- D
- R
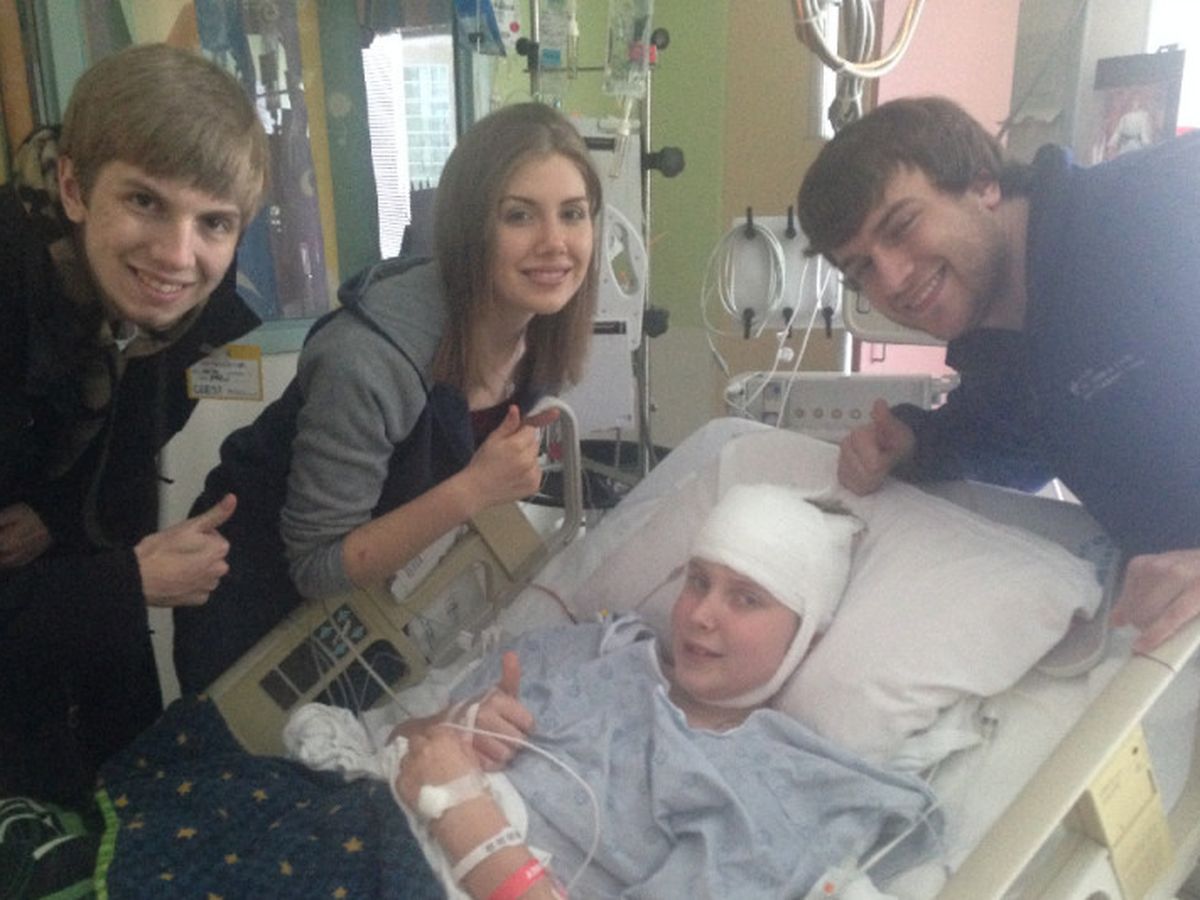
Gina (Dal Ponte) Vugrin and her family have had a very tough year and they need your help. On 12/3/16 Gina’s youngest boy, Luke, was diagnosed with a craniopharyngioma tumor. This tumor was resting on Luke’s pituitary gland and optic nerve and was blocking the channel in which the cerebral spinal fluid drains to the rest of the body causing brain swelling. They quickly found out how serious this was and that surgery was immediately needed. On 12/9/2016 a group of amazing surgeons removed that tumor completely. Luke has been on a new journey since that tumor was removed as his body is learning how to function without many necessary hormones due to the brain injury he sustained from the removal of the tumor. There have been numerous doctors’ appointments, consultations, emergency visits, since the surgery but they remain hopeful and amaze me with their positive attitude. Luke is eager to graduate 8th grade and enter high school and remains positive.
