- K
- A

"It took 12 Years, 22 Doctors, 4 States, and 2 Countries to get a Lyme Disease diagnosis, finally confirmed by a dentist (!) when live Lyme spirochetes were found in my jawbone. I've lost my career, my home, and my savings. My incredible mother, now in her 90s, has sacrificed everything—including her retirement and life insurance—so I could survive." — Annie.
My name is Kat Paro, and I've battled Lyme disease for 13 years. I vowed that if I recovered, I would help others avoid the horrors of this illness. This led me to volunteer with Global Lyme Alliance (https://www.globallymealliance.org/) and the Center for Lyme Action (https://centerforlymeaction.org/). It was through this work that I became acquainted with Annie and her story.
Annie is very ill. Each day, I worry she may not have made it through the night. We urgently need donations. Please donate if you're able, and like, and share with your networks either way. Every little bit gets Annie closer to getting the help she needs to save her life.
Immediate Goal
***$9,378.88 to start Annie's path to healing
*** Estimates for the full day of testing and initial treatment:
$8,878.88 testing/treatment
$450.00 travel
$50.00 food

Annie during the Center for Lyme Action's virtual Advocacy Day. Photo courtesy Annie G. All rights reserved.
In her own words, Annie shares a glimpse into her incredible journey
“I’ll never forget the blue light. I was in a hospital bed, in my 10th coma, near death from an illness no one could figure out. The phone was held to my ear, and through the haze, I heard a soft, familiar voice with a beautiful accent. It was Mother Teresa of Calcutta. She told me to wake up. I did, to her saying, 'You will not perish from this new epidemic. You will write and speak of your journey. Your story will help save hundreds of thousands of lives achieve remission from this destructive and barely understood epidemic-in-the-making.' ”
“My journey is one of survival, but my purpose is to keep that promise. The disease Mother Teresa spoke of is Lyme disease, and for 35 years, I’ve battled it while trying to fulfill the destiny she laid out for me. Now, I have a path to remission—a new beginning.”
“*My mother wasn’t just a friend to Mother Teresa; she was her personal songwriter. Their bond was a source of light. A constant reminder of faith and purpose. At that moment, Mother Teresa didn’t just save my life; she gave me a reason to fight for it.” — Annie

Annie's Mom, Marlene T. Elias, with Mother Teresa in the 1990s. Photo copyright Marlene T. Elias. Used with permission.
*Local Woman to Sing at Mother Teresa Funeral - The Los Angeles Times, Sept. 10, 1997 https://www.latimes.com/archives/la-xpm-1997-sep-10-me-30765-story.html

"Adventures With Mother Teresa - My Life With A Saint" book jacket. Photo copyright the author, Marlene T. Elias. Used with permission.
Annie is a force of will, powering through her fight with Lyme disease and severe, invisible illnesses brought on by nearly half a lifetime of suffering. Her pain is unbearable, but her courage and spirit are unwavering. For over 35 years, Annie has fought this relentless disease, surviving 12 comas, a catastrophic car accident, and the destruction of her home to Hurricane Ian in 2022.
She has given everything, and her incredible mother has sacrificed her life savings for treatment that insurance won’t cover. Annie believes her purpose was given to her by Mother Teresa: to share her story and help others. But her time is running out. I felt that if I didn’t act, she could lose her fight entirely. — Kat
A Path to Healing
With the generous help of a few kind strangers, we were able to take Annie to an initial consultation at Lifeworks Wellness Center (https://www.lifeworkswellnesscenter.com/), a center specializing in integrative medicine for chronic Lyme disease, where they confirmed that there is a clear path to remission.
But I can’t do it alone. The next steps include a series of crucial diagnostic tests and treatments not covered by insurance.
Your Gift Can Save Annie’s Life!
Every donation gets Annie one step closer to the healing she deserves and the life she’s promised to share with others.
If we are successful in reaching this immediate goal, our next financial goal will be significantly higher, *covering the first 8 weeks of her treatment at Lifeworks:
• $47,129.83 estimate for the first 8 weeks (treatments & supplements)
• $15,000.00 - $20,000.00 estimate for the following 4 weeks.
*These numbers reflect testing and treatment costs only. Housing, food, and transportation costs will be tallied after we hit this goal.
** – If all funds are found (including what’s needed), we would get a $5,924.25 discount! — Kat
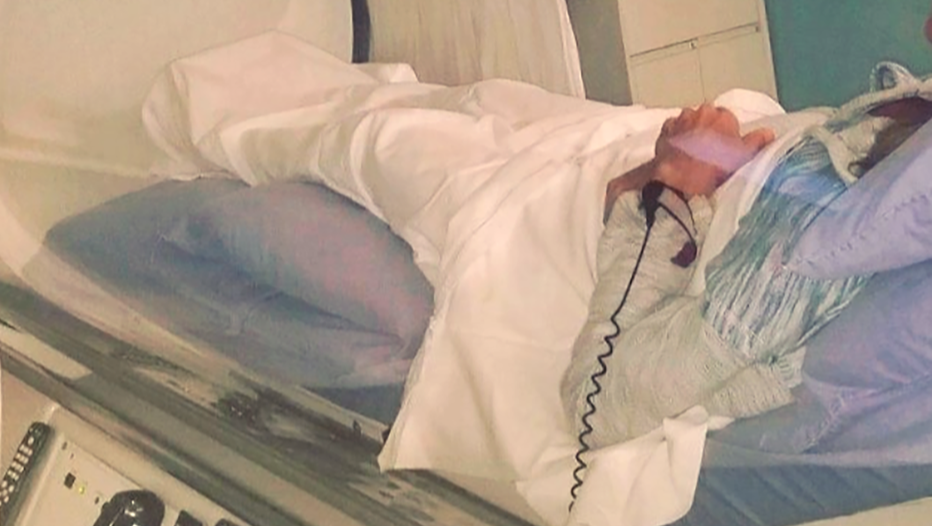
Annie receiving treatment for Lyme disease in a Hyperbaric Oxygen Chamber in the 2000s. She would often work for access to equipment or treatment, bartering for sessions in exchange for representing companies at wellness fairs etc. Photo courtesy Annie G. All rights reserved.
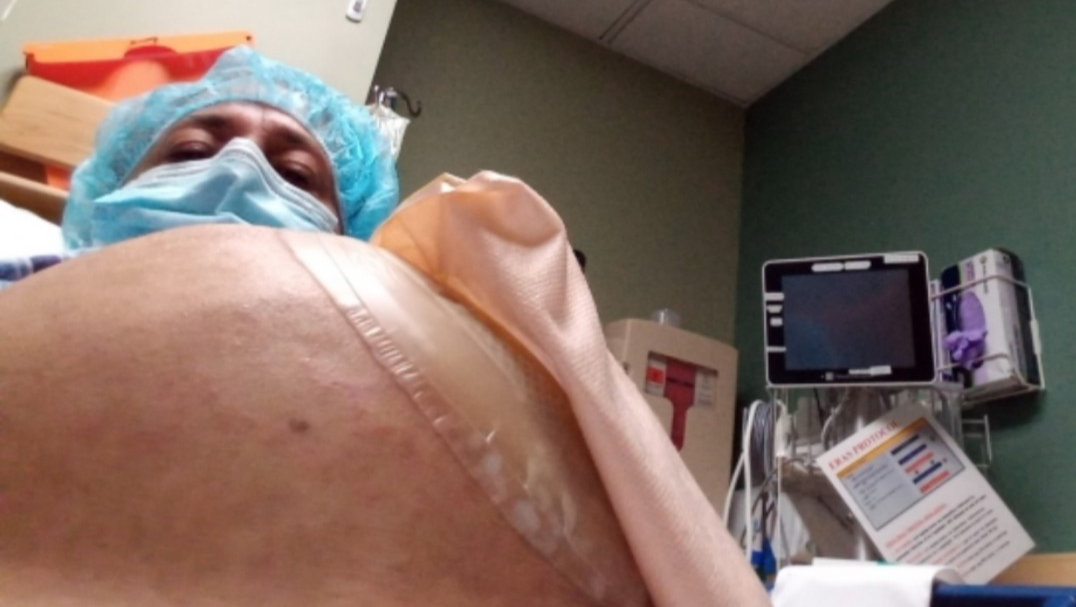
Annie, after a catastrophic hit-and-run accident nearly cut her in half. After 4 months in a coma, she awoke to a colostomy and all female organs removed. Annie was further hurt when airline workers accidentally dumped her out of her wheelchair during transportation, causing the 35-pound tumor seen in this photo. Photo courtesy Annie G. All rights reserved.

Annie's home after Hurricane Ian in the fall of 2022. Photo courtesy Annie G. All rights reserved.
Your donation will directly help get the answers needed to begin these life-saving treatments.
"Every donation gets Annie one step closer to the healing she deserves and the life she’s promised to share with others. Any amount makes a difference! I sincerely appreciate your kindness and generosity." — Kat
“Thank you for giving me a chance to heal. You will forever be in my prayers.” I’d exhausted every resource, but now my hope is stronger than ever. By helping me, you are joining me in keeping the promise made to a modern-day saint. — Annie
To learn more about chronic Lyme disease, coinfections, financial hardship, the work of patient advocates, and other related topics, please visit: LymeDisease.org (https://www.lymedisease.org/).
To understand why fundraisers like these are necessary, please visit: https://www.gofundme.com/c/blog/pay-for-lyme-treatment
And check out our Frequently Asked Questions!
FAQs
What makes tick-borne illness so hard to diagnose?
Diagnosing tick-borne illnesses can be difficult for several reasons, from the nature of the symptoms to the limitations of current diagnostic tests. Here are some of the key challenges:
1. Vague and Overlapping Symptoms
• Flu-like symptoms: Many tick-borne illnesses, like Lyme disease, anaplasmosis, and ehrlichiosis, present with general symptoms such as fever, headache, body aches, and fatigue. These can easily be mistaken for a common cold, flu, or other viral infections, leading to misdiagnosis or a missed diagnosis.
• Lack of a classic rash: While the "bull's-eye" rash (erythema migrans) is a well-known sign of Lyme disease, it doesn't appear in all cases. Many patients don't develop the rash at all, or it may not have the classic appearance.
