- A
- S
- B
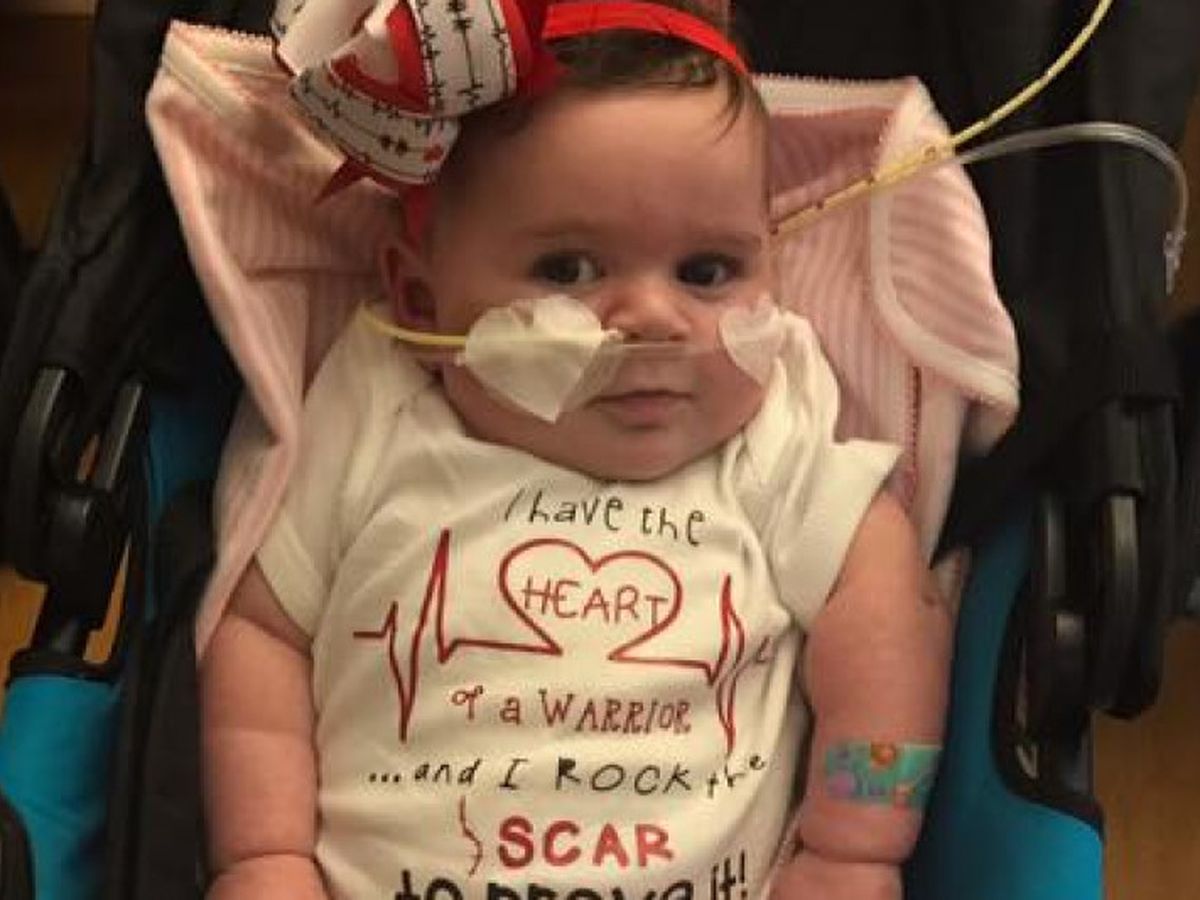
This is the story of my granddaughter's ongoing medical miracle journey as told by her mother, Samantha Bowling Bryant:

My daughter’s medical miracle journey began before she was even born when I went in for what was supposed to be a routine ultrasound. At 29 weeks into my pregnancy the ultrasound revealed my baby, who I had already named Adalyn Grace, had a heart that had only a single ventricle. Three weeks later the news became even more grim when doctors determined Adalyn also had a severely restricted atrial septum and mitral valve atresia. My husband and I were told that without a mitral valve, the only way blood would be able to circulate through her tiny heart was through the severely restricted atrial septum. At this point, doctors could not be certain her lungs were developed enough to sustain life. We put our faith in God and prayed for a miracle. At 36 weeks, after taking early medical leave from my job as a high school math teacher in Laurel County Kentucky, I relocated to Cincinnati to be close to the myriad of doctors at Cincinnati Children's Hospital who were developing a plan for Adalyn's delivery. My husband, Eric, an EMT who was also in his second semester of training to become a paramedic, remained at home in order to work, attend school and take care of our six year old son, Landon. At 38 weeks 5 days, we got our miracle! On April 3, 2017, 9.7 lb/21 inch long, Adalyn Grace Bryant was born in the cath lab at Cincinnati Children's Hospital.