In addition to Luke’s journey the family has many other hardships they are currently enduring. Two of Gina’s children are struggling with auto-immune diseases that require frequent doctor’s visits and have also required hospitalizations. Her son Jonathan, may be facing surgery due to his active Crohn’s Disease. Gina’s husband, Mike, is unable to work due to his medical condition worsening and is waiting for an O positive liver transplant. Gina must be present at all the appointments for her children and husband and is always with them during hospitalizations etc. Gina manages to juggle all of this while maintaining her full time job, she truly is a woman of many hats. Without the financial support from her spouse due to his illness, Gina is trying to support her family and maintain financial responsibility for all the expenses that have resulted from her family’s rising medical circumstances. I know Gina’s main goal is to get awareness out for Luke so people will get a better understanding of what he is going through. The intention of this page is also to help Gina and her family with medical expenses and personal expenses. I know Gina and her family would benefit from any donation and will be so grateful.
Below is Gina’s personal account of Luke’s journey and also the background of craniopharyngioma tumors, as it is a very complex condition. Thank you for your consideration and for helping The Vugrin family spread awareness! Luke’s journey with Craniopharyngioma
Luke’s journey with Craniopharyngioma
Luke had been complaining of daily headaches which were getting progressively worse throughout most of November 2016. After several trips to the doctor and several diagnoses (sinus infection, virus, allergies etc.) his doctors finally ordered an MRI. On 12/3/2016 Luke had an MRI of his brain. Still miserable with headaches said to me “I mean I don’t want them to find anything bad, but I hope they can find a way to make these headaches go away”. I agreed. After returning home several hours later I receive a call from his pediatrician asking how Luke was doing. I said the same. He then told me that the MRI showed something. He, at the time, did not tell me what is was. He told me to get Luke, put him in the car and return to the hospital right away. When I told Luke he began to cry immediately. I told him everything would be ok. When we got back his doctor was in the ER waiting for him. He explained there was a mass, it was not cancer, but it was very serious and we needed to see the neurosurgeon right away. Luke was then admitted to the PICCU. The neurosurgeon came pretty quick and explained to us that this tumor is called a craniopharyngioma and it was sitting on Luke’s pituitary gland and optic nerve and was blocking the channel in which the cerebral spinal fluid drains to the rest of the body. This was causing hydrocephalus (swelling to the brain). They scheduled a surgery the next morning to put a drain in to help to relieve the pressure. Luke was terrified to have to have surgery, but everything went very well and after a day or so his headaches were gone. We were then told that the tumor needed to be removed. After several days of planning they decided that this would be done on 12/9/2016. After many long days Luke’s surgery day came. It was a very stressful day for everyone, but especially Luke. Needless to say he did AWESOME!!! Many thanks to 2 excellent surgeons, lots of prayers, and an outpouring of love and support by many family members and friends. It was finally over and my first thought was thank God now he could finally heal and get back to his normal 14 year old life.
So another journey began. Although Luke started to heal on the outside, he was faced with so many complications of this tumor on the inside. The first was a water imbalance in his body that made him obsessively drink whatever he could get his hands on and then he would urinate excessive amount of fluid uncontrollably. This is called diabetes insipidus and it was due to damage to the part of his brain that controls your water balance. He also started to rapidly gain weight from the high doses of steroids and his body would no longer be making TSH (thyroid) anymore. After getting all of these things regulated Luke was ready to go home. Still thinking
all of this will be over soon and things will get back to normal and he would just have to take some medications.
