- L
- J
Hello!
My name is Sammantha Trias, a 24-year-old aspiring elementary school teacher! I was on my way to start a Master's in Teaching after being accepted to UC Davis' teaching credential program, but on April 11th 2023, I received a call from my doctor that... I have cancer. It all started with a swollen lymph node in my groin and an increasing fatigue. It took a while to schedule appointments just to biopsy the lymph node, but after plenty of tests and scans, we found out that I had stage 4 T-cell lymphoblastic lymphoma/leukemia. Cancerous lymph nodes were found in my mediastinal mass and below my waist. My first bone marrow biopsy also concluded that I had low bone marrow involvement.
There's no way to fully describe how much a cancer diagnosis changes a life. For the first month after getting my diagnosis, I cried every morning and night because I couldn't stand facing the reality of my own mortality. The very real possibility that I could pass away in my twenties terrified me. The google search results for my diagnosis didn't ease my fears in the slightest. My career in education came to a halt and suddenly my dreams of a having family were at risk since treatment could affect my fertility. The weight I felt I put on my loved ones was unbearable. I had no idea what the future looked like for me, and it was horrifying.
[The story so far]
After meeting with my oncologist, she determined that I would start a 2+ year pediatric chemotherapy regimen based on the CALGB10403 protocol for T-ALL patients. The first part of the regimen, called "induction," involved a month long stay at the hospital while they treated me with intensive chemo. On May 9th, 2023, I underwent port surgery (an implant into my chest that connects directly to my vein for easier chemo infusions) and immediately started my treatment.
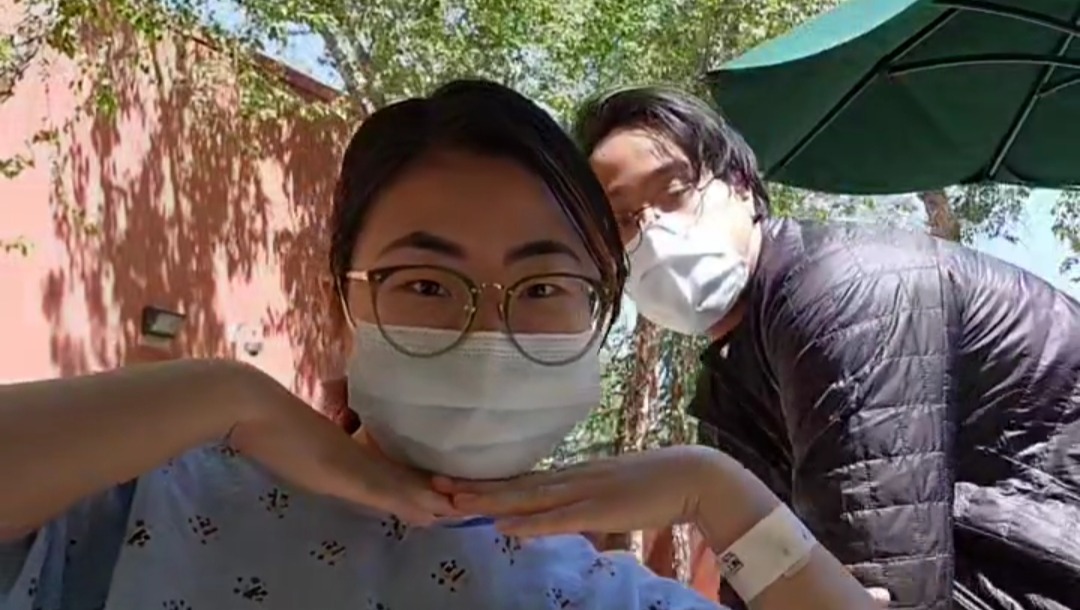
For the first half of the month, I kept a strong spirit. I'm endlessly grateful to my mother and my boyfriend for spending every day with me in that small hospital room. I had lots of supportive family members visit as well. The first two weeks were a blur because the chemo made me too weak to do anything. I tried to bring entertainment, but even just lifting my arm felt exhausting, so most of the time I just sat and stared at the room for hours. By the halfway mark, the stay was taking a toll on my mental health. The inpatient room I stayed in was small with covered windows because of construction. The bathroom felt like a storage room and the only place I could walk was the dim, windowless inpatient oncology floor. If I wanted to be outside, I only had a small, walled up courtyard to sit in. Hospital food was nauseating. Being woken up in the middle of the night for daily blood tests was exhausting. If I couldn't sleep, I was looking up my diagnosis. On top of all that, I faced many complications, the most critical being a developed adrenal insufficiency. My body was not responding to the stress as it should have been, and this caused my blood sugar to often drop to the 40s, so I was constantly being checked, even at the late hours of 3am. Because of my adrenal insufficiency, I have to take three doses of hydrocortisone every day.