• Co-infections: A single tick can carry and transmit more than one pathogen, leading to a patient being infected with multiple diseases at once. These "co-infections" can complicate the symptom picture and make it harder to pinpoint the exact illness.
2. Issues with Diagnostic Testing
• Antibody-based tests: The most common diagnostic tests for many tick-borne illnesses are antibody-based, meaning they look for the body's immune response to the infection rather than the pathogen itself. It can take several weeks for the body to produce a detectable level of antibodies, so tests performed too early may come back with a false negative result.
• Inaccurate in early stages: Due to the time it takes for antibodies to develop, these tests are less accurate in the early stages of the illness when treatment is most effective.
• Lack of direct detection: Some pathogens that cause tick-borne illnesses are only present in the bloodstream for a short time or at very low concentrations, making them difficult to detect directly.
• False positives: There can be false positive results due to cross-reactivity with other infections, meaning the test mistakenly flags antibodies that were created to fight a different bacterium.
• Previous vs. current infection: It can be difficult for tests to differentiate between an old, successfully treated infection and a new one, as antibodies can remain in the body for months or even years after the bacteria are gone.
3. Patient and Doctor Factors
• Unnoticed tick bites: Many people who get a tick-borne illness don't recall being bitten by a tick, especially since ticks, particularly nymphs, can be tiny (the size of a poppy seed).
• Delayed symptoms: Symptoms can appear weeks or even months after a tick bite, making it difficult for a person to connect their illness to a past exposure.
• Lack of awareness: Both patients and some healthcare providers may have a low awareness of tick-borne illnesses, leading to a failure to consider a tickborne illness as a potential diagnosis.
• Geographic location: If a person doesn't live in an area where a specific tick-borne illness is common, their doctor may not immediately think to test for it.
What makes tick-borne illness so hard to diagnose?
Diagnosing tick-borne illnesses can be difficult for several reasons, from the nature of the symptoms to the limitations of current diagnostic tests. Here are some of the key challenges:
1. Vague and Overlapping Symptoms
• Flu-like symptoms: Many tick-borne illnesses, like Lyme disease, anaplasmosis, and ehrlichiosis, present with general symptoms such as fever, headache, body aches, and fatigue. These can easily be mistaken for a common cold, flu, or other viral infections, leading to misdiagnosis or a missed diagnosis.
• Lack of a classic rash: While the "bull's-eye" rash (erythema migrans) is a well-known sign of Lyme disease, it doesn't appear in all cases. Many patients don't develop the rash at all, or it may not have the classic appearance.
• Co-infections: A single tick can carry and transmit more than one pathogen, leading to a patient being infected with multiple diseases at once. These "co-infections" can complicate the symptom picture and make it harder to pinpoint the exact illness.
2. Issues with Diagnostic Testing
• Antibody-based tests: The most common diagnostic tests for many tickborne illnesses are antibody-based, meaning they look for the body's immune response to the infection rather than the pathogen itself. It can take several weeks for the body to produce a detectable level of antibodies, so tests performed too early may come back with a false negative result.
• Inaccurate in early stages: Due to the time it takes for antibodies to develop, these tests are less accurate in the early stages of the illness when treatment is most effective.
• Lack of direct detection: Some pathogens that cause tickborne illnesses are only present in the bloodstream for a short time or at very low concentrations, making them difficult to detect directly.
• False positives: There can be false positive results due to cross-reactivity with other infections, meaning the test mistakenly flags antibodies that were created to fight a different bacterium.
• Previous vs. current infection: It can be difficult for tests to differentiate between an old, successfully treated infection and a new one, as antibodies can remain in the body for months or even years after the bacteria are gone.
3. Patient and Doctor Factors
• Unnoticed tick bites: Many people who get a tickborne illness don't recall being bitten by a tick, especially since ticks, particularly nymphs, can be very small (the size of a poppy seed).
• Delayed symptoms: Symptoms can appear weeks or even months after a tick bite, making it difficult for a person to connect their illness to a past exposure.
• Lack of awareness: Both patients and some healthcare providers may have a low awareness of tickborne illnesses, leading to a failure to consider a tickborne illness as a potential diagnosis.
• Geographic location: If a person doesn't live in an area where a specific tick-borne illness is common, their doctor may not immediately think to test for it.
How does having an invisible illness hamper access to care or concern from the general public?
Having an invisible illness, like a tick-borne disease such as chronic Lyme disease, significantly complicates a person's life by creating major barriers to both healthcare and public understanding. The core of the problem is the disconnect between a person's internal experience and their external appearance.
Access to Care
• Medical Gaslighting and Dismissal: Because a patient with an invisible illness "looks fine," doctors may dismiss their symptoms, attribute them to psychological issues ("it's all in your head"), or simply not take them seriously. This can lead to delays in diagnosis, misdiagnosis, and a feeling of being unheard and invalidated.
• Diagnostic Challenges: As mentioned in the previous answer, the lack of definitive, visible markers makes it difficult to diagnose these conditions. Doctors often rely on what they can see or measure, and when tests come back "normal," they may conclude there is no illness.
• Financial Burden: The journey to a diagnosis can be long and expensive, involving multiple doctor's visits, specialists, and tests, many of which may not be covered by insurance because they are considered experimental or "not medically necessary" for a patient who looks healthy.
• Fragmented Care: Patients with invisible illnesses often have a complex web of symptoms affecting different body systems, requiring them to see multiple specialists (e.g., a neurologist for cognitive issues, a rheumatologist for joint pain, and a cardiologist for heart problems). This creates a fragmented and uncoordinated healthcare experience.
Concern from the General Public
• Disbelief and Judgment: The most common and painful experience for people with invisible illnesses is being told, "But you don't look sick." This can lead to accusations of faking it, laziness, or exaggerating symptoms. This judgment can come from friends, family, employers, and even strangers.
• Social Isolation: Due to the fluctuating nature of many invisible illnesses, a person may be well enough to attend a social event one day but be too exhausted or in pain to attend the next. This can be misunderstood as unreliability or lack of interest, leading to a breakdown in relationships and social isolation.
• Workplace Discrimination: Employers may not believe a person needs accommodations if they don't have a visible disability. A person might be denied time off, a flexible schedule, or other necessary adjustments, leading to job loss or the inability to work at all.
• Stigma and Shame: The constant need to "prove" one's illness can lead to feelings of shame, anxiety, and depression. People with invisible illnesses often feel they have to choose between disclosing their condition and facing skepticism or staying silent and suffering alone.
In essence, having an invisible illness means not only living with the burden of a debilitating condition but also constantly battling societal misconceptions and a healthcare system that is not designed to handle what it cannot easily see. This double burden can have a significant impact on a person's mental, emotional, and financial well-being.
What are some illnesses that people with tick-borne illnesses are commonly misdiagnosed with?
Autoimmune and Rheumatic Conditions
• Fibromyalgia: The widespread muscle pain, fatigue, and "brain fog" of Lyme disease can be almost identical to the symptoms of fibromyalgia.
• Chronic Fatigue Syndrome (ME/CFS): A key symptom of tickborne illnesses is severe, debilitating fatigue, which is the hallmark of Chronic Fatigue Syndrome.
• Multiple Sclerosis (MS): Neurological symptoms of Lyme disease, such as nerve pain, numbness, tingling, vision problems, and cognitive difficulties, can be easily mistaken for MS.
• Rheumatoid Arthritis and Juvenile Arthritis: Joint pain and swelling are common symptoms of tickborne illnesses, leading to misdiagnoses of various forms of arthritis.
• Lupus: The general body aches, fever, and fatigue can overlap with the symptoms of lupus.
Neurological and Psychiatric Conditions
• Alzheimer's Disease and Dementia: In later stages, tickborne illnesses can cause cognitive decline, memory loss, and confusion, leading to a misdiagnosis of early-onset dementia or Alzheimer's.
• Parkinson's Disease: Tremors and other motor symptoms can be misidentified as Parkinson's.
• Psychiatric disorders: Symptoms such as depression, anxiety, panic attacks, and mood swings can be attributed to a mental health issue rather than a physical infection.
Other Conditions
• Viral Infections ("The Summer Flu"): In the early stages, the fever, headache, and body aches of a tickborne illness are often mistaken for the flu or another common viral infection.
• Mononucleosis (Mono): The persistent fatigue, fever, and swollen lymph nodes can mimic mono.
• Colitis and Irritable Bowel Syndrome (IBS): Some tickborne illnesses can cause digestive issues, leading to misdiagnoses of gastrointestinal disorders.
• Bell's Palsy: Facial paralysis is a classic symptom of Lyme disease, but is often initially misdiagnosed as Bell's Palsy.
The problem is compounded by the fact that diagnostic tests for tick-borne diseases are often unreliable in the early stages of the illness and can be complex to interpret. This means that a person may receive a negative test result, leading a doctor to look for other explanations for their symptoms and land on one of these other diagnoses.
What are common coinfections that a tick can give?
Ticks, especially the black-legged tick (or deer tick), are known to carry multiple pathogens, and a single bite can transmit more than one disease. When a person is infected with multiple pathogens from a tick bite, it is known as a co-infection. These co-infections can complicate diagnosis and treatment, often leading to more severe and persistent symptoms. Here are some of the common co-infections associated with tick bites:
• Babesiosis: Caused by a parasite (Babesia microti) that infects red blood cells, this is a malaria-like illness. Symptoms often include fever, chills, fatigue, and hemolytic anemia (the destruction of red blood cells). It can be particularly severe in individuals with weakened immune systems or those who have had their spleen removed.
• Anaplasmosis: A bacterial infection (Anaplasmaphagocytophilum) that invades white blood cells. Symptoms are similar to other tickborne illnesses, including fever, headache, muscle aches, and chills. It was previously known as human granulocytic ehrlichiosis (HGE).
• Ehrlichiosis: Another bacterial infection caused by various species of the Ehrlichia bacteria, such as Ehrlichia chaffeensis. Like anaplasmosis, it affects white blood cells and presents with flu-like symptoms, including fever, headache, and muscle aches. A rash can sometimes occur, but it is not common.