Several days later after Luke was settled back at home we had to make another trip to the ER. And about a week after that Luke had to be readmitted due to his body going into an adrenal crisis. This is when we found out that his body no longer made cortisol, which is a vital steroid that your body needs. Without cortisol you cannot survive. So he was prescribed hydrocortisone that he needs to take three times a day for the rest of his life. We were also told that if for some reason he could not physically swallow the pills because of vomiting or unconsciousness he would need to be injected with an emergency dose of steroids. He also has to be very cautious when he gets sick. If he has a fever of 100.4 or higher or if he is very ill he needs to stress dose and take 3x the normal amount of the hydrocortisone due to the fact that cortisol helps your body fight stress and he cannot naturally produce it anymore. After weeks of seeing doctor after doctor and be physically and emotionally exhausted we were still getting bad news. Luke was afraid to even go to another doctor because all they told him was more bad news that he didn’t want to hear.
After seeing the hematologist/oncologist we were happy to have been told that because the tumor had been completely resected Luke would not need any radiation. Finally some good news!!! He would just need lifelong scans to make sure that the tumor would not return. But we also learned that the limbic system in his brain had been damaged. This is the part that controls emotions. This was hard on Luke because he can’t control emotions and his body has a hard time processing stress to begin with. We luckily found a therapist who has been helping Luke deal with all of this.
After daily phone calls with his endocrinologist we finally seemed to get most of his medications regulated. We then found out that he was deficient in a couple more areas. Luke was not producing growth hormones and unfortunately we were told that giving him growth hormone replacement could cause the tumor to grow back. And also his body stopped producing testosterone but luckily he can get monthly injections to replace this.
Thinking we are on our way Luke’s weight gain continued and he is struggling to lose weight. This we were told by the endocrinologist is probably a result in damage to the hypothalamus and unfortunately there is not a lot that can be done for this. Many times it results in gastric bypass surgery. We were very excited when we got a call from his doctor and she had found a study at Children’s in Minnesota that deals with this exact tumor and the effects of the damage on weight gain. Luke was so excited about this he even told his friends he was finally going to be able to lose weight. We are hoping to start this 36 week study in July 2017.
The latest complication has been elevated heart rate. We are being told that this too could be a result of injury from the tumor to the part of the hypothalamus that helps control heart rate. Fortunately there are medications for this as well.
I believe that this journey will continue, but not downhill. We continue to have a positive attitude and we are looking up. Luke will have to be on lifelong medications and have routine MRI’s, but he will continue to manage this and look forward to his bright future. He was recently accepted to St. Rita and is looking forward to his high school days. Even though this tumor destroyed so much and caused a family’s life to be turned upside down it didn’t win.
I am so very proud of Luke. I call him my brain tumor warrior. Because that is what he is. He has been fighting so hard to beat this and he is winning. Although we will never understand why this happened to our Luke, we will move on and just thank God for the outcome. As long as I can kiss him and hug him every day, I know things will be ok. Like I said the journey is not over, but I believe we are starting a new journey.
I just want to say that my heart feels as if it will burst sometimes when I think about all the love and support we have received. I could never have done any of this on my own. I am grateful especially to Luke that he is such an amazing kid. If we didn’t have each other those 14 long days in the hospital I don’t know what we would have done. I actually think I needed him more than he needed me. I am so very blessed for my family, especially my mom and dad and all our friends and community. We are truly loved and blessed.
Background information on Craniopharyngioma
Craniopharyngioma is a benign brain tumor that accounts for about 3-9% of all pediatric CNS tumors. This tumor results from abnormal overgrowth of a part of the brain called Rathke's pouch, located near the pituitary gland. Craniopharyngiomas do not represent cancers, and craniopharyngioma does not spread to other parts of the central nervous system or body; however, craniopharyngiomas develop in a part of the brain where their growth can cause problems with hormone secretion (from compression of the pituitary gland), or vision (from compression of the nerves responsible for sight).
