- A
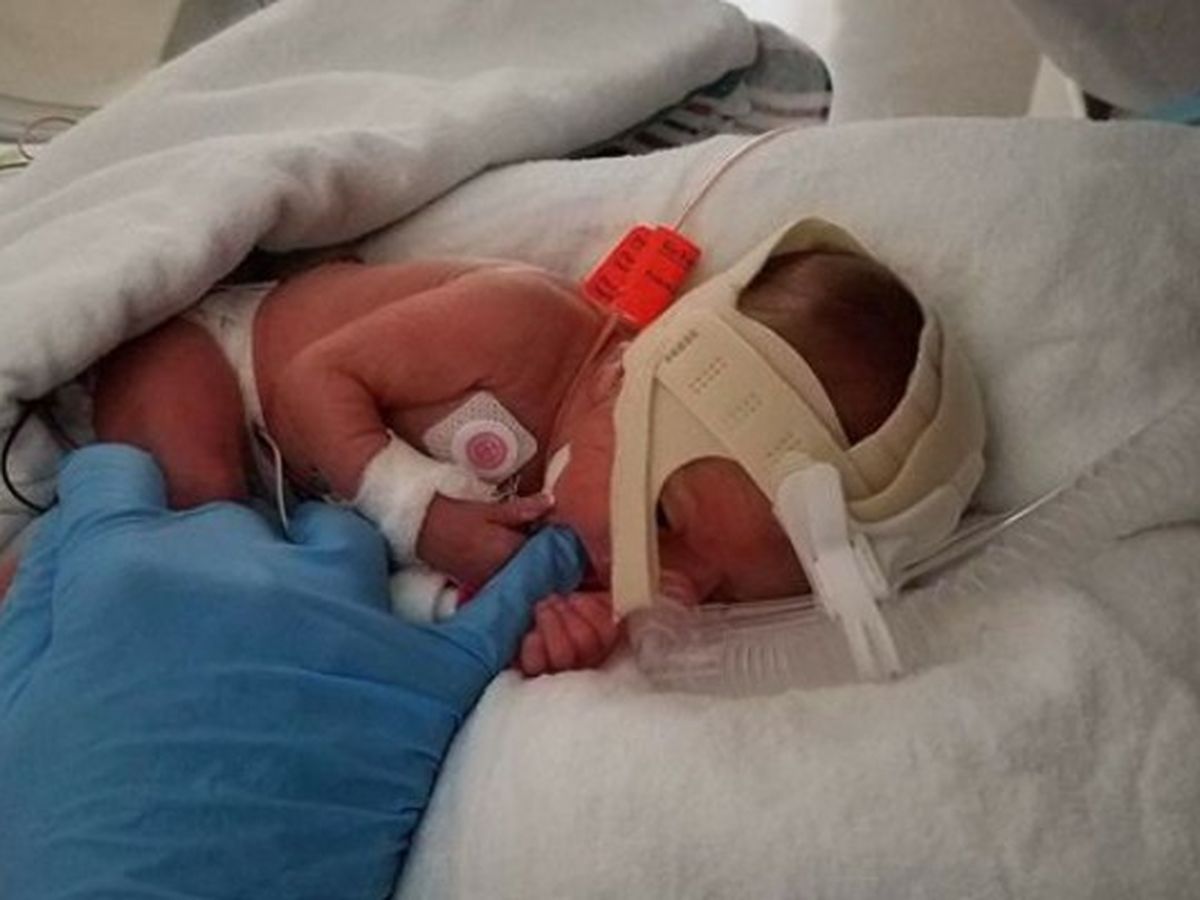
Carleigh Nicole was born on August 11 at only 26 weeks old weighing 2.6lbs. Its been a long couple of weeks with ups and downs, Carleigh is growing good and doing what's expected. She is currently in University of Maryland's NICU.
