- D
- D
- A
I want to thank everyone who has contributed and shared the post.
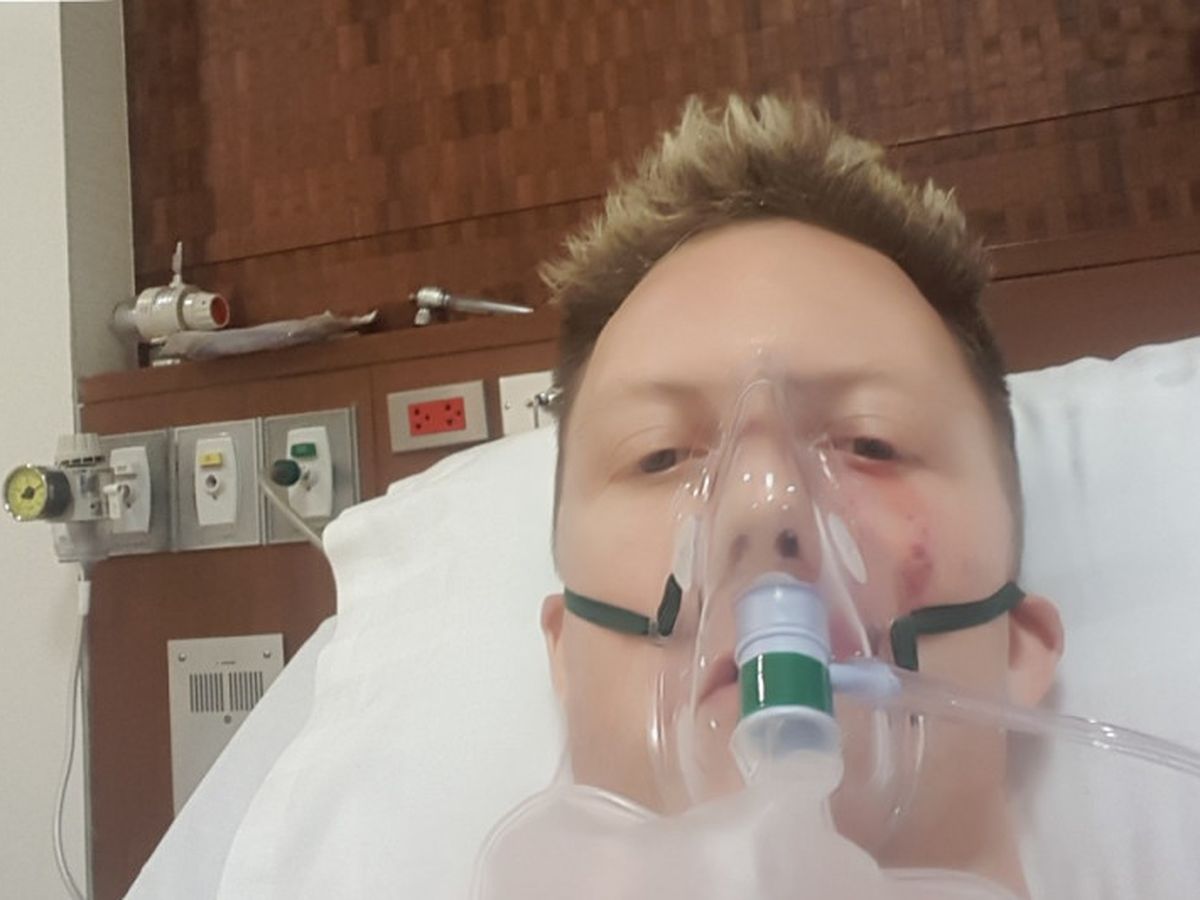
Tony needs your help. He has recently had a medical emergency and undergone 4 surgeries in a week. He devoted his life to helping others, especially children. He has already incurred a lot of out of pocket expenses and complications keep arising. Help Tony in his journey to wellness. Any donation helps and is greatly appreciated. Thank you.
Help spread the word
Below is a letter from Tony written by him when this emergency first occurred:
Hello everybody,
I am updating those who know and informing those who don’t yet, so all ya’ll understand what’s happening, what’s next, and what may be.