Craniopharyngiomas can occur in both children and adults, with a peak in incidence at 9 to 14 years of age. There are approximately 120 cases diagnosed each year in the United States in patients under the age of 19 years old. In fact, more than 50% of all patients with craniopharyngioma are under the age of 18 years. There is no clear association of the tumor with a particular gender or race. It is not really known what causes craniopharyngiomas, but they do not appear to "run in families" or to be directly inherited from the parents.
The craniopharyngioma is known to cause permanent damage to many of the brain structures after removal. In Luke’s case he has been fortunate to have had very little damage to his vision. The major structures that are damage for him are the pituitary gland and the hypothalamus thus causing hypopituitarism and hypothalamic injury.
Hypopituitarism refers to any under function of the pituitary gland. This means that more than function of the pituitary gland are deficient. This damage from the tumor to the pituitary includes growth hormones, gonadotropins which control sexual/reproductive function, TSH (which controls the thyroid hormone release and ACTH which controls the adrenal function.
Deficiency of ACTH resulting in cortisol deficiency is the most dangerous and life threatening of the hormonal deficiency syndromes. Symptoms include fatigue, weakness, depression, apathy, nausea, vomiting, anorexia and hyperpigmentation. As the deficiency becomes more serious or has a more rapid onset, (Addisonian crisis) symptoms may include confusion, stupor, psychosis, abnormal electrolytes (low serum sodium, elevated serum potassium), and vascular collapse (low blood pressure and shock) which can be fatal. Treatment consists of cortisol administration or another similar steroid (like prednisone). For patients with acute adrenal insufficiency (Addisonian crisis), rapid intravenous administration of high dose steroids is essential to reverse the crisis.
Deficiency of TSH and thyroid hormone
Deficiency of thyroid hormone causes a syndrome consisting of decreased energy, increased need to sleep, intolerance of cold (inability to stay warm), dry skin, constipation, muscle aching and decreased mental functions. This constellation of symptoms is very uncomfortable and is often the symptom complex that drives patients with pituitary disease to seek medical
attention. Replacement therapy consists of a daily pill called thyroxine (Synthroid, Levothyroxine etc). The correct dose is determined through blood tests.
Deficiency of LH and FSH (Hypogonadotropic Hypogonadism).
Testosterone deficiency and replacement therapy. On testing, blood levels of testosterone are low and should be replaced by monthly injections.
Growth Hormone Deficiency
Growth hormone is necessary in children for growth, but also appears necessary in adults to maintain normal body composition (muscle and bone mass). It may also be helpful for maintaining an adequate energy level, optimal cardiovascular status and some mental functions. Symptoms of GH deficiency in adults include fatigue, poor exercise performance and symptoms of social isolation. This being said GH replacement is not an option due to the fact that it could cause tumour reoccurrence.
Antidiuretic Hormone deficiency causing diabetes insipidus
This problem arises from damage to the pituitary stalk or the posterior pituitary gland. Patients with diabetes insipidus have increased thirst and urination. Replacement of antidiuretic hormone resolves these symptoms. Antidiuretic hormone (ADH) is currently replaced by administration of DDAVP (also called Desmopressin).
The hypothalamus plays a huge role in both the endocrine and nervous systems. Craniopharyngioma’s often cause injury to the hypothalamus causing many dysfunctions. The role of the hypothalamus and its functions are as follows:
* Body temperature
* Thirst
* Appetite and weight control (hypothalamic obesity)
* Emotions (limbic system disorders)
* Sleep cycles
* Sex drive
* Childbirth * Blood pressure and heart rate
* Production of digestive juices
* Balancing bodily fluids
Hormones of the hypothalamus
To maintain this balance, the hypothalamus is responsible for creating or controlling many hormones in the body. The hypothalamus is also closely related to the pituitary gland, which makes and sends other important hormones around the body.
