- P
- A

Earlier this year, Leeroy nearly died from a type of Necrotizing Fasciitis (aka flesh eating bacteria) called Fournier’s Gangrene. It's a rare, fast-moving and lethal anaerobic infection underneath the skin.
8 months later, Leeroy and his husband, Vega, are faced with a pile of medical bills, costs for career change training and bills in general. Additionally, a bunch of their bills have gone into collections, including their car! They need your help badly!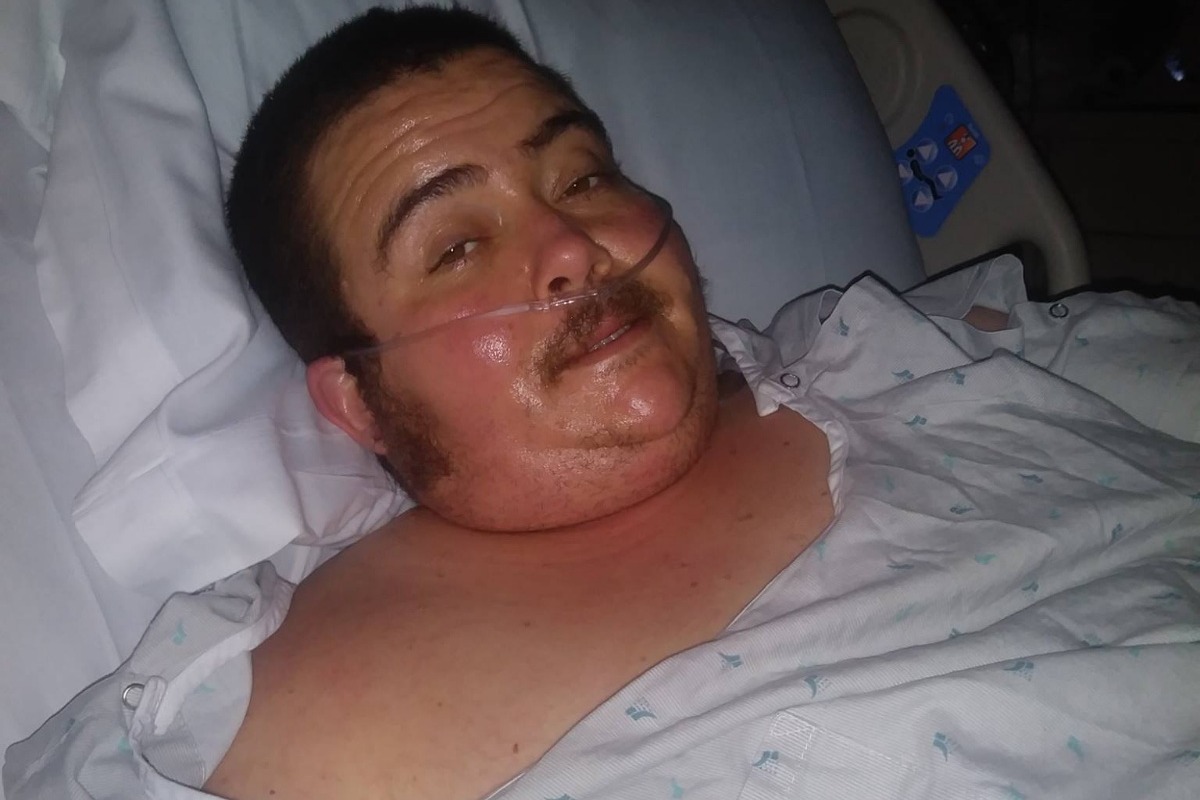
THE STORY
Necrotizing Fasciitis (aka Flesh Eating Bacteria) can infect anyone. Though rare, most everyone carries the bacteria on their skin. It just needs a break in the skin to allow the bacteria into the body to cause a life threatening infection. People with Nec Fasc often start having symptoms within a few hours after an injury. The symptoms may seem like another illness or injury. Some may complain of pain or soreness, similar to that of a “pulled muscle.” The skin may be warm with red or purplish areas of swelling that spread rapidly. Patients often describe their pain as severe and hurting much more than they would expect based on how the wound looks. Later symptoms can include: fatigue, nausea, vomiting, dizziness, fever with chills and sweating.