When first born was on the cpap and having frequent brady destats (when the heart rate ans oxygen drop) after they increased over the next few weeks her crit was low and red blood cells only at 27 later lowering to 21 which made her need a blood transfusion. After the trasnfusion the bradys had become much less than before but oxygen kept destating so xrays and echos were done of her heart and lungs. She is being treated by cardiology for a congenital heart deffect (VSD) a whole in the lower part of her heart, it is causing fluid to build in her lungs which makes her destat (drop oxygen). Shes been on and off lasix to help move the fluid and pass it but its recently made her electrolytes too low so its been stopped which unfortunately leads to more consistent destats in her oxygen when shes off of it. Currently cardiology has said her vsd is larger than a normal preemie size and she will need heart surgery by 7 months of age. If the oxygen issues don't get better it may benefit to have surgery sooner.
At a few weeks old they tried her on room air but she failed the test and was put back on oxygen because she was working herself to hard on room air causing her heart rate to spike.
She is receiving donor breast milk fortified with calories through a feeding tube. Currently all IVs have been removed.
Shes also getting caffeine and iron daily.
In recent weeks she has recievwd 2 eyes exame for retinopathy of prematurity, the first test for zone 2 she scored a stage 0 which is great!! Her test this week they found stage 1 in her right and stage 2 in left eye, so that will be monitored more frequently and if needed laser eye surgery will be done down the road since r.o.p. causes complete blindness but fingers crossed it doesn't progress.
Carleigh is growing great with very few setbacks, and all health issues are being monitored and surgery will be done when shes big enough.
Lately she is also being closely watched due to lessions on her liver.
If Carleigh continues to grow well and no other problems arise she could potentially come home by December.
We were very hesitant to make this go fund me but the nurses at the NICU kept insisting it would be a good idea.
Carleigh's insurance is only covering 65% of her medical coasts and billing us for the rest.
Also with her current conditions it has been brought to our attention with the medical equipment and machines she will come home with that they require us to buy a generator for the home incase of any power outage.
At this time when Carleigh comes home she has 5 different specialists she will have to keep regular checkups with for each area , and cardiology in Hershey PA until she has her heart surgery.
We live a hour and a half away from the hospital and with her father working and commuting daily and 3 small children at home its very difficult to be there as much as we would like.
The hospital expanses and driving, parking all creates added financial stress resulting in her dad working longer days and rarely being home. We would love to be able to not have any added stress and enjoy this time the best we can and be able for us both to be there by her side.
I go as i can but working around our oldest childs school hours, traffic for the drive and keeping a 2yr old and 11 month old entertained in the NICU becomes next to impossible.
The doctors have addressed Carleigh down the road being moved to the step down facility at Mount Washington which is even more far away from us, and with loosing my son in a NICU the way he passed its emotionally hard after just becoming comfortable and trusting with the care shes receiving.
Theres a hospital 15 minutes from our home that ive spoke with and has a level 3 nicu and step down facility and would take Carleigh but insurance isnt trying to approve the transfer cost of over 50k. There has been many issues between PA insurance and her being in MD so its been a constant battle.
Carleigh is a fighter, our miracle and a blessing. This has and continues to be a emotional rollercoaster. There's good days and days when it feels like the poor girl can't catch a break.
No matter how well you prepare nothing prepares you for this. My heart aches for our girl and we all just want her healthy and home.
The prayers and support we are receiving we are grateful beyond words for.
We just cant wait for Carleigh to be home and this all to be in the past.

Below is the information on what lead to Carleighs early arrival.
Carleigh was born at 26 weeks only weighing 2lb 6.3oz on Friday August 11, 2017.
Many friends & family have been following our journey but for those who haven't here's our story..
Carleigh is 1 of 5 siblings her oldest brother Christian 7, a angel sibling Noah who would be 4 & two big sisters Allyanna 2 and Maddilyn her irish twin who was 10 months when she was born. My pregnancies have all had their ups and downs but nothing could prepare us for what we would face this time.
