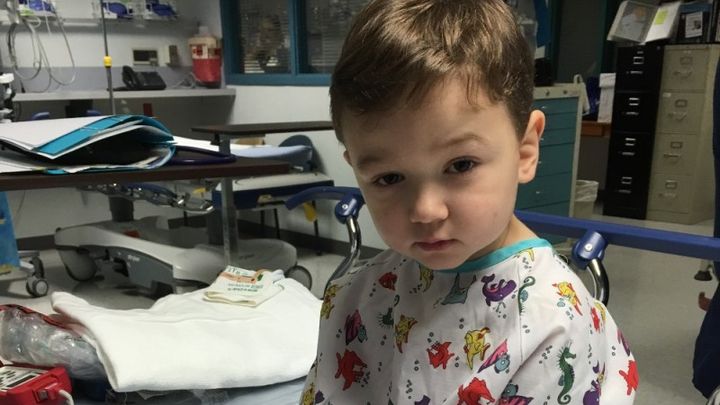
Love for Noah
Donation protected
Our son Noah was diagnosed with acute lymphoblastic leukemia (ALL) just days before his first birthday in December of 2011. Since then, he's been having the fight of his life. Nearly 3.5 years later Noah was scheduled to end treatment after a long (and seemingly successful) battle.
Unfortunately we just learned that Noah has relapsed and his leukemia has returned, just in the past few weeks. The relapse is in his central nervous system and will require immediate reinduction therapy along with specific chemotherapy AND radiation treatment to the nervous system and brain. There are risks of severe side effects with this treatment, but without it, he cannot win.
We are all in shock but we are doing everything we can to prepare Noah for another long battle and make sure he is in the best position to win. It's heartbreaking that just months after he was allowed to finally go back to school and do all the activities he's been waiting to do for years, he must go back into therapy. All the progress and treatment over the past 3.5 years starts all over again. More intensive and more dangerous.
First and foremost, we are asking for your prayers, positive thoughts, well wishes, anything. That is the most important thing!
We are starting this fundraiser to help with some of the costs involved in this very long process. We are still working to pay off the debts from Noah's first round of treatment as well. Cancer, especially leukemia that has such a long treatment cycle (years), is very expensive. While insurance will cover a big portion, there are several treatments deemed "experimental" which are not covered, in addition to sometimes 3-5 co-pays per week, plus specialized care, and anything to keep him happy and positive.
Any donation is deeply appreciated and will be put directly towards Noah's medical expenses and any specialized treatment we can get. I would be forever grateful, even if all you can give is a prayer or positive thought.
We will get him through this -- again! Thank you so much for your love and support!
Regards,
The Keck Family
Unfortunately we just learned that Noah has relapsed and his leukemia has returned, just in the past few weeks. The relapse is in his central nervous system and will require immediate reinduction therapy along with specific chemotherapy AND radiation treatment to the nervous system and brain. There are risks of severe side effects with this treatment, but without it, he cannot win.
We are all in shock but we are doing everything we can to prepare Noah for another long battle and make sure he is in the best position to win. It's heartbreaking that just months after he was allowed to finally go back to school and do all the activities he's been waiting to do for years, he must go back into therapy. All the progress and treatment over the past 3.5 years starts all over again. More intensive and more dangerous.
First and foremost, we are asking for your prayers, positive thoughts, well wishes, anything. That is the most important thing!
We are starting this fundraiser to help with some of the costs involved in this very long process. We are still working to pay off the debts from Noah's first round of treatment as well. Cancer, especially leukemia that has such a long treatment cycle (years), is very expensive. While insurance will cover a big portion, there are several treatments deemed "experimental" which are not covered, in addition to sometimes 3-5 co-pays per week, plus specialized care, and anything to keep him happy and positive.
Any donation is deeply appreciated and will be put directly towards Noah's medical expenses and any specialized treatment we can get. I would be forever grateful, even if all you can give is a prayer or positive thought.
We will get him through this -- again! Thank you so much for your love and support!
Regards,
The Keck Family
Organizer
Chad Keck
Organizer
San Antonio, TX