Only a handful of babies had been delivered in this setting previously; however, doctors knew they only had a narrow window of opportunity to open the atrial septum, so time was one of the biggest factors in her chance at survival. Immediately after birth doctors performed two heart caths. This procedure allowed them to place stents in her heart to open the atrial septum. The doctors were amazed to find that her lungs were fully developed and functioning as they should. We knew at this point, that our Adalyn was not only a miracle, she was also a fighter.

The next step in the process was an echocardiogram that revealed even more bad news. Her heart had a double inlet left ventricle with a hypoplastic right ventricle, a D-loop transposition of the great arteries, mitral valve atresia, a straddling tricuspid valve, ventricular septal defect, tricuspid regurgitation and an overriding aortic arch. In short, in order for Adalyn to survive, it would be necessary for her to have a series of open heart procedures. At only 5 days old, Adalyn had her first open heart surgery, a procedure known as the Norwood, which consisted of doctors placing a 4 mm shunt in her heart and working on her overriding arch.
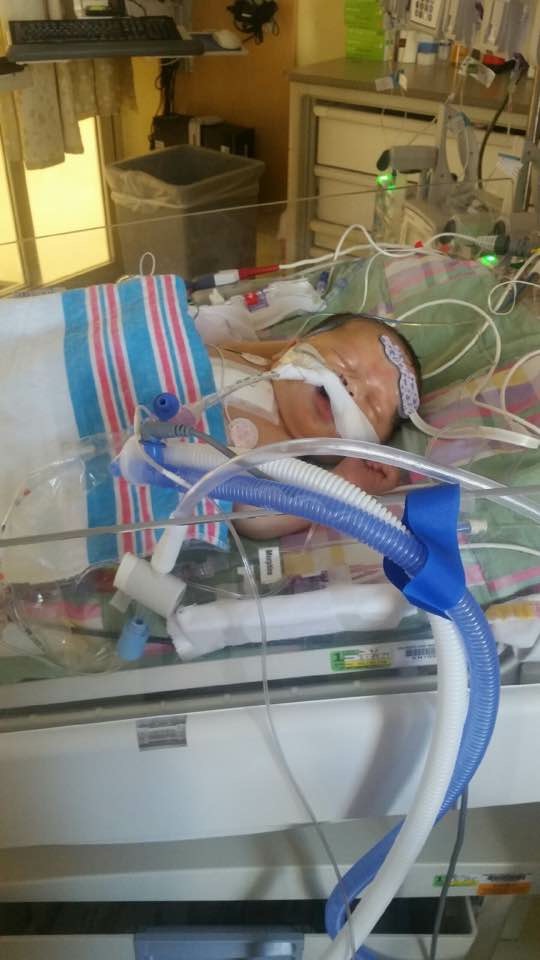
The surgery was a success and Adalyn and I spent another 18 days in the Neonatal Cardiac Intensive Care Unit with round-the-clock care and monitoring. Thankfully Eric was able to spend several nights with her as well, though big brother still was not able to visit.

 During her stay in the NCICU doctors discovered she was having silent aspirations when drinking from a bottle so an NG tube was placed for feedings. Even that didn’t hold her back. She continued to amaze her medical team and was finally moved to a step down unit where I learned to take care of her many medical needs.
During her stay in the NCICU doctors discovered she was having silent aspirations when drinking from a bottle so an NG tube was placed for feedings. Even that didn’t hold her back. She continued to amaze her medical team and was finally moved to a step down unit where I learned to take care of her many medical needs.

Only 23 days after she was born, Adalyn Grace was able to go home.

Since leaving the hospital we have a daily routine that consists of close monitoring of her weight and vital signs along with the dispensing of round-the- clock medications and, of course, feedings through the NGtube. Though we have real-time contact with her medical team via technology, we still are required to make weekly visits to the University of Kentucky Children’s Hospital to meet with a team of doctors there who report to her doctors in Cincinnati.

On June 23 Adalyn began the second step in her medical miracle journey when she underwent another heart cath for imaging for her next open heart procedure. Though the procedure itself was a success, doctors discovered she had developed a blood clot at the sight of the cath so twice daily injections are now required in order to break up the clot. As a result of the imaging done they discovered her pulmonary artery is hypoplastic but there is nothing at this time that can be done to correct it. On July 31st Adalyn will undergo her second open heart surgery at Cincinnati Children’s Hospital. This surgery, called the Bi-directional Glenn, is expected to take at least 9 hours and will require another long hospital stay.