When we first found out we were expecting everything looked great! There were risks we knew with this being a 5th c section in less than 7 years and my body not having much time to heal but my doctor promised a safe and thoroughly monitored pregnancy. Things continued to positively move forward untill about 13 weeks, when i experienced a lot of bleeding and blood loss. I went to the hospital in york, pa and was told i had placenta previa and what looked like the placenta was detaching from the wall, they explained if it was to attach elsewhere it could be fatal but realistically we needed to prepare that our little girl wouldnt make it past 20 weeks. We were faced with the choice that when the time came to choose a D&E and never see her or a c section and see her but ultimately leading to no more future children as my tubes would be tied for safety reasons medically.
I followed up with my normal doctor who is based in baltimore md, he continued to keep up with us and have me checked weekly with fetal assessment. As weeks passed i was going to my regular appointment and fetal assessment twice a week, i had unexplained bleeding and heavy blood loss daily and barely stayed out of the hospital. We soon found out i had a internal bleed that was abnormally large like nothing they have seen before. The fetal assessment doctor prepared us and explained that in cases with a much smaller bleed the baby doesnt make it past 18 to 20 weeks.
I continued to loose large amounts of blood daily, became very weak and was receiving blood transfusions weekly, but we made it to the 20 week mark! As the blood loss continued and my health was at risk the question came of my life or the babies, but that wasnt a choice as she was healthy and it was more of a risk to deliver for us both.
When the 22 week mark was reached we had beat the odds, and where even more closely monitored as i became very ill carrying our girl. The doctors couldn't believe how we were both still together and how good she was doing. My bleed internally only got worse and continuedto grow, several conversations happened preparing us that i possibly wouldnt survive this or delivery. Nothing is more terrifying than thinking my time with the children i have was limited.
24 weeks approached and we discussed lung development shots and delivery at 30 weeks to save me, because going any longer would be to risky, but fetal assessment felt to wait a few more weeks before doing that, they didnt think she would make it to the point of receiving the shots and them being beneficial.
Some days i didnt know if I'd ever meet our girl, and with already holding my son and watching him die my heart couldnt imagine losing another child. The next couple weeks were spent either in a doctors office or a hospital, usually receiving blood to only loose it within a few days and need more. One week i began feeling excruciating pains , breathtaking to the point i couldn't move, walk, talk or even care for my children. I waited 2 days thinking it would go away and be false labor , but after helplessly laying on the couch and almost passing out from the pain i went to the hospital.
I arrived at harbor hospital one night in full blown labor and was placed on magnesium to ease contractions. The following day my obgyn came in and explained the importance of transferring me to University of Maryland Medical Center. This was all uneasy for me after what i went through when a Noah passed, i had built such a close bond with my current obgyn and learned to trust again so the thought of being transferred and placed in a strangers hands was scary but ummc was the only place that could care for Carleigh if she came at 25.5 weeks.
We arrived at ummc and was still on magnesium, they immediately using a more Hi-tech machine did a ultra sound and found the REAL problem! My placenta had ate through my uterus and into my bladder, the bleed they had been treating me for was actuallg caused by the sepration from the uterine wall, and i also had the previa. The specialist told us my survival chances were dependent on how bad it was when they opened me up, but ideally my chances were less than my age. We had to come to terms that this would more than likely kill me. The next morning i had more im depth sonograms and labs done, i met the nicu team and the special ob who would be taking care of me while there for the next few weeks. He went over the results and how much worse it was than we thought. I'll never forget around 3pm he went over our gameplans with me, the goal was to be carefully monitored as Carleigh and I were both losing nutrients and we would do surgery and a full hystorectomy in a few weeks, once she got bigger.
His exact words were.. "we will plan surgery for the morning when we reach that in a few weeks, this type of surgery and complications is something you want to do in the day time , never at night. You need tl be able to have access to all hands on deck"... sure enough just hours after that talk i was having contractions that had me flying up the bed and almost passing out from the pain, the magnesium wasn't even helping.