There are approximately 1200 cases of Nec Fasc in the United States each year.
Without treatment 75% die. With treatment 40% die.
Lucky we caught this just early enough!
On 2/24/18, after a week of severe flu symptoms, Leeroy arrived at Emory University Hospital near death. He was diagnosed with Necrotizing Fasciitis. The infection had reached the edge of the fascia. He had two surgeries, was hospitalized for 12 days, received 3 weeks of IV antibiotics, and was attached to machines for a month. The surgeries to remove infection left a 22 inch long, 2 inch deep wound along the perimeter of his upper thigh. He’s lucky to have his leg, and his life. 
Leeroy's health care team at Emory estimated 5-6 surgeries, 2-3 weeks of hospitalization, and 3-4 months of recovery. Leeroy's husband, Vega, became his full-time caretaker and had to step away from contracted freelance jobs. Vega became very sick and was diagnosed with multiple autoimmune conditions including Type II Diabetes and Psoriatic Arthritis. Leeroy and Vega have had to financially rely heavily on help from one family member, who is very strained by the added expenses. Leeroy’s body is still healing 8 months out from surgery. He has limited mobility and his wound still breaks open regularly.
Insurance covered 80% of the hospitalization. Leeroy has also required Urgent Care, ER visits, Home Nursing Care, Surgical and Wound Care appointments, durable medical equipment, medications, home safety needs, etc. All of which have co-pays or out of pocket costs. These are the hidden costs of getting sick. Leeroy's ER visit, inpatient hospital stay and surgeries Emory University Hospital were initially billed at $81,054.27 before insurance is processed.
Leeroy’s total outstanding out-of-pocket costs for medical care are down to $5000.
TIMELINE
2/16/18 First symptoms. Painful sore, flu-ish. Last day worked.
2/17/18 Fever, chills, nausea. Called out of work.
2/18/18 - 2/23/18 Fever, chills, nausea, vomiting, diarrhea, migraine.
2/24/18 New symptom - redness running down left thigh. Examined at Urgent Care. Sent to ER with “possible NEC.” Triaged in less than 3 minutes. Examined by ER doctor, OB/GYN, surgeon. CT scan, blood tests, X-ray, IV antibiotics, IV fluids. CT scan showed air under the skin which is caused by the bacteria. Diagnosed with necrotizing fasciitis aka flesh eating bacteria and the onset of liver failure. Told he would be in the hospital for 3 weeks, 5-6 surgeries, months of recovery. Sent to first surgery. 5 hours later Leeroy came out of surgery with a 22 inch long, 2 inch deep wound along the perimeter of his thigh and groin to remove necrotic tissue. Lots of visits by teams of doctors from surgery, infectious disease, gyn, etc. Told by doctors that if he would have arrived just 8 hours later he would have died. Admitted to ICU.
2/26/18 Second surgery. 2 hour duration. Successfully removed all necrotic tissue.
2/27/18 Moved from ICU to post surgical ward. Starts telling everyone his left thigh is “swimsuit ready.”
2/28/18 Leeroy's first wound dressing change. He reports that the process of removing the “Drape” (medical tape) is one of the most painful things ever.
3/1/18 Wound dressing changed to wound vac. Leeroy reports this is more comfortable. New experience of being attached to a portable machine that’s attached to your wound.
3/2/18 Out of bed for first time since 2/24. Walked a bit up and down the hallway, sat up in a chair for a few hours. Began to transition to oral pain medications. Had catheter removed. Still has migraine. Can’t read or think.
3/5/18 Migraine is finally gone.
3/7/18 Discharged.
3/9/18 Home nurse was not able to get a seal with the wound vac dressing after 4 hours of trying. Leeroy had to return to the ER for dressing change. 10 hours of wound torture.
3/10/18 Home nurse visit. Found out Leeroy is missing prescriptions including antibiotics.
3/12/18 First shower (with assistance) since surgery. Dressing changed successfully with two nurses at home. Extremely painful. ER applied foam directly to the skin causing more damage to healthy tissue.
3/15/18 Follow up with Emory surgical clinic. PICC line removed!