Together, the hypothalamus and pituitary gland work to control the entire endocrine system, the glands that produce many hormones of the body. This includes the adrenal glands, kidneys, and thyroid.
In addition to Luke’s journey the family has many other hardships they are currently enduring. Two of Gina’s children are struggling with auto-immune diseases that require frequent doctor’s visits and have also required hospitalizations. Her son Jonathan, may be facing surgery due to his active Crohn’s Disease. Gina’s husband, Mike, is unable to work due to his medical condition worsening and is waiting for an O positive liver transplant. Gina must be present at all the appointments for her children and husband and is always with them during hospitalizations etc. Gina manages to juggle all of this while maintaining her full time job, she truly is a woman of many hats. Without the financial support from her spouse due to his illness, Gina is trying to support her family and maintain financial responsibility for all the expenses that have resulted from her family’s rising medical circumstances. I know Gina’s main goal is to get awareness out for Luke so people will get a better understanding of what he is going through. The intention of this page is also to help Gina and her family with medical expenses and personal expenses. I know Gina and her family would benefit from any donation and will be so grateful.
Below is Gina’s personal account of Luke’s journey and also the background of craniopharyngioma tumors, as it is a very complex condition. Thank you for your consideration and for helping The Vugrin family spread awareness!
 Luke’s journey with Craniopharyngioma
Luke’s journey with CraniopharyngiomaLuke had been complaining of daily headaches which were getting progressively worse throughout most of November 2016. After several trips to the doctor and several diagnoses (sinus infection, virus, allergies etc.) his doctors finally ordered an MRI. On 12/3/2016 Luke had an MRI of his brain. Still miserable with headaches said to me “I mean I don’t want them to find anything bad, but I hope they can find a way to make these headaches go away”. I agreed. After returning home several hours later I receive a call from his pediatrician asking how Luke was doing. I said the same. He then told me that the MRI showed something. He, at the time, did not tell me what is was. He told me to get Luke, put him in the car and return to the hospital right away. When I told Luke he began to cry immediately. I told him everything would be ok. When we got back his doctor was in the ER waiting for him. He explained there was a mass, it was not cancer, but it was very serious and we needed to see the neurosurgeon right away. Luke was then admitted to the PICCU. The neurosurgeon came pretty quick and explained to us that this tumor is called a craniopharyngioma and it was sitting on Luke’s pituitary gland and optic nerve and was blocking the channel in which the cerebral spinal fluid drains to the rest of the body. This was causing hydrocephalus (swelling to the brain). They scheduled a surgery the next morning to put a drain in to help to relieve the pressure. Luke was terrified to have to have surgery, but everything went very well and after a day or so his headaches were gone. We were then told that the tumor needed to be removed. After several days of planning they decided that this would be done on 12/9/2016. After many long days Luke’s surgery day came. It was a very stressful day for everyone, but especially Luke. Needless to say he did AWESOME!!! Many thanks to 2 excellent surgeons, lots of prayers, and an outpouring of love and support by many family members and friends. It was finally over and my first thought was thank God now he could finally heal and get back to his normal 14 year old life.
So another journey began. Although Luke started to heal on the outside, he was faced with so many complications of this tumor on the inside. The first was a water imbalance in his body that made him obsessively drink whatever he could get his hands on and then he would urinate excessive amount of fluid uncontrollably. This is called diabetes insipidus and it was due to damage to the part of his brain that controls your water balance. He also started to rapidly gain weight from the high doses of steroids and his body would no longer be making TSH (thyroid) anymore. After getting all of these things regulated Luke was ready to go home. Still thinking
all of this will be over soon and things will get back to normal and he would just have to take some medications.
