- K
- R
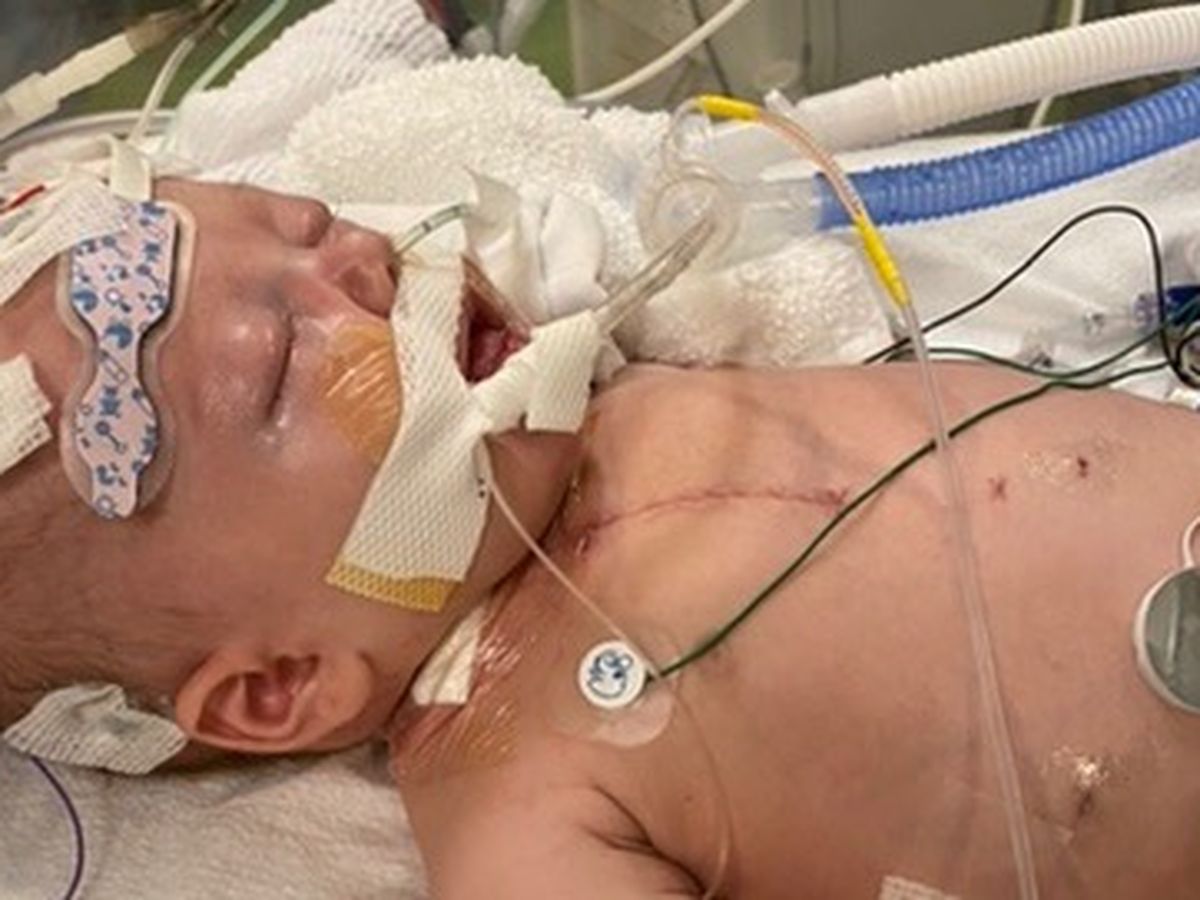
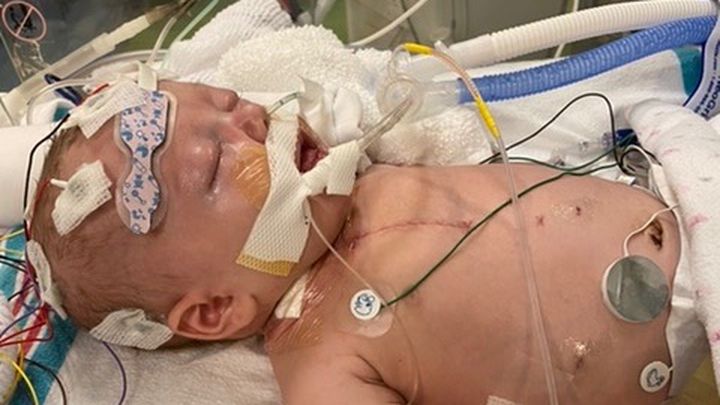
We never could have imagined we would be introducing our daughter to the world on this type of platform. Anyone who knows us personally knows that we aren’t social media people so you may not have met our beautiful daughter Hadley otherwise, but today you are. We honestly thought we would be home by now. I thought we would be spending time on our property, enjoying my favorite time of year. Going on walks and introducing Hadley to all the great things county life living has to offer. We are broken and numb but still very hopeful. Our baby is a fighter and we have to be strong for her. Hadley has already had several surgeries and will have to have at least 2 more open heart surgeries. She will need early intervention therapies to help her over come what she’s been through. Her stay at children’s and our stay at RMH will be much longer then we anticipated. But one thing is for certain is that we love her so much and she brings so much joy to our lives and we can’t picture our lives without her in it. She’s changed me for the better. We have so much love, support, and prayers and we 100% believe in the power of prayer. We are grateful for each and everyone one of you who have reached out and we look forward to the day when you can meet our Hadley.
Before we get into what brought us to this point, let me tell you where it all began for our precious Hadley...
At 17 weeks gestation, Hadley was diagnosed with a congenital heart defect called Pulmonary Atresia with VSD. We were absolutely devastated. They suggested an amniocentesis to rule out any syndromes that were not compatible with life that would attribute to the CHD. All those tests came back negative. We were so relieved. I was closely monitored by maternal fetal medicine doctors and a cardiologist at Children’s National in DC. During our first visit with them, they told us that she would need medication through an IV in her bellybutton as soon as she was born and then she would be transported to Children’s National where they would take over her care and determine if she would have a shunt put in and have the full repair at 6-9 months or have the full repair days after birth. We were scared but confident in their abilities to fix her broken heart.
