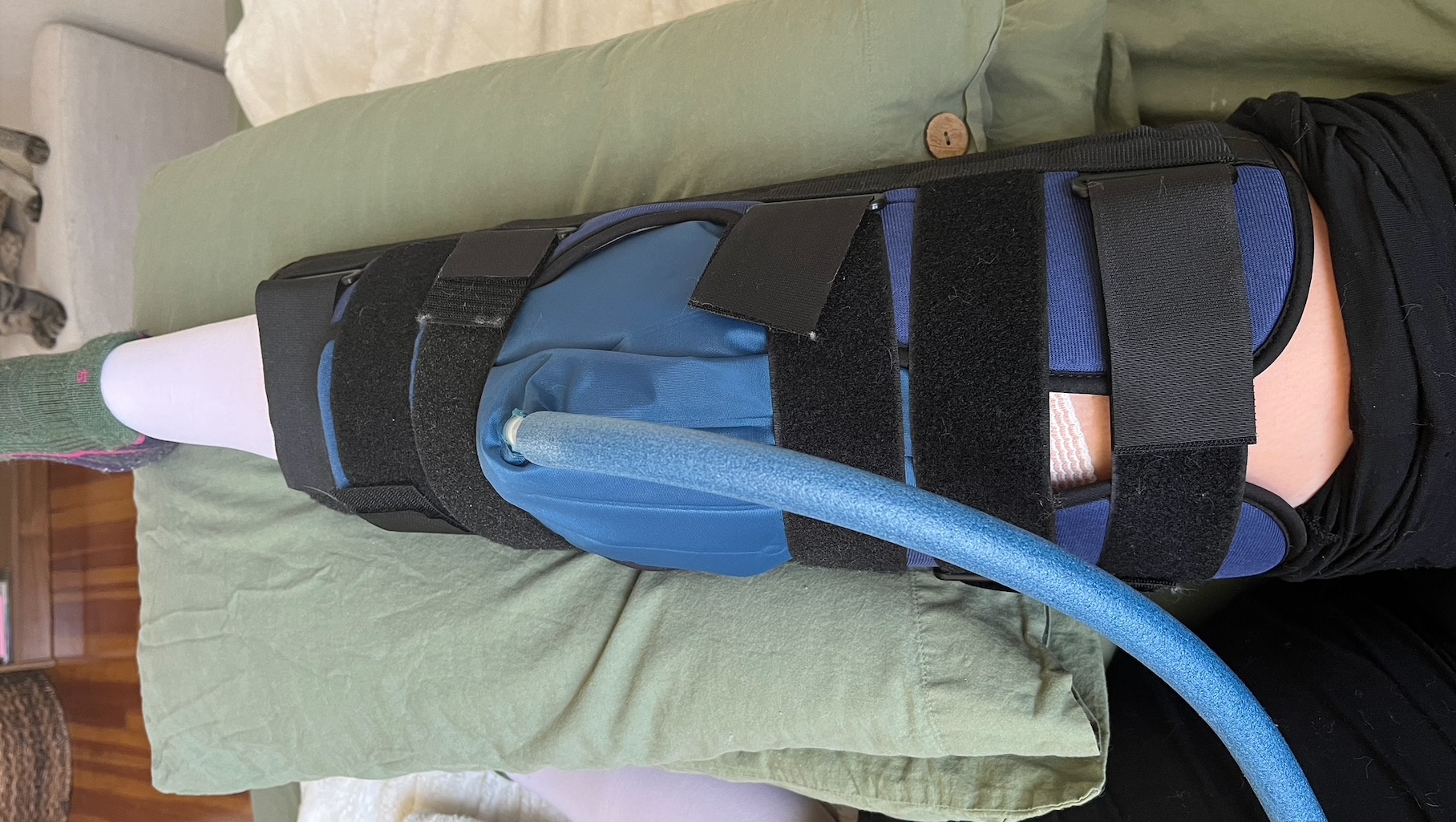

A few months after my second surgery, the pain – which is the very specific burning of nerve pain – started to radiate from my knee to my whole leg and foot. A few months after that, the pain spread to my left leg. This was an incredibly confusing experience, but was an important clue to the underlying issue, as pain spreading to the mirror limb or other parts of the body is common in CRPS. A few months later, I started to feel the burning nerve pain in my arms and hands. CRPS has now spread to my whole body. I have even felt nerve pain on the right side of my face and in my right eye. It took me a year and a half of seeing doctors and none of them being able to explain my pain until I was finally diagnosed with CRPS.