• Bartonellosis: While it is often associated with cat scratches, some species of the Bartonella bacteria are also transmitted by ticks. Symptoms can be wide-ranging, including fever, enlarged lymph nodes, neurological symptoms, and a distinctive rash that looks like streaks.
• Borrelia miyamotoi Disease: This is a type of tick-borne relapsing fever. Caused by the bacterium (Borrelia Miyamotoi), this disease is transmitted by the same ticks that carry Lyme disease. The key symptom is recurring bouts of fever, often alternating with periods of no fever.
• Powassan Virus Disease: This is a much rarer but more severe illness caused by the Powassan virus. A tick can transmit it in as little as 15 minutes. While many people have no symptoms, it can cause severe neuroinvasive disease, including encephalitis (inflammation of the brain) or meningitis (inflammation of the membranes around the brain and spinal cord). There is no specific treatment for the Powassan virus, so care is supportive.
What's the latest discovery of a symptom brought on by a tick-borne illness patient and red meat?
The most significant discovery regarding a symptom linked to a tick-borne illness and red meat is Alpha-gal syndrome (AGS). While not a new discovery in itself (the link was first identified in 2009), there have been several recent developments that have brought it to the forefront of public health awareness.
What is Alpha-gal Syndrome?
Alpha-gal syndrome is a type of delayed allergic reaction to a sugar molecule called alpha-gal. This molecule is found in the meat of most mammals (like beef, pork, and lamb) and in products made from mammals (like gelatin, dairy, and some medications).
The syndrome is triggered by the bite of certain ticks. The most well-known culprit in the United States is the Lone Star tick. When a lone star tick bites a human, it can transmit the alpha-gal sugar, a sugar found in the tissues of all mammals except humans and other primates, from its saliva into the person's bloodstream. The person's immune system, which doesn't have this molecule, recognizes it as a foreign substance and creates antibodies to fight it.
The unique and challenging aspect of AGS is that the allergic reaction is delayed, often occurring 2 to 6 hours or more after a person eats red meat. This delay makes it very difficult for patients and doctors to connect the symptoms to a specific food.
Recent Discoveries and Developments
• Spread of the Condition: Recent research has shown a significant increase in the number of cases and a geographic expansion of the ticks that cause it. The lone star tick, once primarily a resident of the southeastern U.S., is moving northward due to climate change. There have also been confirmed cases linked to other tick species, including the black-legged tick (deer tick), which is the primary vector for Lyme disease. This expands the potential risk to new populations in different regions.
• The Scale of the Problem: The CDC recently reported that there were over 110,000 suspected cases between 2010 and 2022, but they estimate the actual number of people affected could be as high as 450,000, suggesting many cases go undiagnosed due to the delayed and often non-specific nature of the symptoms.
• A Broader Range of Symptoms: While the classic symptoms are hives and anaphylaxis, recent findings suggest that some people with AGS may only experience gastrointestinal issues, such as severe stomach pain, nausea, and diarrhea. This makes diagnosis even more challenging, as these symptoms can be mistaken for Irritable Bowel Syndrome (IBS) or other digestive disorders.
• New Research on Treatment: Researchers are working on new treatments for AGS, including a promising nanoparticle-based approach that was shown to prevent allergic reactions to red meat in mice. This could be a significant step toward developing a treatment that goes beyond simply avoiding red meat.
Why are women more likely to have lingering issues or chronic Lyme with tick-borne diseases?
The relationship between sex and chronic tick-borne illness is complex and an area of ongoing research. While the overall incidence of tick-borne illness might be similar between men and women, studies show that women are more likely to be diagnosed with and suffer from chronic, persistent symptoms. This disparity is likely due to a combination of biological, social, and psychological factors.
1. The Role of Hormones and the Immune System
• A More Robust Immune Response: Women, especially during their reproductive years, generally have a more robust and aggressive immune response than men. This can be a double-edged sword. While it might help fight off an initial infection more effectively, it can also lead to an over-exuberant inflammatory response. In some cases, this heightened inflammation may not resolve after the infection is cleared, leading to lingering symptoms.
• Hormonal Fluctuations: Hormonal cycles throughout a woman's life—from menstruation to pregnancy to perimenopause and menopause—can significantly impact the immune system and the severity of symptoms. Many women with chronic tick-borne illness report that their symptoms worsen during their menstrual cycle, a time when certain inflammatory markers increase.
• Estrogen's Influence: Estrogen, a key female hormone, is known to have both pro- and anti-inflammatory properties depending on its levels. A decline in estrogen, such as during menopause, can weaken the immune system's ability to regulate inflammation, potentially contributing to the persistence of symptoms.
2. Disparities in Healthcare
• Misdiagnosis and Diagnostic Delays: Women are often told their symptoms are psychosomatic, stress-related, or "all in their head." Because many of the symptoms of tickborne illnesses—like fatigue, body aches, brain fog, and mood swings—overlap with common, often dismissed, women's health issues or other conditions like fibromyalgia and chronic fatigue syndrome (which are also more common in women), it can take a long time to get a correct diagnosis. This delay in diagnosis can allow the infection to become more entrenched, making it harder to treat effectively.
• Lack of Gender-Specific Research: Historically, much medical research has not disaggregated data by sex, or has used male subjects as the standard, leading to a lack of understanding of how diseases, including tickborne illnesses, present and progress differently in women.
3. Overlap with Other "Female-Prevalent" Illnesses
• Chronic Fatigue Syndrome and Fibromyalgia: The symptoms of chronic Lyme disease can closely mirror those of Chronic Fatigue Syndrome and Fibromyalgia, both of which predominantly affect women. This clinical overlap can lead to a misdiagnosis, where the underlying infection is missed entirely. A person may be treated for the symptoms of these other conditions without ever addressing the root cause, leading to a lack of improvement and the continuation of the illness.
In summary, the reasons for women having a higher prevalence of chronic tickborne illness are complex. It's not just a single factor but a confluence of biological differences in immune and hormonal systems, combined with systemic issues in healthcare, that can lead to diagnostic delays and a lack of proper treatment.
How does being bitten by ticks change a person's life if not treated properly?
When a tick bite goes unnoticed or a tick-borne illness is not treated promptly and correctly, the consequences can be severe and life-altering. The initial, often flu-like symptoms can progress into a chronic, multi-systemic disease that can profoundly impact a person's physical and mental health, career, and social life.
Here's how an untreated tick-borne illness can change a person's life:
1. Chronic Pain and Physical Disability
• Lyme Arthritis: Untreated Lyme disease can lead to chronic, debilitating arthritis. This most commonly affects large joints, especially the knees, causing severe pain, swelling, and a limited range of motion. The pain can be constant or come and go, making everyday activities, from walking to simply getting out of bed, a challenge.
• Musculoskeletal Pain: Widespread muscle aches and joint pain, often described as similar to fibromyalgia, can become a persistent part of daily life. This can make it difficult to exercise, work, or even sleep comfortably.
2. Neurological and Cognitive Impairment
• Lyme Neuroborreliosis: The bacteria can invade the central and peripheral nervous systems. This can cause a range of neurological issues, including:
• Neuropathy: Numbness, tingling, or shooting pains in the hands and feet.
• Cognitive Dysfunction: Severe "brain fog" that affects memory, concentration, and the ability to think clearly. This can make it impossible to perform well at school or work, leading to career setbacks.
• Facial Palsy (Bell's Palsy): A drooping or paralysis of one side of the face.
• Meningitis or Encephalitis: In more severe cases, inflammation of the brain or spinal cord can occur.
• Psychiatric Issues: The chronic stress of the illness, combined with the inflammatory effects of the infection on the brain, can lead to significant mental health problems, including anxiety, depression, panic attacks, and mood swings. Studies have shown a link between untreated Lyme disease and an increased risk of suicide.
3. Cardiac Complications
• Lyme Carditis: In a small percentage of cases, the infection can affect the heart's electrical system, leading to heart block. This can cause dizziness, fainting, shortness of breath, and an irregular heartbeat. In some rare and extreme cases, it can be fatal. While this is one of the more acute and dangerous complications, it can become a chronic issue for some.
4. Co-Infections and Compound Issues
• More Severe Symptoms: If a tick transmitted a co-infection like Babesiosis or Anaplasmosis along with Lyme, the symptoms can be more severe. For example, Babesiosis can cause a severe, malaria-like illness with high fevers and anemia. Anaplasmosis can lead to respiratory failure, internal bleeding, and organ damage if not treated.
• Long-Term Sequelae: The lingering effects of co-infections can add to the burden of the illness. For example, some people with untreated Babesiosis can have a persistent, low-level infection that causes ongoing fatigue and other symptoms.
5. Social and Financial Consequences
• Loss of Career and Income: The physical pain, chronic fatigue, and cognitive dysfunction can make it impossible to maintain a full-time job. Many people with chronic tick-borne illness lose their careers and have to go on disability, leading to severe financial strain.
• Social Isolation: The "invisible" nature of the illness and the fluctuating, unpredictable symptoms can strain relationships with friends and family. People may be accused of being lazy or making up their illness, leading to social isolation and a lack of a support system.
• A Life of Uncertainty: A person's life becomes dominated by managing their symptoms and navigating a complex and often unsupportive healthcare system. The future is uncertain, as a person doesn't know if or when they will get better.
In essence, an untreated tick-borne illness doesn't just go away. It can evolve into a chronic condition that attacks multiple systems of the body, fundamentally changing a person's quality of life and leaving them in a constant state of pain and uncertainty.
Why doesn't health insurance cover Lyme Disease treatment beyond a few weeks of antibiotics?
The reason health insurance companies often do not cover long-term antibiotic treatment for Lyme disease is rooted in a fundamental medical and political controversy. The core of the issue lies in the lack of consensus on what constitutes an appropriate treatment for persistent symptoms after an initial course of antibiotics.
The Conflict Between Medical Societies
There are two main opposing viewpoints, which guide the decisions of both doctors and insurance companies:
1. The Infectious Diseases Society of America (IDSA) Guidelines: The IDSA is the leading authority on infectious diseases, and its guidelines are widely adopted by insurance companies and the Centers for Disease Control and Prevention (CDC). The IDSA's position is that a short course of oral antibiotics (10-14 days) is sufficient for early Lyme disease, with slightly longer courses (up to 28 days) for later-stage conditions.