At this point, MFM wanted to see me weekly for a sonogram to monitor her heart, brain, and growth. Once a month during one of my weekly visits, I would meet with the cardiologist via telemedicine and they would live scan so they could look at her heart development. As the weeks went on, she was getting bigger and bigger and her CHD was stable but remained unchanged. The team of doctors were very happy with her size as they prefer cardiac babies to be on the larger side. They planned to deliver her at 39 weeks and we chose to have her via cesarian section as to not stress her heart out during the laboring process.
The day she was born, she weighed 8lbs 15ozs and was 20 inches long. She came out crying and was ready to see the world and we were ready to meet her. During her short stay in the NICU at the hospital she was born at, she developed a love for her pacifier ❤️
She was transported via helicopter to Children’s within a few hours of birth while I began my recovery.
Upon arrival at Children’s, she received her first echocardiogram. During which, they found an additional defect. So in addition to the Pulmonary Atresia with VSD, she also has atrioventricular discordance (S,LL). The plan for surgery was the same but they decided to wait until she was 6-9 months old for the big repair to allow the heart to grow and mature. She was scheduled for a BT shunt at 6 days old. We arrived that morning and held her and took our first family photo. We had spent long days and nights with her leading up to this very big day but that morning in particular we knew, it was going to be our first of many long days of waiting and recovering.
During my hospital stay recovering from the c-section, I decided that we needed to be close to her and not travel back and forth to our home (it’s about 52 miles one way) so I reached out to our social worker and asked for a referral to the Ronald McDonald House. It took a few days and a background check but we were approved and were able to check in the night before her surgery. We were so grateful to be 7 minutes away.
The shunt surgery went very well. She spent a week in the CICU after surgery and then was transferred to HKU where she would finish out her stay and eventually be discharged home.