So the doctor sat by my side and at 6pm i saw the look on his face that spoke a million words. I quickly called my fiance and told him i thought it was time, but he was still a good bit away just getting off work...
By 615 it was decided we had to deliver, i held the doctors hand and cried and begged for him to promise i would wake back up, i could see the uncertainty in his eyes when he said he will do his best.
My fiance made it with seconds to spare. Originally they said he could be by my side until the anesthesia had me out and than would have to leave, but because of how urgent things became that was no longer a option.
They wheeled me into the elevator because my surgery was to much for the labor delivery o.r. so i had to be in the shock trauma o.r. and in the elevator we stopped at the 3rd floor where i had to kiss my fiance goodbye and drop him off to go wait in the waiting area.. that was the scariest, hardest thing I've ever done. Nothing prepares you for knowing that could be your final goodbye.
Once he was gone the elevator ride seemed like forever! They pushed me into shock trauma o.r. where i was met by 32 doctors and surgeons for our suegery, Carleigh had her nicu team of surgeons there too.
Carleigh was born within the first half hour, Surgery began at 645 pm and Carleigh arrived just a little after 7pm (715pm) weighing only 2lbs 6oz just slightly over 13 inches long and a corrected birth age of 26 weeks gestational.
My fiance and Mother waited anxiously and were updated with the news of Carleighs arrival and able to go see her in the nicu as they waited for my update. During my surgery they had removed my uterus, the top of my vagina, one ovary and a handful of other things, bladder surgrry was done once the placenta was removed from it. It was found out that during the pregnancy the clots and bleeding i experienced was actually at some times tissue being passed, it was pieces of my uterus.. That's how damaged it was, they also found that every ligament in my abdomen had blood clots completely formed around them.
The doctors had updated my family that they were about to begin clean up, worried becaue it was taking so long we were later told before clean up i hemorrhaged which was what caused the delay. The doctors joked i ended up with pretty much all new blood and not much of my own left in my body and that with all the blood they had to give me that i ended up with more than the red cross.
But... 97 staples & 8 hours later after the most difficult delivery/surgery the high risk ob surgical team had yet to see and handle, we were both out and alive
They kept me sudated for a day when i finally woke up it was 2 days later, i woke intubated and terrified. I stayed in the ICU intubated for a few more days, finally they went to remove my tubes and within hours noticed i wasnt breathing right, they had xrays done and rapid response team came to get me we found out i developed surgical pneumonia and was intubated and back in the ICU for a few more days.
The days passed slowly and was killing me to not see me girl, emotionally i was a wreck especially after already loosing one child and not having much faith in her care, but finally after 1 week and few days i was able to meet Carleigh.
It was love at first sight , so tiny but yet the love for her was so big. Every one was so happy and couldn't believe i survived surgery. They were all so welcoming and patient with my recovery and keeping me updated from there on out.
They explained everything going on with Carleigh and the hope i never had i seemed to find.
After another week or so if being closely monitored and working with physical therapy i was finally able to go home. The hardest goodbye ever! The last baby i left in a NICU never made it home so i was very uneasy. The nurses felt my pain and although it was a bit too soon, they allowed me to have skin to skin wirh Carleigh before i went home.
Now over a month later i am so much better and Carleigh as well. I keep in touch with my surgeons and have been interviewed by teachers to learn more about my condition. I see Carleigh as much as possible but it still never feels like enough, i just wish she wasnt so far away.
The nurses taking care of my baby are a blessing, they are all so kind and amazing. I call 2 or 3 times a day when i cant be there and everytime im treated with patience and descriptive updates.
As if September 27th Carleigh is growing great! She has some health issues being closely followed but nothing that cant be fixed with surgery.
I will continue to write daily updates on this page.
Carleigh is our miracle, she has a big family that cant wait to have her home! We all are so grateful for all the support we continue to receive.
#CarleighsAngels