Several days later after Luke was settled back at home we had to make another trip to the ER. And about a week after that Luke had to be readmitted due to his body going into an adrenal crisis. This is when we found out that his body no longer made cortisol, which is a vital steroid that your body needs. Without cortisol you cannot survive. So he was prescribed hydrocortisone that he needs to take three times a day for the rest of his life. We were also told that if for some reason he could not physically swallow the pills because of vomiting or unconsciousness he would need to be injected with an emergency dose of steroids. He also has to be very cautious when he gets sick. If he has a fever of 100.4 or higher or if he is very ill he needs to stress dose and take 3x the normal amount of the hydrocortisone due to the fact that cortisol helps your body fight stress and he cannot naturally produce it anymore. After weeks of seeing doctor after doctor and be physically and emotionally exhausted we were still getting bad news. Luke was afraid to even go to another doctor because all they told him was more bad news that he didn’t want to hear.
After seeing the hematologist/oncologist we were happy to have been told that because the tumor had been completely resected Luke would not need any radiation. Finally some good news!!! He would just need lifelong scans to make sure that the tumor would not return. But we also learned that the limbic system in his brain had been damaged. This is the part that controls emotions. This was hard on Luke because he can’t control emotions and his body has a hard time processing stress to begin with. We luckily found a therapist who has been helping Luke deal with all of this.
After daily phone calls with his endocrinologist we finally seemed to get most of his medications regulated. We then found out that he was deficient in a couple more areas. Luke was not producing growth hormones and unfortunately we were told that giving him growth hormone replacement could cause the tumor to grow back. And also his body stopped producing testosterone but luckily he can get monthly injections to replace this.
Thinking we are on our way Luke’s weight gain continued and he is struggling to lose weight. This we were told by the endocrinologist is probably a result in damage to the hypothalamus and unfortunately there is not a lot that can be done for this. Many times it results in gastric bypass surgery. We were very excited when we got a call from his doctor and she had found a study at Children’s in Minnesota that deals with this exact tumor and the effects of the damage on weight gain. Luke was so excited about this he even told his friends he was finally going to be able to lose weight. We are hoping to start this 36 week study in July 2017.
The latest complication has been elevated heart rate. We are being told that this too could be a result of injury from the tumor to the part of the hypothalamus that helps control heart rate. Fortunately there are medications for this as well.
I believe that this journey will continue, but not downhill. We continue to have a positive attitude and we are looking up. Luke will have to be on lifelong medications and have routine MRI’s, but he will continue to manage this and look forward to his bright future. He was recently accepted to St. Rita and is looking forward to his high school days. Even though this tumor destroyed so much and caused a family’s life to be turned upside down it didn’t win.
I am so very proud of Luke. I call him my brain tumor warrior. Because that is what he is. He has been fighting so hard to beat this and he is winning. Although we will never understand why this happened to our Luke, we will move on and just thank God for the outcome. As long as I can kiss him and hug him every day, I know things will be ok. Like I said the journey is not over, but I believe we are starting a new journey.
I just want to say that my heart feels as if it will burst sometimes when I think about all the love and support we have received. I could never have done any of this on my own. I am grateful especially to Luke that he is such an amazing kid. If we didn’t have each other those 14 long days in the hospital I don’t know what we would have done. I actually think I needed him more than he needed me. I am so very blessed for my family, especially my mom and dad and all our friends and community. We are truly loved and blessed.
Background information on Craniopharyngioma
Craniopharyngioma is a benign brain tumor that accounts for about 3-9% of all pediatric CNS tumors. This tumor results from abnormal overgrowth of a part of the brain called Rathke's pouch, located near the pituitary gland. Craniopharyngiomas do not represent cancers, and craniopharyngioma does not spread to other parts of the central nervous system or body; however, craniopharyngiomas develop in a part of the brain where their growth can cause problems with hormone secretion (from compression of the pituitary gland), or vision (from compression of the nerves responsible for sight).