Due to being NPO pretty much from birth because of her impending heart surgery, she had to learn how to eat and how to let us know when she’s hungry. She had an ND tube placed for nutrition which would later become an NG tube. She was having trouble keeping the formula and/or breast milk down. She would eat and vomit shortly after. I finally convinced them to let me just bottle feed her. I wanted her to have a chance to be a “normal” baby and just eat from a bottle and tell us when she was hungry. So on the morning of Friday July 16th, the nurse pulled her NG tube and for the first time, she was bare faced. No more tape on her face holding the tube in place. It was such a site to see and a day I had been waiting for. We began the process of letting her eat every 3 hours. Speech came in and practiced with her. She was hesitant at first but she eventually got it down and would feed like a champ. Unfortunately, she was still vomiting a lot. She would keep some of it down, but not enough. As the weekend progressed, she was keeping less and less down. By Monday they were giving her a little more time to try and keep the feeds down but they were also going to reach out to the GI team to see what other tests they could run. Earlier that week before they pulled the NG tube out, she had an upper GI study to make sure there were no blockages. She passed that test with flying colors. On Tuesday July 20th, the GI team finally decided to order an abdominal ultrasound to determine if she had Pyloric Stenosis. The nurse and I wheeled her down to the second floor and she fell asleep on the way. She stayed asleep for the length of the ultrasound and the radiologist saw almost immediately that she did in fact have pyloric stenosis. We went back up to her room and waited for the team to meet to discuss the next steps. While I knew this would involved another surgery so soon after her open heart surgery, we finally had an answer as to why she wasn’t able to keep her formula down.
The team ultimately decided on laparoscopic surgery. Hadley was scheduled for surgery the next morning, July 22nd. And that leads me to where we are now...
On the morning of July 22, we arrived early so that we could spend some time with her before she went it. She was awake when we arrived in her room and for once she was in the same clothes I left her in because she wasn’t up all night vomiting. We held her and talked to her and I’ve been telling her for weeks now “I can’t wait to take you home, this isn’t your home” I know she’s my baby but she really is the sweetest thing. ❤️
Someone from the general surgery team arrived and it was time to wheel her down. We walked down with her. She was a little fussy but nothing her beloved paci couldn’t resolve. They hooked her up to the machines down there and she went over all the risks of the surgery with the cardiac anesthesiologist. Since Hadley has a shunt, she has a 5% risk of complications where as a “normal” baby only has 1%. The doctor came and spoke to us and said that the surgery would be pretty straight forward and she wouldn’t be in there long. We walked over to her bed, I leaned down and said to my sweet baby who was almost asleep “see you in a little bit, we love you.” Daniel bent down and said to his baby girl “we love you, see you soon.” They walked us to the registration desk and we were given a pager. When the pager goes off, we come back to the desk. It was about 45 minutes later and the pager went off. We were so excited to see our Hadley. The doctor came out and said she’s all done and in the CICU. When we rounded the corner on the way to her new CICU room is when the next chapter of our lives began...
When we first got here 5 weeks ago, her first CICU attending physician said “you don’t need to worry unless you see people running in her room.” When we rounded the corner on the way to her room, all we could see were people. Doctors and nurses rushing and communicating. Machines beeping. It was comparable in my mind, in that moment to a busy New York City street. I looked over to my left and the anesthesiologist yelled out to me “she’s okay, she just needs some extra support.” I went to go in her room and our social worker stopped us and said that she just needs some extra support and they are putting her breathing tube back in. My heart sank. She asked us to go wait in the waiting area and someone would be out to get us when we could come back to see her. I told her we would go to her room in HKU to get her stuff. When we came back from getting her stuff, Daniel got a phone call which he stepped outside to take. As soon as he was gone, a doctor and my social worker came out to the waiting area to tell us the news.