Around 1am Sunday (was it Sunday, maybe Sat?), Thai time, I choked on some chicken at home in Jomtien, Pattaya. I am no stranger to this and have learned to choose my food carefully and chew with zest. However, I do have a variety of issue with food as most of you already know. Usually I can fend of an attack on my own or at least know what to expect and how to react/get help.
This time was different.
This time, a burning sensation beyond what I have experienced before started before any real struggle took place. I do not even remember fighting it this time for more than one heave or so. It felt as though the food dropped lower and got stuck in a new place, far away from anything important for breathing. It was a sigh of relief, but also super stuck at the same time.
After about 10 minutes I become worried enough to knock on the neighbors door on the floor below to ask to be observe for about 30 minutes while this passed. Within 10 minutes or so of talking with her, I asked we call an ambulance and that she come with me. Neither of us speak Thai well enough for this.
She looked ahead for security in the lobby and parking area, while I struggled to keep up. Oddly, no one was working that night. Very strange. She crossed the road to talk to a motorcycle taxi driver to get assistance to ensure we got the right ambulance. While she was doing this, I saw a kind looking guy walk down the street and waved him over (her as it turns out to clarify for those who don’t know Thailand very well). I gave her 100 baht and asked she run to 7-11 to buy some cold water to help cool me down. By the time she came back, I was hanging off a gate and couple barely lift an arm to grab it. I was loosing the ability to breath and keep conscious. But not from an obstructed airway.
She offered to drive us to the hospital, but by that time the ambulance came around the corner. She and my neighbor followed in her car.
Every single tiny bump in the road was absolutely excruciating. By the time we arrived, I was quickly getting worse. The pain became unbearable and I could not longer take a full breath, lay back, or sit still very long. The hospital staff informed us that because I had food in the stomach, they would not be able to operate until 10 or 11 am. That was going to be too late, but they kept insisting. This has happen to point of operation before (although not this badly) and the OP was done on the spot without delay. The risk of vomiting during the OP far outweighed the risk of waiting.
After quite a bit of pleading and persistence from my two friends, they finally agreed to do the operation now (5am by now), but only if I cam up with 50,000 baht ($2000CAD) deposit for hospital admittance first. On the spot, I could not do this. Sounds crazy, but that’s the way the world works. My friends contacted my cousin’s, one of which was on her wedding day of all things! They got the ball rolling while I was incapacitated.
Please don’t reply to me with the obvious ‘you should have bough insurance’ advise here – I know this and didn’t have it.
There are far more important issues to address, as I will get into below:
The Dr found during surgery that I had torn the esophagus. I’m not sure when this happened exactly, but I’m sure it became worse during the hours of extreme heaving while waiting for the OP and bouncing around the ambulance for 20 mins. The tear is about 10cm long and very wide, it’s not small by any means. I am extremely lucky that only a smaller portion of that actually went all the way through.
A laceration like this is a big problem. When it perforates the wall, it’s a bigger problem and becomes life threatening.
There is a 20-30% mortality rate for people who have this condition.
This is not a typo or exaggeration, this comes directly from the Dr. The level of my situation is severe, it is not a tiny hole.
Most of the time it’s the complications that get you, which I have plenty of. More on that later.
A second operation, the day involved covering the laceration with a stent delivered from Bangkok. This meant an additional delay of about 10 hours before the perforation was covered an no longer seeping air into the chest cavity. This air puts pressure on organs and can cause the type of fatal complications you could probably imagine. It’s common to affect the lungs, and other things as well.
An X-Ray of the stent of Day 2 & 3 showed it slowly moving downward towards the stomach. They are designed this way because at some point they need to be removed, which until this afternoon was going to be my 3rd scheduled operation 3-4 weeks from now if all went well. Although it was slipping, it was still covering the perforation.
Today a CT scan showed the entire stent in a ball inside my stomach, doing no good. This brings us back to emergency stage #1. Air seeping into the chest cavity, as well as bacteria which causes nearly 50% of fatalities in these cases.
This means a critical operation tomorrow morning (about 9 hours from sending this out) to pull the stent back up to where it should be, so it covers the perforation. This time the Dr is going to try to clip it into place and also glue the perforation shut.