According to the IDSA, any symptoms that persist after this treatment are not due to an active, ongoing infection. They refer to this condition as Post-Treatment Lyme Disease Syndrome (PTLDS), which they view as a result of lingering tissue damage or an autoimmune response, not a persistent bacterial presence. Therefore, they do not recommend or recognize the need for long-term antibiotic therapy.
Insurance companies rely on these guidelines to justify denying coverage for continued antibiotic treatment, deeming it "medically unnecessary" or "experimental."
2. The International Lyme and Associated Diseases Society (ILADS) Guidelines: ILADS, an organization of physicians and researchers, holds a different view. Their guidelines are based on the belief that a short course of antibiotics may not be sufficient to eradicate the Borrelia burgdorferi bacteria, particularly in cases of late or chronic Lyme disease.
They believe the bacteria can persist in the body in various forms (e.g., biofilms) and that chronic symptoms are a result of this ongoing, active infection.
As a result, ILADS recommends longer courses of antibiotics, sometimes for months or even years, based on a doctor's clinical judgment.
Why Insurance Companies Side with the IDSA
• Reliance on Established Guidelines: Insurance companies are in the business of managing risk and costs. They rely on "generally accepted principles of professional medical practice" to determine what is "medically necessary." The IDSA guidelines, endorsed by the CDC, are the most widely accepted and established set of principles for this purpose.
• Cost-Benefit Analysis: Long-term antibiotic treatment, especially with intravenous (IV) antibiotics, is expensive. By adhering to the IDSA's short-term treatment model, insurance companies can limit their financial liability.
The Impact on Patients and Progress
This clash of guidelines creates a tremendous burden for patients. They are often forced to pay for their long-term treatment entirely out of pocket, which can cost tens of thousands of dollars and lead to financial ruin. This has also spurred legal and legislative battles in several states, with some, like Massachusetts and Connecticut, enacting laws to mandate insurance coverage for long-term Lyme disease treatment.
Have there been attempts by the US government to financially help patients with long-term Lyme Disease issues?
Direct financial assistance from the U.S. government specifically for long-term Lyme disease treatment is very limited. The government's approach has been more focused on research and, to a lesser extent, supporting disability claims rather than directly paying for treatments not covered by insurance.
Here's a breakdown of the government's role and the available resources:
1. Research and a Push for Better Diagnostics
The U.S. government, through agencies like the National Institutes of Health (NIH) and the Department of Defense (DoD), has significantly increased funding for research into tickborne diseases. This is a key area where the government is attempting to address the issue. The goal of this funding is to:
• Develop better diagnostic tests: Researchers are working on new tests that can more accurately detect active infections, which could, in turn, help legitimize the need for long-term treatment in the eyes of insurance companies.
• Understand the mechanisms of persistent symptoms: Funding is being directed toward understanding why some people develop chronic symptoms after a short course of antibiotics. This research is crucial for developing new and effective treatments.
• Identify novel therapies: The government is supporting research into new therapeutics to treat both the acute and chronic forms of these illnesses.
2. Social Security Disability
For patients whose illness is so debilitating that it prevents them from working, Social Security Disability (SSDI) or Supplemental Security Income (SSI) can be a source of financial relief. However, obtaining these benefits for chronic Lyme disease is often a difficult and lengthy process.
• Proving the Disability: Applicants must provide extensive medical documentation to prove that their symptoms prevent them from engaging in "substantial gainful activity." Because chronic Lyme disease is not uniformly recognized by the medical community, and because many of the symptoms are subjective, these claims can be challenging to prove and are often initially denied.
• Legal Help is Often Required: Many patients must hire a lawyer to navigate the complex application and appeals process for disability benefits.
3. Patient Advocacy and Non-Profit Organizations
The primary source of financial assistance for patients is not the government, but a network of non-profit organizations. These organizations work to fill the gap left by insurance companies and a lack of direct government aid. Some of these include:
• LymeLight Foundation: Provides grants to children and young adults with Lyme disease.
• Lyme Treatment Foundation: Offers grants to patients of all ages to assist with the cost of treatment and diagnostic testing.
• Lyme Test Access Program (Lyme-TAP): A program that helps patients with financial need access initial Lyme-related lab tests.
• LivLyme Foundation: Provides grants to children to assist with medication and treatment costs.
• Generation Lyme: A patient-led organization that provides resources and a support network.
These organizations raise funds through donations, and their grants are often limited in amount and are highly sought after.
In summary, while the U.S. government has invested in research to better understand and treat tick-borne diseases, there is no large-scale, direct government program to provide financial relief to patients for long-term treatment.
The burden of payment largely falls on the patients themselves, who must navigate a system of private non-profits and a difficult disability application process to get the help they need.
Why is getting an accurate diagnosis so difficult?
Getting an accurate diagnosis for tick-borne illnesses is notoriously difficult due to a combination of clinical, laboratory, and systemic factors. Here are the primary reasons:
1. Non-Specific Symptoms
• The "Great Imitator": Many tick-borne illnesses, especially in their early stages, present with flu-like symptoms such as fever, headache, body aches, and fatigue. These symptoms are common to dozens of other illnesses, from the common cold to chronic conditions, making them easy to dismiss or misdiagnose.
• Lack of a Distinctive Rash: While the "bull's-eye" rash (erythema migrans) is a classic sign of Lyme disease, it doesn't appear in every case, and in many instances, it may not have the typical appearance. Many people don't develop any rash at all. Without this key visual clue, diagnosis is much harder.
• Fluctuating and Progressive Symptoms: Symptoms can come and go, making it seem like the patient is improving on their own. However, the illness may be progressing, and when symptoms return, they may be different, more severe, and affect other body systems, further confusing the clinical picture.
2. Unreliable Diagnostic Tests
• Antibody-Based Testing: The most common diagnostic tests for many tickborne illnesses are antibody-based. They don't look for the bacteria itself; they look for the body's immune response to the bacteria.
• Delayed Response: It takes time for the body to produce a detectable level of antibodies. If a test is performed too early (within the first few weeks of infection), it can result in a false negative, even if the person is infected.
• Long-Lasting Antibodies: Conversely, a person who had a tick-borne illness in the past, was successfully treated, and is now dealing with new symptoms, may still test positive for antibodies, making it difficult to distinguish between a past and a new infection.
• Limitations of the Two-Tiered System: The CDC-recommended two-tiered testing system for Lyme disease has limitations. It can miss a significant number of cases, especially in the early stages, because it requires a positive or equivocal result on the first test (ELISA) to proceed to the second (Western blot).
• Co-infections: A single tick bite can transmit multiple pathogens. Standard tests may only screen for one or two of the most common illnesses, meaning a co-infection can be missed, even if the primary illness is identified. The symptoms of co-infections can also be more severe and harder to interpret.
3. Patient and Doctor Factors
• Unnoticed Tick Bite: Many people who get a tick-borne illness don't recall being bitten by a tick. Nymph ticks, which are the size of a poppy seed, are often the ones that transmit the infection and are easily missed. Without the knowledge of a bite, the patient may not even consider a tick-borne illness as the cause of their symptoms.
• Geographic and Climatic Changes: Ticks are expanding into new regions due to climate change, bringing tick-borne diseases to areas where doctors may not be familiar with their signs and symptoms.
• Lack of Physician Awareness: Not all healthcare providers are well-versed in diagnosing and treating tick-borne illnesses. Some may not consider the possibility, especially if the patient doesn't have a clear "bull's-eye" rash or a remembered tick bite. They may instead attribute the patient's symptoms to other, more common conditions, such as fibromyalgia, chronic fatigue syndrome, or even psychological issues.
• Subjective Symptoms: Many of the most debilitating symptoms, such as fatigue, pain, and "brain fog," are subjective. Without objective, visible signs, it can be easy for a doctor to dismiss the patient's complaints or suggest they are psychosomatic.
What is the status of research and development of vaccines, better testing for the pathogens, and better public education?
Research and development in the field of tick-borne illnesses have been accelerating, but progress is often slow and complex. Here is an overview of the current status of vaccines, diagnostics, and public education.
Vaccines
• Lyme Disease: The only U.S. Lyme disease vaccine, LYMERix, was discontinued by its manufacturer in 2002, citing insufficient consumer demand driven by public concerns about its safety. However, new vaccine development has been a major focus of research. The most promising candidate, VLA15, developed by Pfizer and Valneva, is a multivalent, protein subunit vaccine that targets a protein on the surface of the bacteria. It is currently in Phase 3 clinical trials, a major step toward potential public availability.
• Other Tick-borne Diseases: There are no vaccines available in the U.S. for other common tick-borne diseases like anaplasmosis, babesiosis, or ehrlichiosis. There is a vaccine available for Tick-borne Encephalitis (TBE) in the U.S. (TICOVAC), but TBE is primarily a concern for travelers to Europe and Asia and is not endemic in North America.
Better Testing for Pathogens
• The Problem with Current Tests: The current two-tiered system for Lyme disease testing, which looks for antibodies, has limitations. It often produces false negatives in the early stages of the disease before the immune system has had time to mount a response.
• Advanced Molecular and Serological Testing: There is significant research and development to improve diagnostic tools. This includes:
• Multiplex PCR and Protein Microarrays: These new technologies are designed to detect multiple pathogens or antibody responses in a single blood sample, which is critical for identifying co-infections.
• Biomarker Discovery: Researchers are actively searching for new biomarkers in the blood that could indicate an active infection or a risk for developing chronic symptoms. This would help clinicians provide more accurate diagnoses and measure the effectiveness of treatment.
• Direct Detection of Pathogens: Scientists are working on developing tests that can directly detect the pathogen, even when it's present in low concentrations, which would overcome the limitations of antibody-based tests.
Better Public Education
• Targeted Campaigns: Public health organizations, including the CDC and various state-level departments of health, have launched public education campaigns. These campaigns often focus on promoting preventative behaviors such as using tick repellent, performing tick checks, and creating "tick-safe" yards.