Craniopharyngiomas can occur in both children and adults, with a peak in incidence at 9 to 14 years of age. There are approximately 120 cases diagnosed each year in the United States in patients under the age of 19 years old. In fact, more than 50% of all patients with craniopharyngioma are under the age of 18 years. There is no clear association of the tumor with a particular gender or race. It is not really known what causes craniopharyngiomas, but they do not appear to "run in families" or to be directly inherited from the parents.
The craniopharyngioma is known to cause permanent damage to many of the brain structures after removal. In Luke’s case he has been fortunate to have had very little damage to his vision. The major structures that are damage for him are the pituitary gland and the hypothalamus thus causing hypopituitarism and hypothalamic injury.
Hypopituitarism refers to any under function of the pituitary gland. This means that more than function of the pituitary gland are deficient. This damage from the tumor to the pituitary includes growth hormones, gonadotropins which control sexual/reproductive function, TSH (which controls the thyroid hormone release and ACTH which controls the adrenal function.
Deficiency of ACTH resulting in cortisol deficiency is the most dangerous and life threatening of the hormonal deficiency syndromes. Symptoms include fatigue, weakness, depression, apathy, nausea, vomiting, anorexia and hyperpigmentation. As the deficiency becomes more serious or has a more rapid onset, (Addisonian crisis) symptoms may include confusion, stupor, psychosis, abnormal electrolytes (low serum sodium, elevated serum potassium), and vascular collapse (low blood pressure and shock) which can be fatal. Treatment consists of cortisol administration or another similar steroid (like prednisone). For patients with acute adrenal insufficiency (Addisonian crisis), rapid intravenous administration of high dose steroids is essential to reverse the crisis.
Deficiency of TSH and thyroid hormone
Deficiency of thyroid hormone causes a syndrome consisting of decreased energy, increased need to sleep, intolerance of cold (inability to stay warm), dry skin, constipation, muscle aching and decreased mental functions. This constellation of symptoms is very uncomfortable and is often the symptom complex that drives patients with pituitary disease to seek medical
attention. Replacement therapy consists of a daily pill called thyroxine (Synthroid, Levothyroxine etc). The correct dose is determined through blood tests.
Deficiency of LH and FSH (Hypogonadotropic Hypogonadism).
Testosterone deficiency and replacement therapy. On testing, blood levels of testosterone are low and should be replaced by monthly injections.
Growth Hormone Deficiency
Growth hormone is necessary in children for growth, but also appears necessary in adults to maintain normal body composition (muscle and bone mass). It may also be helpful for maintaining an adequate energy level, optimal cardiovascular status and some mental functions. Symptoms of GH deficiency in adults include fatigue, poor exercise performance and symptoms of social isolation. This being said GH replacement is not an option due to the fact that it could cause tumour reoccurrence.
Antidiuretic Hormone deficiency causing diabetes insipidus
This problem arises from damage to the pituitary stalk or the posterior pituitary gland. Patients with diabetes insipidus have increased thirst and urination. Replacement of antidiuretic hormone resolves these symptoms. Antidiuretic hormone (ADH) is currently replaced by administration of DDAVP (also called Desmopressin).
The hypothalamus plays a huge role in both the endocrine and nervous systems. Craniopharyngioma’s often cause injury to the hypothalamus causing many dysfunctions. The role of the hypothalamus and its functions are as follows:
* Body temperature
* Thirst
* Appetite and weight control (hypothalamic obesity)
* Emotions (limbic system disorders)
* Sleep cycles
* Sex drive
* Childbirth * Blood pressure and heart rate
* Production of digestive juices
* Balancing bodily fluids
Hormones of the hypothalamus
To maintain this balance, the hypothalamus is responsible for creating or controlling many hormones in the body. The hypothalamus is also closely related to the pituitary gland, which makes and sends other important hormones around the body.
Together, the hypothalamus and pituitary gland work to control the entire endocrine system, the glands that produce many hormones of the body. This includes the adrenal glands, kidneys, and thyroid.
Organizer and beneficiary
Gina Vugrin
Beneficiary