If you’re not sure what a stent is in this case, it’s basically a plastic membrane tube lined with expandable (springy) metal mesh that forces itself into place against the esophageal wall – protecting it from foreign contact and allowing the tear to heal. If it’s too tight, it the healing tissue may attach itself to the stent and cause it to become permanent… which is a whole new set of problems.
As you may start to be understanding, there are many different types of complications with this issue and because it is so rare there aren’t any Dr’s who have had a need to study it, let alone have experience.
This brings us to where things are now:
Even had the stent stayed where it should be, there are a couple important complications.
Air seeping through the esophagus into the chest cavity has build up enough to cause pain with deep breaths and is very apparent when you lightly press against the pectoral area. The skin feels spongy and you can feel hundreds of bubbles. Left alone, this was expected to clear itself as it was a relatively low amount due to the stent placement within the first 24 hours. The Dr suggested we give it a couple weeks if there was no associated pain or increase with other symptoms.
Bacteria seeping the same. This can cause an infection within the chest cavity and lungs.. which it has. The lung infection seems to be a little better with each passing day (antibiotic drip), however there is a ‘patch’ of infection growing underneath the lower left pectoral.
The combination of these two, along with the now released stent has turned this into an emergency situation again.
(Please read this with a level head and remain calm, I need extra emotional friends to be relaxed and logical at this point. Need support, not to become emotional or depressed myself. I NEED to be strong and focus all my strength on the solution)
The Dr has told me that without continued treatment, I am not going to survive with the condition as is. Despite all current efforts my health is declining with complications.
** Please keep this in mind when I ask for your collective help at the end **
Continuing treatment my chances are as I mentioned before. 20-30% mortality rate. Each new complication disfavourably increases those odds.
If left untreated, I will succumb to infection.
The next Steps:
Scenario 1
The 3rd OP tomorrow as mentioned is to replace the stent. Once that is done, it is a waiting game until the next complication shows it’s face or an existing one does not show signs of healing. Best case scenario, I go home 3-4 days after and return for a checkup every 2-3 days to see where the stent is sitting, check infection and trapped air levels. In a perfect world, the body will heal itself with the help of modern medicine and some love from friends and family.
Scenario 2
The stent holds, but the current pocket of infection required draining. This means a chest tube and more antibiotics. Back to the hospital for awhile.
This scenario also includes the trapped air issue, if the body does not naturally absorb it, it may need to be released. Probably not as bad as it sounds.
Scenario 3
The stent dislodges again. If this happens, things get a little more serious. There are more extreme options for suturing the laceration. The lowest mortality rate comes from instances where a conservative approach can be used, such as mine. Although the laceration is actually quite huge, the perforation is manageable. If the entire laceration was also a perforation, I may be writing a different type of letter.
The hell of living the current situation and my request to the Dr.
I woke up from the first OP on a breathing tube and a team of people hovering above. What woke me up? I could not breath. The shock of waking up to that is one thing, but another is that I could not breath out due to a lung infection clogging the air tube. Panic set in.
Panic turned into what I thought were my last breaths of life. In my mind, I was going to die by suffocating on my own spit. I sat up, flailed a bit and tried to show them with my hand I needed to write down what was happening so they could fix it. They thought I wanted to rip the tube out and strapped me down to the bed, that made the panic worse so after strapping y hands and legs, they tied down a ‘pycho’ sheet to keep e more snug and let me fight the mucus. They did not know I was drowning in phlem.
A very hard last ditch exhale dislodged the mucus into the tube and I was OK for a little while. It quickly built up aver and over requiring multiple similar experiences. I continually made a writing gesture with my hand to show I wanted to write on paper, they did not understand and told me ‘NO’. They thought I was going to rip the tube out or fight them. At times being cheeky as well and laughing to themselves. It was an absolute nightmare like torture. After 3-4 hours when the Dr finally came to update me, he explained the handcuffs and I showed him my writing gesture. He allowed me to write, and instructed the staff to let me go.
I had this reaction probably 5-6 times during the final 30 minutes and honestly did no think I could keep it up much longer. I felt lucky the Dr finally came. They gave me one hand to allow me to suction my own mouth and the other after some time later.
NOTE: My very clear request to the Dr in a private talk tonight was to not wake me up if that is the scenario again. I asked him to keep me asleep until after they are able to safely remove any life support machines. I don’t mind the machine or even a coma if need be to keep the body still a couple weeks. But I do not want to live that hell ever again.
