- J
On Tuesday morning 24th of May I rushed my daughter Talia down to a private hospital in London from Wolverhampton in order to save her life. It is unfortunate that the NHS was unable to provide the care Talia desperately needed, which gave me no alternative but to seek help from a Gastroenterologist in London.
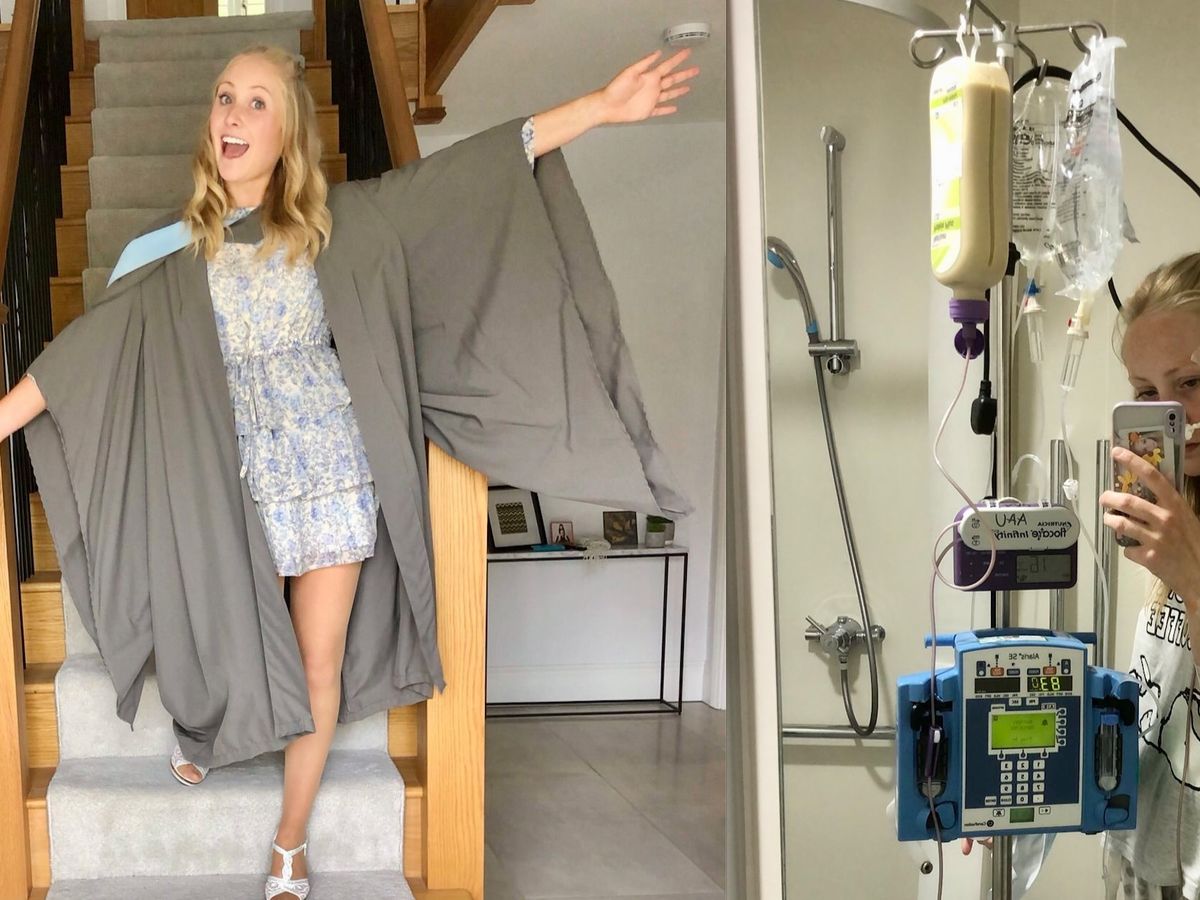
On arrival at the HCA Wellington Hospital in St Johns Wood she was met by a team of nurses and doctors and within hours was receiving emergency treatment, including six intravenous drips, a PICC line direct to an artery to the heart, and a feeding tube to her small intestine.