The doctor walked up to me and said “we are doing chest compressions on your daughter and we will need to open her chest and put her on ECMO.” My heart broke. I was in complete shock. I didn’t know what to say. I just hung my head and started to cry. I thought they were coming out to tell me we could see her and everything was fine after putting the breathing tube back in. They went back to attend to her and I immediately called Daniel and said “you need to get up here!” He said “what’s wrong?” I said “you need to get up here now!” He hung up and the next time I looked up he was standing in front of my. He kneeled down in front of where I was sitting and I repeated the heart breaking words I had just heard myself. He picked me up out of the chair and walked me to the other side which was a little more private. I looked up at him and sobbed “this wasn’t suppose to happen!!” Over the next hour several doctors, surgeons, NP’s, and our social worker would come out and update us. Every time we heard footsteps, we weren’t sure of the status we were going to be given. Her NP from HKU even came over and was consoling us. She said she would go be with her and try to find out more details. Everyone was in our corner that morning because no one expected for this to happen. The more updates we got, the calmer their body language was when they would approached us. Which was calming for me because body language and facial expressions are more powerful then words sometimes. The last update we got, they pulled us into a private room. My heart sank again, I thought for sure they were going to tell us our precious, sweet, feisty little girl was gone. But they didn’t. They went through a play by play of everything that went on. We were so numb at this point, we didn’t even know what to say. The only words I can remember them saying was “she’s on ECMO and she’s stable.” At this point, we’d heard this term “ECMO” so many times and I had no idea what it was but it was keeping our baby alive so it must be a miracle machine! The heart surgeon came out and had us sign a consent form. He explained what the ECMO machine was and that Hadley had 2 canulas in her chest that were doing all the work for her heart and lungs. They thankfully did not have to open her chest to place the canulas, they instead when through her neck, down into her heart.
Eventually our social worker came out and said “let’s go see your baby!” She wheeled her cart of all her pretty things into her room and we followed behind her. It was a site to see in there. These rooms are not very big but her room was just big enough for all her life saving equipment. Due to her critical condition, she had a full time bedside nurse that wasn’t allowed to exit the room unless someone knew it. She had 2 ECMO techs that monitored the machine very closely and they were also not allowed to leave the room unless someone sat in their place. N95 masks were required by all the hospital staff and Hadley was NOT to be moved in any way. Time passes by so slowly in the hospital sometimes but other times it passes by so fast. Before we knew it, it was shift change and she had a new nurse. The goal was to keep her comfortable and pain free and to keep her stable until the morning where she would go to the cath lab so they could look at her shunt to make sure it was functioning as it should. Hadley had an uneventful night that night. The next day, around 1:00pm, they began to prep her for transport to the cath lab. It’s a very delicate process moving her and all her life saving machines together. It takes a lot of skill and patients and her team did a great job. It took 10 people, each having their own roles in getting her safely to the cath lab. We went outside and got some fresh air while we waited. We eventually made our way back upstairs and the interventional cardiologists came out and told us Hadley indeed had a blood clot in her shunt. He showed us pictures and he was able to put a stent in her shunt to allow the blood to flow as it should. He said she tolerated the procedure well and they would let us know when we could see her again. We were so relieved. It was the first time in 30 hours that we were able to breathe. Hadley’s risk of a blood clot was 5%. He said she will need to be on multiple blood thinners going home and closely monitored. He anticipated that she could come off the ECMO machine the next day. The rest of the day and night was uneventful. They did an echocardiogram and the cardiologist gave have her 2 thumbs up to come off ECMO. We were so excited!
The next day (Friday) we got a call at 5:45 am from her nurse letting us know that Hadley was having seizures. She had been hooked up to an EEG machine since Wednesday evening so they could monitor her brain activity. My heart broke again. She said she didn’t have much more information but the doctors would talk to us when we came in that day. We cried and eventually went back to sleep. Those are phone calls we hoped we’d never get. Hadley was scheduled at 8:30 to come off the ECMO machine. It was considered a surgery so they called and asked for consent. They do the surgery at her bed side so we weren’t able to be with her. The nurse said she would call us when they were all done. We felt more comfortable waiting at RMH. By noon we still hadn’t heard anything so we called to get an update. The nurse said Hadley was off ECMO and it went very well and we could come whenever we felt comfortable. We found out later on that they didn’t start the surgery until 11:30 so she wasn’t in surgery for as long as we feared. We couldn’t wait to see our baby. She was still swollen but still looked like our sweet Hadley.