Moving forward & why I wrote everyone in one big batch
Obviously there is a lot to explain. It would be impossible to explain pertinent information to everyone individually and then reply to each several times to answer questions. Need to get the message out those who need to know or may be able to assist in some fashion, and then I need to refocus on making sure the next step is the best it can be.
This may be too much information for some, too family oriented for others, and too impersonal for some as well. It’s simply a bulk “What’s up” update for all.
How you can help!
1. Research
– I need help finding the best possible Doctor.
If you live in Pattaya (or Thailand actually), it would be great to learn of Doctor who specialize in esophageal perforation repair. My current Dr claims to have two previous cases. Both were successful. I do not know the details. The GI in Vancouver who did my colonoscopy a couple years ago has done more than 10,000. See where I’m going with this?
I am not fit for travel. Perhaps if stabilized could make it to Bangkok, but would need to ask. Flights are out of the question due to the trapped air pressure and trauma of movement to the laceration.
2. Immediate Need for Funds
My cousins have pledged to assist with initial hospital fees, which are already far more than anyone expected from day one. Today, the Dr explained various paths that complications may take treatment and unfortunately it may include a month or two in hospital trying to exhaust all efforts. Best case, they clear me by the end of the week. I doubt this though as the infection is growing even though I have been under multiple antibiotics as a precaution the moment I came out of the first OP. A very rough guesstimate is that we are only 1/3 – 1/2 done the way it looks at the moment.
That means I need to plan to raise up to another $40kCAD
Saving money is the easiest way to earn money, however it can also be dangerous in my case.. which is why I put Research as the #1 at the moment.
I made a bad investment last year and have been putting my extra money into building a small but now successful little business. I have used what I have left and now need help, there’s no way around it.
I am in a private hospital, with the best Dr’s Pattaya has. As you can see, it does not mean they also have much experience with this condition. They do have public hospitals. The downside to those are many more customers per patient and lower standards & equipment due to lack of funding.
Although better than no treatment, the inherent risks make this critical situation even more so than it already is. The hospital here is great for it’s local, but lacks in some very basic service details that can be downright scary when you consider what may be missed in the bigger picture as well. Going to a public hospital is an absolute last resort.
3. If you can thinking of any other way to pitch than what I’ve mentioned, please do!
I need great organizers (in case I need to do a crowdfund),People with friends that have friends in Thai medical land, People who can help with a donation or two, People who can simply send their best positive energy if nothing else!
Please message me on FB, or whatever media you have. Tomorrow is supposed to be a light OP, so I should be awake later in the afternoon (Thai time) to check messages. Unless someone screwy goes on, I should have at least 2-3 more days before the next potential complication is expected.
Thank you all very much for reading this incredibly long explanation. I’ve a few people reach out to me who have heard of a bad situation and wanted to learn more. As I mentioned, I just can’t explain it all to everyone without doing it this way, plus I’m a geek so this is actually easier than it might seem, lol
<3
----------
July 30th Update:
Thank you all who have been watching this.
The stent did not hold as hoped, it's off to the OR again tomorrow. Thankfully, this is a fairly minor procedure to remove. The Dr will not try a 3rd time. He did manage to glue to hole during the last stent relocation, so hopefully it is still holding. Will know more in the next few days when they do a CT to check for leaking.
This translates to: I'm stable for the moment. However, now I have heart complications. Joy...
The good part it also means I can now look to transfer to a new hospital, with lower costs and a fresh set of Dr eyes (and experience) to look at the situation. I feel the current Dr has done what he can and is taking some very serious risks to save a few baht that I would never considering the consequences. Thailand is a beautiful country. Insurance or not – you do NOT want to get stuck here with a medical emergency. The experience, service and facilities just doesn't compare to what we are accustomed to back home. I have heard stories of expats losing their lives due to 'common' issues we have back home.
Tony needs your help. He has recently had a medical emergency and undergone 4 surgeries in a week. He devoted his life to helping others, especially children. He has already incurred a lot of out of pocket expenses and complications keep arising. Help Tony in his journey to wellness. Any donation helps and is greatly appreciated. Thank you.