Though we are nowhere near the end of this medical miracle journey, we have already amassed over $1 million in medical bills, a percentage not covered by medical insurance. The medical charges, the cost of travel and lodging, a depletion of paid sick days, and the many daily expenses needed for Adalyn’s care have placed our family in financial distress. On July 31, we will continue our journey with little funds and no paid time off work. Any help that is provided would go a long way in meeting our family’s immediate needs and would be greatly appreciated.


My daughter’s medical miracle journey began before she was even born when I went in for what was supposed to be a routine ultrasound. At 29 weeks into my pregnancy the ultrasound revealed my baby, who I had already named Adalyn Grace, had a heart that had only a single ventricle. Three weeks later the news became even more grim when doctors determined Adalyn also had a severely restricted atrial septum and mitral valve atresia. My husband and I were told that without a mitral valve, the only way blood would be able to circulate through her tiny heart was through the severely restricted atrial septum. At this point, doctors could not be certain her lungs were developed enough to sustain life. We put our faith in God and prayed for a miracle. At 36 weeks, after taking early medical leave from my job as a high school math teacher in Laurel County Kentucky, I relocated to Cincinnati to be close to the myriad of doctors at Cincinnati Children's Hospital who were developing a plan for Adalyn's delivery. My husband, Eric, an EMT who was also in his second semester of training to become a paramedic, remained at home in order to work, attend school and take care of our six year old son, Landon. At 38 weeks 5 days, we got our miracle! On April 3, 2017, 9.7 lb/21 inch long, Adalyn Grace Bryant was born in the cath lab at Cincinnati Children's Hospital.

Only a handful of babies had been delivered in this setting previously; however, doctors knew they only had a narrow window of opportunity to open the atrial septum, so time was one of the biggest factors in her chance at survival. Immediately after birth doctors performed two heart caths. This procedure allowed them to place stents in her heart to open the atrial septum. The doctors were amazed to find that her lungs were fully developed and functioning as they should. We knew at this point, that our Adalyn was not only a miracle, she was also a fighter.

The next step in the process was an echocardiogram that revealed even more bad news. Her heart had a double inlet left ventricle with a hypoplastic right ventricle, a D-loop transposition of the great arteries, mitral valve atresia, a straddling tricuspid valve, ventricular septal defect, tricuspid regurgitation and an overriding aortic arch. In short, in order for Adalyn to survive, it would be necessary for her to have a series of open heart procedures. At only 5 days old, Adalyn had her first open heart surgery, a procedure known as the Norwood, which consisted of doctors placing a 4 mm shunt in her heart and working on her overriding arch.

The surgery was a success and Adalyn and I spent another 18 days in the Neonatal Cardiac Intensive Care Unit with round-the-clock care and monitoring. Thankfully Eric was able to spend several nights with her as well, though big brother still was not able to visit.

 During her stay in the NCICU doctors discovered she was having silent aspirations when drinking from a bottle so an NG tube was placed for feedings. Even that didn’t hold her back. She continued to amaze her medical team and was finally moved to a step down unit where I learned to take care of her many medical needs.
During her stay in the NCICU doctors discovered she was having silent aspirations when drinking from a bottle so an NG tube was placed for feedings. Even that didn’t hold her back. She continued to amaze her medical team and was finally moved to a step down unit where I learned to take care of her many medical needs. 
Only 23 days after she was born, Adalyn Grace was able to go home.

Since leaving the hospital we have a daily routine that consists of close monitoring of her weight and vital signs along with the dispensing of round-the- clock medications and, of course, feedings through the NGtube. Though we have real-time contact with her medical team via technology, we still are required to make weekly visits to the University of Kentucky Children’s Hospital to meet with a team of doctors there who report to her doctors in Cincinnati.

On June 23 Adalyn began the second step in her medical miracle journey when she underwent another heart cath for imaging for her next open heart procedure. Though the procedure itself was a success, doctors discovered she had developed a blood clot at the sight of the cath so twice daily injections are now required in order to break up the clot. As a result of the imaging done they discovered her pulmonary artery is hypoplastic but there is nothing at this time that can be done to correct it. On July 31st Adalyn will undergo her second open heart surgery at Cincinnati Children’s Hospital. This surgery, called the Bi-directional Glenn, is expected to take at least 9 hours and will require another long hospital stay.

Though we are nowhere near the end of this medical miracle journey, we have already amassed over $1 million in medical bills, a percentage not covered by medical insurance. The medical charges, the cost of travel and lodging, a depletion of paid sick days, and the many daily expenses needed for Adalyn’s care have placed our family in financial distress. On July 31, we will continue our journey with little funds and no paid time off work. Any help that is provided would go a long way in meeting our family’s immediate needs and would be greatly appreciated.

Organizer and beneficiary
Samantha Bryant
Beneficiary