I also think it’s important to share that my dad passed away unexpectedly between the first and second surgeries. I have learned a lot about pain, and one of the most fascinating things I’ve learned is that at the deepest level, our bodies can’t tell the difference between emotional and physical pain. And grief can also manifest as pain in the body. Scientifically, CRPS is the result of a neurological malfunction in the central nervous system. There’s a chance that it could have been triggered for me by any injury, but I often wonder how much the specific sequence of physical and emotional trauma within a very short time period contributed to its onset.
What is CRPS?
CRPS is classified as rare, with a 0.005% incidence rate. It is also ranked as one of the most painful conditions known to humankind on the McGill Pain Scale. This score indicates that CRPS pain can be more severe than childbirth. When I read statistics like this after being diagnosed, I truly thought that my life was going to be ruined by this condition. It was a very scary and dark time; I wanted to be informed and learn about my diagnosis, but the more I read about it the more fearful I became. I read that CRPS is nicknamed the “Suicide Disease” because there is no cure for the condition, and because the pain can be so severe it feels like you’re being burned alive. I recognize there is a lot of shock value in these statements, and they took a huge toll on my mental health at first.
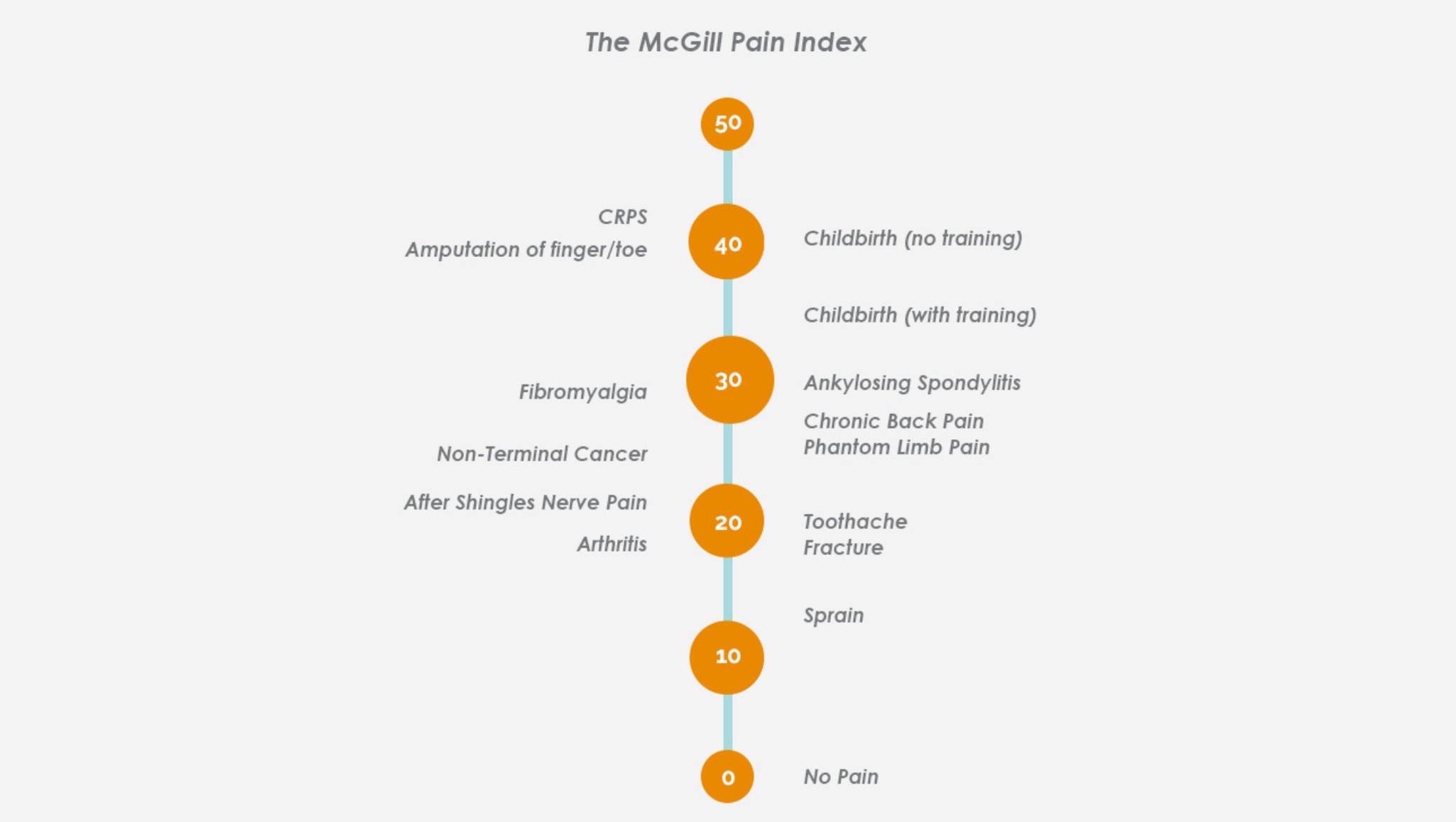
At its worst, I’ve felt pain that is probably an 8 out of 10, if 10 is the worst pain imaginable. I’ve been in so much pain that I could barely even speak. It really did feel like my whole body was on fire. Because I was fortunate to begin treating my symptoms early, I have been able to lower my pain a lot, and I do not feel this level of excruciating pain on a daily basis. I can tell the thousands of hours I’ve spent trying to get better are working. These days, my pain fluctuates a lot. I’ll still have flare ups, but some days it’s very manageable. Some days I just feel a tingly, buzzing, pins-and-needles sensation. It's uncomfortable and I can feel my nerves mis-firing, but those are good days compared to really painful ones.