Help spread the word
Below is a letter from Tony written by him when this emergency first occurred:
Hello everybody,
I am updating those who know and informing those who don’t yet, so all ya’ll understand what’s happening, what’s next, and what may be.
Around 1am Sunday (was it Sunday, maybe Sat?), Thai time, I choked on some chicken at home in Jomtien, Pattaya. I am no stranger to this and have learned to choose my food carefully and chew with zest. However, I do have a variety of issue with food as most of you already know. Usually I can fend of an attack on my own or at least know what to expect and how to react/get help.
This time was different.
This time, a burning sensation beyond what I have experienced before started before any real struggle took place. I do not even remember fighting it this time for more than one heave or so. It felt as though the food dropped lower and got stuck in a new place, far away from anything important for breathing. It was a sigh of relief, but also super stuck at the same time.
After about 10 minutes I become worried enough to knock on the neighbors door on the floor below to ask to be observe for about 30 minutes while this passed. Within 10 minutes or so of talking with her, I asked we call an ambulance and that she come with me. Neither of us speak Thai well enough for this.
She looked ahead for security in the lobby and parking area, while I struggled to keep up. Oddly, no one was working that night. Very strange. She crossed the road to talk to a motorcycle taxi driver to get assistance to ensure we got the right ambulance. While she was doing this, I saw a kind looking guy walk down the street and waved him over (her as it turns out to clarify for those who don’t know Thailand very well). I gave her 100 baht and asked she run to 7-11 to buy some cold water to help cool me down. By the time she came back, I was hanging off a gate and couple barely lift an arm to grab it. I was loosing the ability to breath and keep conscious. But not from an obstructed airway.
She offered to drive us to the hospital, but by that time the ambulance came around the corner. She and my neighbor followed in her car.
Every single tiny bump in the road was absolutely excruciating. By the time we arrived, I was quickly getting worse. The pain became unbearable and I could not longer take a full breath, lay back, or sit still very long. The hospital staff informed us that because I had food in the stomach, they would not be able to operate until 10 or 11 am. That was going to be too late, but they kept insisting. This has happen to point of operation before (although not this badly) and the OP was done on the spot without delay. The risk of vomiting during the OP far outweighed the risk of waiting.
After quite a bit of pleading and persistence from my two friends, they finally agreed to do the operation now (5am by now), but only if I cam up with 50,000 baht ($2000CAD) deposit for hospital admittance first. On the spot, I could not do this. Sounds crazy, but that’s the way the world works. My friends contacted my cousin’s, one of which was on her wedding day of all things! They got the ball rolling while I was incapacitated.
Please don’t reply to me with the obvious ‘you should have bough insurance’ advise here – I know this and didn’t have it.
There are far more important issues to address, as I will get into below:
The Dr found during surgery that I had torn the esophagus. I’m not sure when this happened exactly, but I’m sure it became worse during the hours of extreme heaving while waiting for the OP and bouncing around the ambulance for 20 mins. The tear is about 10cm long and very wide, it’s not small by any means. I am extremely lucky that only a smaller portion of that actually went all the way through.
A laceration like this is a big problem. When it perforates the wall, it’s a bigger problem and becomes life threatening.
There is a 20-30% mortality rate for people who have this condition.
This is not a typo or exaggeration, this comes directly from the Dr. The level of my situation is severe, it is not a tiny hole.
Most of the time it’s the complications that get you, which I have plenty of. More on that later.
A second operation, the day involved covering the laceration with a stent delivered from Bangkok. This meant an additional delay of about 10 hours before the perforation was covered an no longer seeping air into the chest cavity. This air puts pressure on organs and can cause the type of fatal complications you could probably imagine. It’s common to affect the lungs, and other things as well.
An X-Ray of the stent of Day 2 & 3 showed it slowly moving downward towards the stomach. They are designed this way because at some point they need to be removed, which until this afternoon was going to be my 3rd scheduled operation 3-4 weeks from now if all went well. Although it was slipping, it was still covering the perforation.
Today a CT scan showed the entire stent in a ball inside my stomach, doing no good. This brings us back to emergency stage #1. Air seeping into the chest cavity, as well as bacteria which causes nearly 50% of fatalities in these cases.