3/20/18 Discontinued use of wound vac two weeks early due to some medical hiccups with dressing changes. No longer hooked up to any machines! Estimated minimum healing time is 10 more weeks.
7/15/18 Still have open wounds. Diagnosed as pre-diabetic and learned that the elevated blood sugar levels affect healing time.
8/23/18: Emory wound care appointment. Given silver gel to apply to wound area.
9/7/18: Leeroy’s first bath since illness.
9/24/18: Several inches of Leeroy’s skin continues to split open and bleed, taking days to heal. His skin lacks flexibility and his mobility is still limited.
10/13/18: Still dealing with weak skin that keeps breaking open.
FROM LEEROY
Okay, so I didn’t die. What am I facing now? A slow healing process, with no way for me to work just yet. I still suffer from some profound issues tied to this medical emergency. My mobility is limited. I cannot bend, crouch, or walk more than a few minutes without possibly tearing my skin. Sitting is often painful due to the location of the wound. My leg does not bend well, the scar tissue and wound limit range of motion, and I have nerve damage to my thigh. I still need to use a cane or walker at times, and wheelchair or motorized cart for shopping. I have to keep my wound dry or risk skin damage or tearing at the wound site. Seven months later, wound care is still the main focus of my days.
My memory is shot. It simply isn’t working right now. I ask the same questions many times, and I cannot retain the answer given. Before this illness, my memory was good and I could remember things. Today, I cannot say the same thing. I’m exhausted. All. The. Time. My severe childhood stutter has returned, as well as an inability to remember words or be able to speak as I did before. The doctors believe that there are multiple reasons for these issues. Number one is the sustained high-fever I ran for over 7 days. This could have caused brain damage. Number two is the toxins from the infection. The brain oftentimes gets scrambled by all the waste products which are super toxic. Add to that, my liver’s function was not good resulting in my body having a large amount of toxic waste matter with slowed filtration.
I cannot return to my previous job as a server at a fine dining restaurant because my body and mind have not healed, and my mobility is limited. I have decided to change career directions and train to be a Phlebotomy Technician. The cost of training is $905.
In addition, I have two additional serious, chronic infections -- a pilonidal cyst near my tail bone and hidradenitis suppurativa which is related to several autoimmune conditions. I am being treated with a 4 month round of hardcore antibiotics and a topical antibiotic. Hopefully I will not require surgery to remove these infections.
I was diagnosed in July with pre-diabetes. High blood sugar slows healing and encourages infection. I am taking my pre-diabetic nutritional needs very seriously. I am attending workshops on pre-diabetes and diabetes and have a nutritionist as part of my care team. I have adjusted my diet and eating schedule to optimize my healing and reduce blood glucose. I am on a higher protein diet to encourage tissue healing and to lessen muscle loss. My diet is mostly whole foods, plant based and lean proteins. I will be able to start Physical Therapy soon to regain some strength I have lost recuperating for the past seven months.
I cracked a couple teeth while in the hospital. This brought me into the dentist with extreme pain. I have started the course of treatment and had several teeth extracted to alleviate the immediate pain and discomfort. I will need two root canals, two bridges, a crown, a couple fillings and treatment for early periodontal disease. My estimated dental bills are $8,500 out-of-pocket with dental insurance.
This experience was very traumatic. I mean, I almost died! I was assaulted by a doctor at the hospital. I have been in pain for 7 months. I'm suffering from classic PTSD symptoms. I find myself zoning out often. I get trapped in my trauma. I have anxiety attacks. My body overreacts to touch near the wound site. I have started seeing a therapist to help me with the tools to move beyond this trauma.
Today, we have a BUNCH of bills that have entered collections, including:
Emory University: $2000
Kaiser $1800
And now our car is in danger of being REPOSSESSED.
I believe in the power of commUNITY. My family is so close to what we need to be safe, healthy, and financially stable again. I have so much more life to live and so much more work to do for the community. Please help me reach these goals. Donate. Share on Social Media. Contact Media. Send encouraging messages. <3




*A previous YouCaring campaign organized by Leeroy's friends has been added to the current funding total.
Co-organizers5
Vega Darling
Beneficiary