• Effectiveness and Challenges: Research has shown that these campaigns can be effective in increasing public awareness and leading to a modest increase in preventative behaviors. However, a significant portion of the population still does not consistently follow these recommendations.
Challenges to effective public education include:
• Lack of Public Urgency: Many people underestimate the risk of tick-borne illnesses, especially in areas where they are not yet widespread.
• Misinformation and Pseudoscience: The contentious nature of chronic Lyme disease has led to a proliferation of misinformation that can undermine credible public health messaging.
• Reaching High-Risk Groups: It can be difficult to reach and influence the behavior of key high-risk groups, such as children and outdoor enthusiasts.
In conclusion, while progress is being made in all three areas—vaccine development, diagnostic testing, and public education—significant challenges remain. The research is slow, and funding is often limited, but there is hope that new advancements will eventually lead to more effective prevention, diagnosis, and treatment for tickborne illnesses.
Are people in degree programs to practice as infectious disease specialists taught much about Lyme Disease and other tick-borne illnesses?
Yes, infectious disease (ID) specialists are taught about Lyme disease and other tickborne illnesses. These diseases are a core part of the curriculum for infectious disease training. However, the depth and perspective of this training are an important part of the ongoing debate about chronic Lyme disease.
Here's a breakdown of how and what they are taught:
1. In Medical School
• General Introduction: All medical students are exposed to tick-borne illnesses in their microbiology, infectious disease, and internal medicine coursework. They learn the basic epidemiology, clinical presentation, and standard treatment protocols for diseases like Lyme, anaplasmosis, and babesiosis. The focus is on the classic presentations and the CDC and Infectious Diseases Society of America (IDSA) guidelines.
2. In Infectious Disease Fellowships
• In-Depth Training: The most comprehensive training on tick-borne diseases occurs during a physician's ID fellowship. This is a specialized, post-residency training program. Here, fellows learn in-depth about the diagnosis and management of a wide range of infectious diseases, including those transmitted by ticks.
• IDSA-Driven Curriculum: The curriculum for most ID fellowship programs in the U.S. is heavily influenced by the IDSA. As a result, the training emphasizes the IDSA's evidence-based guidelines, which:
• Focus on Acute Treatment: Recommend short courses of antibiotics (typically 2-4 weeks) for acute infections.
• Define PTLDS: Acknowledge that a small percentage of patients experience persistent symptoms after treatment, but classify this condition as Post-Treatment Lyme Disease Syndrome (PTLDS), which they do not attribute to an active, ongoing infection.
• Do Not Recommend Long-Term Antibiotics: Discourage and do not recommend long-term antibiotic therapy for PTLDS, citing a lack of evidence for its effectiveness and potential for harm.
• Exposure to a Wide Range of Illnesses: ID fellows are trained to differentiate tick-borne illnesses from other conditions, as well as to recognize co-infections. They learn about less common but more severe illnesses like the Powassan virus and Rocky Mountain Spotted Fever.
3. Key Points of Contention in Training
• The "Chronic Lyme" Debate: The primary point of friction is the existence of "chronic Lyme disease." While many patients and some clinicians believe that persistent symptoms are due to an ongoing, active infection that requires long-term treatment, this viewpoint is generally not supported by the IDSA and is therefore not part of the standard curriculum. ID specialists are trained to look for other causes of a patient's lingering symptoms and do not typically prescribe long-term antibiotics.
• Limited Training on Controversial Treatments: Many of the alternative or long-term treatments sought by patients are not taught or endorsed in mainstream medical education. This knowledge gap can lead to a disconnect and a lack of understanding between the patient's experience and the doctor's training.
While many programs, especially in highly endemic areas, may have dedicated clinics or research on tick-borne diseases, the standard ID training in the U.S. is based on the IDSA guidelines. This is a major reason why patients with long-term symptoms often feel misunderstood or dismissed by infectious disease specialists who are following the established protocols they were taught.
Are physicians in training taught about the complexities of Lyme disease and how to correctly diagnose it?
Yes, physicians in training are taught about Lyme disease and other tick-borne illnesses. However, the depth and perspective of this training, particularly regarding the complexities of diagnosis and treatment, can be a major source of the controversy surrounding chronic Lyme disease.
The Standard Medical Curriculum
In medical school and residency, doctors are taught to diagnose Lyme disease based on a combination of a clinical presentation and a laboratory test.
• Clinical Picture: The curriculum emphasizes the most recognizable sign of early Lyme disease: the "bull's-eye" rash (erythema migrans). Physicians are taught to recognize this rash and that, in its presence, a blood test is not necessary for diagnosis or treatment.
• Two-Tiered Testing: In cases where the rash is absent or a patient has later-stage symptoms, physicians are trained to follow the CDC's recommended two-tiered testing system. This involves an initial ELISA test, followed by a Western blot if the first test is positive or inconclusive. This is the standard of care taught in most medical schools and residency programs.
The Complexities and Gaps in Training
Despite this training, there are significant complexities that can lead to misdiagnosis and frustration for patients
• Symptom Overlap: Medical students are taught that Lyme symptoms often mimic other conditions, such as fibromyalgia, chronic fatigue syndrome, and multiple sclerosis. This makes it easy for a doctor to land on a different diagnosis, especially if they are not in a highly endemic area or if a patient doesn't recall a tick bite.
• Test Limitations: The training highlights that the standard tests for Lyme disease are antibody-based, not direct pathogen tests. This means they are unreliable in the early stages of the disease when a patient's body hasn't had time to mount an immune response. This leads to false negatives that can be a major barrier to a correct diagnosis.
• The Chronic Lyme Controversy: The most significant gap in standard medical training is the approach to patients with persistent symptoms after treatment. The mainstream medical community, guided by the Infectious Diseases Society of America (IDSA), teaches that these symptoms are not due to an ongoing, active infection. The condition is called Post-Treatment Lyme Disease Syndrome (PTLDS), and it is not treated with long-term antibiotics. This perspective is a core part of the curriculum for most physicians in training. The alternative view—that persistent symptoms are a result of an ongoing, active infection requiring long-term treatment—is not taught in mainstream medical education.
Do medical doctors face pressure concerning how to treat someone with a positive Lyme test due to political aspects or persecution by their state or medical board?
Yes, doctors can face significant pressure regarding how they treat patients with a positive Lyme test, particularly for long-term or chronic cases. This pressure stems from the ongoing medical and political controversy surrounding Lyme disease, which can lead to scrutiny from state medical boards and professional organizations.
The Conflict of Guidelines
• IDSA Guidelines: The Infectious Diseases Society of America (IDSA) is the mainstream authority. Its guidelines, endorsed by the Centers for Disease Control and Prevention (CDC), state that a short course of antibiotics (typically 2-4 weeks) is sufficient to cure Lyme disease. They classify persistent symptoms as Post-Treatment Lyme Disease Syndrome (PTLDS), which they believe is not caused by an active infection and therefore does not require long-term antibiotics. Most state medical boards and insurance companies adhere to these guidelines.
• ILADS Guidelines: The International Lyme and Associated Diseases Society (ILADS) represents a group of physicians who believe that Lyme disease can be a persistent infection requiring long-term antibiotic treatment. They advocate for a more individualized approach to care.
Persecution and Loss of License
Physicians who choose to follow the ILADS guidelines or treat patients with long-term antibiotics can face persecution from their state medical boards. This is because their treatment protocols are considered "unconventional," "experimental," or "outside the standard of care" by the mainstream medical community. The consequences can be severe:
• Investigations: Doctors may be subjected to investigations by their state's medical board based on complaints from other physicians, patients, or insurance companies.
• Disciplinary Action: These investigations can lead to disciplinary actions, including official reprimands, fines, mandated supervision, and in some cases, the suspension or revocation of their medical license.
• Professional Isolation: Doctors who treat chronic Lyme disease may be ostracized by their peers, face difficulty getting referrals, and have their practice scrutinized.
This pressure creates an ethical and professional dilemma for doctors, especially in states without specific legal protections for them. They must choose between adhering to the dominant, insurance-friendly guidelines or providing a form of treatment they believe is in the best interest of their patient, knowing it could put their career at risk.
Is there a list of doctors' names who have treated Lyme patients outside of the CDC's guidelines, who had their licenses suspended but whose patients have gotten better from that treatment?
Due to privacy concerns and the legal and professional implications involved, there is no public, official list of doctors who have had their licenses suspended for treating Lyme patients outside of CDC guidelines, whose patients have gotten better from that treatment. However, there are well-known cases of doctors who have faced disciplinary action from medical boards, and in response, their patients have publicly defended them and shared stories of recovery.
Notable Cases
• Dr. Joseph Jemsek: A prominent case involves Dr. Joseph Jemsek, an infectious disease specialist in North Carolina. His medical license was suspended after the state medical board found his long-term antibiotic treatment for chronic Lyme disease to be outside the standard of care. Despite this, he has a significant following of patients who claim he helped them recover after years of suffering. A few years ago, the North Carolina Medical Board reinstated Dr Jemsek’s license. (https://www.lymedisease.org/nc-medical-board-lifts-restrictions-on-prominent-lyme-treating-physician/)
• Dr. Charles Ray Jones: A pediatrician from Connecticut, Dr. Jones was a polarizing figure known for treating thousands of children for Lyme disease. He faced disciplinary action from the Connecticut Medical Examining Board, including a fine and probation, for his treatment protocols. His patients and their families have been vocal advocates, claiming he was the only doctor who could correctly diagnose and treat their children, leading to their recovery. (https://www.lymedisease.org/charles-ray-jones-dies-at-age-93/)
Why This Information Is Not Publicly Tracked
1. Patient Confidentiality: Medical boards do not publicly release patient information or medical records, so there is no official, verifiable record of patient outcomes.
2. Lack of Scientific Consensus: The core of the issue is the disagreement over what constitutes "recovery" and the cause of a patient's symptoms. Mainstream medicine (IDSA) does not believe the symptoms are due to an active infection, so they would not attribute any improvement to long-term antibiotics.
3. Legal and Professional Risk: Due to the risk of lawsuits and disciplinary action, doctors and patients are often hesitant to make public claims about treatment and recovery that fall outside of the established guidelines.