This means a critical operation tomorrow morning (about 9 hours from sending this out) to pull the stent back up to where it should be, so it covers the perforation. This time the Dr is going to try to clip it into place and also glue the perforation shut.
If you’re not sure what a stent is in this case, it’s basically a plastic membrane tube lined with expandable (springy) metal mesh that forces itself into place against the esophageal wall – protecting it from foreign contact and allowing the tear to heal. If it’s too tight, it the healing tissue may attach itself to the stent and cause it to become permanent… which is a whole new set of problems.
As you may start to be understanding, there are many different types of complications with this issue and because it is so rare there aren’t any Dr’s who have had a need to study it, let alone have experience.
This brings us to where things are now:
Even had the stent stayed where it should be, there are a couple important complications.
Air seeping through the esophagus into the chest cavity has build up enough to cause pain with deep breaths and is very apparent when you lightly press against the pectoral area. The skin feels spongy and you can feel hundreds of bubbles. Left alone, this was expected to clear itself as it was a relatively low amount due to the stent placement within the first 24 hours. The Dr suggested we give it a couple weeks if there was no associated pain or increase with other symptoms.
Bacteria seeping the same. This can cause an infection within the chest cavity and lungs.. which it has. The lung infection seems to be a little better with each passing day (antibiotic drip), however there is a ‘patch’ of infection growing underneath the lower left pectoral.
The combination of these two, along with the now released stent has turned this into an emergency situation again.
(Please read this with a level head and remain calm, I need extra emotional friends to be relaxed and logical at this point. Need support, not to become emotional or depressed myself. I NEED to be strong and focus all my strength on the solution)
The Dr has told me that without continued treatment, I am not going to survive with the condition as is. Despite all current efforts my health is declining with complications.
** Please keep this in mind when I ask for your collective help at the end **
Continuing treatment my chances are as I mentioned before. 20-30% mortality rate. Each new complication disfavourably increases those odds.
If left untreated, I will succumb to infection.
The next Steps:
Scenario 1
The 3rd OP tomorrow as mentioned is to replace the stent. Once that is done, it is a waiting game until the next complication shows it’s face or an existing one does not show signs of healing. Best case scenario, I go home 3-4 days after and return for a checkup every 2-3 days to see where the stent is sitting, check infection and trapped air levels. In a perfect world, the body will heal itself with the help of modern medicine and some love from friends and family.
Scenario 2
The stent holds, but the current pocket of infection required draining. This means a chest tube and more antibiotics. Back to the hospital for awhile.
This scenario also includes the trapped air issue, if the body does not naturally absorb it, it may need to be released. Probably not as bad as it sounds.
Scenario 3
The stent dislodges again. If this happens, things get a little more serious. There are more extreme options for suturing the laceration. The lowest mortality rate comes from instances where a conservative approach can be used, such as mine. Although the laceration is actually quite huge, the perforation is manageable. If the entire laceration was also a perforation, I may be writing a different type of letter.
The hell of living the current situation and my request to the Dr.
I woke up from the first OP on a breathing tube and a team of people hovering above. What woke me up? I could not breath. The shock of waking up to that is one thing, but another is that I could not breath out due to a lung infection clogging the air tube. Panic set in.
Panic turned into what I thought were my last breaths of life. In my mind, I was going to die by suffocating on my own spit. I sat up, flailed a bit and tried to show them with my hand I needed to write down what was happening so they could fix it. They thought I wanted to rip the tube out and strapped me down to the bed, that made the panic worse so after strapping y hands and legs, they tied down a ‘pycho’ sheet to keep e more snug and let me fight the mucus. They did not know I was drowning in phlem.
A very hard last ditch exhale dislodged the mucus into the tube and I was OK for a little while. It quickly built up aver and over requiring multiple similar experiences. I continually made a writing gesture with my hand to show I wanted to write on paper, they did not understand and told me ‘NO’. They thought I was going to rip the tube out or fight them. At times being cheeky as well and laughing to themselves. It was an absolute nightmare like torture. After 3-4 hours when the Dr finally came to update me, he explained the handcuffs and I showed him my writing gesture. He allowed me to write, and instructed the staff to let me go.