By the last week of my inpatient stay, I wanted to go home more than anything in the world. Finally, after an excruciatingly tough month, I was able to go home on June 7th. They did another bone marrow biopsy and found no bone marrow involvement anymore! Scans looked good as well, yay! Once I got back home, I barely had enough strength to do anything. My muscles deteriorated so much that I could barely pick myself up from the floor or walk a block. It was hard going from a strong, energetic girl to someone who needed help standing up. I shaved my head because the hair loss was getting crazy (I kept my brows and lashes surprisingly!), and I gained weight because of the steroids. My appearance changed so quickly, and it was hard to recognize the person I'd stare at in the mirror.
My oncologist had told me that induction was the "hard part," but little did I know that was far from the truth. The next part of my treatment plan was "consolidation," which included weekly outpatient chemo appointments, intrathecal (spinal) chemo, at-home chemo where I have to give myself subcutaneous chemo shots, and daily chemo pills. My family and I were all so new to this, and everything worried us. I didn't know how to work with the side-effects, and ended up feeling sick throughout most of the course. I lost a lot of my appetite as well, which didn't help the cause. We went to the ER often because of my severely low white blood cell, red blood cell, or platelet counts. Despite the struggles, I still enjoyed the days I didn't feel awful.
After consolidation, I began "interim maintenance." During this course, I experienced a lot more hardship.
In my treatment plan, there is a chemotherapy drug called "pegaspargase." This drug is a leading difference between pediatric and adult chemotherapy protocols, and is seen as an important chemo to better prevent relapse rates. In terms of side-effects, it is a very nasty drug, but I viewed it as immensely important. I had two full doses until things went south. During one pegaspargase infusion, I started to flush and swell up. The nurses immediately stopped my infusion, but my oncologist wanted to challenge the rest of the dose. After getting the rest of the dose, I was faced with two weeks of chemo-induced gastritis. My stomach was in constant pain and I vomited everything I ate. I could only eat chicken broth and saltine crackers, which were still hard to keep down. It took a long time to recover.
The last time I received my pegaspargase infusion was the worst. Within four minutes of the infusion, I started to get flushed, my chest started hurting, and I was vomiting. I was also in a state of panic from the pain. The nurses rushed to give me steroids and oxygen. Pegaspargase is known to cause allergic reactions-- to the point of anaphylaxis. Thankfully, I was still able to breathe during my reaction, but since then my oncologist and I decided that we will omit pegaspargase from my treatment plan.
This decision was tolling on me. I had even tried a substitute chemo for pegaspargase, but my body was not tolerating it. I felt that I had thrown away my chances at preventing relapse. I broke down to my oncologist, but she comforted me, letting me know that sometimes we need to stray "from the book" to find a treatment plan that works best for me. Since then, I haven't been stressing about pegaspargase as much, and have been enjoying going through treatment without it's painful side effects.
It's been a long 9 months of treatment with plenty of setbacks and dark moments. I developed a lot of PTSD and medical trauma from my infusions, and now I take Ativan whenever I go to an infusion to help with the fears (especially with intrathecal chemo). Unfortunately, I had to miss Thanksgiving with my family due to severe post-spinal headaches and daily vomiting from a bad intrathecal chemo procedure. However, my oncologist gave me the whole month of December off because she felt I needed a break! I spent the whole month feeling "normal" again, and I enjoyed every second of it. It was nice to eat and do what I want without worry.


My last scans and bloodwork were in October, in which my oncologist told me everything looks good! She doesn't use the word "remission" because she explained that there's no real way to say with 100% certainty that the cancer is gone from my blood, but my swollen lymph nodes disappeared and my blood work detects no cancer cells, so I'm comforted every day knowing that. Through this whole journey I've learned to enjoy the moment while I can, and not stress too much about my fears. I still need to follow my two year chemo plan, and since the beginning of January 2024, I am currently in phase 4/5: delayed intensification! The chemo hit me pretty hard, but I'm staying stronger than I was in my previous phases! I'm very proud that I got here. During this phase I will be doing at-home chemo shots, chemo pills, and outpatient infusions again. Unfortunately, my hair is falling out again due to the "red devil," but that's what wigs are for!
Before my diagnosis, I was the only working person in my family and helped my mother with any bills. I've been very thankful to be on medical leave, but will unfortunately exhaust leave as of January 2024. This will require me to change my insurance, which I'm not too excited about. Treatment still prevents me from being able to work, so I wanted to reach out and ask for support in my fight against cancer and related expenses.
I will try to update this page as much as possible. Thank you for taking the time to read my story!
Love, Sam