What is the official stance of health insurance companies regarding the treatment of Lyme disease and other tick-borne illnesses?
The official stance of most U.S. health insurance companies regarding the treatment of Lyme disease and other tick-borne illnesses is to follow the guidelines set by the Infectious Diseases Society of America (IDSA). This position has a significant impact on what treatments are covered and for how long.
Here's a breakdown of that official stance:
1. Coverage for Acute Illness
Health insurance companies generally cover the initial diagnosis and treatment of acute Lyme disease and other tick-borne illnesses. This includes:
• Initial doctor's visits: Consultations with a primary care physician or infectious disease specialist.
• Standard Diagnostic Tests: Coverage for the recommended two-tiered testing for Lyme disease (ELISA and Western Blot).
• Short-Term Antibiotics: The initial course of oral or, in some cases, intravenous antibiotics, typically lasting for 2 to 4 weeks, is almost always covered.
2. The Stance on Chronic Symptoms
The official stance of insurance companies is that once a patient has completed the standard course of antibiotics, the infection is considered cured.
If a patient continues to experience symptoms, this is classified as Post-Treatment Lyme Disease Syndrome (PTLDS).
The IDSA and the insurance industry's position is that these symptoms are not due to an active, ongoing infection and are therefore not treated with additional antibiotics.
Because of this, insurance companies generally do not cover long-term antibiotic therapy for PTLDS. This treatment is often classified as "experimental," "investigational," or "medically unnecessary" because it is not supported by the IDSA's guidelines.
3. State-Specific Exceptions
In a growing number of states, patient advocacy and legislative efforts have forced a change in this policy. Some states, including Connecticut, Massachusetts, Maine, and Maryland, have passed laws that mandate insurance companies to cover long-term antibiotic treatment for Lyme disease under certain conditions, usually with the attending physician's clinical recommendation.
4. Patient Burden
For patients living in states without such protective laws, the cost of long-term treatment falls almost entirely on them, leading to significant out-of-pocket expenses. Many patients have to seek care from "Lyme-literate" doctors (LLMDs) who practice outside of the IDSA guidelines, and most of these doctors are not in-network with major insurance companies. This financial burden is a major part of the reason why chronic Lyme disease is so life-altering.
Are there other health conditions where patients are denied care the way tick-borne disease patients are?
Yes, unfortunately, the struggles faced by patients with long-term tickborne illnesses are not unique. Several other health conditions, particularly those that are complex, "invisible," and lack a definitive diagnostic test or a universally accepted treatment protocol, face similar challenges. This often leads to a cycle of medical dismissal, insurance denials, and patient frustration.
Here are some other health conditions where patients face similar battles:
1. Myalgic Encephalomyelitis/Chronic Fatigue Syndrome (ME/CFS)
• The Problem: ME/CFS is a debilitating, multi-system illness with no known cause, no cure, and no single diagnostic test. Its symptoms—including severe fatigue, post-exertional malaise (worsening of symptoms after physical or mental exertion), pain, and cognitive issues—are subjective and can fluctuate, leading many doctors to dismiss them as psychological or stress-related.
• Lack of Consensus: Like chronic Lyme, there is a lack of consensus on the underlying biology of ME/CFS, which leads to limited and often insufficient treatment options. Patients frequently face medical gaslighting, where their symptoms are minimized or attributed to their emotional state.
2. Fibromyalgia
• The Problem: Fibromyalgia is a chronic disorder characterized by widespread pain, fatigue, and other symptoms. It is a diagnosis of exclusion, meaning doctors diagnose it after ruling out other conditions. There is no blood test or scan to confirm it, and its cause is not fully understood.
• Treatment Controversy: There is no cure, and treatment focuses on symptom management with a combination of medication, physical therapy, and lifestyle changes. The subjective nature of the pain and the lack of a clear biological marker have historically led to the same kind of dismissal and disbelief from the medical community that Lyme patients face.
3. Long COVID
• The Problem: In the wake of the COVID-19 pandemic, a new "contested illness" has emerged: Long COVID. Millions of people are experiencing lingering, debilitating symptoms such as fatigue, "brain fog," shortness of breath, and pain, often months or even years after their initial infection.
• The Parallel to Lyme: The experience of Long COVID patients mirrors that of chronic Lyme patients. They are often told by doctors that their symptoms are psychological, their tests come back normal, and there is no standard, effective treatment. This has created a new wave of patient advocacy to push for more research, better diagnostic tools, and a recognized standard of care.
4. Endometriosis and Other Chronic Pain Conditions
• The Problem: Endometriosis is a condition where tissue similar to the lining of the uterus grows outside of it, causing severe pain. It can take years to get a diagnosis, as its symptoms are often dismissed as "bad period pain" or a normal part of a woman's life.
• Delayed Diagnosis: On average, it takes 7 to 10 years for a person with endometriosis to be accurately diagnosed. This is due to a lack of awareness and a tendency for medical professionals to gaslight patients by minimizing their pain and symptoms.
These conditions highlight a systemic issue in medicine where complex, invisible, or poorly understood illnesses are often relegated to a category of "contested illnesses." This can leave patients feeling invalidated, financially drained, and without a clear path to recovery.
On average, how many doctors does a patient suffering from tick bites see before receiving a proper diagnosis?
Based on studies and patient surveys, it's not uncommon for a person with a tickborne illness to see four or more doctors before receiving an accurate diagnosis. Some surveys show an even higher number, with some patients reporting seeing more than ten doctors.
Here's why this number is so high:
• Misdiagnosis is Common: A significant number of tickborne illness cases, especially those without the classic "bull's-eye" rash, are initially misdiagnosed. A 2018 study found that 72% of patients were misdiagnosed with another condition before receiving a Lyme diagnosis. Common misdiagnoses include fibromyalgia, chronic fatigue syndrome, multiple sclerosis, and various psychiatric disorders.
• Vague Symptoms: Early symptoms like fever, fatigue, and muscle aches are often mistaken for the flu or other viral infections, leading to a "wait-and-see" approach from the initial physician.
• Unreliable Tests: The standard antibody tests for Lyme disease can produce false negatives in the early stages of the illness. A patient may get a negative result from their first doctor, leading that doctor to rule out a tick-borne illness and refer them to specialists for other conditions, such as a rheumatologist for joint pain or a neurologist for cognitive issues.
• Lack of Awareness: In areas where tick-borne illnesses are not highly endemic, doctors may not even consider it as a possibility, further contributing to a long and frustrating diagnostic journey
Why are tick-borne illnesses harder to treat than most cancers?
Comparing the treatment of tick-borne illnesses to cancer is complex, but for many patients, particularly those with chronic, debilitating symptoms, tick-borne illnesses can be far more challenging to treat. This difficulty is not about the risk of death, as many cancers are more fatal, but about the long-term, systemic nature of the illness and a lack of medical and scientific consensus.
Here are the key reasons why severe tick-borne illnesses are often harder to treat than most cancers:
1. Diagnostic Uncertainty vs. Definitive Diagnosis
• Tick-borne Illnesses: There is no definitive "gold standard" test for many tick-borne illnesses, particularly in later stages. The current tests are antibody-based and can produce false negatives in the early stages and remain positive long after a perceived "cure," making it difficult to determine if an infection is still active.
• Cancer: Cancer is diagnosed through objective measures such as biopsies, imaging (MRI, CT scans), and blood markers that can be used to track the disease's progression and a treatment's effectiveness. There is a clear, objective diagnosis to work from.
2. Lack of a Proven, Universal Cure
• Tick-borne Illnesses: While most early-stage cases are cured with a short course of antibiotics, a significant percentage of patients go on to develop Post-Treatment Lyme Disease Syndrome (PTLDS). The cause of PTLDS is not fully understood, and there is no universally accepted or FDA-approved treatment for it. The debate over whether to use long-term antibiotics is highly contentious, leaving many patients without a clear path to recovery.
• Cancer: For many cancers, there are well-established, evidence-based treatment protocols (surgery, chemotherapy, radiation, immunotherapy). A patient's response to these treatments is often predictable and measurable, with a clear endpoint for treatment.
3. Bacterial Persistence and Evasion
• Tick-borne Illnesses: Research suggests that the Lyme bacteria (Borrelia burgdorferi) can be incredibly difficult to eradicate. They may be able to hide in tissues, form biofilms (protective communities of bacteria), or transform into dormant "persister" cells that are tolerant of antibiotics. This could explain why symptoms return after a patient completes a standard course of treatment.
• Cancer: While cancer cells can be very aggressive and difficult to eliminate, they do not have the same ability to hide and evade treatment as bacteria can. Treatment focuses on directly killing or shrinking the cancerous cells.
4. Co-infections and Immune Dysregulation
• Tick-borne Illnesses: A single tick bite can transmit multiple pathogens (e.g., Lyme, Babesiosis, Anaplasmosis). These co-infections can complicate the diagnosis and lead to more severe, systemic symptoms that are harder to treat. In addition, tick-borne illnesses can trigger a persistent inflammatory or autoimmune response in the body that can continue long after the infection is gone.
• Cancer: While cancer treatment can have severe side effects, the goal is to kill the cancerous cells, not to combat multiple different pathogens and an overactive immune system at the same time.
5. Medical and Financial Disbelief
• Tick-borne Illnesses: Patients with long-term symptoms often face disbelief from the medical community, who may dismiss their symptoms as psychological or a different, less serious condition. Because the standard treatment is not working and the illness is not "visible," patients can struggle to get insurance coverage for continued care and face a significant financial burden.
• Cancer: While cancer patients face their own significant financial and emotional burdens, the disease is universally recognized as real and serious. They are not typically dismissed by doctors or denied coverage for standard, protocol-based treatments.
Which organs can be affected by tick-borne vectors?
Tick-borne illnesses are systemic diseases, meaning they can spread throughout the body and affect multiple organ systems. The specific organs and severity depend on the type of illness, whether it's an early or late-stage infection, and whether co-infections are present.
Here is a list of organs and systems commonly affected by tick-borne vectors:
1. Nervous System
• Brain: Infections can cause meningitis (inflammation of the membranes around the brain and spinal cord) and encephalitis (inflammation of the brain itself). This can lead to severe headaches, neck stiffness, confusion, memory loss, and in severe cases, seizures, coma, or permanent neurological damage.