I had this reaction probably 5-6 times during the final 30 minutes and honestly did no think I could keep it up much longer. I felt lucky the Dr finally came. They gave me one hand to allow me to suction my own mouth and the other after some time later.
NOTE: My very clear request to the Dr in a private talk tonight was to not wake me up if that is the scenario again. I asked him to keep me asleep until after they are able to safely remove any life support machines. I don’t mind the machine or even a coma if need be to keep the body still a couple weeks. But I do not want to live that hell ever again.
Moving forward & why I wrote everyone in one big batch
Obviously there is a lot to explain. It would be impossible to explain pertinent information to everyone individually and then reply to each several times to answer questions. Need to get the message out those who need to know or may be able to assist in some fashion, and then I need to refocus on making sure the next step is the best it can be.
This may be too much information for some, too family oriented for others, and too impersonal for some as well. It’s simply a bulk “What’s up” update for all.
How you can help!
1. Research
– I need help finding the best possible Doctor.
If you live in Pattaya (or Thailand actually), it would be great to learn of Doctor who specialize in esophageal perforation repair. My current Dr claims to have two previous cases. Both were successful. I do not know the details. The GI in Vancouver who did my colonoscopy a couple years ago has done more than 10,000. See where I’m going with this?
I am not fit for travel. Perhaps if stabilized could make it to Bangkok, but would need to ask. Flights are out of the question due to the trapped air pressure and trauma of movement to the laceration.
2. Immediate Need for Funds
My cousins have pledged to assist with initial hospital fees, which are already far more than anyone expected from day one. Today, the Dr explained various paths that complications may take treatment and unfortunately it may include a month or two in hospital trying to exhaust all efforts. Best case, they clear me by the end of the week. I doubt this though as the infection is growing even though I have been under multiple antibiotics as a precaution the moment I came out of the first OP. A very rough guesstimate is that we are only 1/3 – 1/2 done the way it looks at the moment.
That means I need to plan to raise up to another $40kCAD
Saving money is the easiest way to earn money, however it can also be dangerous in my case.. which is why I put Research as the #1 at the moment.
I made a bad investment last year and have been putting my extra money into building a small but now successful little business. I have used what I have left and now need help, there’s no way around it.
I am in a private hospital, with the best Dr’s Pattaya has. As you can see, it does not mean they also have much experience with this condition. They do have public hospitals. The downside to those are many more customers per patient and lower standards & equipment due to lack of funding.
Although better than no treatment, the inherent risks make this critical situation even more so than it already is. The hospital here is great for it’s local, but lacks in some very basic service details that can be downright scary when you consider what may be missed in the bigger picture as well. Going to a public hospital is an absolute last resort.
3. If you can thinking of any other way to pitch than what I’ve mentioned, please do!
I need great organizers (in case I need to do a crowdfund),People with friends that have friends in Thai medical land, People who can help with a donation or two, People who can simply send their best positive energy if nothing else!
Please message me on FB, or whatever media you have. Tomorrow is supposed to be a light OP, so I should be awake later in the afternoon (Thai time) to check messages. Unless someone screwy goes on, I should have at least 2-3 more days before the next potential complication is expected.
Thank you all very much for reading this incredibly long explanation. I’ve a few people reach out to me who have heard of a bad situation and wanted to learn more. As I mentioned, I just can’t explain it all to everyone without doing it this way, plus I’m a geek so this is actually easier than it might seem, lol
<3
----------
July 30th Update:
Thank you all who have been watching this.
The stent did not hold as hoped, it's off to the OR again tomorrow. Thankfully, this is a fairly minor procedure to remove. The Dr will not try a 3rd time. He did manage to glue to hole during the last stent relocation, so hopefully it is still holding. Will know more in the next few days when they do a CT to check for leaking.
This translates to: I'm stable for the moment. However, now I have heart complications. Joy...
The good part it also means I can now look to transfer to a new hospital, with lower costs and a fresh set of Dr eyes (and experience) to look at the situation. I feel the current Dr has done what he can and is taking some very serious risks to save a few baht that I would never considering the consequences. Thailand is a beautiful country. Insurance or not – you do NOT want to get stuck here with a medical emergency. The experience, service and facilities just doesn't compare to what we are accustomed to back home. I have heard stories of expats losing their lives due to 'common' issues we have back home.