Talia is facing a life-changing battle after being diagnosed with Hypermobility (Ehlers-Danlos Syndrome) and Gastroparesis. Gastroparesis is a long-term chronic condition where the stomach cannot empty in the normal way. Food passes through the stomach slower than usual. It's thought to be the result of a problem with the nerves and muscles that control how the stomach empties. For further information please see: Gastroparesis
Talia was, until just after Christmas, a healthy and happy 24-year-old who was enjoying the first year of her Doctorate course at Hull University as a Trainee Clinical Psychologist. The photo at the top of this page shows Talia celebrating her graduation from York University last August where she gained a BSc in Psychology.
Talia has been suffering from a mild form of Gastroparesis for several years, which would manifest in episodes lasting a few weeks. She was able to manage the condition by eating smaller meals more frequently. Although she underwent some clinical tests, no-one had actually diagnosed the problem.
Unfortunately, a few days after Christmas and before she was due to return from home in Wolverhampton to Hull, Talia was struck down by an unknown and undiagnosed virus. This triggered another episode of what we assumed to be Gastroparesis, which left Talia in excruciating pain every time she ate or drank. She would be sick up to 10 times every time she attempted to eat.
It’s now over 5 months from the start of the flare-up and Talia has lost 2-stone in weight and is unable to tolerate any food other than digestive biscuits and the odd rice pudding. She has remained in Wolverhampton unable to re-join her course in Hull.
From our research into Gastroparesis, we discovered that it is a poorly understood illness and many sufferers are diagnosed as having a mental illness or an eating disorder. It is a life-changing illness and can be fatal without the right treatment. There is no cure, but there are some options that may improve a person’s outlook.
Talia was referred to a local Gastroenterologist in February who prescribed a series of five tests to confirm a diagnosis of Gastroparesis. The second test clearly showed that her digestive system was not functioning normally, however, the specialist declared she should be referred to an eating disorders clinic for an assessment before any further tests. We were shocked, to say the least, and immediately sought a second opinion.
Thankfully, after a lot of research, we found a specialist in London who operates the only Gastroparesis clinic in the UK and who has successfully diagnosed and treated patients from around the world. Talia had a consultation with him in April and he immediately diagnosed Hypermobility (Ehlers-Danlos Syndrome) and Gastroparesis. He outlined a pathway of treatment and arranged a gastro emptying study prior to starting treatment.
Unfortunately, the day before Talia was scheduled to go to The Princess Grace Hospital in London for the gastro emptying study on 24th May, she became very ill. An ambulance was called but there was a wait of 4-5 hours, so I took her to our local A&E only to be told it would be 7 hours before she could see a doctor, and it was now 2.00am in the morning. We returned home and called our GP as soon as the surgery opened at 8.00am for an immediate appointment but he told us to go to A&E.
At this point, I was fearful for Talia’s life and had no option other than to call her specialist in London. He arranged for her to be admitted to the Wellington Hospital in St Johns Wood for a 2-week stay. I immediately drove Talia, who was in great pain and discomfort, to London where nurses and doctors were waiting on our arrival.
Within hours Talia was receiving life-saving treatment with intravenous drips administering calcium, potassium, magnesium, phosphate and glucose. A ‘PICC’ line was inserted to provide access to the large central veins near the heart, and two tubes were inserted – one into her stomach to drain hydrochloric acid and the other directly into the small intestine to provide nourishment.
To enable this level of care and to save Talia’s life it has already cost £37,524 in hospital fees.
When Talia’s medical team is happy to release her from the hospital, she will return home with a feeding tube directly into her small intestine bypassing the stomach until she is strong enough to continue with the pathway of urgent treatment.
The urgent treatment includes several processes and depending on the level of success may lead to an implant of a Gastric Neurostimulator, which is similar to a heart pacemaker. The NHS will not fund this treatment, which means without it, Talia would have to be tube fed for the rest of her life, never being able to eat normally again.
The Neurostimulator is a small electronic device that is positioned under the rib cage and has two electrodes that send electrical pulses to the stomach muscles to stimulate the digestive process. Please see the following for further information: Neurostimulator
This treatment will cost upwards of £45,000 and that is why we are reaching out to our friends, colleagues and clients in the hope that they may wish to make a donation.
Talia has only one goal in life and that is to become a Clinical Psychologist so she can help and support young people with acute eating disorders, who are sadly slipping through the net because of underfunding and scarce NHS resources.
We thank you in advance for your support which we will always be most grateful for.
Any funds that are not used will go towards setting up a charity and foundation to support research and funding for other Gastroparesis sufferers.