• Peripheral Nerves: Tick-borne illnesses can cause neuropathy, leading to pain, numbness, tingling, or weakness in the hands and feet.
• Cranial Nerves: Lyme disease can cause facial palsy, which is the temporary paralysis of one side of the face.
2. Joints and Muscles
• Joints: One of the most common and well-known complications of untreated Lyme disease is Lyme arthritis, which causes pain, swelling, and inflammation, most often in the large joints like the knees.
• Muscles: Widespread muscle pain and body aches are common symptoms in the early and late stages of many tick-borne illnesses, including Lyme, anaplasmosis, and ehrlichiosis.
3. Heart
• Cardiac Tissue: The Lyme bacteria can invade heart tissue, causing Lyme carditis. This can disrupt the heart's electrical signals, leading to irregular heart rhythms (heart block), dizziness, shortness of breath, and in rare cases, heart failure and death.
4. Blood and Lymphatic System
• Blood Cells: Several tick-borne illnesses directly affect blood cells.
• Anaplasmosis and Ehrlichiosis invade white blood cells, which can lead to a low white blood cell count (leukopenia) and low platelet count (thrombocytopenia), increasing the risk of bleeding.
• Babesiosis is a parasitic infection that invades and destroys red blood cells, leading to a condition similar to malaria. This can cause severe anemia and jaundice.
• Spleen and Lymph Nodes: Swollen lymph nodes are common, and in some cases, the spleen can become enlarged.
5. Liver and Gastrointestinal Tract
• Liver: Many tick-borne illnesses, including Lyme, anaplasmosis, and ehrlichiosis, can cause inflammation of the liver, leading to elevated liver enzymes and, in some cases, liver dysfunction.
• Gastrointestinal Tract: Non-specific symptoms like nausea, vomiting, diarrhea, and abdominal pain are common in many tickborne diseases.
6. Skin
• Rash: The most well-known skin symptom is the erythema migrans rash of Lyme disease. Other tick-borne illnesses like Rocky Mountain spotted fever can cause different types of rashes.
In summary, a tick-borne infection is not a localized problem. The pathogens can spread throughout the body, making them a systemic threat that can affect virtually every major organ system if not caught and treated in time.
Is tick-borne illness considered a multi-sympton, multi-organ disease?
Yes, tick-borne illness is absolutely considered a multi-system, multi-organ disease, especially if left untreated. While the initial symptoms might be limited to a rash and flu-like complaints, the pathogens (bacteria, viruses, or parasites) can spread throughout the body, affecting a wide range of organs and systems. This is a key reason why tick-borne illnesses are so complex and challenging to diagnose and treat.
Here's a breakdown of how different organ systems can be affected:
1. Neurological System
• Brain: Can be affected by meningitis (inflammation of the membranes covering the brain and spinal cord), encephalitis (inflammation of the brain itself), or encephalopathy (cognitive impairment). This can lead to severe headaches, "brain fog," memory problems, confusion, and nerve pain.
• Peripheral Nerves: Infections can cause neuropathy, leading to shooting pains, numbness, tingling, or weakness in the hands and feet.
• Cranial Nerves: A classic sign of disseminated Lyme disease is facial palsy, which is the paralysis of one side of the face.
2. Musculoskeletal System
• Joints: Lyme arthritis is a common late-stage complication, causing painful swelling and inflammation, most often in large joints like the knees.
• Muscles: Widespread muscle aches (myalgia) are a frequent symptom in many tickborne illnesses, including Lyme, anaplasmosis, and ehrlichiosis.
3. Cardiac System
• Heart: Tick-borne pathogens can infect the heart's tissues, leading to Lyme carditis. This can cause irregular heart rhythms, dizziness, shortness of breath, and in rare cases, heart failure.
4. Blood and Lymphatic System
• Blood Cells: Some tick-borne illnesses, like anaplasmosis and ehrlichiosis, invade white blood cells, which can lead to low white blood cell counts (leukopenia). Babesiosis is a parasitic infection that destroys red blood cells, causing anemia and severe fatigue.
• Lymph Nodes: Swollen lymph nodes are a common symptom as the body fights the infection.
5. Liver and Gastrointestinal System
• Liver: Tick-borne illnesses can cause inflammation of the liver (hepatitis), which may be a source of gastrointestinal symptoms like nausea, vomiting, and abdominal pain.
• Spleen: The spleen can become enlarged (splenomegaly) as it works to filter the blood and combat the infection.
This multi-system involvement is why a patient with a tick-borne illness might be bounced between specialists, seeing a rheumatologist for joint pain, a neurologist for nerve issues, and a cardiologist for heart palpitations—each treating a symptom without recognizing the underlying systemic cause.
What's the latest discovery of a symptom brought on by a tick-borne illness patient who is consuming red meat?
The most significant discovery regarding a symptom linked to a tick-borne illness and red meat is Alpha-gal syndrome (AGS). While not a new discovery in itself (the link was first identified in 2009), there have been several recent developments that have brought it to the forefront of public health awareness.
What is Alpha-gal Syndrome?
Alpha-gal syndrome is a type of delayed allergic reaction to a sugar molecule called alpha-gal. This molecule is found in the meat of most mammals (like beef, pork, and lamb) and in products made from mammals (like gelatin, dairy, and some medications).
The syndrome is triggered by the bite of certain ticks. The most well-known culprit in the United States is the Lone Star tick. When a Lone Star tick bites a human, it can transmit the alpha-gal sugar from its saliva into the person's bloodstream. The person's immune system, which doesn't have this molecule, recognizes it as a foreign substance and creates antibodies to fight it.
The unique and challenging aspect of AGS is that the allergic reaction is delayed, often occurring 2 to 6 hours or more after a person eats red meat. This delay makes it very difficult for patients and doctors to connect the symptoms to a specific food.
Recent Discoveries and Developments
• Spread of the Condition: Recent research has shown a significant increase in the number of cases and a geographic expansion of the ticks that cause it. The Lone Star tick, once primarily a resident of the southeastern U.S., is moving northward due to climate change. There have also been confirmed cases linked to other tick species, including the black-legged tick (deer tick), which is the primary vector for Lyme disease. This expands the potential risk to new populations in different regions.
• The Scale of the Problem: The CDC recently reported that there were over 110,000 suspected cases between 2010 and 2022, but they estimate the actual number of people affected could be as high as 450,000, suggesting many cases go undiagnosed due to the delayed and often non-specific nature of the symptoms.
• A Broader Range of Symptoms: While the classic symptoms are hives and anaphylaxis, recent findings suggest that some people with AGS may only experience gastrointestinal issues, such as severe stomach pain, nausea, and diarrhea. This makes diagnosis even more challenging, as these symptoms can be mistaken for Irritable Bowel Syndrome (IBS) or other digestive disorders.
• New Research on Treatment: Researchers are working on new treatments for AGS, including a promising nanoparticle-based approach that was shown to prevent allergic reactions to red meat in mice. This could be a significant step toward developing a treatment that goes beyond simply avoiding red meat.
What is the dollar value per person of funding for Lyme Disease research in relation to other diseases in the United States?
When looking at federal research funding, particularly from the National Institutes of Health (NIH), the dollar value per person for Lyme disease is significantly lower than for other major illnesses. This disparity is a key point of contention for patient advocates who argue that the funding does not match the public health burden of the disease.
While specific, up-to-the-minute figures for a "per-person" comparison can be hard to pinpoint and vary each fiscal year, historical and recent data illustrate the vast difference:
• Lyme Disease: The number of new Lyme disease cases is estimated to be around 476,000 per year, though the actual number is likely much higher. In 2022, NIH funding for Lyme research was approximately $50 million. This equates to about $105 per case for that year's confirmed infections. While more recent figures show an increase in funding, the total amount is still a fraction of what is allocated for other major diseases.
• HIV/AIDS: HIV/AIDS has long been a model for well-funded research due to aggressive advocacy and a strong government response. Historically, NIH funding for HIV/AIDS has been in the billions of dollars. A 2023 report from LymeDisease.org highlighted that Lyme research received less than 2% of the public funds invested in HIV/AIDS, even though the annual case count for Lyme is over an order of magnitude higher. This vast difference in funding per patient is a major argument made by advocates for increased Lyme research.
• Cancer: Cancer research receives the largest portion of NIH funding, with billions of dollars allocated annually. For example, the Cancer Moonshot initiative alone has received billions in a proposed budget. This funding level is a reflection of the significant public health burden of cancer, but when compared on a per-patient basis, the disparity with Lyme disease is clear.
The reason for this discrepancy is a mix of historical context, advocacy, and the medical community's perception of the diseases. HIV/AIDS and cancer are universally recognized as life-threatening, and their research has had decades of substantial, uninterrupted government support.
In contrast, Lyme disease, particularly the chronic form, has been mired in a medical controversy that has made it more difficult for advocates to secure commensurate funding.
Have tick-borne diseases been found in all 50 states?
Yes, tickborne diseases have been found in all 50 states and Washington, D.C. While the risk and prevalence vary significantly by region and state, no state is completely free of tickborne illnesses.
Here's a breakdown of the geographic distribution:
• Lyme Disease: The most common tick-borne illness, Lyme disease, is heavily concentrated in the Northeast and upper Midwest. However, it is also found on the West Coast, and its range is expanding due to climate change and other factors.
• Rocky Mountain Spotted Fever: Despite its name, Rocky Mountain spotted fever is most commonly found in the southeastern and south-central United States.
• Other Illnesses: Diseases like Anaplasmosis and Babesiosis are also prevalent in the Northeast and upper Midwest. In the South, you'll find other pathogens carried by different tick species, such as those that cause Ehrlichiosis and Alpha-gal Syndrome.
The key takeaway is that while certain states are considered high-risk, a person can contract a tick-borne illness almost anywhere in the country. Therefore, it is important to take precautions against tick bites regardless of location.
How can people best protect themselves from tick bites?
Protecting yourself from tick bites is crucial, especially when spending time in wooded, grassy, or brushy areas. The most effective strategy involves a combination of personal and environmental precautions.