At around 3:30pm, they came in and said she was still having seizures. They ordered a CT scan and would know more after that. Shift change came around again and we were blessed with the night nurse we really liked and when she came on the floor, we expressed to her that no one had talked to us all day or given us any updates on Hadley’s status. During the day we didn’t really realize that no one had talked to us but when we realized how late in the day it actually was, we wanted answers.
At 8:34pm our world shattered again. When you get bad news, you think to yourself “how much worse could it be.” We never thought our hearts could break as many times as it had over the last 3 days. The doctor sat down next to me and said “Hadley had a stroke.” I was lost for words again. I was out of emotions to feel. I didn’t know what to say to her except “that’s awful news” she didn’t reply. She said “I know the word stroke is very scary, and for you and I, it is. But strokes in babies are different because their brains are still developing and can over compensate for the injury.” I asked a few questions, one of them being if she was ever going to wake up. She put her hand on my knee and said “we fully expect her to wake up and I’m so sorry if you thought she wouldn’t!” They said they won’t know the extent of the damage until she actually wakes up. Daniel was of course not with me when they gave me the news. We wait and wait for these doctors to come around and as soon as we need a break and want to go for a walk, they come by. Once the doctor left the room, I immediately tried calling Daniel. I, once again had to deliver bad news to him. I took the elevator down and when I turned the corner he was standing there answering my phone call. I was so out of it, I didn’t even realize I was still trying to dial him. He looked at me and said “what’s wrong?” I gave him the news and we just walked outside to go sit on what we now claim as OUR stoop. We eventually went back upstairs to be with our baby. We talked to her and touched her hands and toes and let her know how much we loved her and missed her and that we couldn’t wait to hold her again. Midnight rolled around and we decided we needed to go home. We needed to be in our own bed. We needed to go home and to take care of our house while Hadley was being taken care of at the hospital. We knew in the coming days, she would be waking up and at this point she was still heavily sedated. We packed up our laundry and few things and made the long trip home. It was weird to be back in our house. It was like we went back in time. We slept in and got a lot of stuff done. But as the day went on, I knew when we got back to Children’s, we would be meeting with the Neurology team and they would be giving us the rest of the story regarding her stroke. We checked in with her nurse several times while we were away and she was still having seizures. They were getting shorter but still happening.
When we made it back to the hospital, the neurologist told us that the injury was to the left side of her brain and it was a blood clot. She too told us that when babies her age have strokes, the brain over compensates for the injury. We asked if it effected her memory and if she would remember us upon waking up and if she would still have those natural reflexes a baby has when eating and sucking. She said that there was no way to be certain at this point but talking to her now and touching her will stimulate her brain so that when she wakes up she has an easier time with those things. I also asked her if she thought she would wake up and she agreed with the other doctor in that they fully expect her to wake up. She would need therapies and early intervention to help her along and help her brain figure out her new normal. She said Children’s has a great team of people that work with babies like Hadley so they thrive. They have 2 concerns at this point:
- Monitor her Heparin dose very closely. She needs it for her heart to prevent another blockage but she can’t have too much and cause a brain bleed.
- Get her seizures under control. Seizures cause stress on the brain which could lead to a brain bleed.
Once her seizures were under control, they would be able to extubate her. The seizure medication that she is on is also used as a sedative so while she’s on such a high dose, they don’t want her to be off the ventilator.
Now you’re all caught up. It is now Sunday July 25th and her last seizure was 2:30pm yesterday and she had an uneventful night. During morning rounds, they said she is doing very well and still no seizures. They are lowering her settings on the ventilator and decreasing some of her other meds. The nurse said all her numbers looked really good and she’s moving around some. Her movements are more on the left side then the right but that’s to be expected considering her stroke. Last night before we left, the nurse let her arms free so we could see the movement and it was triumphant to see her move her right arm above her shoulder and back down. Our girl is such a fighter!