Treating CRPS:
Just because there is currently no cure for CRPS, it does not mean that healing isn’t possible. It just means that there isn’t a drug that reverses the condition. And I personally don’t think that healing from CRPS will come from medication. I've been put on a lot of different meds over the past three years (gabapentin, steroids, duloxetine, and low-dose naltrexone, to name a few). They haven’t helped my pain much, and I have experienced really terrible side effects from some. I have also tried a ton of treatments, including:
- Lumbar sympathetic nerve blocks
- Vagus nerve stimulation
- Pulsed electromagnetic field therapy (PEMF)
- Transcutaneous Electrical Nerve Stimulation
- Red light therapy
- Neurofeedback
- Low light laser therapy
- Neuroplasticity training
- Biofeedback using heart rate variability (HRV)
- Frequency-Specific Microcurrent
- Neurologic rehabilitation
- Ketamine infusions

In addition to these “medical” or western treatments, I’ve also tried many holistic and eastern treatments like acupuncture, reiki, trauma release exercises, and more. The combination of all of these has helped bring my pain down a lot. I believe that it will take a multi-disciplinary approach to fully heal.
There are only a few CRPS specialists in the world. In January 2025, I travelled to Boise, Idaho, to see one of these specialists, Dr. Traci Patterson. I did 4-5 hours of treatments every day for two weeks in Idaho, and I am ecstatic to report that my pain has never flared up as bad as it did before I went to this doctor! My family and I spent $12,000 to see this specialist for two weeks. The financial burden was very worth it for the relief it brought.

Even though my stint in Idaho was tremendously helpful, my pain still persists. My family and I have decided that the next step is to go see another specialist, Dr. David Pascal, in North Carolina. He’s recommended that I come for 3 months of treatment, as that is the average length of time he treats someone with full body CRPS.
Even though there’s no cure yet, pain remission can be possible and both Dr. Patterson and Dr. Pascal have helped CRPS patients go into long-term remission. Unfortunately, these specialized CRPS treatment programs are not covered by insurance. Without getting on a soapbox about how broken our health care system is, the main reason is because CRPS is very rare, poorly understood, and underfunded. As such, large clinical trial data on CRPS treatments simply does not exist. Without clinical data, insurers label the treatments as investigative, experimental, or not medically necessary.
There is also ongoing debate in the medical field about whether CRPS has an autoimmune component (It certainly feels like my body is attacking itself!). Dr. Pascal takes a holistic approach and looks at ALL of the systems in the body. His approach is also non-invasive, and I want to exhaust all of the non-invasive options I can before exploring one of the only treatments I haven’t tried yet: a spinal cord stimulator. These are devices that are surgically implanted into the spinal cord and deliver mild electrical impulses to help disrupt pain signals before they reach the brain. Stimulators only have about a 50% success rate, and I’ve heard horror stories from people in the CRPS community. This is Plan Z, and I am very optimistic that Dr. Pascal’s treatments will mean I never have to consider this option.
Not that long ago, I didn’t have any health issues. And now I’m having to temporarily uproot my life to seek care for this condition. But I really have made immense progress already, and I know that healing is possible. I will stop at nothing to get my pain-free life back.

Thank you from the bottom of my heart for taking the time to read Emily’s story and for considering supporting her in this journey. Every donation, no matter the amount, brings her one step closer to healing and relief. We are incredibly grateful for your kindness—and even sharing this page can make a meaningful difference.
Beyond the support, Emily hopes that sharing her story helps raise awareness about CRPS and, one day, leads to better understanding and support for those living with this condition.