1. Protect Your Body and Clothing
• Wear Appropriate Clothing: When outdoors, wear long pants, a long-sleeved shirt, and socks. Tuck your pants into your socks and your shirt into your pants to create a physical barrier.
• Choose Light Colors: Wearing light-colored clothing makes it easier to spot ticks crawling on you.
• Use an EPA-Approved Repellent: Apply an insect repellent to exposed skin and clothing. Look for products that contain an EPA-registered active ingredient, such as:
• DEET: Concentrations of 20-30% provide excellent protection.
• Picaridin: A good alternative to DEET that is less greasy and has a milder smell.
• Oil of Lemon Eucalyptus (OLE) or PMD: A plant-based option.
• Treat Clothing with Permethrin: Permethrin is an insecticide that can be applied to clothing, shoes, and gear, but never directly on skin. It kills ticks on contact and remains effective through several washings. You can buy pre-treated clothing or treat your own.
2. Check for Ticks
• Perform a Full-Body Check: After spending time outdoors, conduct a thorough check of your body, your children, and your pets. Ticks love to hide in warm, moist, and hard-to-see areas, but can be found on any part of the body.
• Under the arms
• In and around the ears
• In the hair and on the scalp
• Behind the knees
• Between the legs and around the groin
• Inside the belly button
• Check Your Gear: Ticks can hitch a ride on clothing, backpacks, and gear. A simple trick is to tumble-dry your clothes on high heat for 10 minutes after returning indoors to kill any ticks that may be clinging to them.
• Shower Soon After Coming Inside: Showering within two hours of coming indoors has been shown to reduce the risk of Lyme disease. It can help wash off unattached ticks and provides a great opportunity for a thorough tick check.
3. Tick-Proof Your Yard
• Maintain Your Yard: Keep your lawn mowed short and clear away leaf litter, tall grasses, and brush, especially around the edges of your property where the lawn meets wooded areas.
• Create a Barrier: Place a barrier of wood chips or gravel (at least 3 feet wide) between your lawn and wooded areas.
• Stack Wood Neatly: Store woodpiles in a dry, sunny area away from your house to discourage rodents, which can carry ticks.
• Limit Wildlife Access: Consider fencing to keep deer and other wildlife that may carry ticks from entering your yard.
What should a person do if they find a tick embedded?
Finding a tick embedded in your skin can be unsettling, but quick, proper removal is the most important step to reduce your risk of a tick-borne illness. The key is to remove it as soon as possible, as the risk of transmitting diseases like Lyme disease increases the longer the tick is attached.
Here is a step-by-step guide on what to do:
1. Remove the Tick Safely
• Gather your tools: You'll need clean, fine-tipped tweezers, rubbing alcohol or an iodine scrub, soap, and warm water.
• Grasp the tick: Using tweezers, grab the tick as close to the skin's surface as possible, ideally by its head or mouthparts. Do not grab the tick by its body, as squeezing it could force infected fluids from the tick into your skin.
• Pull with steady pressure: Pull the tick straight upward with slow, even pressure. Avoid twisting or jerking, which can cause the mouthparts to break off and remain in the skin
• Clean the area: After removal, thoroughly clean the bite area and your hands with rubbing alcohol, an iodine scrub, or soap and water.
• Dispose of the tick: To prevent it from biting someone else, dispose of the tick by placing it in a sealed container, wrapping it tightly in tape, or flushing it down the toilet. Do not crush the tick with your fingers.
What should one do with the tick once it's been pulled from the skin?
Once a tick has been properly removed, you have a few options for what to do with it. The most common and recommended approach is simply to dispose of it to prevent it from biting anyone else. However, some people choose to save the tick for testing.
1. The Recommended Method: Disposal
The Centers for Disease Control and Prevention (CDC) and most public health organizations recommend the following disposal methods:
• Flush it down the toilet: This is a simple and effective way to ensure the tick is gone for good.
• Wrap it tightly in tape: You can wrap the tick in clear tape and then throw it in the trash. This prevents it from getting out.
• Place it in a sealed container or bag: You can put the tick in a small, sealed container with rubbing alcohol to kill it.
Do NOT crush the tick with your fingers. This can release infectious fluids that could enter your bloodstream through small cuts or abrasions on your skin.
2. Do NOT Use "Home Remedies"
Avoid unproven methods to remove a tick, such as burning it with a match or smothering it with petroleum jelly, nail polish, or essential oils. These methods can agitate the tick and cause it to regurgitate into the bite wound, increasing the risk of disease transmission.
3. Testing the Tick
Some people choose to save the tick to have it tested for pathogens. While this can provide some peace of mind, it is not recommended by the CDC for guiding treatment decisions.
• What to do: If you want to have the tick tested, place it in a sealed plastic bag or container. You may want to record the date of the bite, where you were bitten on your body, and the location where you were when you were bitten.
• Why the CDC discourages it: The CDC advises against using the results of tick tests to decide on a course of treatment for several reasons:
• Results may not be reliable: The laboratories that test ticks are not required to meet the same quality standards as those used for patient care.
• A positive result is misleading: Even if a tick tests positive for a disease, it doesn't mean that the pathogen was successfully transmitted to you.
• A negative result is also misleading: You may have been bitten by another infected tick that you didn't see.
Instead of relying on the tick test, the CDC recommends focusing on monitoring your own symptoms. If you develop a rash, fever, or other flu-like symptoms in the days or weeks following a tick bite, you should contact your doctor immediately. Your doctor will make a diagnosis based on your symptoms, your history of exposure, and, in some cases, blood tests.
4. Monitor Your Symptoms
Over the next few weeks, pay close attention to the bite area and any changes in your health. Keep an eye out for:
• A rash, especially an expanding red patch or a bull's-eye rash.
• Fever, chills, or flu-like symptoms.
• Headaches, muscle aches, or joint pain.
• New or worsening redness, swelling, or oozing at the bite site.
5. When to See a Doctor
It is advisable to contact a healthcare provider if:
• You are unable to remove the entire tick.
• You develop a rash or any of the symptoms listed above.
• You live in an area where Lyme disease is common, and the tick was attached for more than 24 hours.
How can I locate a Lyme Literate Medical Doctor (LLMD) in my area?
Finding a "Lyme-literate medical doctor" (LLMD) can be challenging because the term is not a formal medical designation or board certification. Instead, it refers to a doctor who, through clinical experience or specialized training, is willing to diagnose and treat Lyme disease and other tickborne illnesses beyond the standard of care recommended by the Infectious Diseases Society of America (IDSA).
Here are the most common and effective ways to find an LLMD in your area:
1. Patient Advocacy and Support Organizations
These are often the best resources for finding an LLMD. Because of the controversial nature of treating chronic Lyme disease, many doctors who specialize in it are not publicly listed in mainstream medical directories to avoid professional persecution. Patient groups and non-profits, however, maintain referral lists.
• International Lyme and Associated Diseases Society (ILADS): ILADS is the leading organization for doctors who treat Lyme disease with long-term protocols. Their website has a "Provider Search" tool where you can look for members in your area. They also offer a physician training program, and you can refine your search to find doctors who have completed it.
• LymeDisease.org: This patient advocacy group has a "Physician Directory" and a referral system that can help you find a doctor who is knowledgeable about chronic Lyme disease and other tickborne illnesses.
• Global Lyme Alliance (GLA): The GLA has a service where you can submit an online form, and they will provide you with a list of specialists in your area.
• State and Local Lyme Organizations: Many states have their own Lyme disease advocacy groups (e.g., the Pennsylvania Lyme Resource Network, the Lyme Disease Association of New Jersey). These organizations often have a deeper understanding of which doctors in their state are willing to treat long-term Lyme and may offer referral lists or a more personalized referral service.
2. Online and Local Support Groups
Online communities, particularly on platforms like Facebook, are a common way for patients to find referrals. Search for groups for Lyme disease in your state or region. Once you join a private group, you can ask other members for recommendations for doctors they have seen and had a positive experience with. This provides a direct, patient-to-patient referral network.
3. Integrative and Functional Medicine Practices
Many doctors who treat chronic Lyme disease do so from an integrative or functional medicine perspective. These practitioners focus on identifying and treating the root cause of a patient's symptoms, which aligns with the belief that chronic Lyme is a persistent infection. When searching, you can look for practitioners who specialize in chronic illness, complex cases, or multi-system disorders.
Important Considerations:
• Discreet Practices: Due to the professional risks, many LLMDs do not advertise their specialty. Their websites may use more general language like "complex chronic illness" or "multi-system disorders" rather than explicitly mentioning Lyme disease.
• Insurance and Cost: Be aware that most LLMDs do not accept health insurance, as their treatment protocols are often not covered. You should ask about their fees, and if they offer any payment plans or financial assistance.
Answers were drawn from a vast dataset that includes information from a wide range of sources, including:
• Public Health Organizations: The Centers for Disease Control and Prevention (CDC), the National Institutes of Health (NIH), and state and local health departments.
• Medical Societies: The Infectious Diseases Society of America (IDSA), the American Academy of Neurology, and the American College of Rheumatology.
• Patient Advocacy Groups: The International Lyme and Associated Diseases Society (ILADS), LymeDisease.org, Global Lyme Alliance (GLA), and others.
• Academic and Medical Journals: Articles and research published in journals such as The New England Journal of Medicine, JAMA, and Clinical Infectious Diseases.
• Medical Textbooks and Training Materials: Information found in standard medical school and residency curricula.
• News Reports and Articles: Reputable news sources that have covered the science, politics, and patient experiences related to tickborne illnesses.
The information on the different perspectives regarding treatment protocols, the challenges in diagnosis, and the political and financial aspects is all well-documented in these various sources. The goal has been to provide a comprehensive and balanced overview of a complex topic by incorporating different viewpoints, while also distinguishing between mainstream medical consensus and the perspectives of patient advocates. — Kat
#lymedisease, #tickborneillness, #invisibleillness, #chronicillness, #chroniclyme, #persistentlyme, #PTLDS #babesiosis, #lymeliteratemedicaldocter, #HBOT, #lymeliteracy, #functionalmedicine, #integrativemedicine, #alphagal, #lifeworkswellnesscenter, #prayersforannie


